Aqueous humor is defined as the clear, watery fluid inside the front of the eye. It works by bringing nutrients to the eye and by maintaining the eye’s normal pressure and shape.
The eye is constantly producing new aqueous, while old fluid drains from the eye through the trabecular meshwork. Having equal amounts of aqueous humor created and drained simultaneously keeps the pressure of the eye balanced.
Aqueous humor anatomy
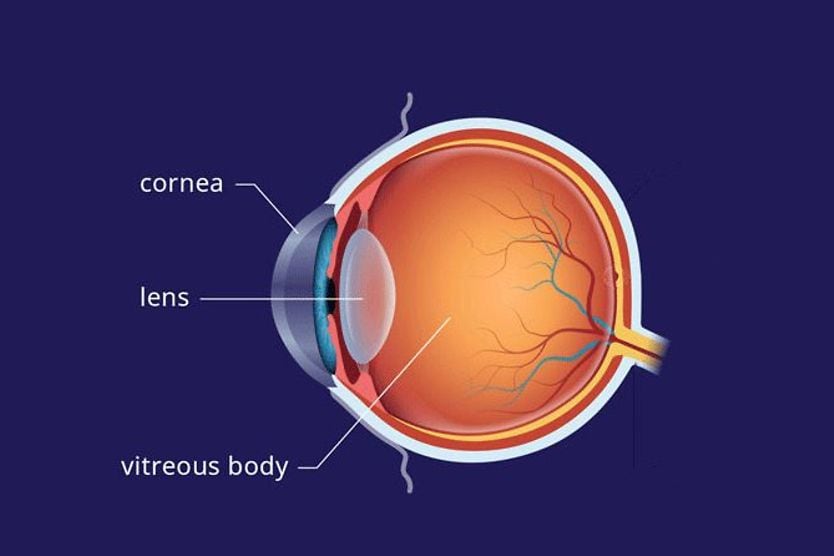
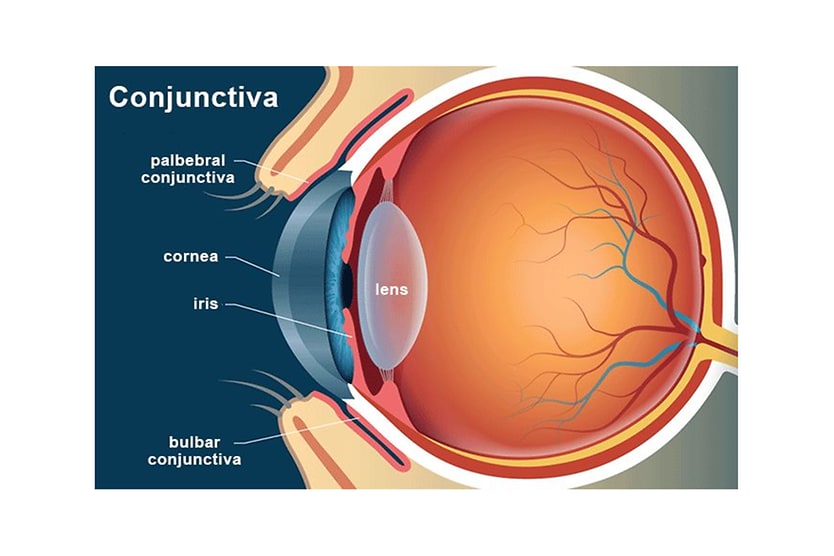
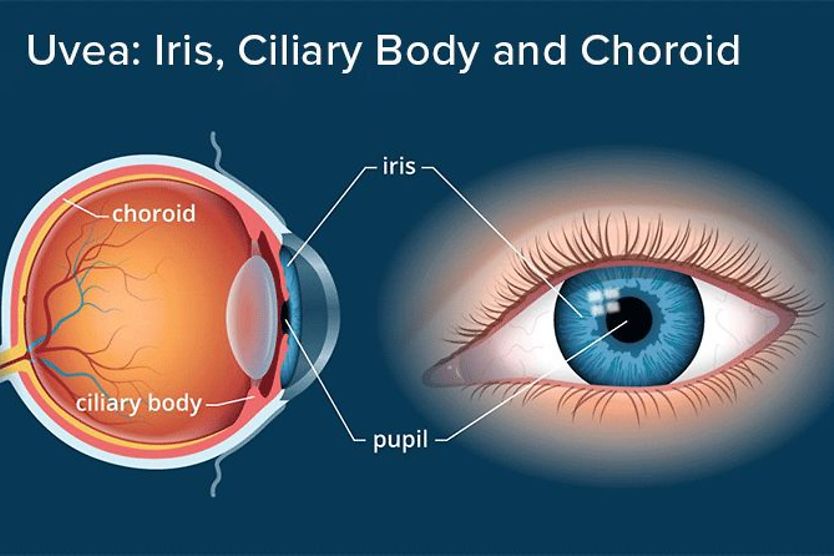
Regarding eye anatomy, aqueous humor is found in the anterior and posterior chambers of the eye.
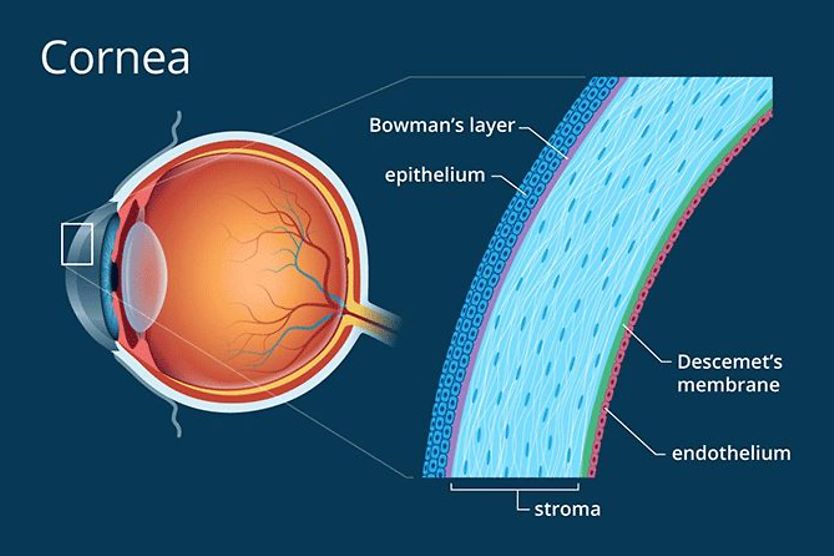
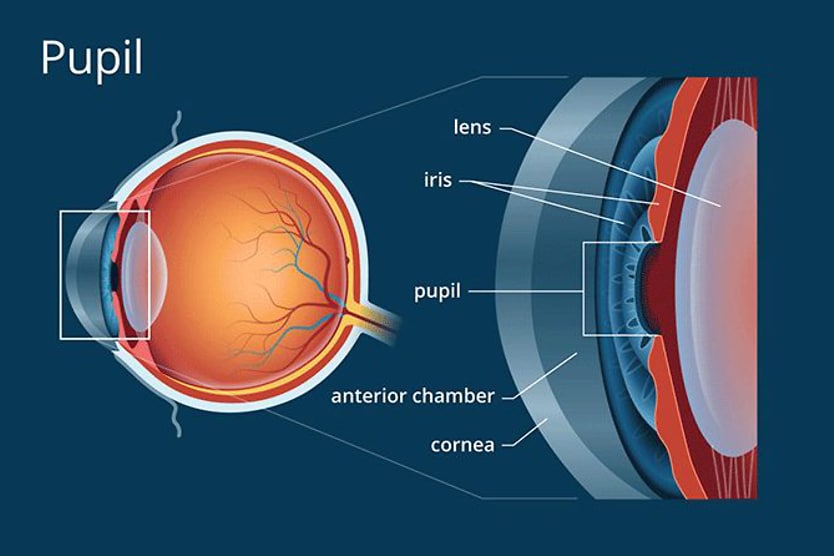
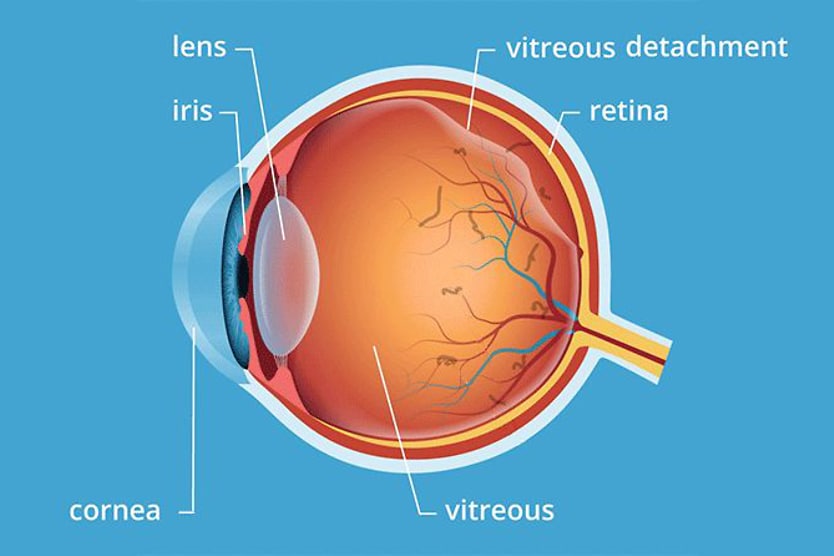
The anterior chamber is located between the cornea (the front layer of the eye) and the iris (the colored part of the eye). The posterior chamber lies between the iris and the front of the lens.
Aqueous humor consists almost entirely of water — 99.9% to be exact. The remaining 0.01% is made up of nutrients such as sugars, proteins and vitamins.
Aqueous humor function
Several eye structures that are located in the anterior and posterior chambers of the eye don’t have a blood supply. Instead, they rely on aqueous humor for nourishment.
Aqueous fluid also removes waste from the eye with its constant flow through the anterior and posterior chambers.
While providing nourishment and removing waste, aqueous humor is also responsible for maintaining proper, balanced pressure within the eye. This may seem like a simple task, but it’s incredibly important for eye health.
Imbalances in the creation and drainage of aqueous humor can lead to high intraocular pressure, also called IOP or eye pressure. High eye pressure is a main factor of glaucoma, a potentially sight-threatening condition.
Aqueous humor flow
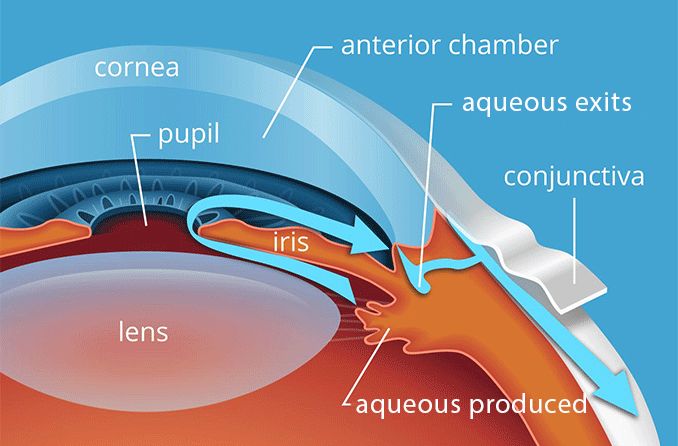
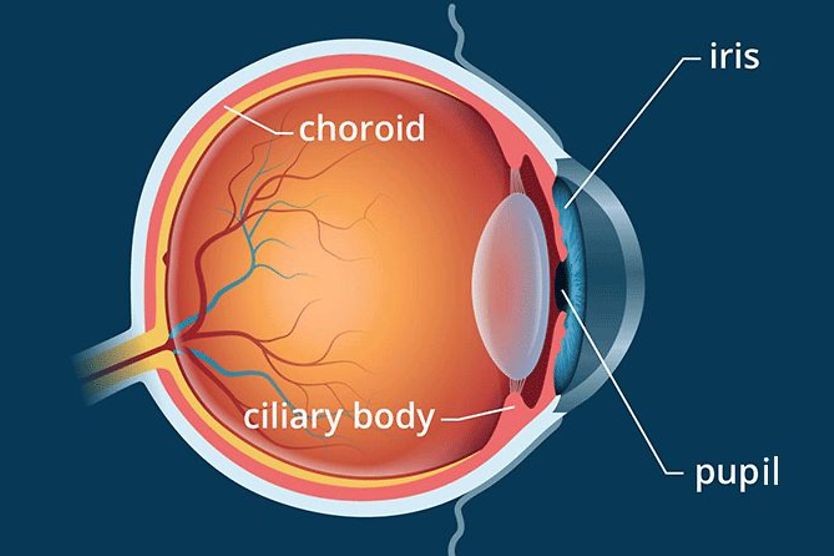
The flow of aqueous humor begins in its production by the ciliary body, in the posterior chamber of the eye. From the ciliary body, aqueous humor flows through the pupil and into the anterior chamber.
Aqueous humor then leaves the anterior chamber through a structure called the drainage angle. Once inside the drainage angle, the aqueous fluid leaves the eye through a spongy tissue called the trabecular meshwork.
The trabecular meshwork moves the liquid into a drainage canal, called Schlemm’s canal, where the aqueous humor then drains into the eye’s circulatory system.
Aqueous humor and glaucoma
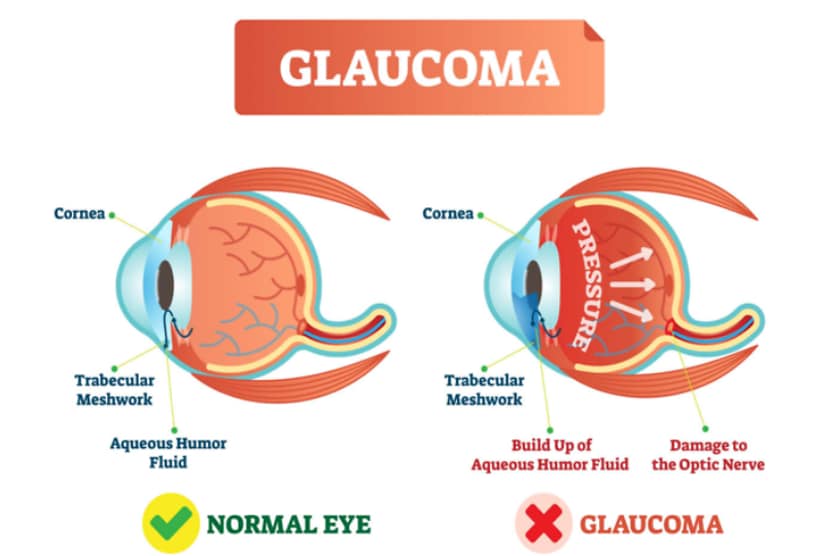
Imbalances in the amount of aqueous produced and aqueous drained can lead to ocular hypertension, or high eye pressure. This can occur because of an overproduction of aqueous humor or an insufficient drainage of it.
As mentioned earlier, aqueous humor leaves the eye through the drainage angle. It’s possible for the drainage angle to be “open” or “closed,” meaning the passageway is narrow. The narrower the drainage angle becomes, the more difficult it is for the aqueous humor to drain.
When the drainage canal narrows to the point where aqueous can’t drain effectively, it results in narrow-angle glaucoma: High eye pressure caused by a closed drainage angle. This type of glaucoma is rare and may occur gradually or suddenly (called acute angle closure).
It’s also possible to experience poor aqueous drainage even when the drainage angle is wide open.
This is known as open-angle glaucoma and is caused by a blockage in the drainage canals — like the trabecular meshwork or Schlemm’s canal — rather than the drainage angle. Open-angle glaucoma typically develops slowly and is the most common type of glaucoma, representing at least 90% of cases.
Both types of glaucoma, if left untreated, can damage vision and eventually cause blindness.
When to see an eye doctor
Many times, when glaucoma development is gradual, a person may experience few to no symptoms. This is especially dangerous because people with glaucoma won’t know something is wrong until their vision is affected.
While treatment is available for both open and narrow-angle glaucoma, the damage done to vision before treatment is administered cannot be reversed. Having regular eye exams can keep you and your eye doctor mindful of your eye health, lessening your chances of glaucoma-related vision loss.
During a comprehensive eye exam, the eye doctor will check your eye pressure. If you appear to be a glaucoma suspect — meaning you don’t have glaucoma, but have higher than normal eye pressure — they may recommend preventive measures to lower your risk.
READ MORE: 3 main causes of glaucoma