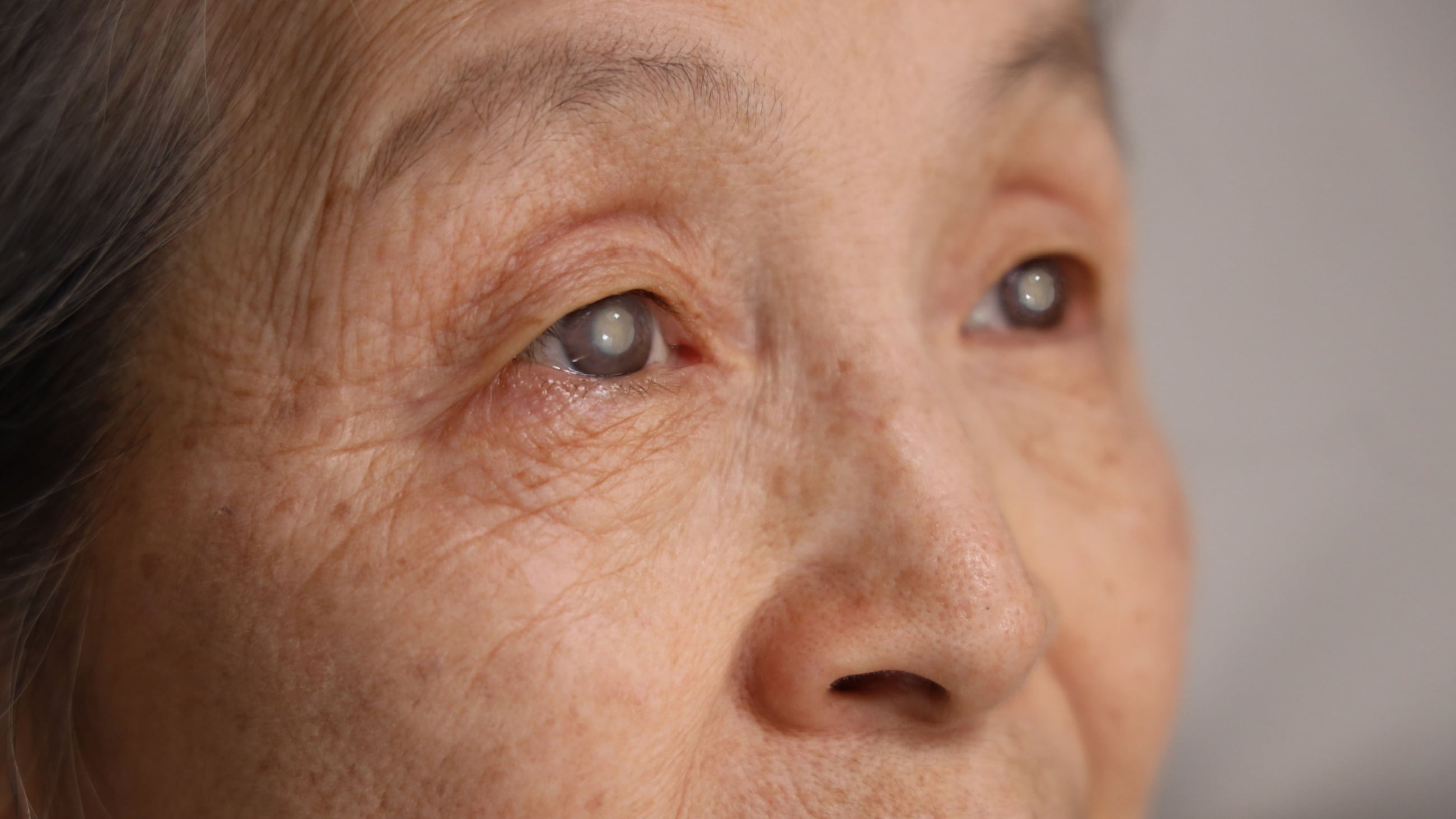
Complications and side effects of cataract surgery
Cataract surgery is one of the most common surgeries used today. It's safe and effective overall, but all surgeries have risks of complications and side effects. It's important to recognize the signs of a problem in case it happens to you.
Some side effects are normal. They should go away on their own.
Most complications can be treated with medication or surgery when they're diagnosed early enough.
If you think something is wrong, tell your eye doctor. Some complications need to be treated as soon as possible.
Complications
It can be scary to read about cataract surgery complications, but serious problems are rare.
Most post-cataract surgery problems are treatable when they're treated quickly.
Rarely, a complication can lead to permanent vision loss in that eye. This happens to around 1 in every 1,000 people who have cataracts removed.
The possible complications of cataract surgery include:
Secondary cataracts
A secondary cataract is clouding on the natural capsule or "bag" that holds your artificial lens in place.
This is the most common complication. Around 2 in 5 patients will get secondary cataracts eventually.
It can also occur years after the procedure. Many people don't notice visual problems until several years after their procedure.
A secondary cataract isn't a real cataract, but it can cause some of the same symptoms as one. If you notice blurry or cloudy vision a while after your cataract surgery, you might have a secondary cataract.
The treatment is a laser procedure that only takes about five minutes.
Talk to an eye doctor if: You have blurry or foggy vision after cataract surgery, even if it's been months or years since your procedure.
Leftover lens fragments
During most cataract surgeries, the surgeon breaks up the cloudy lens and removes the pieces. It can be hard to remove all of these fragments. Tiny lens pieces can get left behind inside your eye.
Your eye doctor may be able to treat small fragments with medicated eye drops. If the drops work, the lens pieces should dissolve over time.
If the fragments are big, or if there are a lot of them, they can cause inflammation and other serious problems inside your eye. You may need another surgery to remove them.
Your original cataract surgeon may not perform this procedure. They could refer you to a retina doctor called a vitreoretinal surgeon.
You might have leftover fragments if your mild side effects aren't getting better in the days and weeks after surgery. Normal side effects may last longer for some people, so ask your eye doctor if you're not sure.
Get help right away if: You have severe eye redness, pain or any vision loss.
Artificial lens moves out of place
Rarely, the artificial lens inside your eye will move out of place.
This can cause:
- Changes in vision (including blurry vision)
- Double vision
- Glare
- Headache and eye pain
- A visible lens edge in your field of view
Double vision after cataract surgery isn't very common. It may go away on its own, but it could also mean you have a dislocated artificial lens or another eye problem.
You may be able to manage your symptoms with new prescription glasses or contact lenses. Your eye doctor may also recommend another surgery.
Most people still have 20/40 vision or better when they manage or treat a dislocated lens. But you may need to treat it quickly.
If you need surgery but wait too long, it could lead to serious eye problems.
Seek medical help if: You're in severe pain or it looks like a dark curtain is moving across your vision.
High eye pressure
It's not uncommon to have changes in your eye pressure after cataract surgery. Most changes should go back to normal within 24 hours of your procedure.
High eye pressure can permanently damage your eyesight if it spikes too high. It may need to be treated quickly.
Eye pressure spikes can happen to anyone. But your eye doctor could be even more concerned if:
- You have glaucoma.
- You're a glaucoma suspect.
- You have another eye problem that puts you at risk.
The doctor's office will ask for this information before surgery.
Talk to your surgeon as soon as you can if:
- You have eye pain or a headache.
- You feel sick to your stomach or throw up.
- You see changes in your vision.
Infection
There's a small chance bacteria or fungi could cause a serious infection inside your eye. It can cause vision loss if it isn't treated quickly.
The infection can cause symptoms like:
- Eye pain that gets worse as time goes on
- Eye redness
- Swollen eyelids
- Blurry vision or vision loss
- White or yellow eye discharge
Your eye doctor will run tests to see if you have an infection. If so, they'll give you antibiotics or antifungal medicine so it doesn't spread.
This complication can happen to anyone, but it's more common in older people over 85 and males.
Call your surgeon right away if: You have any of these symptoms, especially if it's only been a few days (or less) since your procedure.
Macular edema (swelling)
The macula is a small spot in the center of your retina (the inner back lining of your eye that helps you see). Cataract removal can sometimes cause swelling and tiny blisters on the macula.
This is called cystoid macular edema. There are several ways to treat it.
This type of macular edema can make things look wavy or blurry in the center of your eyesight. Tell your eye doctor if you see things like this.
Corneal edema (swelling)
Corneal edema is swelling on the clear, front layer of your eye called the cornea. It's often caused by inflammation, infections or high eye pressure in your eye.
Some cornea swelling is common after surgery. It could get better once your eye doctor treats the underlying problem.
Corneal edema can cause eye pain, blurry vision and light sensitivity, especially if your symptoms are worse when you wake up.
You may need another procedure if the swelling doesn't improve or if you're in a lot of pain.
Bleeding
Sometimes small blood vessels inside your eye can leak or burst after your cataract removal. Without treatment, it could threaten your eyesight.
Your eye doctor may suggest medication or surgery if the bleeding worsens or causes other problems.
Seek help right away if:
- You have any amount of vision loss.
- You have severe pain, headache and nausea.
- Your eyesight is getting blurrier.
- Everything looks like it's tinted red.
Retinal detachment
Your retina can peel away from the back of your eye after surgery. This is called retinal detachment. It can cause permanent vision loss if it isn't treated quickly.
Someone who's very nearsighted could be more at risk for a detached retina after cataract removal.
Get immediate help if:
- It looks like there's a shadow or curtain over part of your vision.
- You see a lot of new floaters (they look like little squiggly lines or dark spots).
- You see flashes of light.
Side effects
It's often normal to have certain mild side effects after cataract surgery. They should go away on their own within a few days or weeks of your procedure.
Talk to your eye doctor if you aren't sure whether a side effect is normal or not.
Possible side effects include:
Blurry vision
Blurry vision is a common side effect. It makes things look fuzzy or out of focus.
Most people have blurry vision after cataract surgery because their eye is still inflamed from the procedure.
Blurred vision should get better within a few days, but it can take as long as four to six weeks.
How to help: Your surgeon may give you special eye drops to reduce inflammation and swelling. Make sure to follow the directions closely.
Dry eye
There's a good chance you'll have some degree of dry eye after your cataract surgery.
Your eye might feel gritty, uncomfortable or sensitive to light. Your vision could be a little blurry, too.
Any dry eye symptoms should feel better within three months.
How to help: Artificial tears may help moisturize dry eyes and make them feel better. You can buy them at most supermarkets and drugstores, and you don't need a prescription.
Consider using eye drops that say "preservative free" on the box. They may make your eyes feel less irritated.
If your eye doctor also prescribed medicated drops, don't use artificial tears within 15 minutes before or after your prescription drops.
Red eye
Your eye might look red or bloodshot after surgery. Some redness is normal, and it should go away on its own.
You might also notice a deep red spot on your eye. Most of the time, this is a normal reaction to surgery. It should go away within a few weeks.
Your ophthalmologist might prescribe medicated eye drops to help with eye redness and make your eyes feel more comfortable.
Call your ophthalmologist if: Your eye is very red, irritated or painful. You could be having an allergic reaction to your eye drops or another problem.
It feels like something is stuck in your eye
The little incision in your eye usually takes about a week to heal. Until then, the incision can make it feel like something is stuck in your eye.
It could take longer to fully heal if your surgeon used a stitch or if you already had dry eyes before surgery. Some people feel some discomfort for up to three months.
Normal discomfort should get better after you take prescribed pain medicine. If it doesn't, call your eye doctor.
Glare or halos around lights
You could see more glare or halos around bright lights after surgery. This is more common in low-light situations (like nighttime driving).
These side effects should go away on their own after a few months.
Sensitivity to light
You might feel like your eyes are a little more sensitive to light after surgery. This usually happens because your eye is dry, which is typically normal.
Long-term light sensitivity after cataract surgery is not normal. It could mean you have blepharitis or other dry eye problems.
How to help: Your eye doctor might recommend preservative-free artificial tears to ease the sensitivity.
Talk to an eye doctor as soon as you can if:
- You feel like your eyes are extremely sensitive to light.
- You automatically squint or close your eyes in bright light.
Eye floaters
It's often normal to see some eye floaters after surgery. These squiggly lines and spots can be annoying, but they're usually harmless.
Get immediate medical help if:
- You see floaters or flashes of light in bursts.
- It looks like a dark curtain is covering the side of your vision.
Droopy eyelid
It's common to have a droopy eyelid after cataract surgery. It usually gets better within six months. You might need to have surgery if it's still drooping after that.
Risk factors
You could be at a higher risk for complications if:
- You're older.
- You're female.
- You have macular degeneration.
- You have diabetic retinopathy.
- You have problems with your cornea.
- You've had a retinal detachment before.
- You've had a vitrectomy procedure before.
- You take alpha-blocker medicine (often used for high blood pressure).
- You have certain other medical conditions.
Make sure your surgeon has your full medical history and a list of your medications before your procedure.
Can I lower my risk of complications?
Some complications are out of your control. However, you can lower your risk for other complications by carefully following your surgeon's instructions before and after surgery.
Before surgery, you might need to:
- Stop taking medications that could affect surgery or healing.
- Use any prescribed medication as directed.
- Clean your eyelids and eyelashes with baby shampoo.
- Abstain from eating or drinking anything.
- Arrange for a ride home from surgery (you won't be able to drive yourself home).
After surgery, you'll probably need to:
- Relax for the first few days.
- Wear an eye patch or special glasses for a while.
- Use any prescribed eye drops as directed.
- Avoid touching or rubbing your eye for a few weeks.
- Avoid bending over or lifting heavy things for a few weeks.
- Avoid swimming for two to six weeks.
- Avoid driving or flying until your eye doctor says you can.
- Go to your scheduled check-ups (the doctor uses these appointments to make sure your eye is healing well).
When to get help
Some cataract surgery side effects are normal. You might feel like your eye is dry or your vision is a little blurry, among other mild symptoms.
If symptoms are severe or last longer than they should, you may have a complication that needs treatment.
Talk to an eye doctor right away if:
- The pain is severe and doesn't get better with pain medicine.
- Your vision seems much worse than before.
- You have any vision loss.
- Your eye is very red.
- Pus or drainage is coming from your eye.
- You see lots of new floaters or flashes of light.
- A dark shadow is covering part of your vision.
- You're sick to your stomach or throwing up.
- You have a fever of 100.4°F or higher.
If you aren't sure if what you're feeling is normal, talk to your eye doctor. They'll help you decide what to do next.
SEE RELATED: June is Cataract Awareness Month