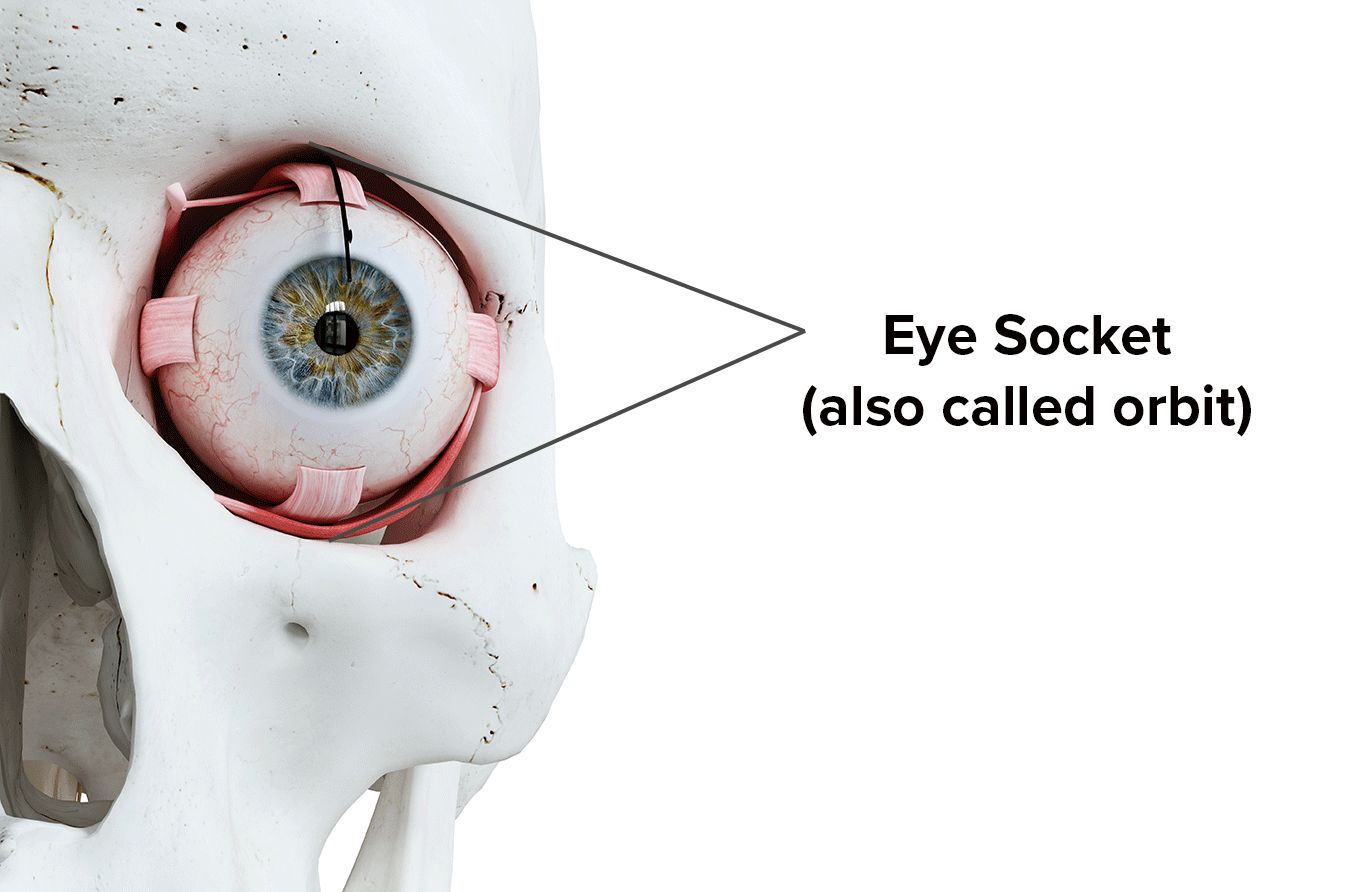
Eyes are designed to last from birth through old age, so their delicate contents need to be protected. The eye socket (or orbit) is tasked with this responsibility. It keeps the eyeball shielded and in place as the eye adapts to a constantly changing environment over its lifetime.
Several other features of the eye assist with this job of keeping it safe:
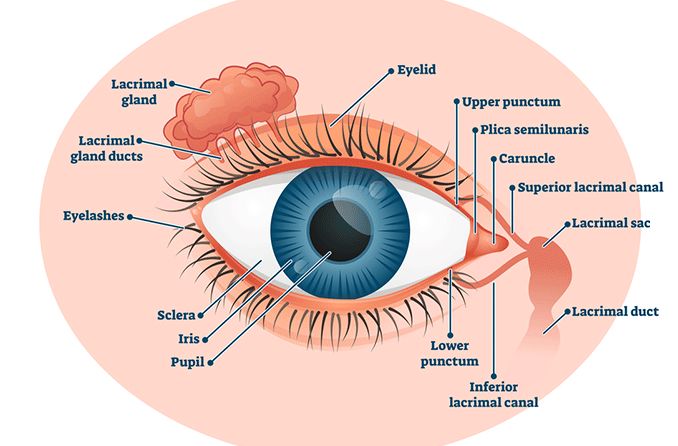
- Eyelashes keep the eye moist and shield it from foreign particles.
- Eyelids block debris and bright light.
- Conjunctiva provides the sclera (the white of the eye) with a layer of protection.
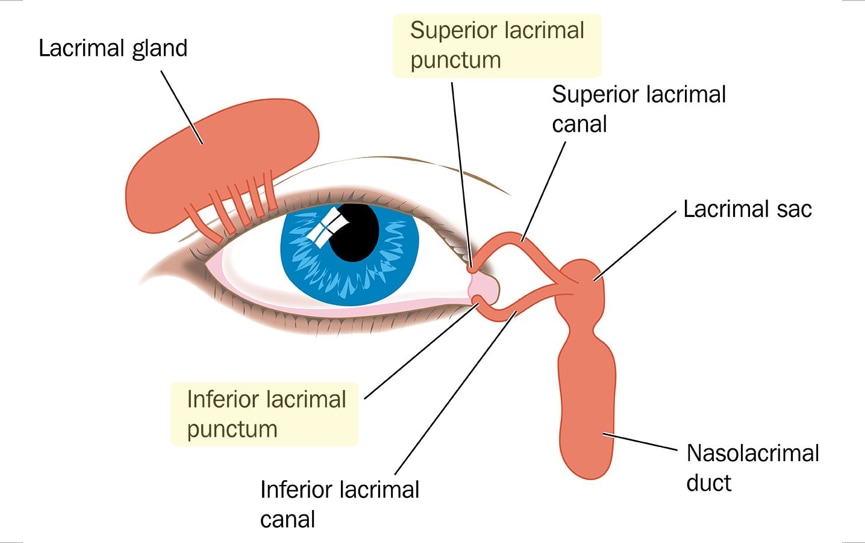
- Lacrimal glands create tears to lubricate the eye and wash out irritants.
But it’s the orbit that provides a solid structure to support and house all these features.
Eye socket anatomy
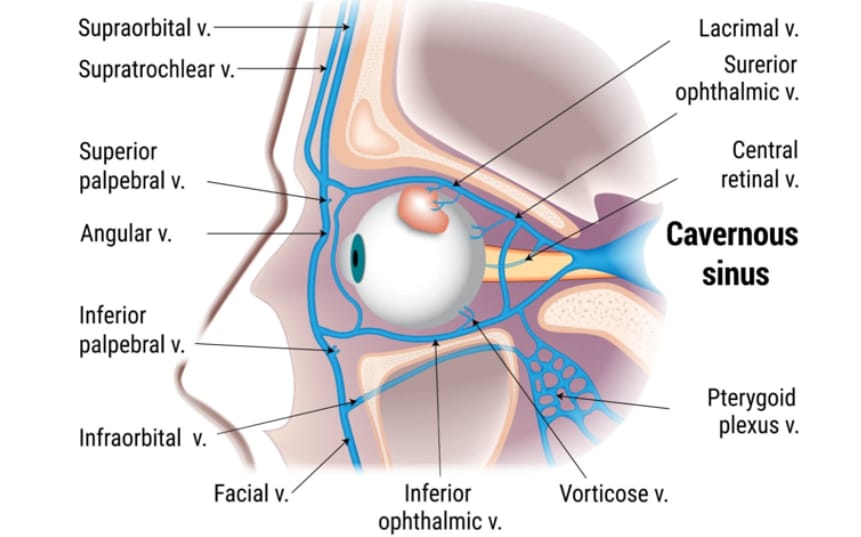
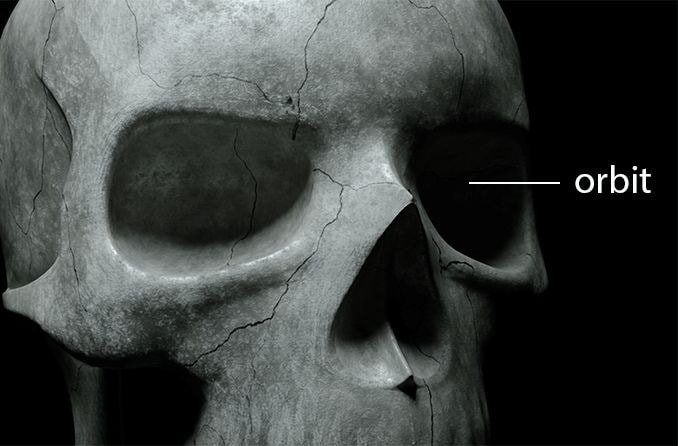
The orbit is the part of the skull surrounded by the forehead, temple, cheeks and nose. It’s approximately the size of a golf ball, with a volume of about 30 cubic centimeters (about 2 tablespoons). In addition to the globe (the eyeball), the eye socket contains blood vessels, nerves, muscles and fat.
It’s made up of seven orbital bones: frontal, sphenoid, zygomatic, maxillary, lacrimal, ethmoid and palatine. Together, they form a cone-like shape that opens outward. At the tip of the cone (at the back of the eye socket) is the opening to the optic canal, and at the base of the cone (the front of the eye) are the sclera and cornea.
Eye socket bones are arranged into a roof, floor and walls that range in structure from thick (at the back and front) to thin (floor and walls). Several openings in the orbital bones allow for nerves, veins, arteries and ganglion to pass through.
SEE RELATED: Osteo-Odonto Keratoprosthesis Surgery (OOKP)
Pain in the eye socket
Outward signs of conditions that might cause pain in eye sockets can be obvious — bruising, swelling, a bulging (exophthalmos) or sunken (enophthalmos) appearance of the eye or red-colored sclera. Symptoms are often present as blurriness, numbness, restricted eye movement, light sensitivity (photophobia) or nausea.
Eye socket pain can come from:
- Surface of the eye (ocular pain) – You may experience redness, wateriness, burning, itchiness or irritation. Any number of things can cause ocular pain, from dry eyes, eye strain and pink eye (conjunctivitis) to a corneal scratch, chemical exposure, inflammation of the iris (iritis) and more.
- Below the surface of the eye (orbital pain) – You could have double vision (diplopia) or feelings of stabbing, throbbing or elevated eye pressure. Possible causes of orbital pain include migraines, toothaches, sinusitis, vitreous hemorrhages and paralysis of eye muscles (ophthalmoplegia), among other things.
Pain in one or both eye sockets is most commonly caused by injury or trauma, specifically from the fracturing of the orbit. Motor vehicle crashes, accidental falls or a hard blow to the face from a baseball can all cause trauma to the eye. Accidents account for 85% of cases of traumatic eye injuries.
If you’re experiencing intense or prolonged pain or discomfort in or around your eye socket, contact an eye doctor right away. Any damage to the soft tissue contained in the orbit should be monitored or treated.
Broken or fractured eye socket
Broken and fractured mean the same thing when it comes to bones — both words refer to a break that results from excessive pressure on a bone. The severity of a break ranges from a complete break to a partial fracture. Any of the bones in the eye socket can be broken.
A broken eye socket (also called orbital fracture) can happen when the bones around the eyeball are severed, shattered, cracked or stressed. Types of eye socket fractures include:
- Orbital rim fracture – This fracture occurs to the rim bones of the eye socket, most likely displacing these bones. Because this kind of injury requires a lot of force, it can not only affect the contents of the orbit but also extend to other parts of the face and head, such as the cheekbone, upper jaw and forehead. Zygomatic (cheekbone) fractures account for 25% of all facial fractures.
- Orbital floor fracture – This fracture happens to the floor bone of the eye socket. With a direct fracture, both the rim and the floor bones break. With an indirect fracture (or blowout fracture), the floor bone fractures but the rim bones stay intact. In this case, the fractured floor bone can trap eye muscles or other contents of the orbit, keeping the eye from moving normally.
- Trapdoor fracture – This fracture refers to a rare instance in which a floor bone pivots open, traps soft tissues and then pivots back, cutting off blood supply to the tissue. Children are commonly at risk for this type of injury since their bones are more elastic and not fully developed.
Any time an eye socket is broken or fractured, eye movement can be affected because the eyeball may be out of position, causing pressure and swelling. It is recommended to seek immediate medical attention, as this can escalate into a serious situation that may require surgery.
Empty eye socket
An eye may be removed from an eye socket for several reasons, such as from trauma, injury, tumors or diseases like glaucoma or diabetes. Children can have a rare birth defect in which eyeballs are absent (anophthalmia).
Surgery to remove part or all of the eye from the eye socket includes:
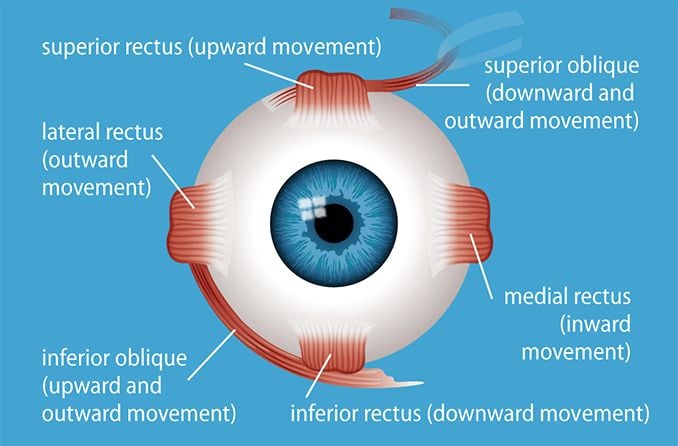
- Enucleation – In this procedure, all extraocular muscles (muscles that control eye movement) are detached, the optic nerve is cut and the eyeball removed. If a prosthetic eye is being inserted, the extraocular muscles are attached to it and the soft tissues are placed over the top.
- Evisceration – This involves removing the intraocular structures (iris, retina, vitreous, etc.) but keeping the extraocular muscles, sclera and optic nerve. An implant is inserted, extraocular muscles attached to it and soft tissues are placed over the top.
- Exenteration – This surgery removes everything in the eye socket, leaving it completely empty. An artificial eye (prosthesis) may be recommended.
Seeing your eye doctor
Keeping up with the health of your eyes is important for long-lasting vision. If you’re experiencing any signs or symptoms of eye socket pain or notice any dramatic changes in your vision, it is recommended to make an appointment with an eye doctor for a comprehensive eye exam. If necessary, your eye doctor can recommend several non-invasive tests, such as a slit lamp exam, air puff test, X-ray or computed tomography (CT) scan, to help determine the cause.