What is ocular hypertension?
Ocular hypertension means the pressure in your eyes is higher than normal. If left untreated, high eye pressure can cause glaucoma and permanent vision loss. The medical term for the pressure inside the eye is intraocular pressure, or IOP.
An estimated 4% to 10% of people over age 40 have high eye pressure. About a quarter of them will develop glaucoma due to elevated IOP.
Detecting ocular hypertension
Ocular hypertension has no obvious signs or symptoms, such as eye pain or red eyes. The only way to tell if you have high eye pressure is to have a comprehensive eye exam by an optometrist or ophthalmologist.
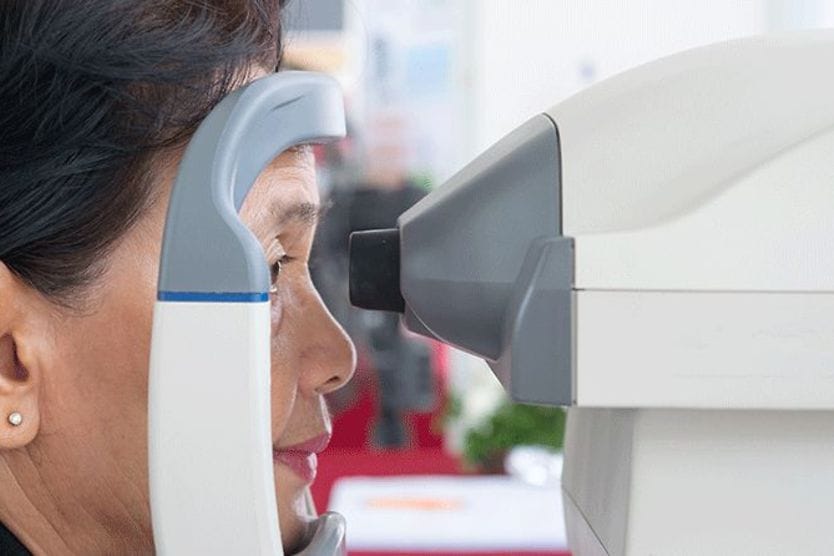
During a comprehensive eye exam, your eye doctor will measure your IOP with an instrument called a Goldmann tonometer. You might also have your eye pressure checked with an air puff test (a type of non-contact tonometry). Both of these IOP measurements are quick and painless.
Intraocular pressure is measured in millimeters of mercury (mm Hg). Normal intraocular pressure is 12 to 22 mm Hg, and it varies throughout the day. An IOP that is consistently higher than the normal range is considered elevated and requires additional testing to make sure there is no damage to the optic nerve. These tests can include a visual field test, gonioscopy and optic nerve imaging.
High eye pressure significantly increases your risk of damage to the optic nerve, causing glaucoma and permanent vision loss.
If you have ocular hypertension, your eye doctor may recommend further tests to check for signs of glaucoma. These can include a visual field test, a gonioscopy exam and retina imaging.
READ NEXT: Hypotony: Low eye pressure
What causes high eye pressure?
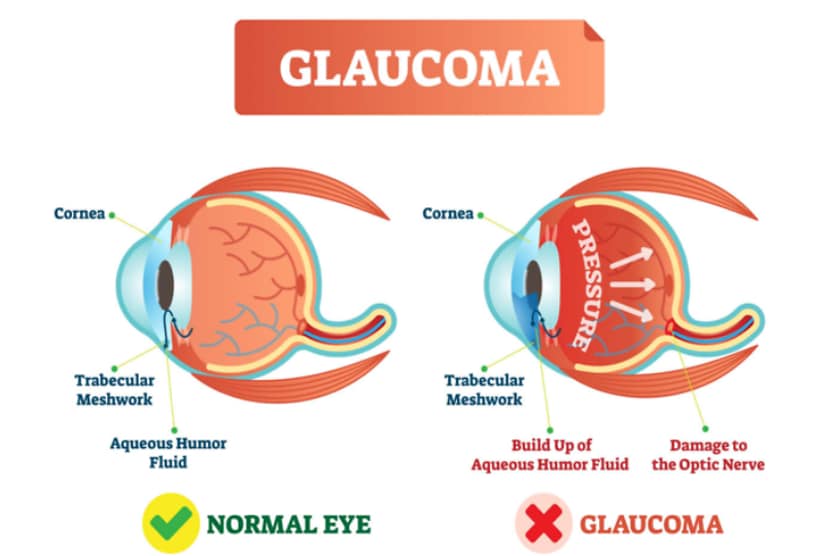
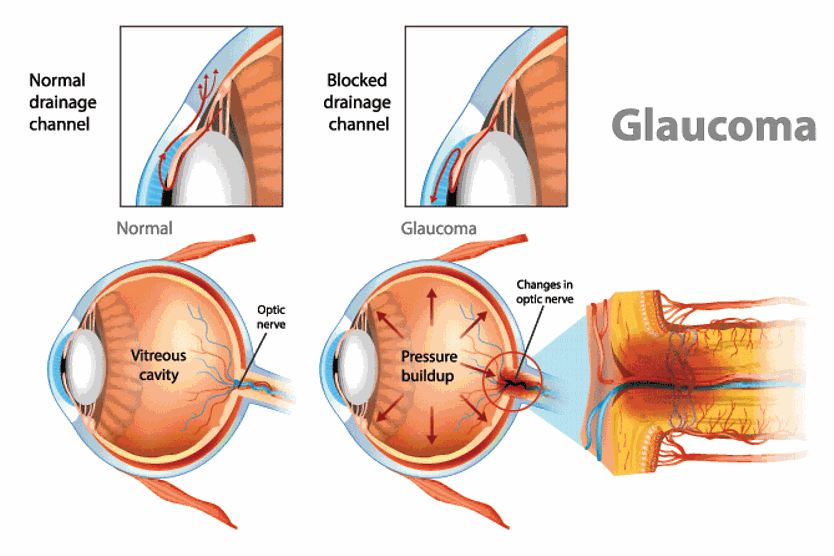
Factors that cause or are associated with ocular hypertension are virtually the same as the causes of glaucoma. In most cases, it’s related to the flow of aqueous humor through the eye.
The aqueous is a clear fluid that is produced in the eye by the ciliary body, a structure located behind the iris. The aqueous flows through the pupil and fills the anterior chamber of the eye, which is the space between the iris and the cornea. From there, it leaves the eye through tiny drainage channels located at the angle where the white (the sclera) meets the colored part of the eye (the iris).
High eye pressure is usually due to changes in this flow. These can include:
Inadequate aqueous drainage
High eye pressure can occur if the aqueous is produced at a normal rate but drains too slowly from the eye. Poor drainage is the most common cause of high eye pressure.
Excessive aqueous production
If the aqueous forms faster in the eye than it can drain out, the pressure inside the eye increases, causing ocular hypertension.
But, like with glaucoma, there usually isn’t a specific known cause for the changes in aqueous flow. Some of the known causes include:
Certain medications
Some medications can have the side effect of causing ocular hypertension. Steroid medicines used to treat asthma and other conditions have been shown to increase the risk of high eye pressure.
Be sure to tell your eye doctor if you are using steroid eye drops for any reason.
Eye trauma
An injury to the eye is another thing that can damage the angle, affecting the balance of aqueous production and drainage. Inflammation and damage inside the eye due to an injury can lead to ocular hypertension. Sometimes this can occur months or years later, even when injuries seem minor.
During your routine eye exams, be sure to mention to your doctor if you have experienced any recent or past eye injuries.
Other eye conditions
Ocular hypertension has been associated with a number of other eye conditions, including:
- Pseudoexfoliation syndrome (PXF)
- Pigment dispersion syndrome (PDS)
- Uveitis
- Ocular tumor
- Large cataracts
- High degree of nearsightedness or farsightedness
If you have any of these conditions, your eye doctor may recommend that you have more frequent eye exams and eye pressure measurements.
Race, age, family history and other health conditions can also play a role in your risk for ocular hypertension and glaucoma. Though anyone can develop high eye pressure, the following groups are generally at greater risk:
- Non-white populations
- People over age 40
- Anyone with a family history of ocular hypertension or glaucoma
- People with high blood pressure and/or diabetes
- People living with chronic stress
There is also growing evidence that menopause-related hormone changes may increase the risk of ocular hypertension.
Ocular hypertension treatment
Ocular hypertension, by definition, means there is no glaucomatous damage to the optic nerve. Because of this, ocular hypertension is usually not treated, however is monitored with follow up visits with special testing on a schedule.
However, there are instances when it is too risky to wait for treatment. These instances occur when the pressure is high enough that it can be predicted with some certainty that optic nerve damage will happen in the near future.
When a doctor deems the risk of optic nerve damage (and therefore glaucoma) is high enough based on a combination of factors (including intraocular pressure over 30), treatment may be started before any optic nerve damage has occurred.
In some cases (or if eye drops are ineffective in reducing your IOP), your eye doctor might recommend other glaucoma treatment measures, including laser glaucoma surgery, to treat high eye pressure.
Because elevated eye pressure increases your risk of glaucoma, be sure to follow your eye doctor’s advice. Have your IOP checked at recommended intervals to monitor the condition.
Medications
Often, ocular hypertension doesn’t need to be treated. Your eye doctor will likely only recommend treatment if you’re at moderate to high risk for glaucoma. In those cases, treatment is typically with the same types of eye drops used to treat glaucoma. They can include:
- Prostaglandins
- Beta blockers
- Carbonic anhydrase inhibitors
- Alpha agonists
- Rho-kinase inhibitors
Lifestyle modifications
Your eyes are closely connected to your overall health. Sticking to a healthy lifestyle is an important factor in eye health, as well as in managing ocular hypertension. Some of the key lifestyle modifications for healthier eyes and vision include:
- Keep other conditions, such as diabetes or high blood pressure, under control.
- Eat a balanced diet that includes plenty of leafy greens, vitamin C, omega-3 fatty acids, vitamin E and vitamin B3.
- Have a regular routine of moderate cardiovascular exercise or activities.
- Stay hydrated throughout the day (vs. drinking too much water all at once).
- Quit smoking and any other nicotine habits.
- Keep your head elevated slightly while sleeping.
- Take regular breaks while reading or using digital screens.
- Avoid wearing tight neckwear, such as ties, as this may increase your eye pressure.
Living with ocular hypertension
Because ocular hypertension doesn’t cause any symptoms, yearly eye exams are critical. This is especially true if your eye doctor has already told you that your eye pressure is high.
For many people, high eye pressure never develops into glaucoma. However, it is the most important risk factor. It’s also the easiest risk factor to modify. Seeing your eye doctor regularly and following their advice for any treatments are optimal to help prevent vision loss from glaucoma.
READ MORE: What is hypertensive retinopathy