
Related Medical Conditions
Often, issues with our eyes can stem from something else that may seem totally unrelated. Learn about some of the underlying conditions can have an effect our eyes
Discover the 15 different ways heart health can affect your eyes and vision.
A stroke can result in many changes to vision, including visual field loss, double vision, and difficulties with visual perception and visual memory.
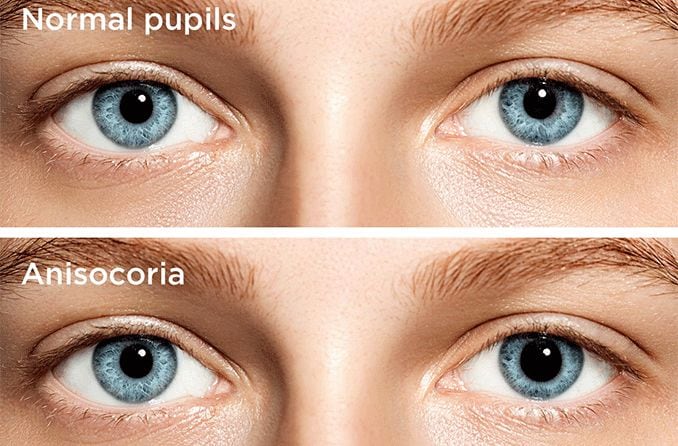
Adie’s tonic pupil is a neurological condition that causes the pupils to react to light differently in one eye than the other.

Akinetopsia, or motion blindness, affects a person’s ability to detect objects in motion. Learn more about this visual processing disorder.

Alice in Wonderland syndrome is a set of symptoms involving a change to personal and visual perceptions. Learn more about this condition.

Learn about how anti-anxiety drugs, such as Xanax, Paxil and Valium, can cause eye-related side effects such as dry eye and blurry vision.

Learn the eye-related side effects of antidepressants, such as dry eye, dilated pupils, blur, eye twitch, and, less commonly, acute angle-closure glaucoma.
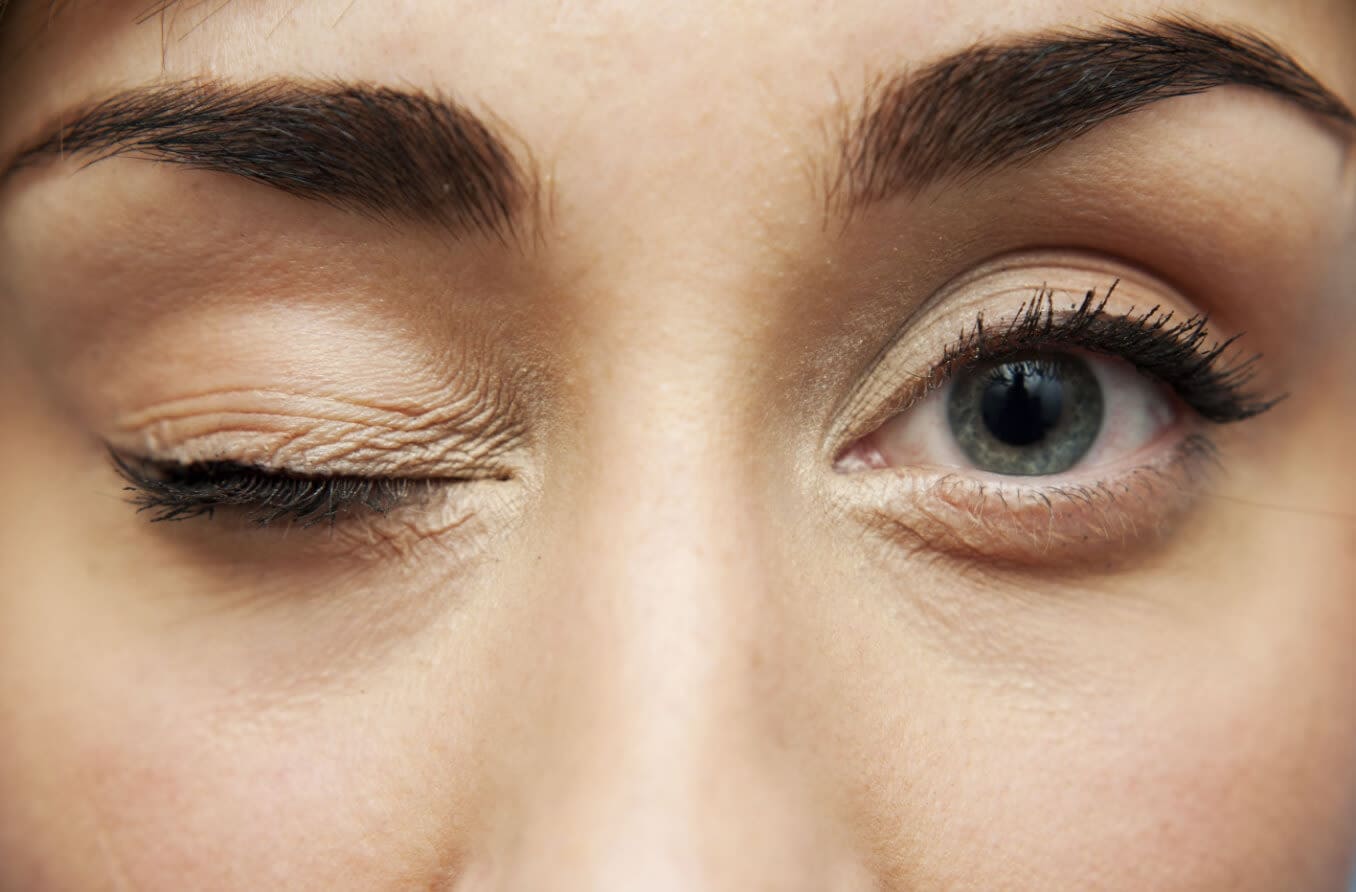
Uncover the intricacies of apraxia of eyelid opening, its causes and symptoms, and find out how to cope with this unique eye condition.

Argyll Robertson (AR) pupil is a condition causing small pupils and light–near dissociation. Learn about the causes, diagnosis and treatment of AR pupil.

Axenfeld-Rieger syndrome (ARS) is a rare, inherited condition that mainly affects the eye. Learn more about its symptoms, causes, diagnosis and treatment.
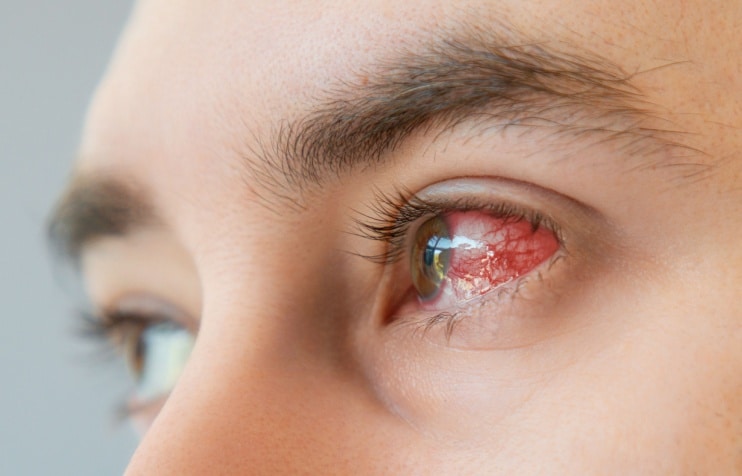
Behçet's disease is an autoimmune condition that causes blood vessel inflammation. Learn how it can affect the eyes and other parts of the body.
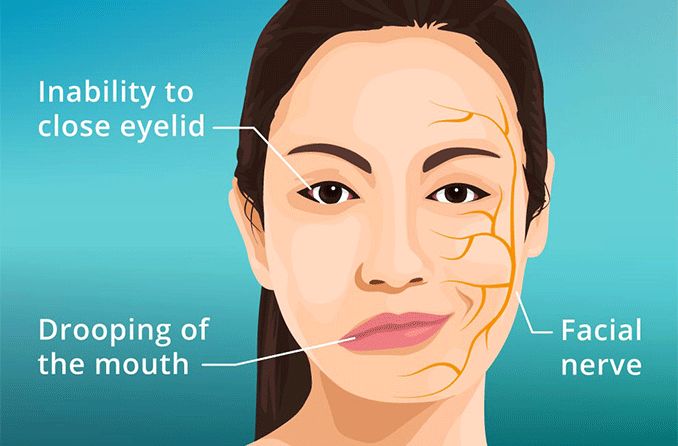
Bell’s palsy is temporary facial muscle weakness or paralysis caused by inflammation or compression of the facial nerve.
Studies suggest that people with blood type A, B or AB have an increased risk of cardiovascular disease, which can increase the risk of some eye diseases.
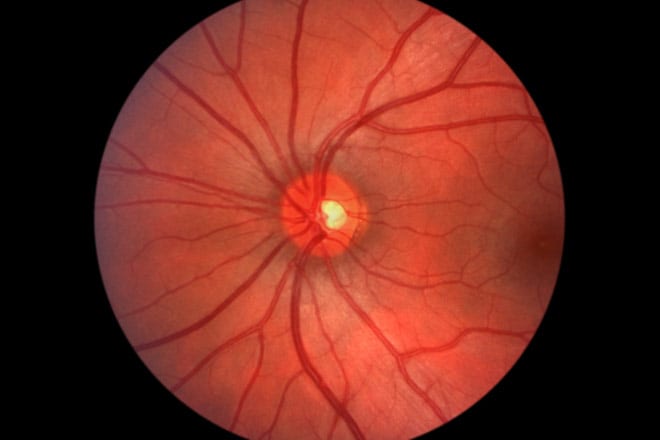
Learn about CMV retinitis, a sight-threatening complication of HIV/AIDS, chemotherapy & bone marrow transplants. Discover cytomegalovirus symptoms & treatment.
Cogan’s syndrome is a chronic autoimmune disease of the eyes and inner ears. Learn about its symptoms, causes and various ways to treat it.
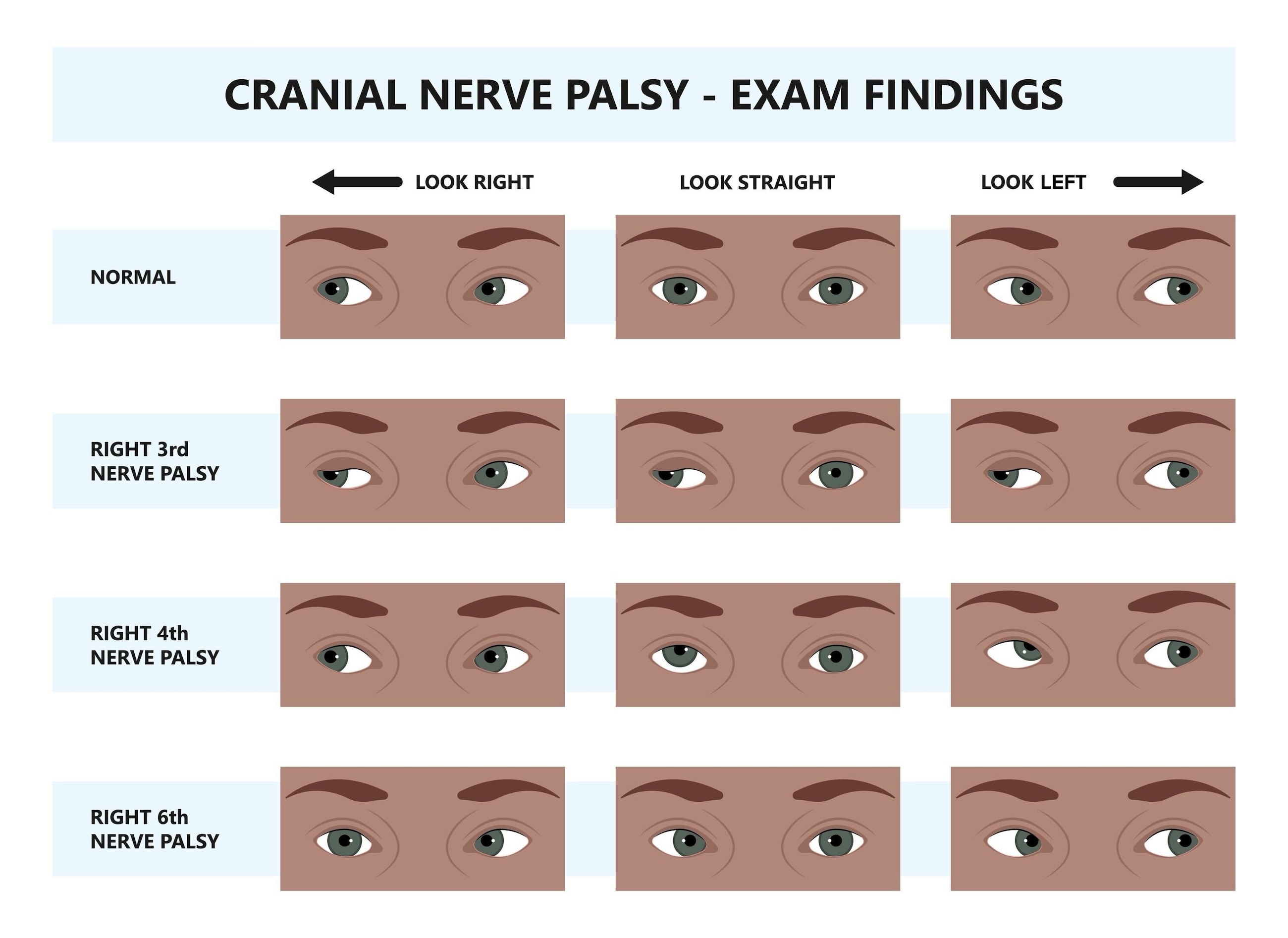
Learn all about cranial nerve palsies and how they affect the eye — visual symptoms, causes, treatment and when to see a doctor.

Eyelid psoriasis is an autoimmune skin condition. Learn how it can be managed with coping strategies, lifestyle choices and medication.
The U.S. Food and Drug Administration approved the first drug to treat thyroid eye disease, also called Graves’ eye disease. thyroid eye disease is associated with proptosis (eye bulging), diplopia (double vision), blurred vision, pain, inflammation and facial disfigurement.

For Lupus Awareness Month, discover how this autoimmune disease affects the eyes and vision.

Graves’ disease is an immune system disorder that causes hyperthyroidism, which can affect many parts of the body, including the eyes.
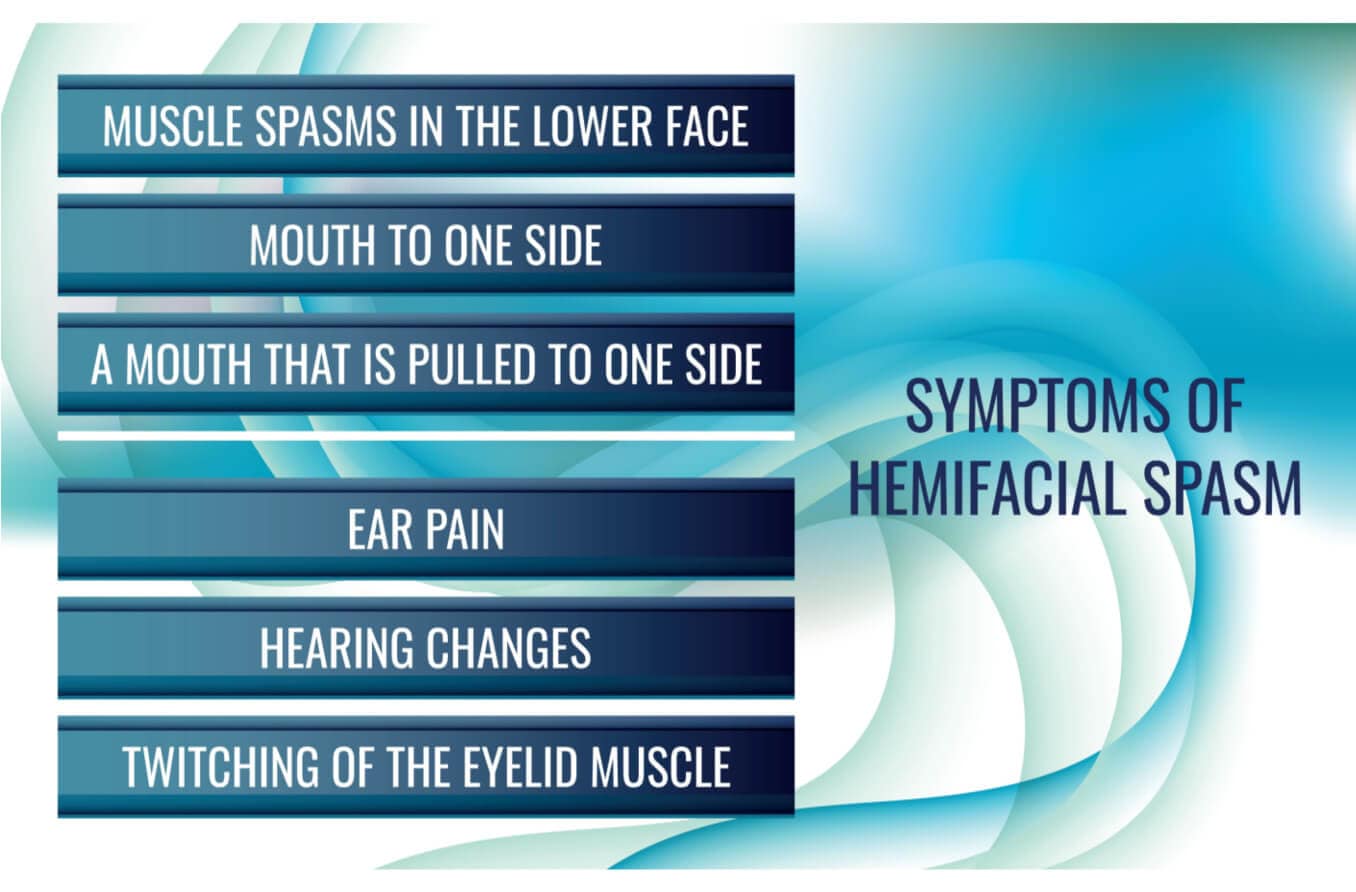
Hemifacial spasm is a chronic disorder causing painless, uncontrolled twitching on one side of the face. Learn what causes it and how it is treated.

Horner’s syndrome is a rare disorder that causes the pupil in one eye to constrict and the eyelid to droop. It may be the result of an underlying condition.

Learn about common eye problems that many people with Down syndrome experience, including their symptoms and treatment options.
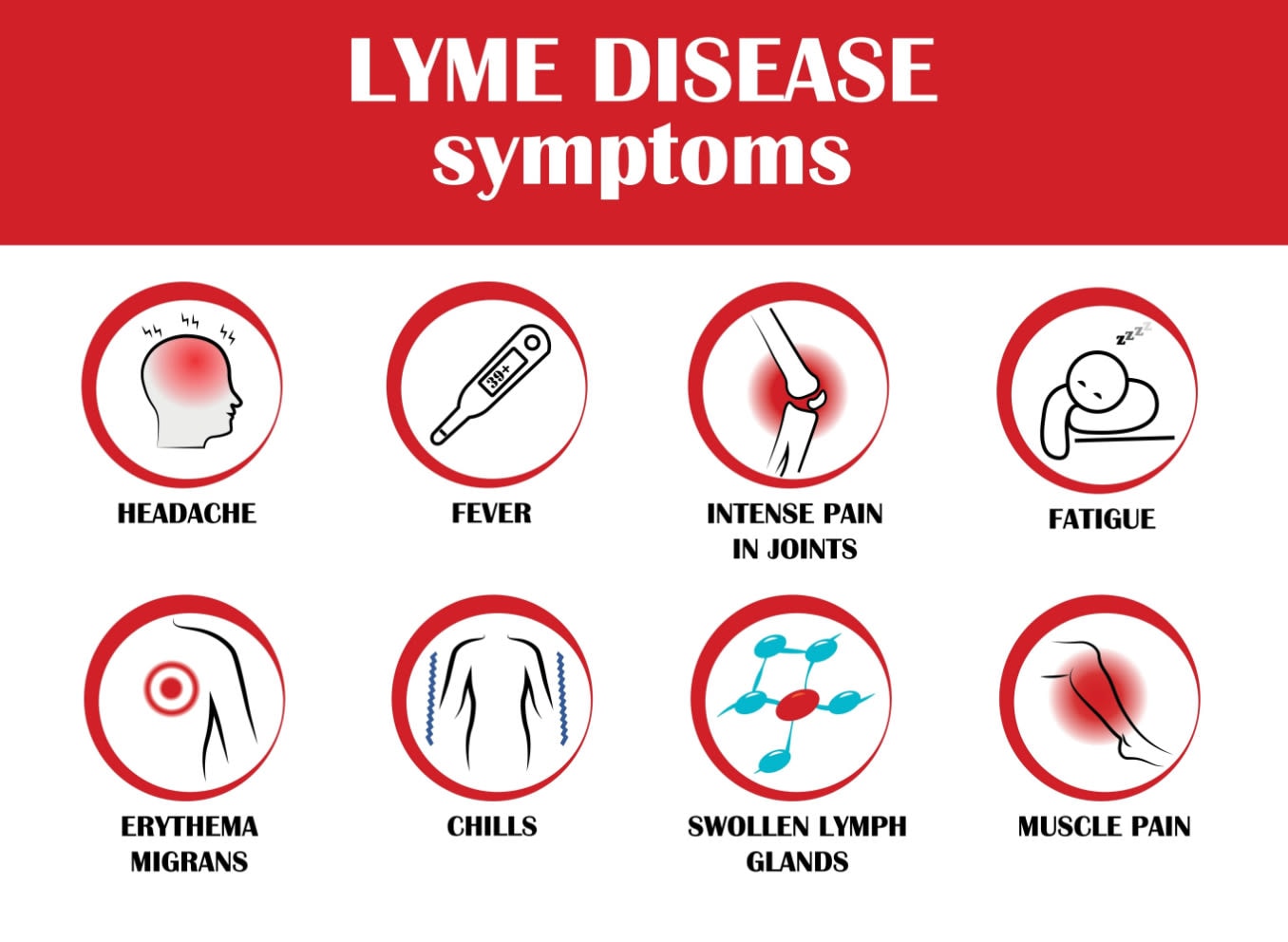
Discover how Lyme disease can affect the eyes, common symptoms, potential complications and vision care tips for those affected.

Dehydration can impact your eyes and vision. Learn the signs and symptoms, causes, and treatments for this common condition.

Explore the effect mental health conditions, like depression, can have on eyesight.

Learn how Parkinson's disease affects eyesight, causing vision changes like double vision and dry eyes. Explore causes and management strategies.

Albinism is a rare genetic condition that can affect a person’s vision and the pigmentation of their skin, hair and eyes in multiple ways.

Leprosy can affect your eyes and vision in different ways. Learn more about these eye conditions and what you can do to protect your eyesight.
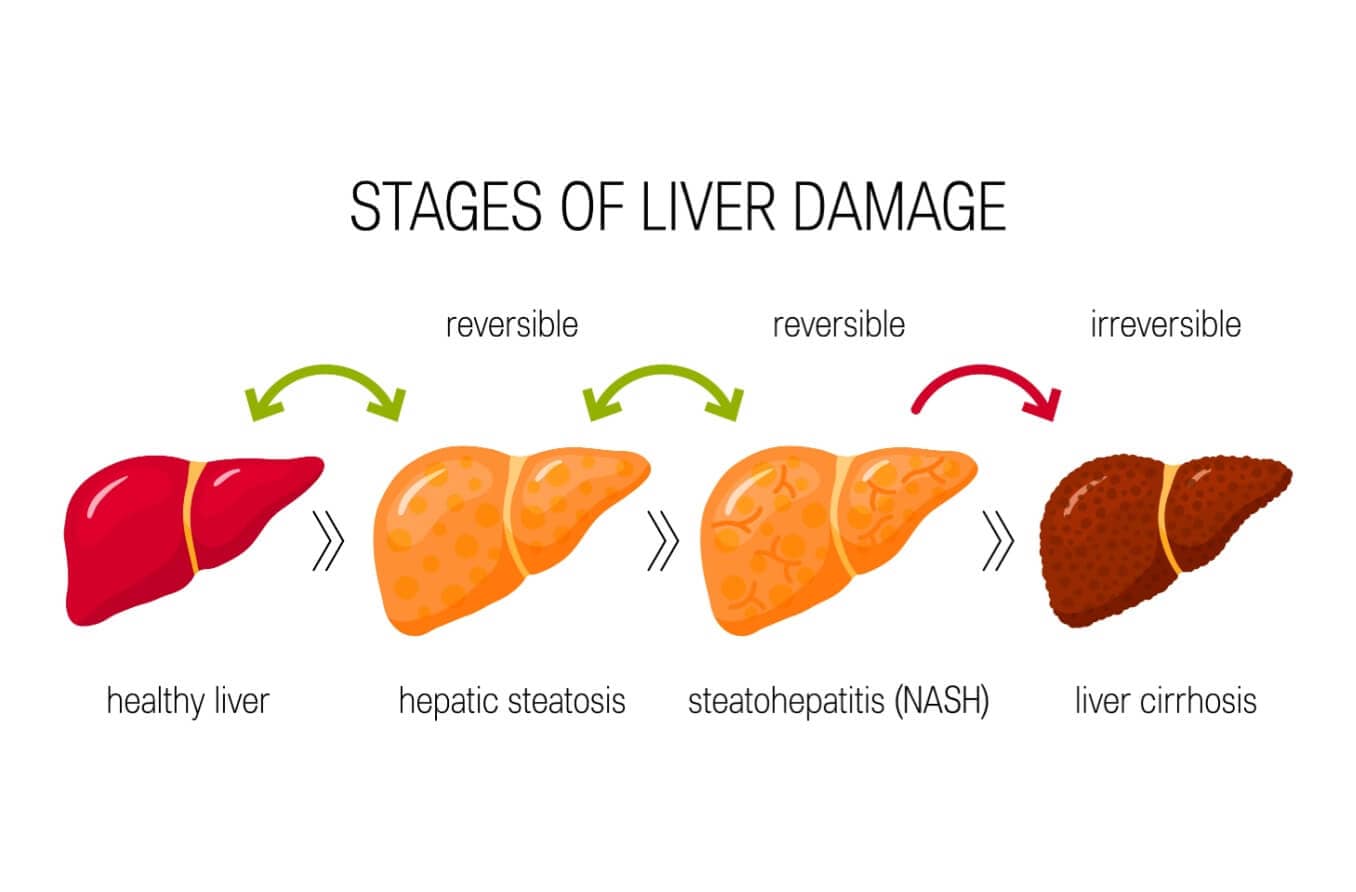
Observe World Hepatitis Day on July 28 by learning how the eyes can reflect liver health.

Do you know how measles affects eyesight? All About Vision reveals how measles can put your child's eyesight at risk through keratitis, and corneal scarring.

Meth is a highly addictive drug that damages the central nervous system. It can have short-term and long-term impacts on eye health and vision.

Sinus infections and other sinus issues can cause pain around and behind the eyes, along with eyelid swelling and other eye issues.

Stress can cause several vision issues, include eye twitching, blurry vision, headaches, watery or dry eyes, dizziness, eye strain and sensitivity to light.
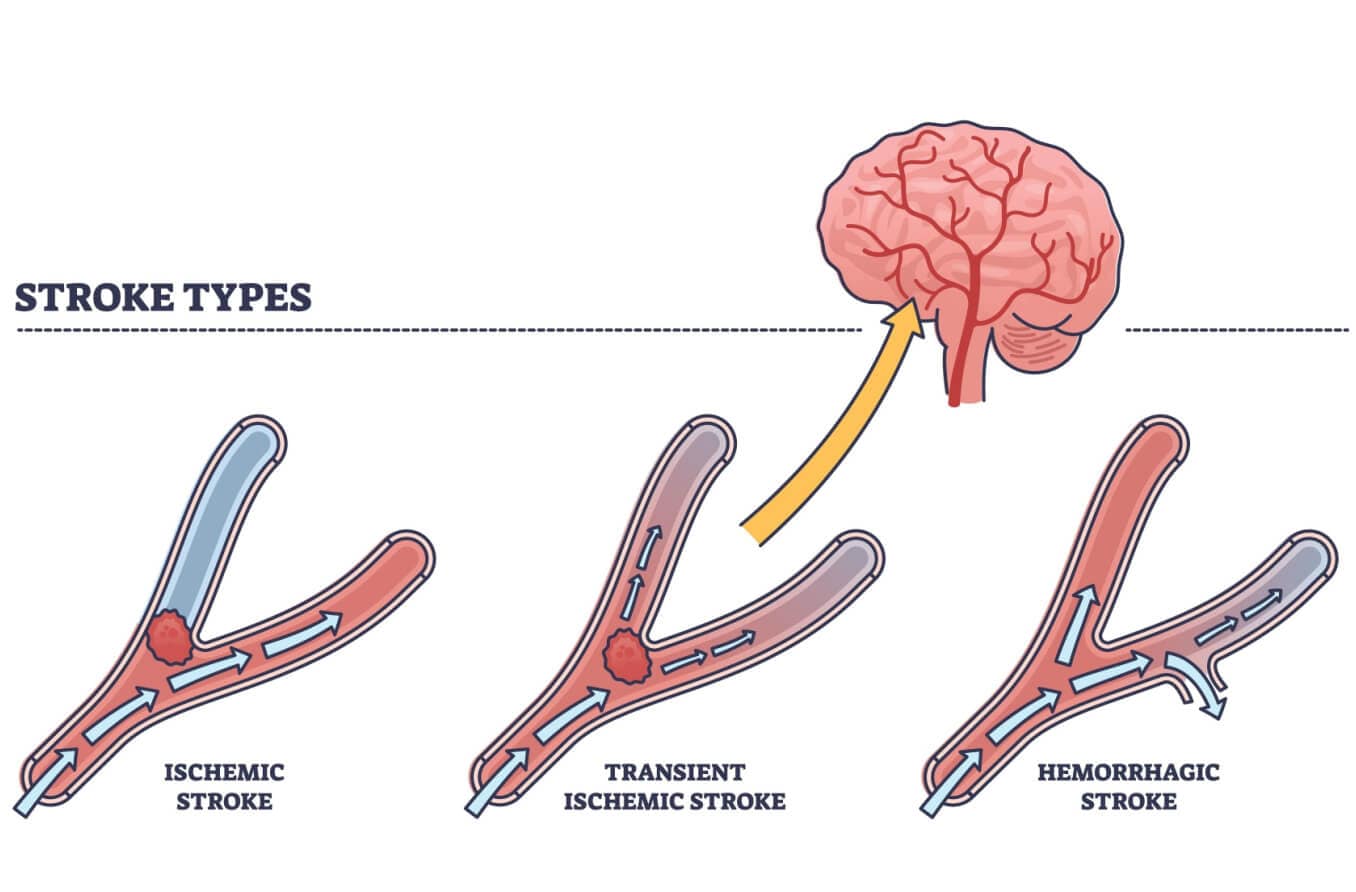
A TIA, or mini-stroke, is a sudden and brief blockage of blood supply to the brain that can cause temporary vision issues, weakness, numbness and confusion.

Hypertelorism describes an excessive width between a person’s eye sockets. Learn its causes as well as how it’s diagnosed and managed.
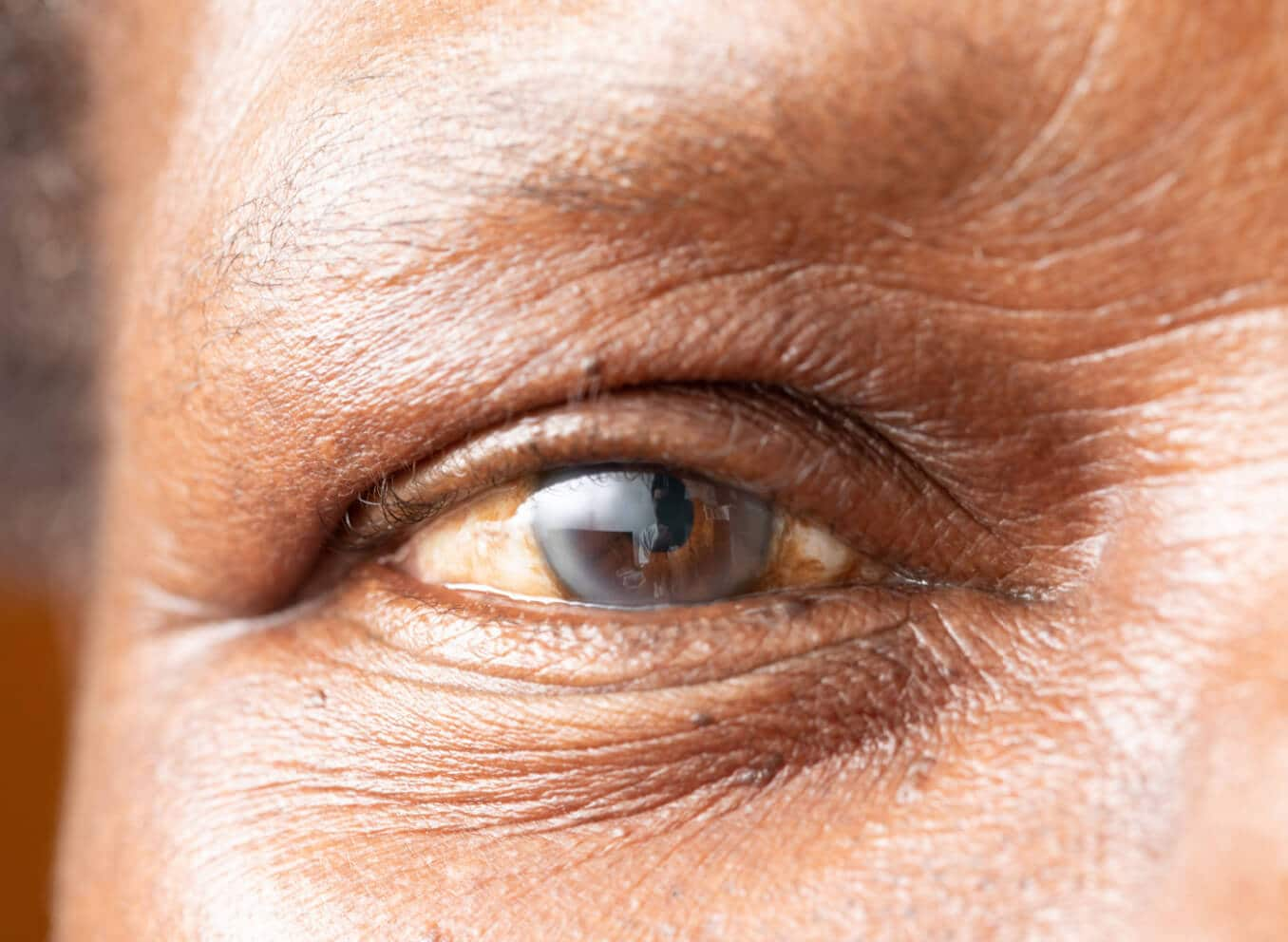
Intraoperative floppy iris syndrome (IFIS) is a type of small pupil syndrome brought on by the use of certain alpha-blockers.
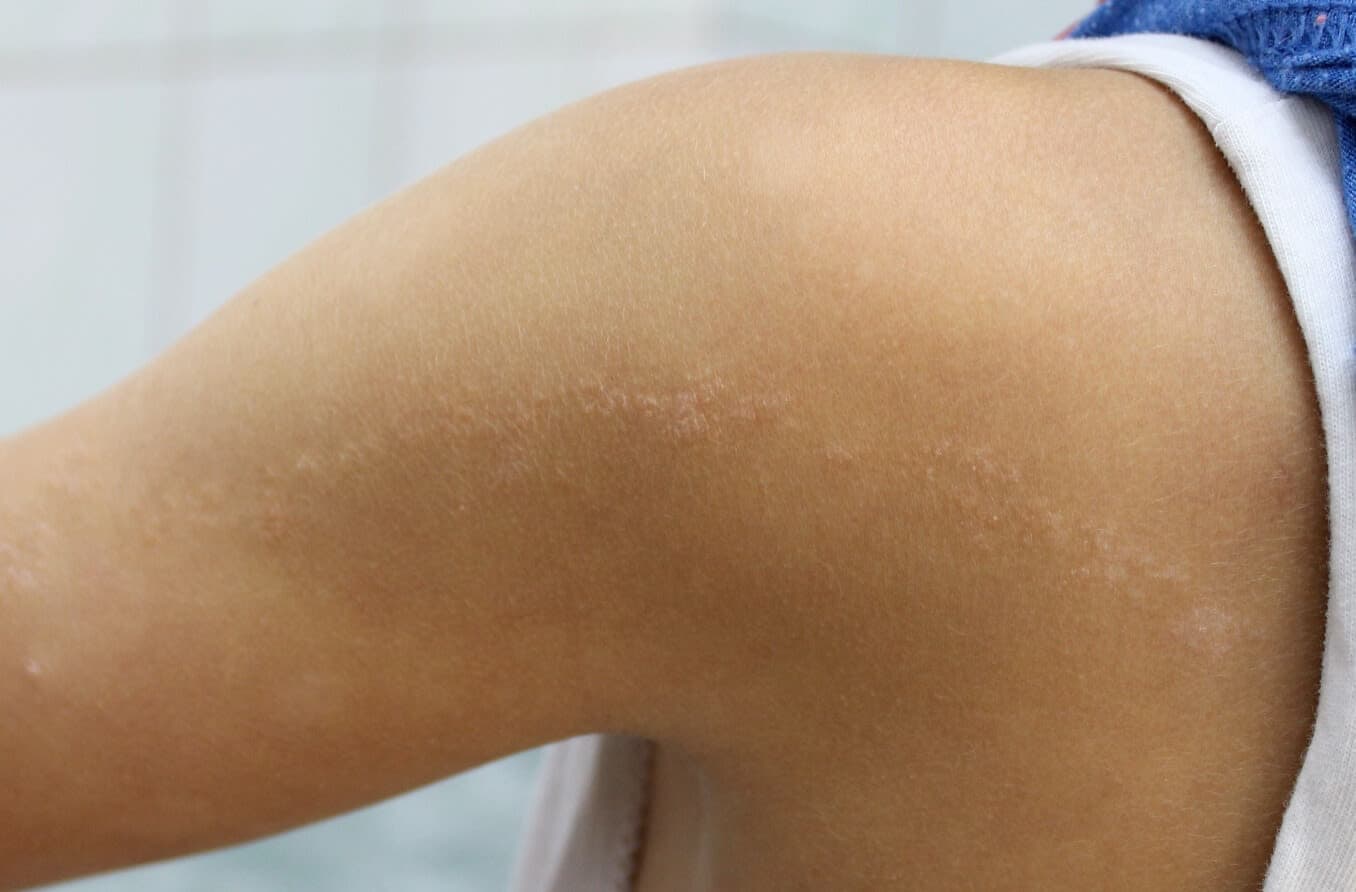
Linear nevus sebaceous syndrome is a rare congenital condition that can impact ocular development. Learn more about the symptoms and treatment.

Madarosis is the loss of eyebrow or eyelash hair. It is typically due to an underlying eye, skin or health condition and can be temporary or permanent.

Learn about obstructive sleep apnea and the eye conditions linked to this sleep disorder. Find out how you can get treatment and protect your vision.
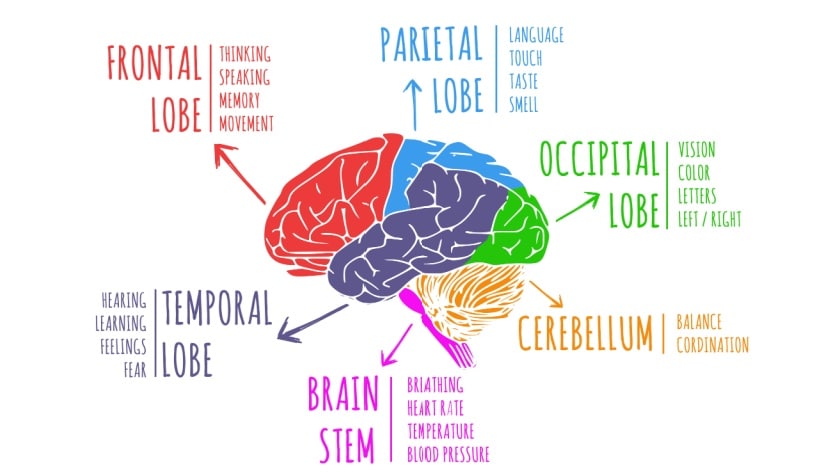
Occipital lobe seizures, a rare type of seizure, can affect vision and other brain functions. Learn about their symptoms, causes and treatment options.
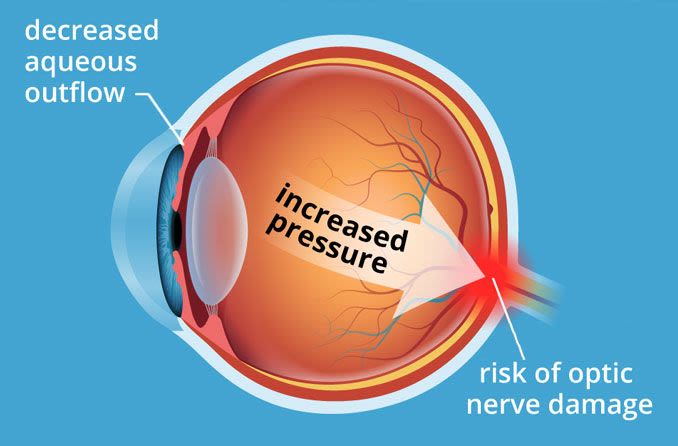
Ocular hypertension (high eye pressure) significantly increases your glaucoma risk. Keep up with routine eye exams that include an eye pressure test.
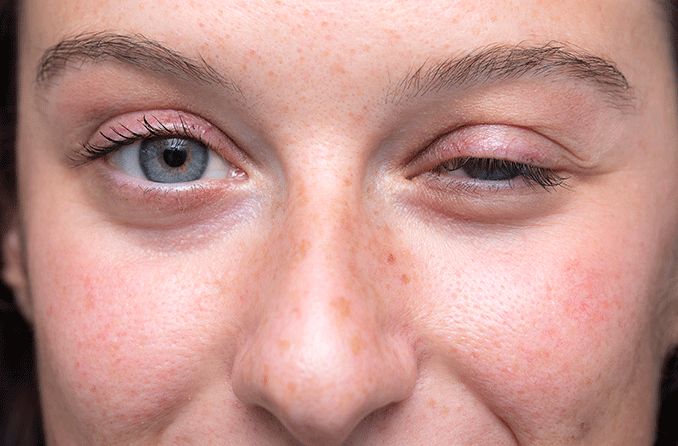
Ocular myasthenia gravis (MG) is an autoimmune disorder causing muscle weakness around the eyes. Learn about the cause, symptoms and treatments of MG.
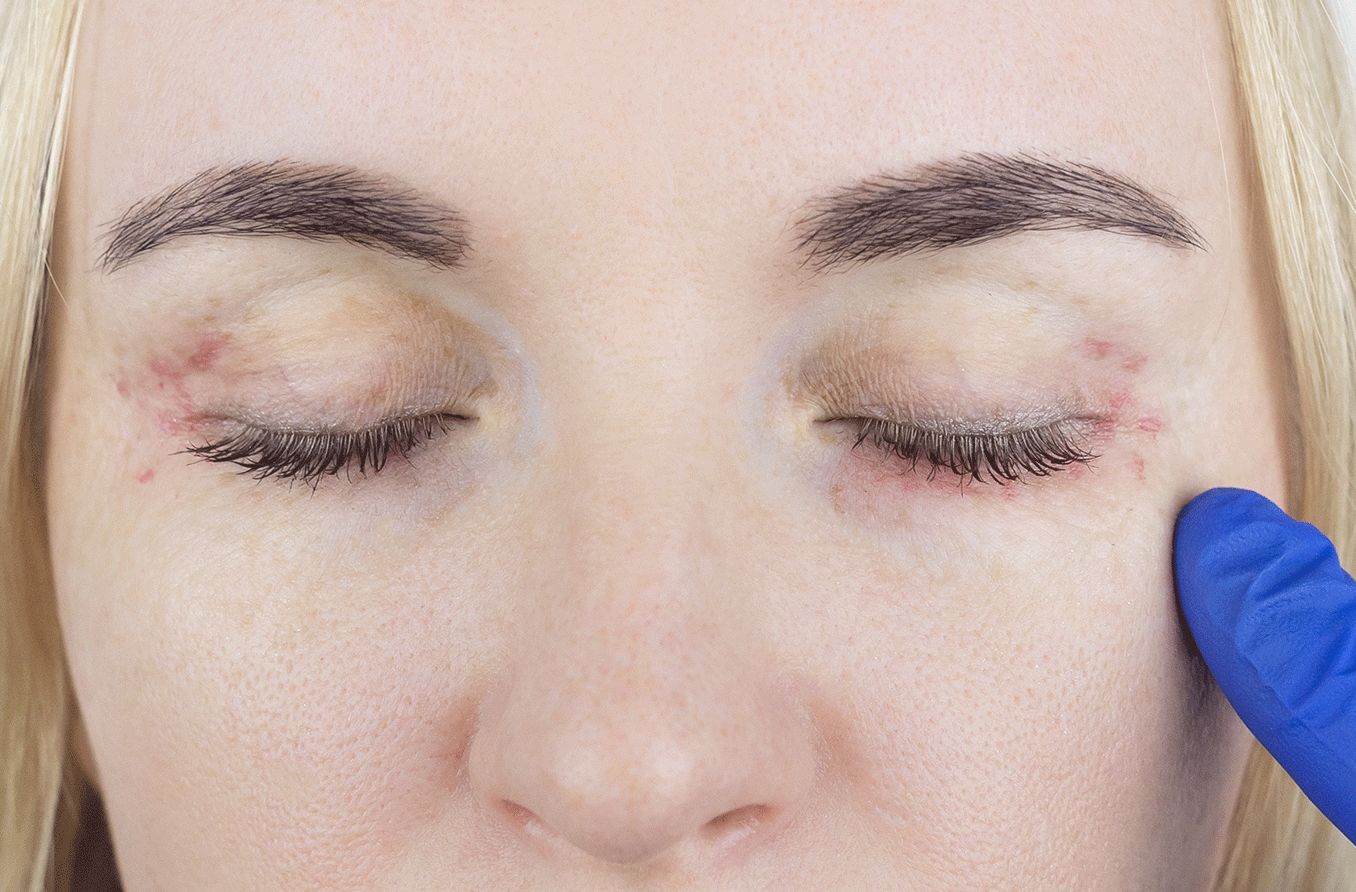
Ocular rosacea is very common in people with this skin condition; learn about causes, such as stress, and treatments.

Oscillopsia is the illusion that the world is shaking, jittering or moving in ways it isn’t. Read on to learn more about this condition.

Palinopsia are a type of long-lasting or recurring visual afterimage. Learn more about the causes and treatments for illusory and hallucinatory palinopsia.
Parinaud syndrome is a neurological condition that causes upward gaze palsy and other visual disturbances.
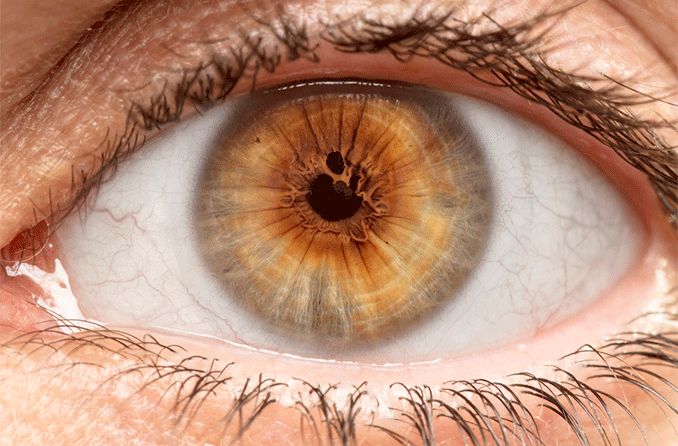
Polycoria — having multiple pupils — is so rare that most eye doctors never see a case. Here are the causes of and treatment for the eye condition.

Pregnancy can cause dry eyes and other vision changes. Mothers-to-be with diabetes face special risks. Your eyes can be warning sign of high blood pressure.
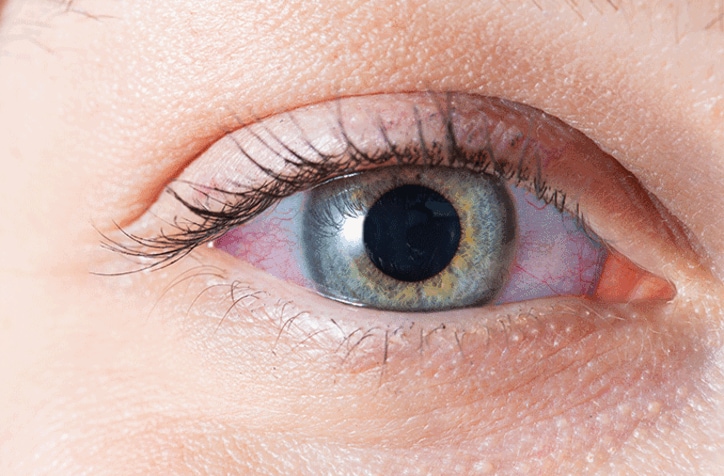
Learn about this rare genetic disorder and how it can affect the eyes' tissues.

Ramsay Hunt syndrome is a rare neurological condition that causes facial paralysis. Find out how it affects the eyes, mouth and ears.

A Roth spot is a retinal hemorrhage that is identified by its unique appearance. It can be caused by a number of underlying medical conditions.

Schizophrenia is a mental disorder that can also impact vision. Learn more about the visual symptoms and changes associated with it.
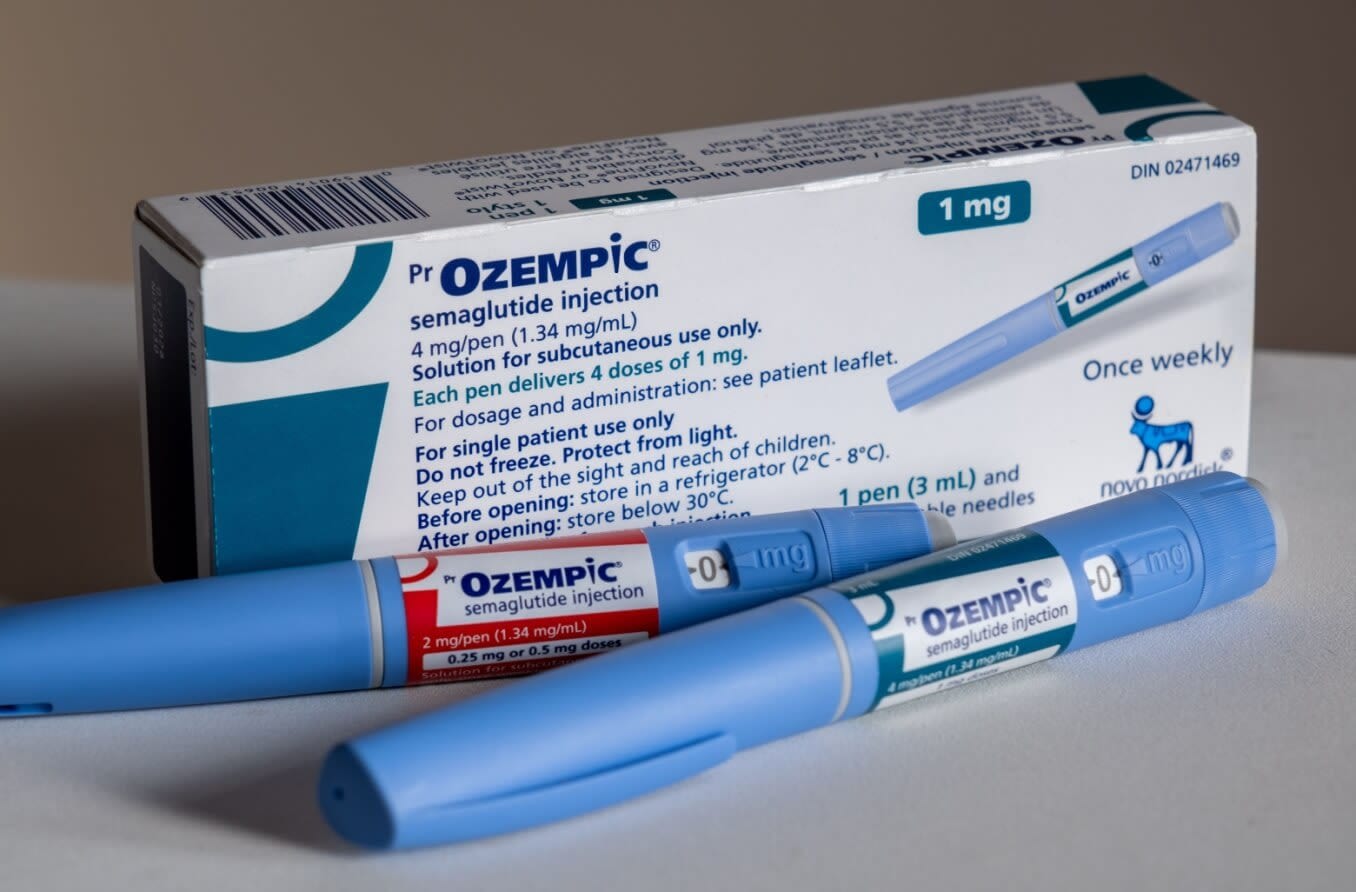
Learn how Ozempic works and whether studies show that Ozempic can cause vision changes or worsen complications in people with diabetic retinopathy.

Setting sun eyes are often associated with conditions that cause elevated intracranial pressure, which can affect eye movements.
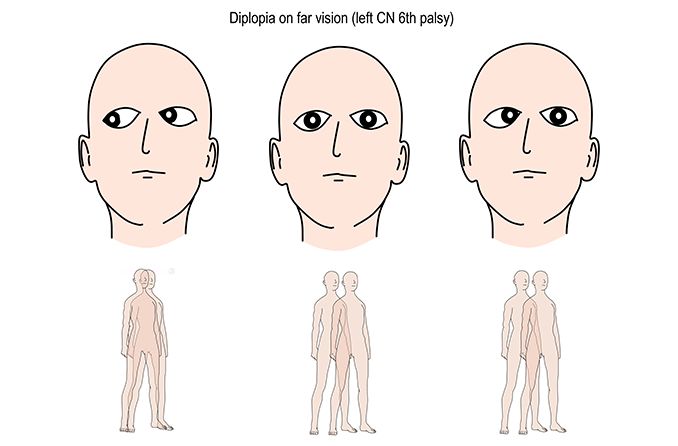
Sixth nerve palsy affects the eye’s ability to move outward. Learn what could cause 6th nerve palsy, as well as risk factors and treatment.

July 23 is World Sjögren's Day — discover how this autoimmune disease affects the eyes.
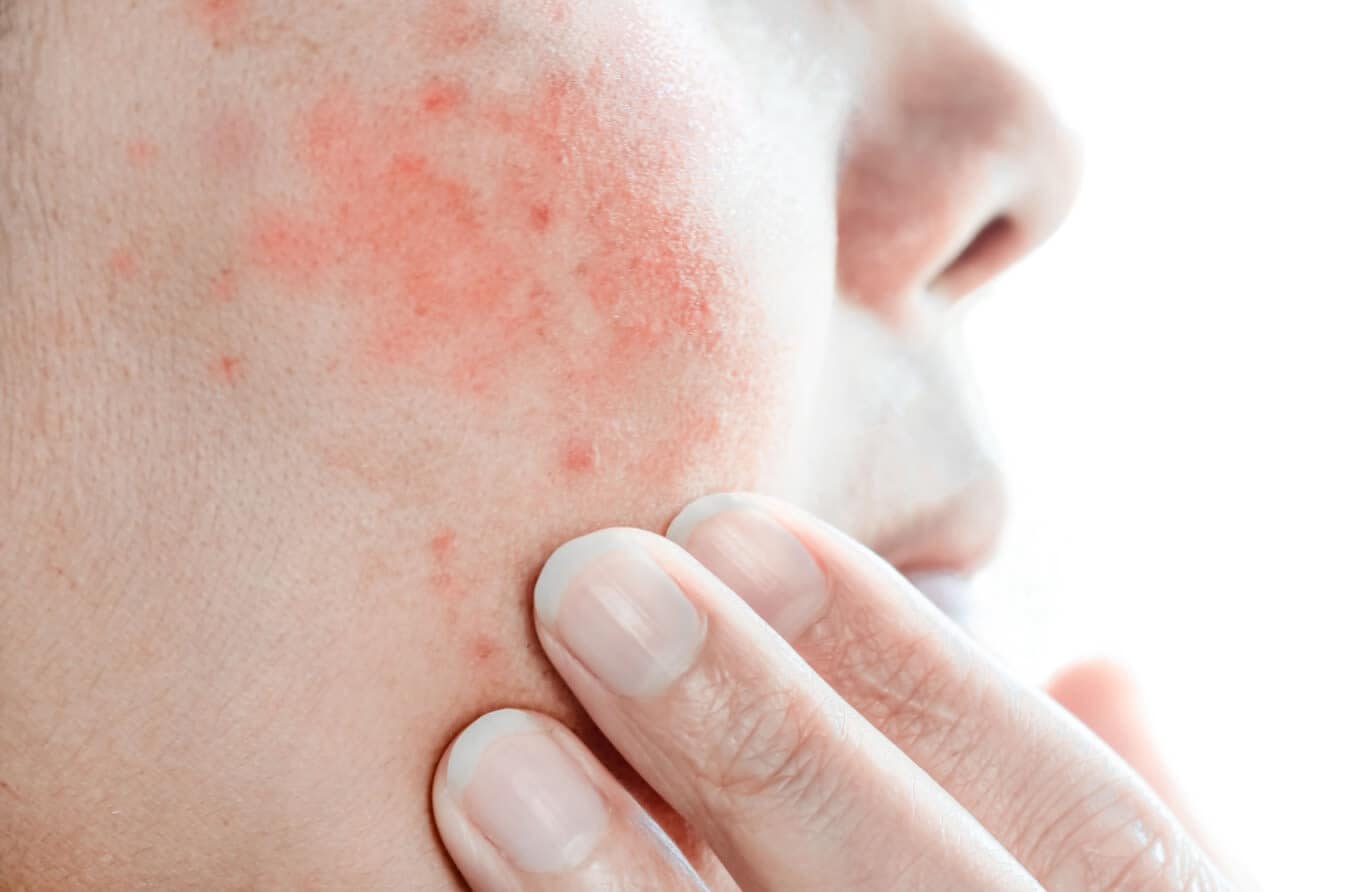
Stevens-Johnson Syndrome is a severe skin reaction affecting your health and your eyes. Learn its symptoms, effects on the eyes and treatment options.

Synesthesia is a condition in which two senses are linked together. Learn more about the different forms and how it can impact vision.

Rheumatoid arthritis (RA) is an autoimmune disease that causes inflammation in the eye’s tissue, leading to pain, redness and potential vision loss.
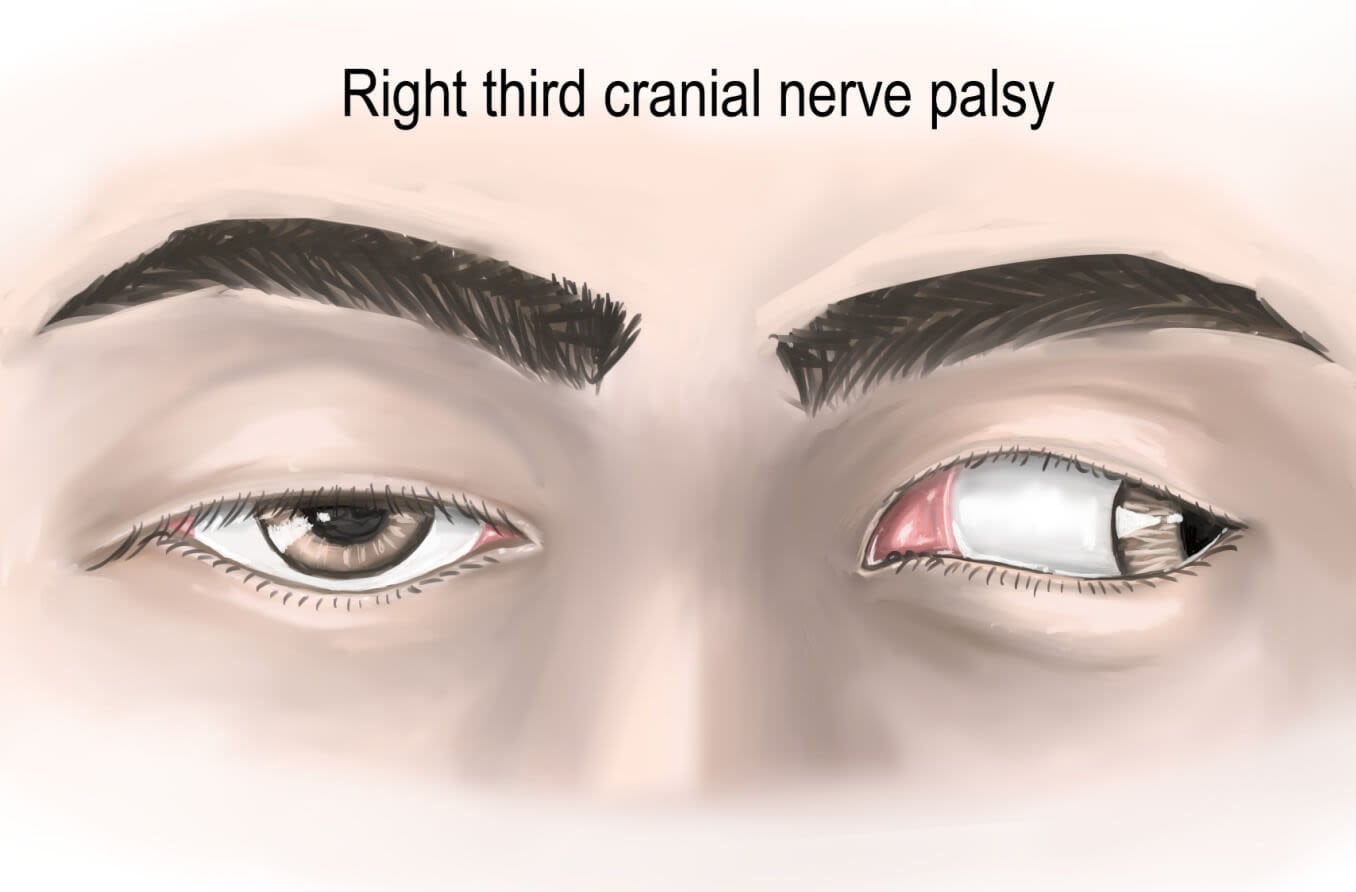
Third cranial nerve palsy causes symptoms such as eye misalignment, double vision, drooping eyelid or enlarged pupil. Sudden onset is a medical emergency.
Thyroid eye disease often causes the eyes to bulge outward. It can occur alone, or more commonly, along with other conditions such as Graves’ disease.
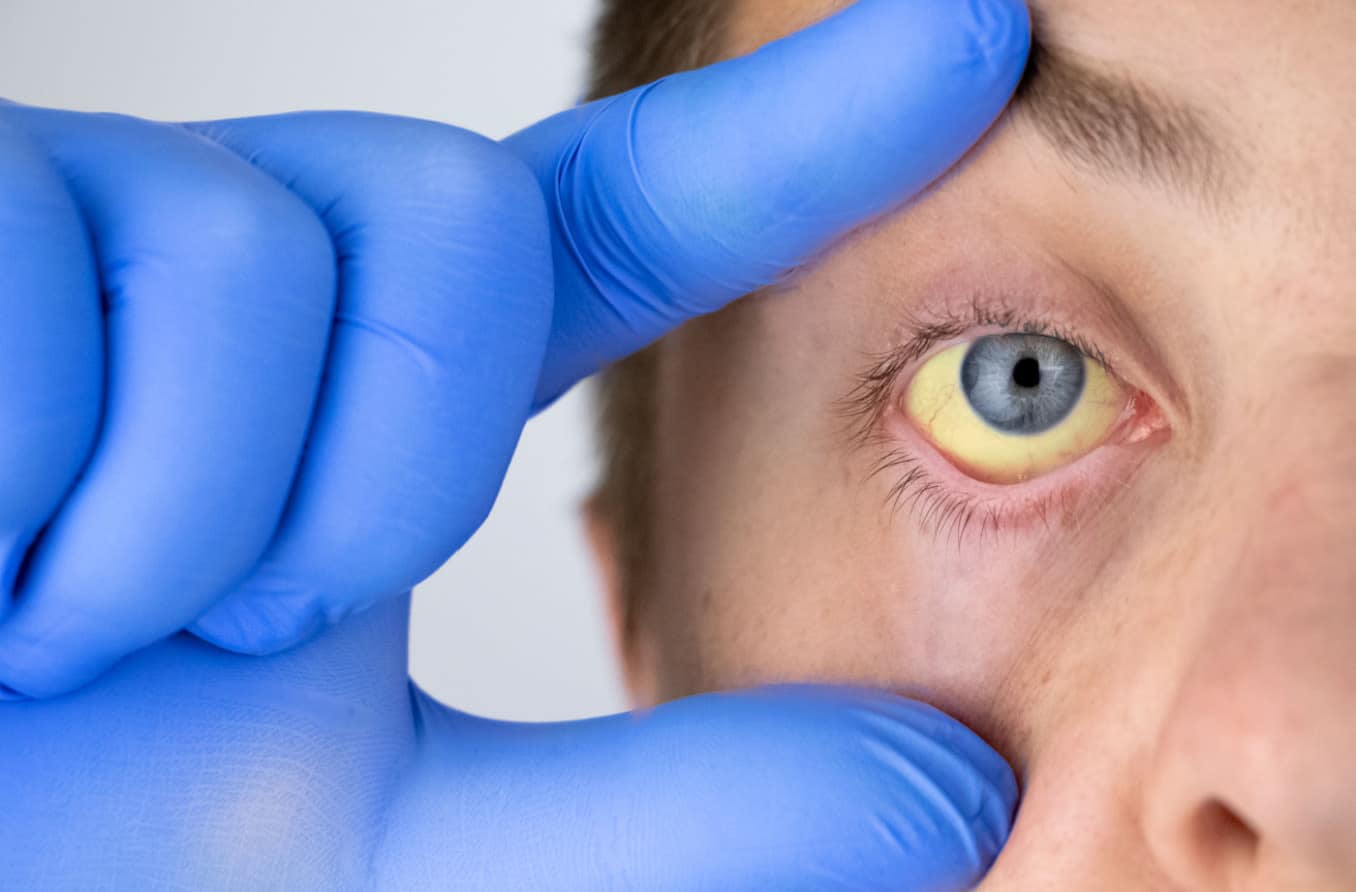
Learn how severe anemia can cause the whites of the eye to develop a blue hue, the inner lower eyelids to become pale, and the retina to become damaged.

Visual agnosia is a rare neurological disorder that affects your ability to recognize familiar objects by sight alone even if your vision is sharp.
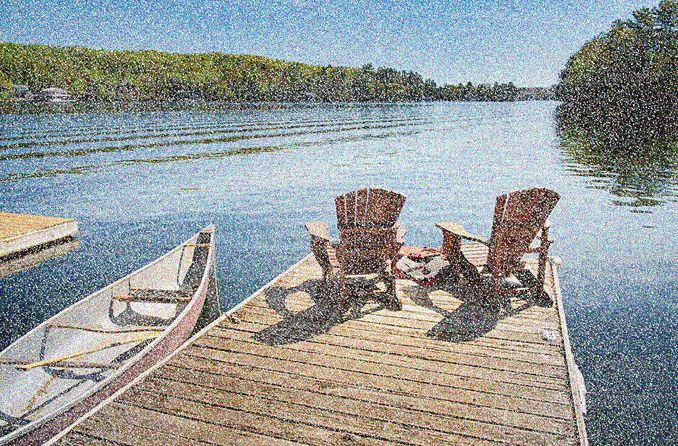
Visual snow syndrome is a rare neurological condition that causes images and scenery to appear “snowy.”

Visual vertigo is an uncomfortable set of symptoms triggered by your vision. Find out what causes this problem and how it can be treated.

Learn about Brushfield spots, including how they're related to Down Syndrome and how they affect vision.
Ophthalmoplegia is a condition characterized by paralysis or weakness in eye muscles which can affect eye movement and vision focus.

Discover the ways your eyes can reflect your heart and cardiovascular health.

Does hearing loss affect vision? Absolutely. If you lose your hearing, your sight becomes much more important because any loss of visual acuity makes it harder to read lips and use sign language.
Wilson disease often causes symptoms involving the eyes. Learn about Kayser-Flesicher rings and the other symptoms associated with the condition.
All About Vision and AllAboutVision.com are registered trademarks of AAV Media, LLC. © 2000-2025 AAV Media, LLC. The content on this site is for informational purposes only. All About Vision does not provide medical advice, diagnosis or treatment. Contact an eye doctor if you need medical attention.