What is Ramsay Hunt syndrome?
Ramsay Hunt syndrome is a neurological condition caused by the reactivation of the varicella–zoster virus. This is the same virus that causes chickenpox and shingles. The condition develops when the varicella–zoster virus affects the facial nerve near the inner ear.
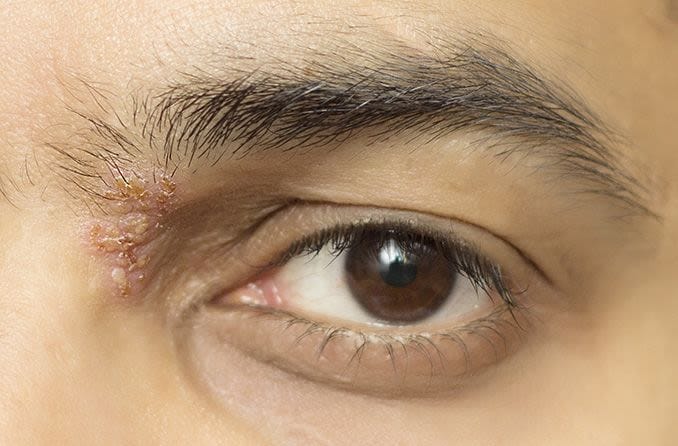
There are two facial nerves, one on each side of the head. Typically, only one side is affected. A person who develops Ramsay Hunt syndrome may experience a painful rash in or on the mouth, ears or face on the affected side. It can also cause facial paralysis on one side of the face.
Ramsay Hunt syndrome was named after a neurologist named James Ramsay Hunt, who identified three diseases and named them all after himself. The three types are only connected to each other by their name.
The most notable type of Ramsay Hunt syndrome is Ramsay Hunt syndrome type 2 (sometimes referred to as herpes zoster oticus or auricular herpes zoster). It affects areas in and around one side of the face. This is the type discussed in this article. Justin Bieber is one prominent figure who has spoken out about their experience with the condition.
How does Ramsay Hunt syndrome affect the eyes?
Ramsay Hunt syndrome can trigger eye-related symptoms in a few ways. This includes facial paralysis, which interferes with eye movement, as well as potential harm to the cornea.
Facial paralysis caused by Ramsay Hunt syndrome

The facial paralysis associated with Ramsay Hunt syndrome often affects eye movement. While it usually only occurs on one side of the face (and in one eye), the effects can be extreme in patients who experience the symptom.
Ramsay Hunt syndrome is sometimes compared to Bell’s palsy. This condition also affects the facial nerve and causes temporary facial paralysis. And it, too, prohibits a person from opening and closing their eyes. It also makes it difficult for a person to have full control over their facial expressions.
However, Ramsay Hunt syndrome has a known cause (varicella-zoster virus), whereas Bell’s palsy does not have an exact origin. Experts suggest that symptoms and recovery are worse with Ramsay Hunt syndrome than they are with Bell’s palsy.
Eye damage caused by Ramsay Hunt syndrome
Certain eye damage is also possible. When a person has facial paralysis, they don’t have control over their eye muscles. And if the eyelid does not close completely due to the paralysis, it can dry out the cornea and expose the eye.
This can lead to infections, corneal abrasion or corneal ulcers if the eye is not protected. If these conditions are not treated, they may lead to vision loss.
To prevent such damage, patients may be directed to wear an eye patch or apply artificial tears to the affected eye daily.
Ramsay Hunt syndrome symptoms
In addition to facial paralysis, there are several symptoms associated with Ramsay Hunt syndrome.
These can include:
- A painful rash or blisters in or around the ear, mouth or tongue
- Earache
- Tinnitus (ringing in the ears)
- Loss of hearing or sensitive hearing
- Vertigo
- Nausea and vomiting
- Feeling weak on one side of the face
Patients may also experience a change in their sense of taste (in rare cases). And they may have trouble closing their eyes or raising their eyebrows.
SEE RELATED: 9 causes of dizziness and blurred vision
Ramsay Hunt syndrome causes
The varicella–zoster virus causes Ramsay Hunt syndrome. It’s the same virus that causes chickenpox and shingles.
Varicella–zoster virus stays in your body after you have chickenpox, and it can reactivate years later as shingles. If that reactivation affects your facial nerves, it causes Ramsay Hunt syndrome to develop.
Although the origin of the disease is the same across all patients, some may not develop all of the symptoms.
SEE RELATED: Eye shingles: Causes, symptoms, treatments
Are there risk factors for Ramsay Hunt syndrome?
If you’ve had the chickenpox virus, it’s possible that you can develop Ramsay Hunt syndrome. (But keep in mind, it is a rare condition.)
Additionally, if you are immunocompromised or have not had the varicella vaccine, you may be at greater risk of developing shingles. And this, in turn, can also put you at higher risk for developing Ramsay Hunt syndrome.
Ramsay Hunt syndrome affects more adults than it does children. Most of the adults who develop Ramsay Hunt are also 60 years or older.
How rare is Ramsay Hunt syndrome? It’s estimated that 5 out of every 100,000 people develop the condition in the United States every year.
SEE RELATED: Eye herpes (ocular herpes)
Ramsay Hunt syndrome treatment
Typically, steroids and antiviral medications are initially prescribed in combination. They work together to treat the varicella–zoster virus and reduce inflammation in the nerves.
Additional medication may be needed if a patient experiences other symptoms, such as vertigo or neuralgic pain (pain caused by damaged nerves).
Treatment should start within the first three days of symptoms for optimal recovery.
Ramsay Hunt syndrome recovery
People with Ramsay Hunt syndrome have a high likelihood of full recovery if they are diagnosed and treated with steroids and antivirals within the first three days. If treatment is started after one week, studies show that only about one-third recover from facial paralysis.
Some people may also experience ongoing hearing loss or synkinesis. (Synkinesis is involuntary twitching of the facial muscles that occurs when someone attempts to move their face.)
Sometimes, Ramsay Hunt syndrome can spread to other nerves, as well as the spinal cord or brain. If this happens, it can cause complications, such as headaches, drowsiness, weakness in the limbs and confusion.
The best way to prevent these problems is to begin treatment within three days of the onset of symptoms. That said, don’t hesitate to contact your eye doctor if you notice any abnormal movement or paralysis around the eye. Whether it’s Ramsay Hunt syndrome or something else, seeking care promptly is always advised.
SEE MORE: Is eye twitching a sign of a stroke