What are eye patches used for?
Eye patches serve a variety of purposes beyond dressing up as a pirate for Halloween. In everyday life, wearing an eye patch usually means you’re healing from surgery, an injury or an eye disease. For children, eye patches can provide a practical way to trick the eyes into fixing vision problems. Indeed, if you or somebody you know has to wear an eye patch, you might have questions such as:
How many types of eye patches are there to choose from?
What kinds of problems do eye patches solve?
How do I encourage a child to use an eye patch as directed by a doctor?
Is it okay to start wearing an eye patch if I start experiencing vision issues?
Let’s start walking through some answers to these questions. (Just for fun, we’ll close with a nifty tidbit about eye patches and pirates).
What are the most common varieties of eye patches?
Anything that blocks vision can work as an eye patch in a pinch, but most patches come in these varieties:
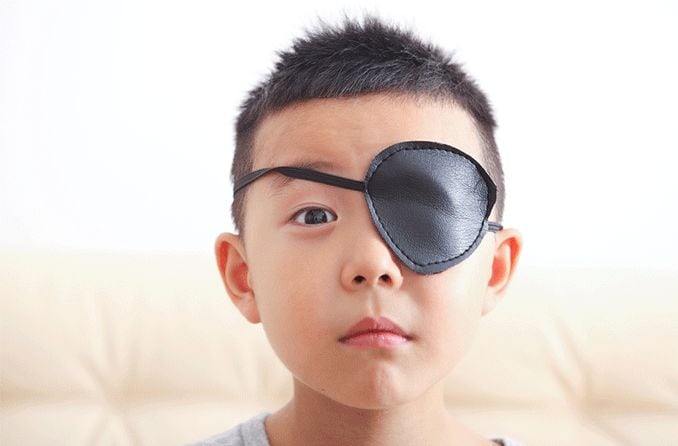
Adhesive – These eye patches work like the bandages in a first-aid kit: They use a sticky substance to hold them in place over the eye.
Non-adhesive – These eye patches are made of soft, comfy cloth and a band that wraps around the head to hold the patch in place.
Eyeglass lens covers – These devices, usually made of plastic, block vision from one half of a pair of eyeglasses. Some are designed to wrap around eyeglass frames to prevent the eye from trying to focus on nearby objects.
Each of these varieties has its pluses and minuses. Children are apt to enjoy the more playful variations of eye patches, but the final decision should come down to a doctor’s recommendations.
What are the medical reasons for wearing an eye patch?
Historically, people wore an eye patch to hide the evidence of an eye lost to injury or disease (a challenge that drove the development of artificial eyes).
These days, eye patches are crucial to the treatment of medical conditions:
Eye injury and disease – Damage to the eyeball from an injury may require an eye patch while the wound heals. Some people wear an eye patch to cover severe injuries that leave disfiguring scars. Certain diseases might require an eye patch to help the patient recover. Keratoconus, a thinning of the cornea, is one such condition.
Eye surgery – Operations like cataract surgery that cut into the eye may require an eye patch for a designated period of time.
The eye and the eye socket (made up of the orbital bones) are complex mechanisms that can work together to promote healing. An eye patch may help or hinder that process. Doing the wrong thing could mess up your eyesight, so make sure you follow your doctor’s guidance.
How do eye patches help with “lazy eye”?
The eyes and the brain work together to produce visualization, the combination of optics, light waves and neurological processes that give us eyesight. The brain does the best it can with the visual information it gets. If one eye is stronger than the other, the brain may focus on the strong eye and ignore the weak one — a condition called lazy eye (or amblyopia).
Usually, this happens in young children whose visual systems are still developing. If left untreated, children can develop permanently impaired vision in the weak eye. This can result in decreased depth perception and narrower field of vision all their lives.
Amblyopia can be caused by uncorrected refractive error, eye misalignment (strabismus) or if vision is obscured in childhood by cataracts or another condition. Once the underlying condition is treated through eyeglasses or surgery, occlusion therapy may be considered.
An eye patch is used to occlude, or block, the view in the strong eye for a little while. An eye patch serves this purpose by encouraging use of the weaker eye.
Prevent Blindness, a nonprofit serving children with eye issues, notes that all a child with a lazy eye needs to do is wear a patch while putting their eyes to work. They can do this while watching TV or playing video games, of course.
But it may do even more good to read books or get into arts-and-crafts projects because it encourages hand-eye coordination, according to Prevent Blindness.
SEE RELATED: Eye doctor Q & A about strabismus surgery
How do I get my child to use an eye patch?
Kids may have a hard time adapting to wearing an eye patch. It’s the grown-up’s job to make sure they wear it anyway. How do you pull this off? Prevent Blindness suggests:
Avoiding power struggles – If you issue demands or try to frighten a child into wearing a patch, you could strengthen their resolve not to wear it.
Creating a schedule – Tell the child the patch comes off at a certain time, then stick to the schedule.
Reducing skin irritation – Hypoallergenic patches may cause less irritation. Ask your doctor about the best adhesives for a child’s skin.
Stop by the Prevent Blindness website for more tips.
When should I start using an eye patch?
If you suddenly develop double vision, it might seem like a good idea to cover one eye to see if that clears things up. Not so fast.
Medical professionals discourage people from using an eye patch without consulting with a doctor first. Moreover, double vision might be a sign of a serious health problem like a brain tumor or an aneurism. Thus, your first priority is to see a doctor ASAP and figure out what’s going on.
What’s up with pirates and eye patches?
Eye patches often show up in tales of pirates roaming the seas in search of gold, jewels and other loot.
It’s natural to presume the buccaneers of history wore patches after unfortunate contact with a dagger or cutlass. But the intrepid fact-checkers at the MythBusters TV show tested another hypothesis that’s been floated over the years: Wearing a patch over one eye during the day produced better vision in the dark of night or the black depths of a ship’s inner compartments.
The MythBusters’ tests showed there’s something to this hypothesis, so they did not declare the myth “busted.” Alas, they also couldn’t find any evidence that pirates ever used eye patches to improve their vision in the dark. Thus, they called this myth plausible but not provable.