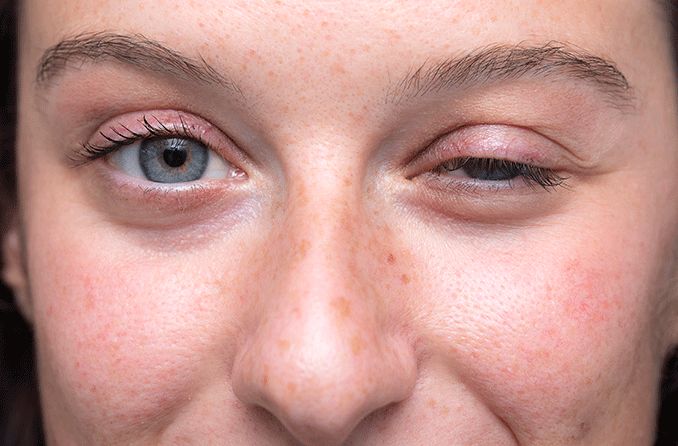
Eyelid psoriasis (pronounced “suh-RYE-uh-sis”) is a non-contagious autoimmune skin condition that causes overproduction of the body’s skin cells, leading to inflammation and thick, scaly patches around the eye area that can make the eyes feel irritated and swollen.
There is no clear cause for this psoriasis but it’s believed that genetics and immune system dysfunction are contributing factors. In addition to medications, there are several coping strategies and lifestyle choices that can help manage symptoms.
What is psoriasis?
Psoriasis is an immune-mediated condition that affects nearly eight million people in the United States and 125 million globally. It appears as reddish patches of skin and can include painful silvery scales that burn and itch.
When there is an imbalance in the immune system, extra skin cells are produced faster than normal. This causes the skin to thicken and become scaly (or develop plaques) in certain areas. It typically takes a month for skin cells to regenerate, but with psoriasis this process happens every three to four days.
Psoriasis usually affects the joints, scalp, elbows and knees but it can develop anywhere on the body, including the eyelids and around the eyes. Psoriasis affects women, men and children, and while symptoms often begin between ages 15 and 25, they can start at any age.
Psoriasis on the eyelid
Around half of people with psoriasis experience it on their face, typically near the hairline, eyebrows, forehead or between the nose and upper lip. However, psoriasis around the eyes or on the eyelids is extremely rare.
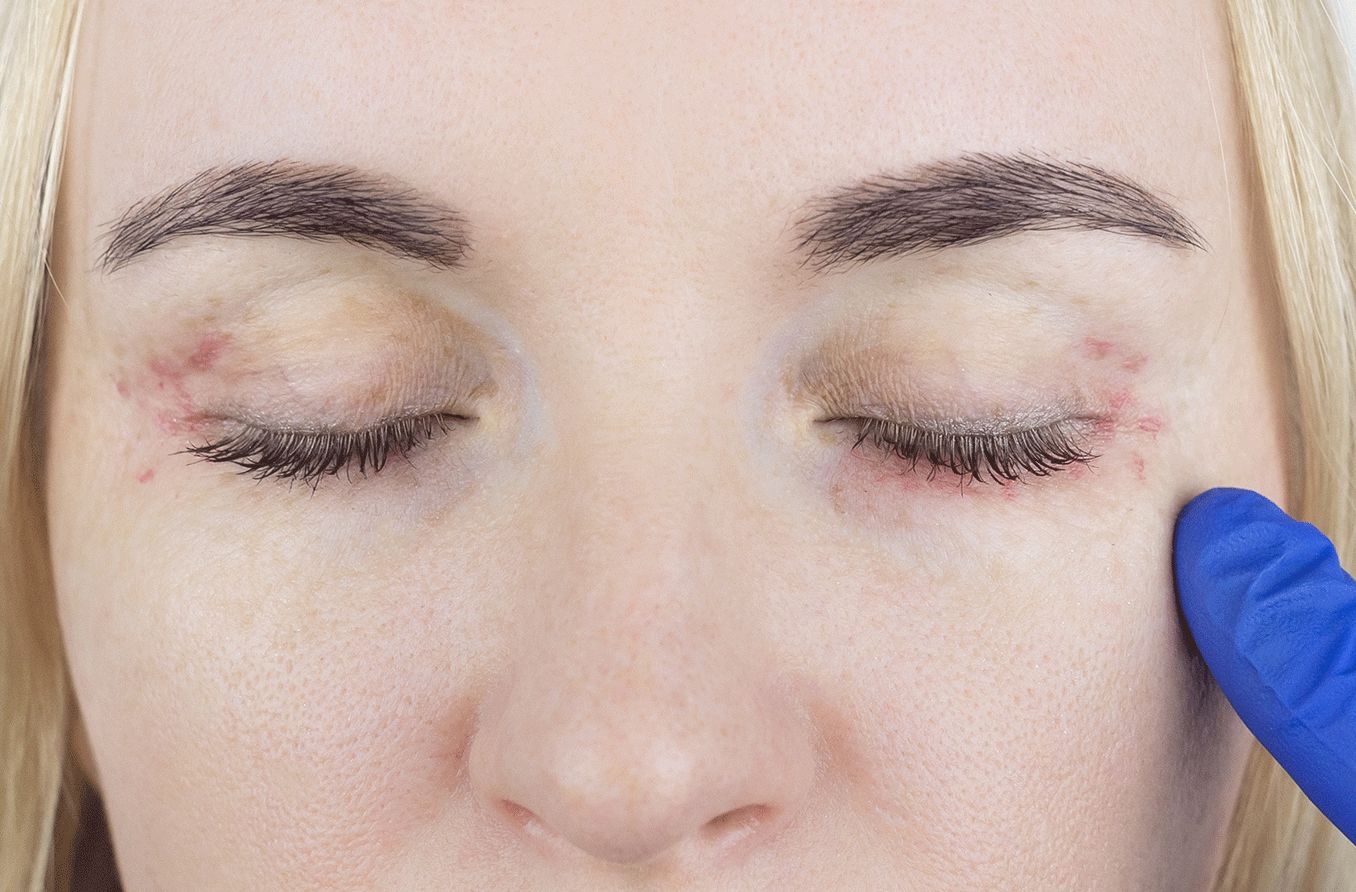
Eyelid psoriasis symptoms
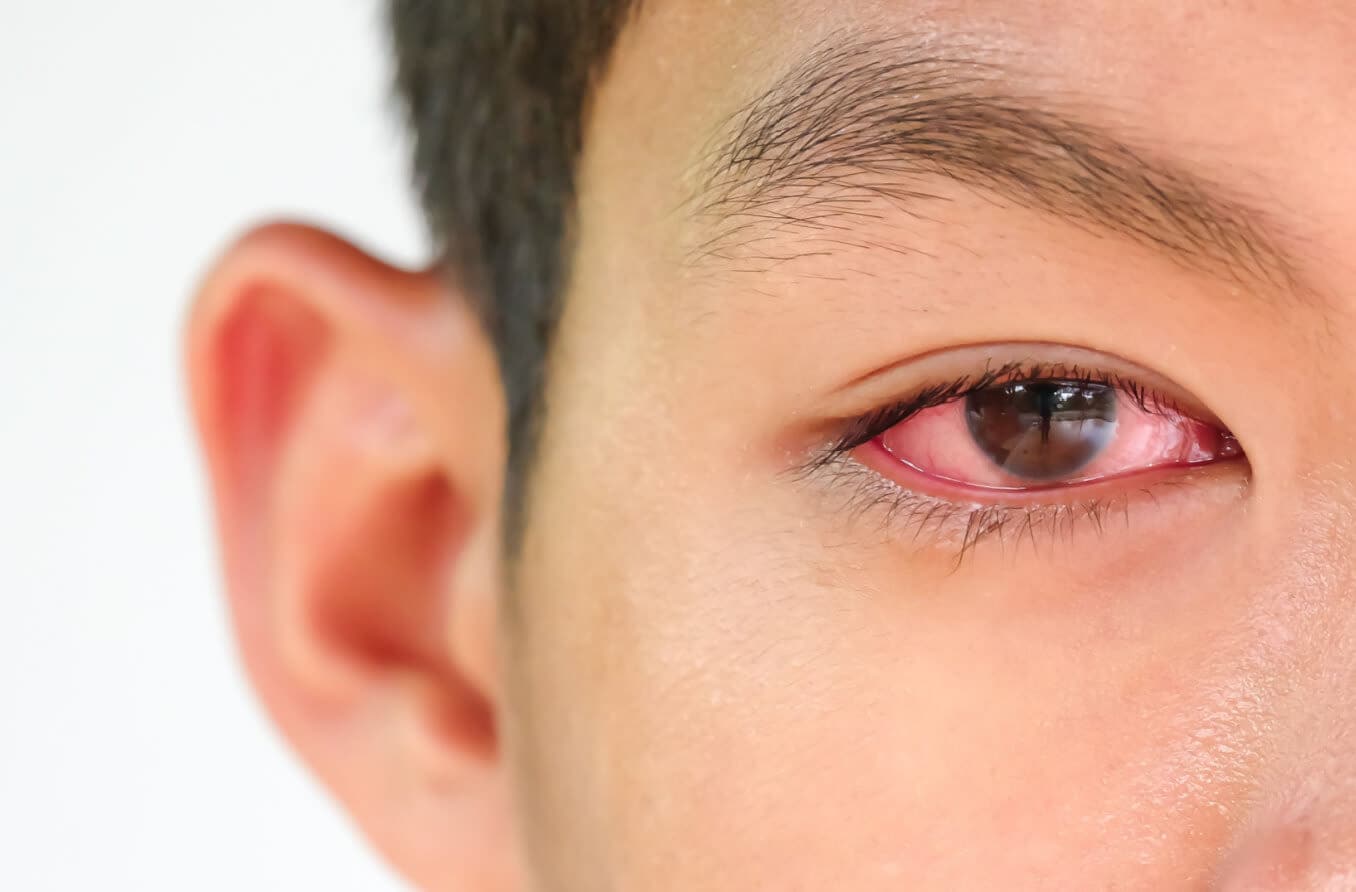
In the rare cases where psoriasis does affect the eye area, it can lead to eye dryness, inflammation, discomfort and possibly vision loss. If a buildup of skin patches becomes large enough, it can result in difficulty opening and closing the eyes.
Other symptoms of eyelid psoriasis may include:
- Scaly, red growths in the affected area
- Dry, cracked skin that may bleed
- Eyelid inflammation that can cause eyelashes to rub against the eye (trichiasis)
- Dandruff-like scales that flake off and stick to the eyelashes
- Eye dryness from scales pulling the eyelid outward
- Pain when moving, opening or closing the eyelids
Eyelid psoriasis causes
Generally considered a disorder of the immune system, genetics can also play a role in psoriasis (though there may be no family history of the disease). Additionally, some triggers can cause symptoms to flare up or become more severe, including:
- Stress
- Illness, specifically throat infections (e.g., strep throat) and immune disorders (e.g., HIV)
- Skin injuries such as bug bites, sunburns and some vaccinations
- Weather, such as less sunlight and decreased humidity, which can also lead to drier heated air indoor
- Allergies, smoking, excess alcohol intake, certain foods and/or environmental factors
- Medications, such as beta blockers used to control high blood pressure or heart rate, or lithium used to treat bipolar disorder
Eyelid psoriasis treatment
Working with a dermatologist and an eye doctor is important when creating a treatment plan for eyelid psoriasis, as conditions that affect the sensitive areas on the face and around the eyes should be managed carefully.
Doctors may use one or more of the following methods to help manage eyelid psoriasis:
- Topical steroids, such as retinoids, corticosteroids and calcineurin inhibitors, may help reduce inflammation and slow excessive skin cell reproduction.
- Non-steroid topicals, such as anthralin, synthetic vitamin D3 and vitamin A or tacrolimus ointment may be used to control psoriasis plaques.
- Over-the-counter topicals may soothe and help remove itchy scales. Options include salicylic acid, coal tar, bath solutions, shampoos, lotions, aloe vera and jojoba.
- Home remedies such as wet dressings may soothe itching by wrapping the area with a wet bandage.
- Phototherapy (light therapy) may help reduce itching and inflammation with a special machine that emits ultraviolet light onto the skin.
- Oral medications, such as methotrexate, cyclosporine, deucravacitinib, apremilast are some of the options that may help clear lesions around the eyes.
Eyelid psoriasis vs. eczema
These two skin conditions develop in different stages of life: Psoriasis usually starts around age 15, while eczema can begin in childhood and continue through adulthood with varying levels of severity. Eczema is more common than psoriasis and affects over 31 million Americans.
While eyelid psoriasis symptoms include pain moving the eyelid and red, scaly patches, eyelid eczema is usually very itchy. Other symptoms include:
- Oozing or crusting
- Sensitive, dry eyelid skin
- Swelling
- Inflamed, discolored skin patches
Also like psoriasis, different types of eczema can appear in different areas of the body.
When to see a doctor
It’s important to call an eye doctor if you notice any changes in your vision or think you might be experiencing symptoms of eyelid psoriasis. A dermatologist is also an excellent point of contact for assessment of psoriasis symptoms and questions about the condition.
Even when your vision seems perfect, it’s important to get an annual eye exam so your eye doctor can check for early warning signs of certain conditions and help protect your overall health.