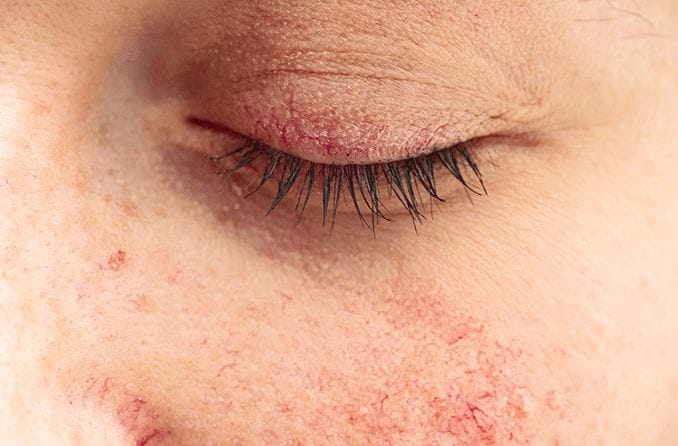
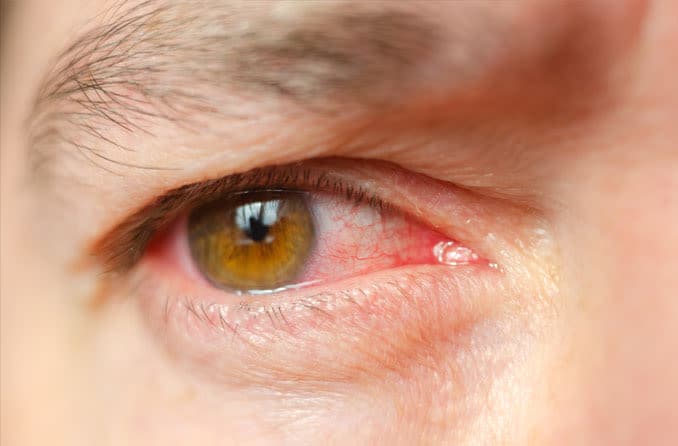
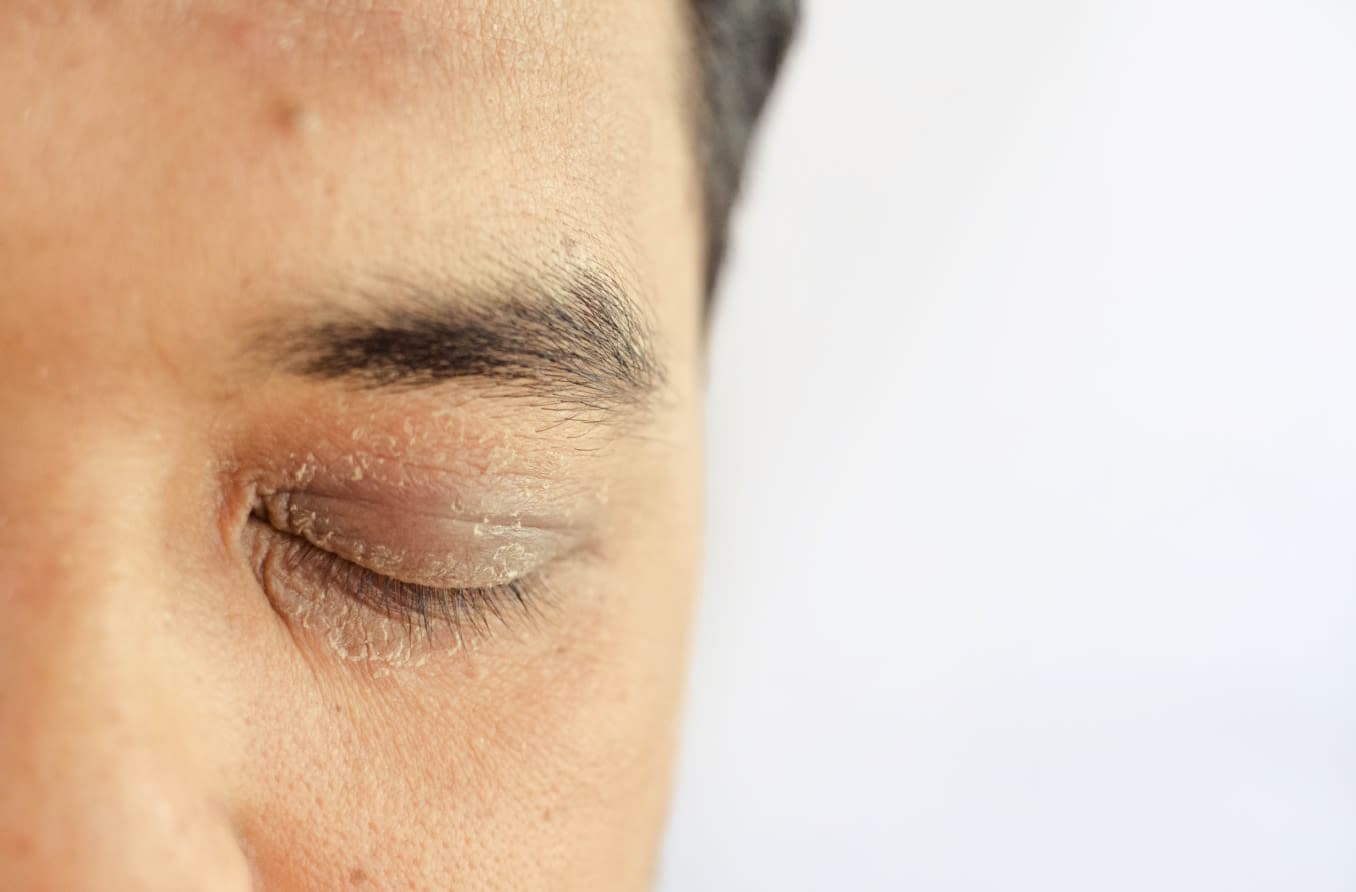
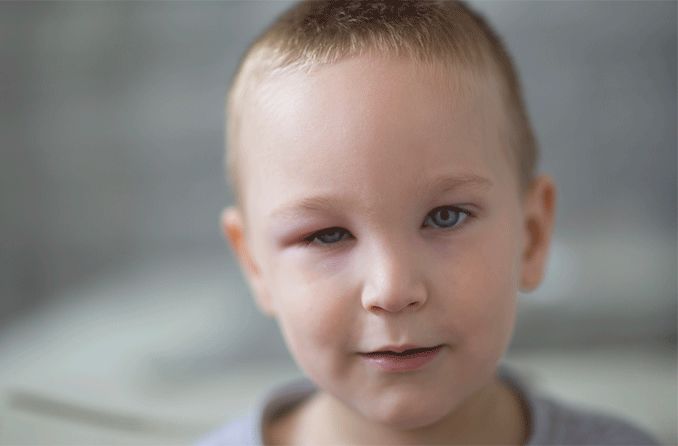
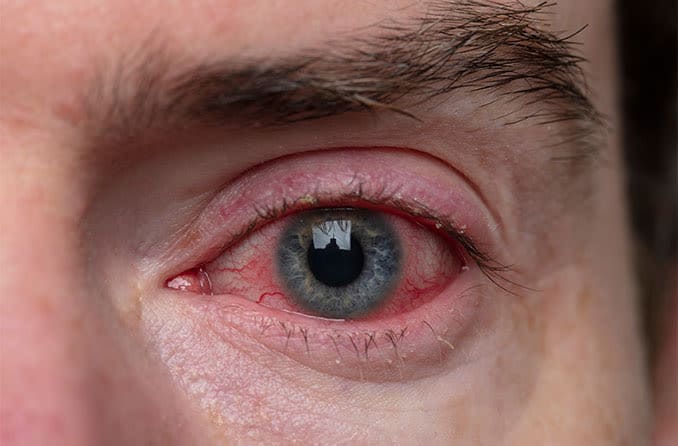
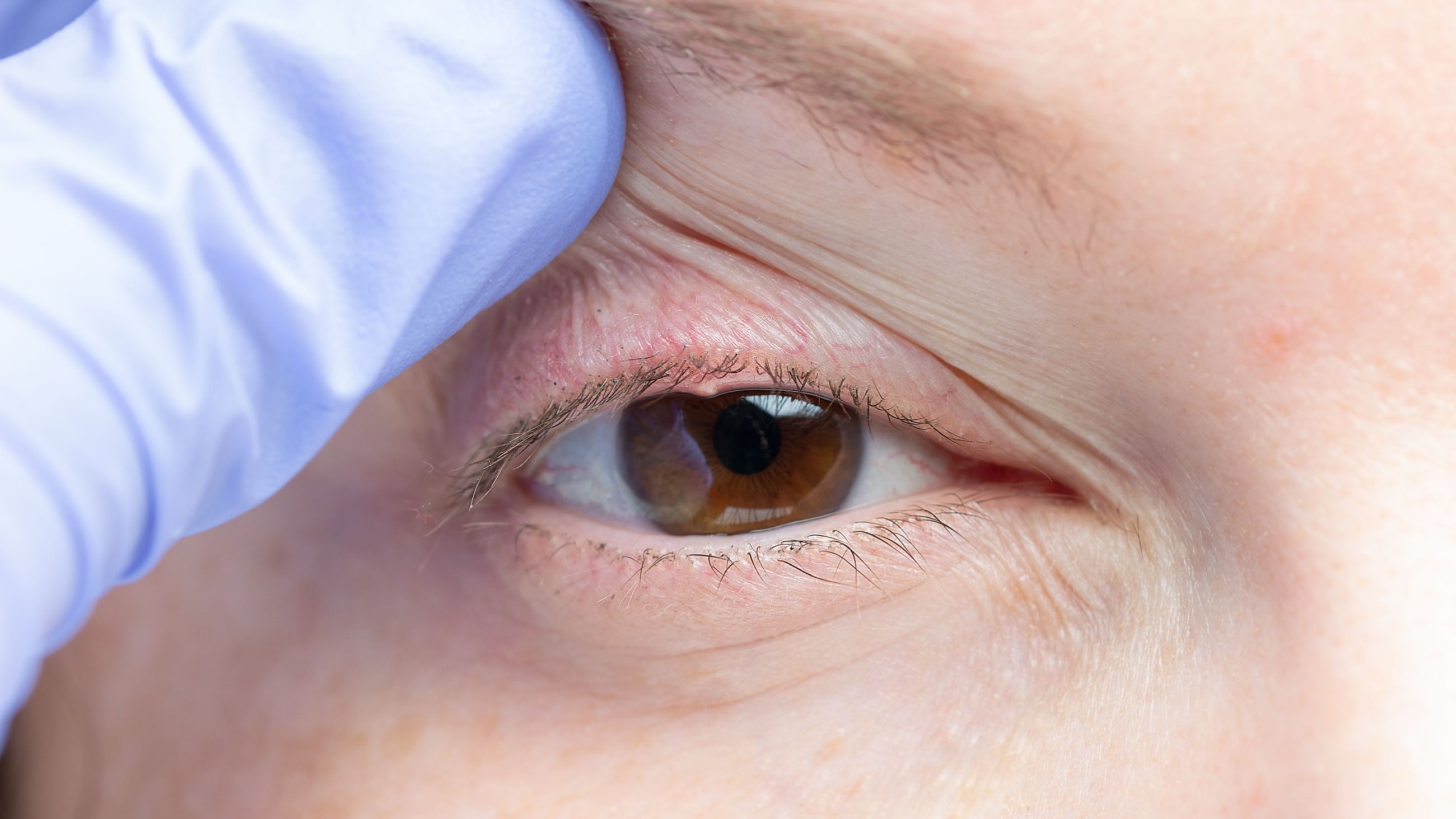
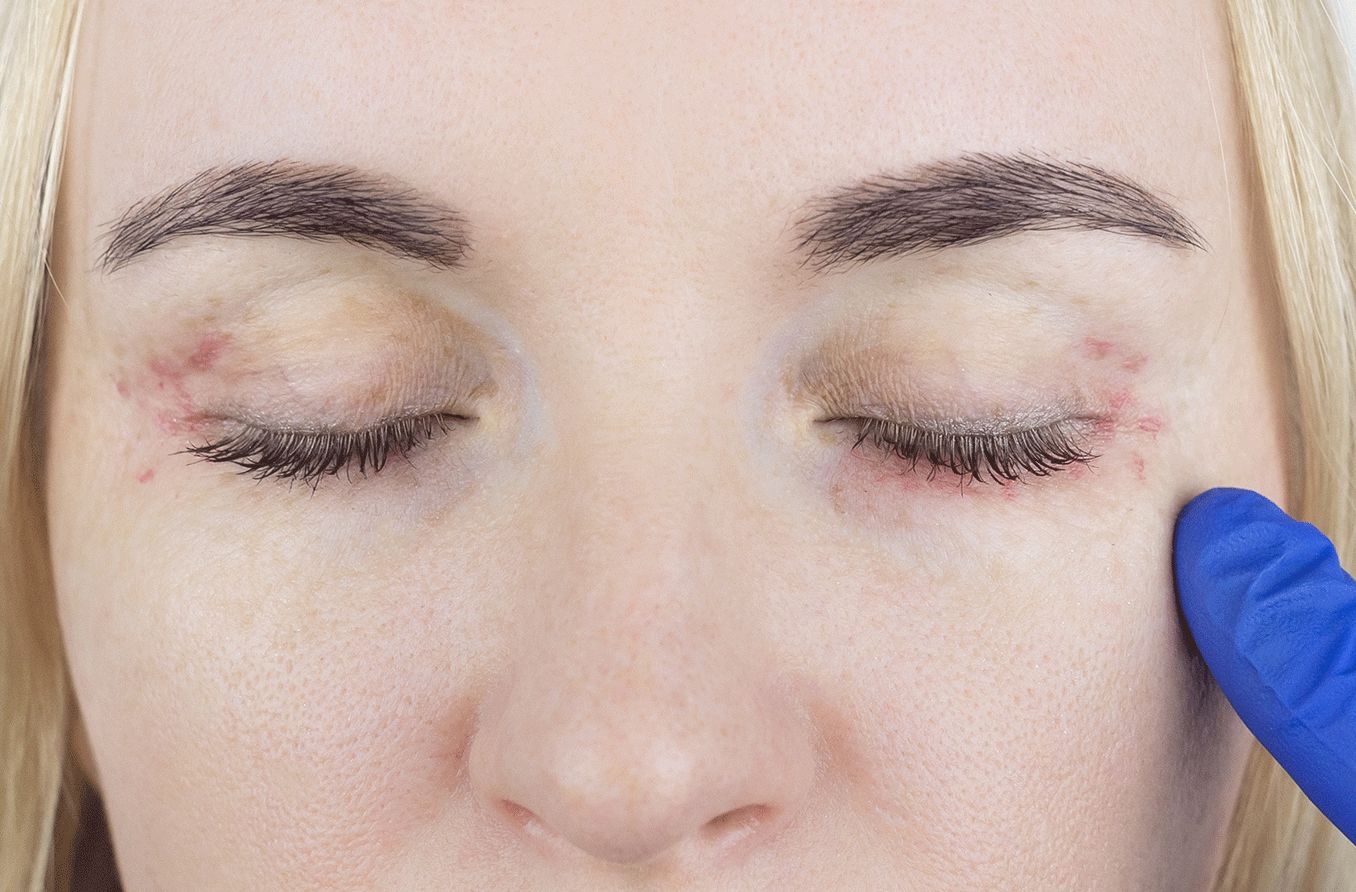
Types of eyelid dermatitis
The eyelids are complex structures made out of muscles and nerves — all covered by a thin layer of skin called the epidermis. Skin on the eyelids is thinner than what’s on the rest of your body, which makes it more prone to irritation. Inflammation in this area is known as eyelid dermatitis.
Eyelid dermatitis, also known as eyelid eczema, is a specific type of dermatitis categorized by the area it affects (the eyelids). Dermatitis and eczema are general terms to describe irritation of the epidermis — the outermost layer of skin.
There are different types of eyelid eczema, and, though the symptoms often look similar, they have varying causes. The ideal way to treat the different types of eczema is to avoid things that trigger flare ups, which differ between people.
Atopic dermatitis
Atopic dermatitis is the most common type of eczema. While research has yet to find an exact cause, experts know that it results from an overactive immune system. This causes the skin barrier to become dry, damaged, itchy and inflamed.
The condition affects over 16 million adults in the U.S. and nearly 10 million children. Of those affected, a percentage of people with atopic dermatitis have a mutation in the gene that creates filaggrin. This is a special protein that strengthens the skin, allowing it to be a better barrier to the environment.
With the absence of filaggrin, this protective barrier is weak or missing, which lets moisture out and harmful germs in. The result is dry, flaky skin that’s prone to infection.
Atopic eczema often begins within the first six months of an infant’s life and is a life-long condition. Symptoms may improve or worsen as a child gets older, and they usually have phases of calmness or severity.
Allergic contact dermatitis
Contact eczema is a reaction to a certain substance that causes a rash to appear. Allergic contact dermatitis occurs due to exposure to an allergen that your skin disagrees with.
When this occurs, the body’s immune system releases white blood cells to the skin. Once there, the cells release chemicals that cause inflammation and present as a rash.
It may be difficult to pinpoint what allergen is causing contact dermatitis on the eyelids, as it can take a few days for a reactive rash to develop. However, some reactions occur within minutes or hours of exposure.
Irritant contact dermatitis
Like allergic contact eczema, irritant contact dermatitis happens when the epidermis is exposed to a harsh substance. However, unlike allergic dermatitis, it focuses more on the skin than on the body’s immune system.
Harsh chemicals found in certain detergents, acids, dyes and solvents can irritate the epidermis. This causes a reaction to occur much quicker than allergic dermatitis reactions. And the rash that develops is usually more painful and itchy.
Seborrheic dermatitis
Seborrheic eczema is a chronic type of dermatitis. It usually affects areas where there are many oil-producing glands. A mixture of genetic and environmental factors contributes to the condition, but a likely cause is an overproduction of lipophilic (oil-loving) yeast on the skin. This overproduction triggers an inflammatory response.
Seborrheic dermatitis usually affects infants and adults between age 30 and 60. In infancy, it may present as a rash on the head called cradle cap, as well as hard-to-treat diaper rash. In these cases, the condition often clears up after infancy and never returns. Cases that develop in late teen years and adulthood often cause an ebb and flow of symptoms for life.
Common symptoms associated with seborrheic dermatitis include dandruff, itchiness and a ring-shaped rash. Other than on the eyelids, the rash is often on the eyebrows, behind the ears and elsewhere on the scalp. It also appears often around the mouth, especially in the nasolabial folds.
SEE RELATED: Eye allergies: Get relief from itchy, watery eyes
Causes of eyelid dermatitis
Like eczema anywhere else on the body, eyelid symptoms can be triggered by anxiety, stress and other factors within and out of your control. Below are some of the more common reasons a person might get eyelid eczema and things that could worsen symptoms in chronic cases.
Genetics
Eczema tends to run in families. You may be more likely to develop eyelid eczema if a parent, sibling or other immediate family member has the condition.
As mentioned earlier, a mutation in the genes that produce filaggrin — a protective skin protein — can weaken the epidermal barrier. The lack of protection on the skin’s surface can lead to eczema symptoms.
Experts believe this mutation can be passed through families, making many cases of eczema a genetic condition.
Immune system sensitivity
Our immune system works by fighting off harmful substances that it believes are a threat to the body. However, it’s possible for the immune system to overreact.
In these cases, the immune system will trigger a big response for a small irritant or allergen that isn’t necessarily harmful. These responses can cause inflammation in the affected area.
Exposure
Dermatitis is usually caused by exposure to substances that trigger an immune response like the one explained above. It’s sometimes difficult to pinpoint exactly what causes an eyelid dermatitis flare up. However, there are some common culprits that often cause a reaction.
One of the more common causes of eczema on the eyelids is an allergic reaction to a product used on or around the face. Triggers that fall under this category include sunscreens, eye makeups, moisturizers, soaps and oils.
Irritants you may not suspect can include eyelash curlers or tweezers that contain nickel. Also included are eye drops, contact solution and the material used in certain goggles or eyewear frames. A reaction may also be caused by false eyelashes or the adhesive used to apply them.
It’s possible for exposure somewhere else on the body to spread to the eyes from the fingers. Common examples of this are with nail polish, poison ivy or poison oak, fragrances and topical antibiotics such as neomycin.
Another cause is the overtreatment of blepharitis — an inflammation of the eyelid that can look similar to dermatitis.
Blepharitis is often treated with baby-shampoo lid scrubs and frequent applications of a hot wet washcloth. But some treatments, such as hypochlorous acid and tea tree oil, can irritate and destroy the skin’s barrier properties. This can cause dermatitis.
Environmental factors
Eyelid eczema can occur as a result of airborne irritants or allergens that cause a reaction around the eyes. Extreme climates with excessive heat, cold, humidity or dryness can do this.
Seasonal allergens, including pollen, pet dander and dust, can make the eyes itchy, leading to rubbing or scratching the area. These factors can cause dermatitis on their own; when combined, it’s a recipe for eyelid eczema.
People in certain professions are exposed to airborne fumes such as acetone, paint or glue. This can upset the area around the eyes. Working with or around chemicals like chlorine or noxious fumes can also irritate the eyes and eyelids.
Finally, handling certain plants and vegetation, such as poinsettias or peppers, can spread to the face and cause eyelid dermatitis. Wearing gloves is important to avoid spreading dangerous oils or chemicals to the eyes. Be mindful, however, as latex used in many types of disposable gloves can trigger eczema symptoms as well.
SEE RELATED: Why do I have dry skin on my eyelid?
Signs and symptoms
Those who have experienced eczema in other areas of the body are aware of how eczema symptoms look. However, because the skin around the eyes is more delicate than anywhere else on the body, symptoms can appear a little differently.
Some signs and symptoms to look out for with eyelid dermatitis are:
- Dryness, flakiness or scaliness in the upper and lower eyelids and the area around the eyes
- Red rash surrounding the eyelids
- Thick or creased-looking skin in the eye area
- Burning, stinging and itchy eyes
- Puffy, swollen eyelids
- Pinkness or redness around the eyes
- Pain around the eyes
- Blistering
While symptoms of eyelid dermatitis are often bothersome, they aren’t usually painful. However, it’s possible for chapped areas to sting or burn when topical treatment is applied.
If at any point you have severe pain in your eyeballs, or if your eyelids are swollen to the point that vision is affected, see an eye doctor. You should also see an eye doctor if your symptoms last longer than a week or become progressively worse.
Tests and diagnosis
Because eczema is so common, dermatologists can often diagnose it by looking at the affected area and asking some questions about your family medical history. Some questions they may ask include:
- Do any of your blood relatives have dermatitis, hay fever, asthma or year-round allergies?
- What symptoms are you experiencing?
- When did your symptoms appear?
- Where is the rash appearing?
Using this information, your eye doctor may be able to make a diagnosis and suggest specific treatment. However, if further evaluation is needed, they may perform one or more skin tests to determine a diagnosis.
There are three common methods to test the skin for allergies: a patch test, a skin prick test and an intradermal test.
Skin patch test
Patch testing is used to pinpoint the cause of a reaction after it’s contacted your skin. It involves taping patches of potential allergens and irritants to your skin and leaving them there for 48 hours.
After 48 hours, you will return to the dermatologist to have the patches removed and to be checked for a reaction. You will also return after 4 to 7 days for another follow-up check to see if new reactions developed in that time. This follow-up appointment is important, as some reactions take some time to show up.
Skin prick test
During this test, your doctor will place a tiny amount of different substances on your skin that they suspect are causing your symptoms. They usually place the substances on your forearm, upper arm or back.
Once the substances are applied, the skin is pricked so they can penetrate below its surface. The areas are monitored for swelling, redness or other adverse reactions to the substances. You can usually get results within 15 to 20 minutes.
Substances that cause a skin reaction are categorized as triggers, and your doctor will advise you to avoid them, if possible.
Intradermal test
An intradermal test involves injecting a small amount of allergen or irritant into the skin, rather than placing it on top. After injecting, the doctor will watch the injection sites for reactions.
While this test can be used to diagnose dermatitis, it’s more often used to detect a bee or penicillin allergy. It may also be used if a skin prick test was negative for an allergen and the doctor still believes you’re sensitive.
Radioallergosorbent (RAST) test
RAST testing is a diagnostic method in which blood is drawn and measured for its allergic response. An antibody called IgE is produced by the blood when it's exposed to proteins — specifically proteins found in certain foods — it doesn’t like.
Experts measure the levels of this antibody when the blood is exposed to proteins they suspect are causing your reaction. RAST testing doesn’t only confirm or deny a food allergy. It’s also used when patients have severe eczema, are extremely sensitive or cannot stop taking antihistamines, which is required for a skin prick test.
Eyelid eczema vs. psoriasis
Eyelid psoriasis may look like eyelid eczema due to similar symptoms of redness and scaly skin. They both can also be passed genetically and have to do with the immune system. But how the immune system reacts is what mainly differentiates the two.

Eyelid Psoriasis
Psoriasis is a disease in which the immune system overreacts and leads to an overproduction and growth of skin cells. Because too many skin cells are being produced too quickly, a buildup of cells — called plaque — develops on the epidermis. The plaques can become thick, scaly, flaky and painful.

Eyelid Eczema
While the two conditions look similar, psoriasis tends to have more patches (plaques) of inflammation than eczema. With psoriasis, the flakes on the eyelashes and skin are also more silver in appearance. It is less itchy than eczema and often gets better when the skin is exposed to sun.
With eczema, the immune system is also overly reactive to triggers like irritants or allergens. But rather than responding with an overproduction of new cells, the body responds by sending inflammation to preexisting skin cells. Inflammation can cause the skin to become red, itchy and dry.
Both conditions may be worsened by stress and anxiety and are appropriately managed by avoiding things that trigger symptoms.
Home remedies and medical treatment options
Many eyelid dermatitis cases can be soothed by home remedies. However, severe instances may need medical treatment.
Some eyelid eczema treatments that you can do at home include:
- Avoid irritants – If you know there are certain products or substances that cause a flare up, keep away from them. For products that you can’t stop using, try to find a similar alternative that won’t trigger a reaction.
- Don’t scratch! – Affected areas may be irritated and itchy, but avoid scratching or rubbing the eyelids — especially with unwashed hands. Doing so can break the skin, which raises the risk of infection.
- Use lukewarm water – Hot water strips the skin of important oils that help keep it hydrated. When washing the face, use lukewarm water instead to help keep the oils intact.
- Moisturize – Apply a gentle, fragrance-free moisturizer to the affected area right after you bathe, shower or wash your face. This helps lock in hydration. Petroleum jelly is an eczema-friendly option that may offer more itch relief than a moisturizer.
- Use gentle products – Cosmetics, sunscreen and any other products used should be mild and fragrance-free. You may also benefit from products marketed for “sensitive skin.” Be sure to read the ingredients list to check for irritants or allergens.
- Avoid overheating the skin – When possible, keep your environment cool with low humidity.
- Lower your stress levels – As mentioned earlier, stress can worsen dermatitis symptoms. Make an effort to manage stress naturally. If necessary, talk to a therapist to see if medication can help.
If home remedies can’t seem to manage eczema on the eyelids, a doctor — usually an eye doctor or a dermatologist — can prescribe you treatments that may be more effective. A few treatments they may suggest are:
- Corticosteroids – May be applied topically to reduce itching and inflammation; examples include hydrocortisone cream. Since creams can shed into the eye and cause irritation, avoid applying them close to the eye lashes. For dermatitis that is close to the edge of the eyelid, use a steroid eye ointment instead.
- Phosphodiesterase inhibitors – This is a nonsteroidal ointment that works to block substances that cause inflammation. Crisaborole is an example of a phosphodiesterase inhibitor.
- Calcineurin inhibitors – Another nonsteroidal treatment that works as an immunosuppressant to prevent eczema flare ups. Common topical calcineurin inhibitors include tacrolimus and pimecrolimus.
- Oral medications – These may include steroids (like prednisone), antihistamines or antibiotics to prevent infection.
- Injectable drugs – Injections of dupilumab may be used to treat chronic eczema. However, there are risks of side effects involving the eye, such as conjunctivitis and dry eye syndrome.
- Phototherapy – This treatment method uses different wavelengths of ultraviolet (UV) light to reduce symptoms. Products are available for you to perform this treatment from home. However, it’s recommended to consult with a doctor beforehand and follow their instructions.
SEE RELATED: Vision problems? Check your medications
Risk factors and prevention
Eczema on the eyelids can affect just about anybody, regardless of age or ethnicity. However, there are a few factors that can make someone more vulnerable to developing eyelid dermatitis. Some of these risk factors may include:
- Having a family history of eczema, asthma or hay fever
- Being biologically female
- Having sensitive skin
- Being African-American
- Working in an environment where you’re exposed to harsh chemicals or fumes
- Having a weakened skin barrier or a history of epidermal inflammation
The majority of cases of eyelid dermatitis clear up after a few weeks of treatment. Once an outbreak has calmed, prevention may be as simple as avoiding the irritants that caused the initial problem.
Here are some suggested tactics for avoiding eye eczema in the future:
- Steer clear of known irritants when possible.
- Resist the urge to scratch or rub your eyelids.
- Avoid touching your eyelids with dirty hands or fingers — they may have irritants on them.
- Test cosmetic products before applying them all over the face.
- When washing your face (especially in the eye area), use a cleansing cream made for sensitive skin.
- Limit your showers to 5-10 minutes and use lukewarm water to wash your face.
- Moisturize your face and eyelids with a gentle, fragrance-free moisturizer after showering or washing the face.
- Choose products specially formulated for sensitive skin.
- Wear loose-fitting, breathable clothing.
- Protect your eyes by wearing wraparound sunglasses or goggles when exposed to irritants.
Ask your doctor for brochures or other information about preventing eyelid dermatitis from returning.
When to see an eye doctor
If you notice that new soap or makeup seems to make your eyelids red or itchy, stop using it immediately and see if the irritation clears up. That could be all there is to it.
Unfortunately, many cases are harder to resolve because the cause isn’t so clear. If you think you’re experiencing symptoms of eyelid dermatitis, contact an eye doctor for proper assessment and treatment.
Anything that creates discomfort in your eyelids is going to make your life unpleasant. It’s a good idea to set up an appointment if eyelid dermatitis, or any other condition, has started bothering you and doesn’t resolve within a week.
Tom Mangan and Allie Johnson also contributed to this article.
SEE RELATED: Stevens-Johnson syndrome