What is a hemifacial spasm?
Hemifacial spasm is a chronic neuromuscular disorder causing painless, uncontrolled twitching on one side of the face. It typically begins at the eyelid and spreads toward the mouth and cheeks. In the early stages, the twitching typically occurs occasionally, but in later stages, it can occur constantly.
Hemifacial spasm is often long-lasting. Middle-aged women are more likely to have this condition, although it can occur in both men and women. This condition is more frequently seen in people with Asian heritage. A person experiencing a hemifacial spasm can appear to be having a seizure, although it is not one.
What causes hemifacial spasm/face twitching?
Facial twitching in hemifacial spasms is caused by abnormal activity of the facial nerve — the seventh cranial nerve.
A hemifacial spasm can result when the facial nerve is irritated, often because something is pressing against it. When pressure is applied to a nerve, it can cause it to fire spontaneously and abnormally.
When an irritated facial nerve discharges, it sends signals to different parts of the nerve along its pathway, causing spasms in different parts of the face the nerve controls.
The facial nerve is responsible for some functions and movements of the:
- Eyebrows
- Eyes
- Mouth
- Lips
The orbicularis oculi muscle — responsible for closing the eyelid — is typically the first to be affected. Over time, the spasm may progress beyond eye twitching, and the other muscles of facial expression may become involved as well.
Hemifacial spasm can be the result of one of several causes:
Idiopathic
Many cases of hemifacial spasm do not have a clear cause — meaning they are idiopathic.
Pressure from a blood vessel
When a cause is identifiable, the spasm is typically because another structure is pressing on and irritating the facial nerve as the nerve it leaves the base of the brain. The source of compression is often a blood vessel, in some cases a dilated artery or hardened artery. A blood vessel that has moved out of its normal position may also place pressure on the facial nerve, causing it to become irritated.
READ MORE: 15 ways heart disease affects eye health
Pressure from a tumor
A less common cause may be a benign (not cancerous) head or neck tumor pressing on the nerve.
Secondary to an injury
Damage to the facial nerve can cause a secondary hemifacial spasm. This can occur when the facial nerve does not grow back normally after an injury, and nerve signals may be misdirected, causing spasms on that side of the face.
Secondary to Bell’s palsy
A viral infection can cause inflammation of the facial nerve and may result in weakness on one side of the face, causing Bell’s palsy. While many patients recover from the weakness, hemifacial spasm can occur months later — in some cases, even years later.
Less common causes
Some uncommon causes can also lead to a hemifacial spasm. These may include:
- Aneurysms
- Brain tumors
- Multiple sclerosis and other demyelinating diseases
READ MORE: Eye symptoms commonly seen in multiple sclerosis
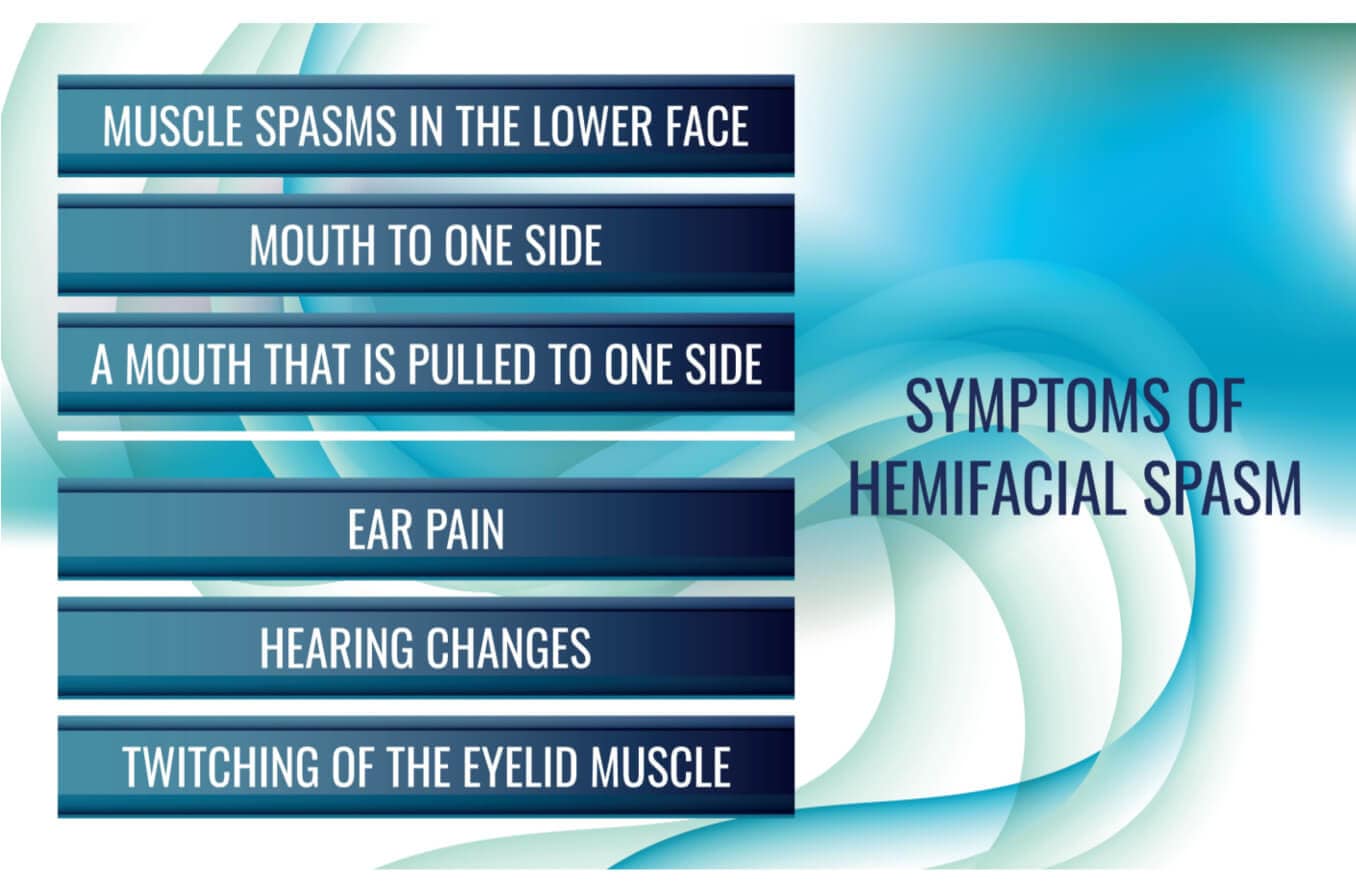
Signs and symptoms
One apparent symptom of a hemifacial spasm may be uncontrollable and painless twitching on one side of the face, often pulling it to that side. The symptoms often begin near the eye and become more severe. Over time, the face may twitch continuously, involving the cheeks and mouth. The facial nerve does not receive pain stimuli, which is why the spasms are typically not painful.
A patient with hemifacial spasm may experience other symptoms in addition to facial twitching, and these may include:
- Fatigue
- Facial tic
- Skin rash
- Nausea
- Balance issues
- Hearing loss or ear pain
- Vision issues
Some people with hemifacial spasm may have mild symptoms with periods when they may be free of symptoms. Certain factors can increase the frequency and severity of hemifacial spasms, such as:
- Specific facial expressions
- Specific head postures
- Stress
- Anxiety
- Fatigue
Painful tic convulsif syndrome
Painful tic convulsif syndrome (PTCS) is a rare syndrome in which hemifacial spasm occurs at the same time as a condition called trigeminal neuralgia. This is caused by abnormal discharge of the trigeminal nerve or fifth cranial nerve.
This disorder typically causes sudden, chronic facial pain and hemifacial spasms because the facial and trigeminal nerves are both involved.
Diagnosis
It is recommended that a person experiencing hemifacial spasm symptoms be evaluated by a neurologist. Magnetic resonance imaging (MRI) may be ordered to rule out tumors or other issues that can cause symptoms similar to a hemifacial spasm. This imaging test can also detect whether a blood vessel is pressing on the facial nerve and causing the spasm.
A neurologist may also order a test for or perform the following:
- Eye and vision evaluation
- Muscle strength and reflex evaluation
- Electromyography (a test that measures the electrical activity of the muscles)
- CT scan (a test that takes many X-ray images from different angles around your body)
- Angiography (a test that performs an X-ray of the blood vessels using contrast dye)
Treatment, management and prognosis
Many cases of a hemifacial spasm may require treatment. Several types of treatments exist, including antiseizure drugs, botulinum toxin injections and surgery.
Oral Medication
Hemifacial spasms can be treated with medication, although this option may not be effective and can result in side effects.
Anticonvulsant medications that can be used to treat this condition in some cases may include:
- Carbamazepine
- Clonazepam
- Phenytoin
- Gabapentin
- Baclofen
These medications can cause side effects that can range from mild to severe, such as:
- Sleepiness
- Nausea
- Balance issues
- Skin irritation
Injections
Botulinum toxin injections may be available at an in-office procedure and may be the first treatment option for many patients with hemifacial spasm. A small needle is typically used to inject botulinum toxin into the muscles of the face. This treatment weakens the muscles temporarily so that the twitching may stop.
It typically takes about one week for the injection to work, and the effects may last up to 3-4 months, after which the injection may be repeated. There may be a risk of developing resistance, and side effects can occur, including:
- Irritation in and around the eye
- Dry eye
- Drooping eyelids
- Incomplete eyelid closure
- Double vision
- Facial weakness (typically temporary)
Statistics show about 80% to 95% of patients may see improvement.
READ MORE: Botulinum toxin and side effects
Surgery
The surgery for hemifacial spasm depends on the underlying cause. Microvascular decompression may be performed if a hemifacial spasm is due to an artery pressing on the nerve.
This surgery is done under general anesthesia and is typically performed by a neurosurgeon. An incision is made behind the ear. The blood vessel pressing on the nerve is moved away, and padding is placed between the artery and nerve to remove the pressure.
The benefits and risks of surgical treatment vary with each individual. Statistics show as many as 90% of patients may see improvement.
But there are potential risks involved, including:
- Brain hemorrhage
- Stroke
- Paralysis or weakness of the facial muscles
- Decrease or loss of hearing
- Infection
There also may be a chance that the spasm will come back after surgery.
Conditions related to hemifacial spasms
Although many cases of hemifacial are considered idiopathic (unknown origin), some conditions may increase the chances of developing a hemifacial spasm.
These may include:
- Seventh cranial nerve (CN VII) injury
- Injury to the face
- Atherosclerosis (narrowing and hardening of arteries due to buildup of cholesterol and fats)
- Bell’s palsy
- Family history
READ MORE: Why healthy blood pressure is important for healthy eyes
Coping with hemifacial spasm
Hemifacial spasm is typically a chronic condition. In addition to treatment, it is helpful to take steps to try to minimize symptoms associated with it.
These may include:
- Decreasing caffeine intake
- Getting plenty of rest and avoiding fatigue
- Decreasing stress
- Managing anxiety
Your eye doctor also may have information about clinical trials in your area that may be available and could offer potential new treatments.
In addition, there are national nonprofit organizations that can assist individuals and caregivers of people living with hemifacial spasm.
A caring team of doctors and healthcare professionals, along with a supportive network of family and friends, are important resources for those living with hemifacial spasm.
READ MORE: Glossary of eye care terms