What does it mean to have hypotony (low eye pressure)?
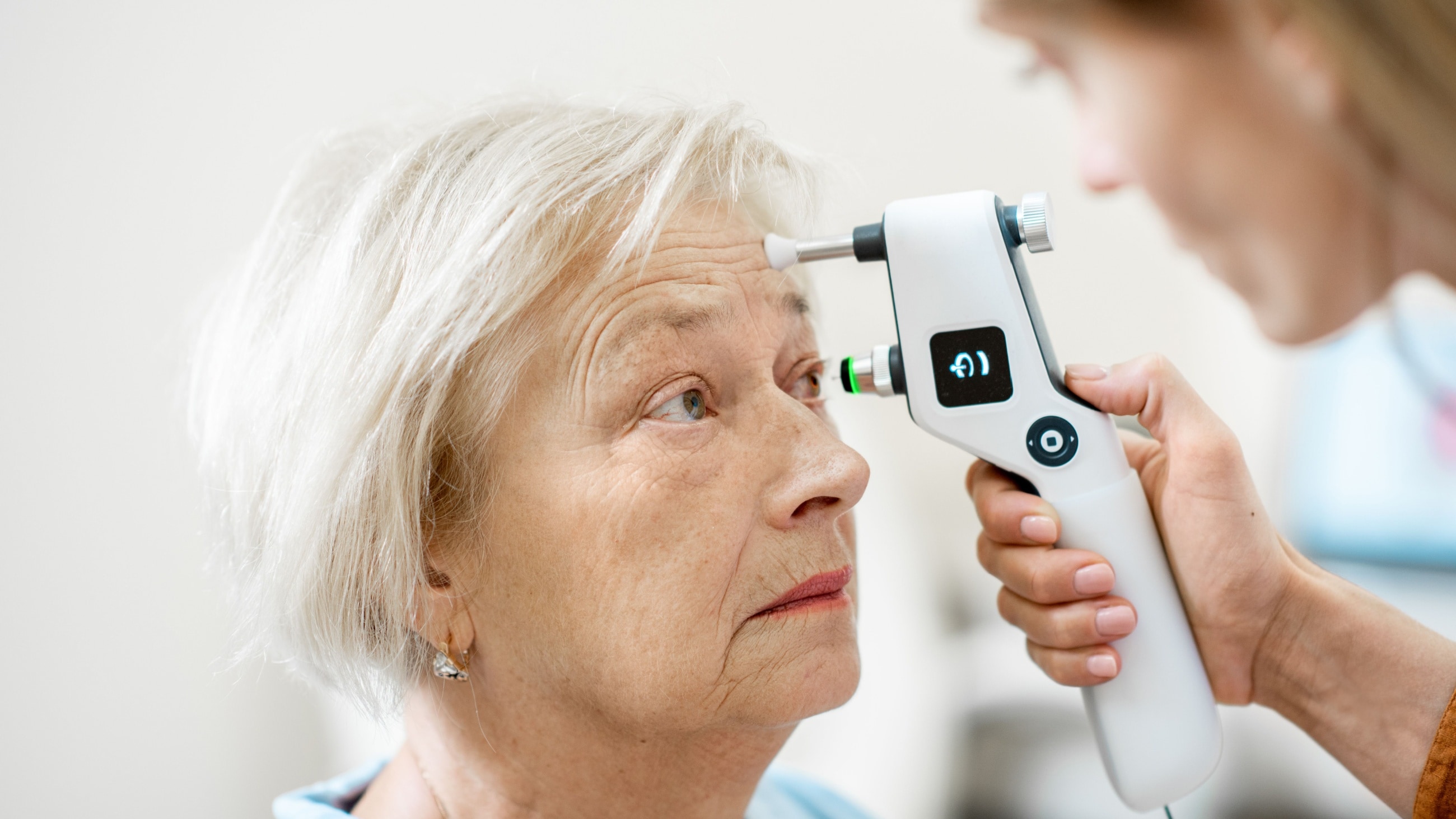
There are two ways hypotony can be described: statistically and clinically. Statistically, an eye is considered to have hypotony when intraocular pressure (IOP) is below 6.5 mm Hg. Clinically, hypotony occurs when eye pressure is low enough to cause vision loss.
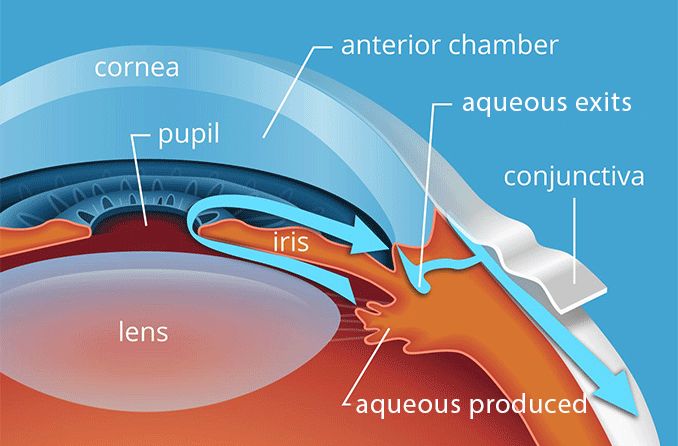
Eye pressure, or IOP, is regulated by the aqueous humor. This is located near the front of the eye, between the cornea and iris. The IOP is regulated by a constant inflow and outflow of this aqueous humor.
The normal range for IOP falls somewhere around 12 to 22mm Hg. When that pressure becomes too low, structures within the eye can become compromised. This can lead to vision loss and other complications.
The effects of low IOP vary from individual to individual. Some eyes may be particularly susceptible to low IOP. Others may hardly be affected. The rest fall somewhere in between.
Low eye pressure symptoms
The symptoms of hypotony vary. Some individuals may not experience any symptoms at all, despite their low eye pressure. When symptoms of low IOP do appear, they can lead to vision loss or distortion. Low IOP may also cause an individual to be slightly more farsighted than before.
Complications of hypotony
Hypotony can also lead to secondary complications caused by the eye’s reduced structural integrity.
Some of the potential complications include:
- Ciliochoroidal detachment – A ciliochoroidal detachment results from an abnormal amount of fluid buildup in the suprachoroidal space. This complication can result in reduced aqueous humor production and worsen the already present hypotony.
- Hypotony maculopathy – When the eye’s IOP falls low enough, the scleral wall will collapse and macular folds develop. These changes in the eye can lead to visual decline and hyperopia (farsightedness).
- Papilledema – Papilledema is optic disc swelling caused by increased pressure around the brain. This can cause headaches, vomiting, and short periods of distorted vision.
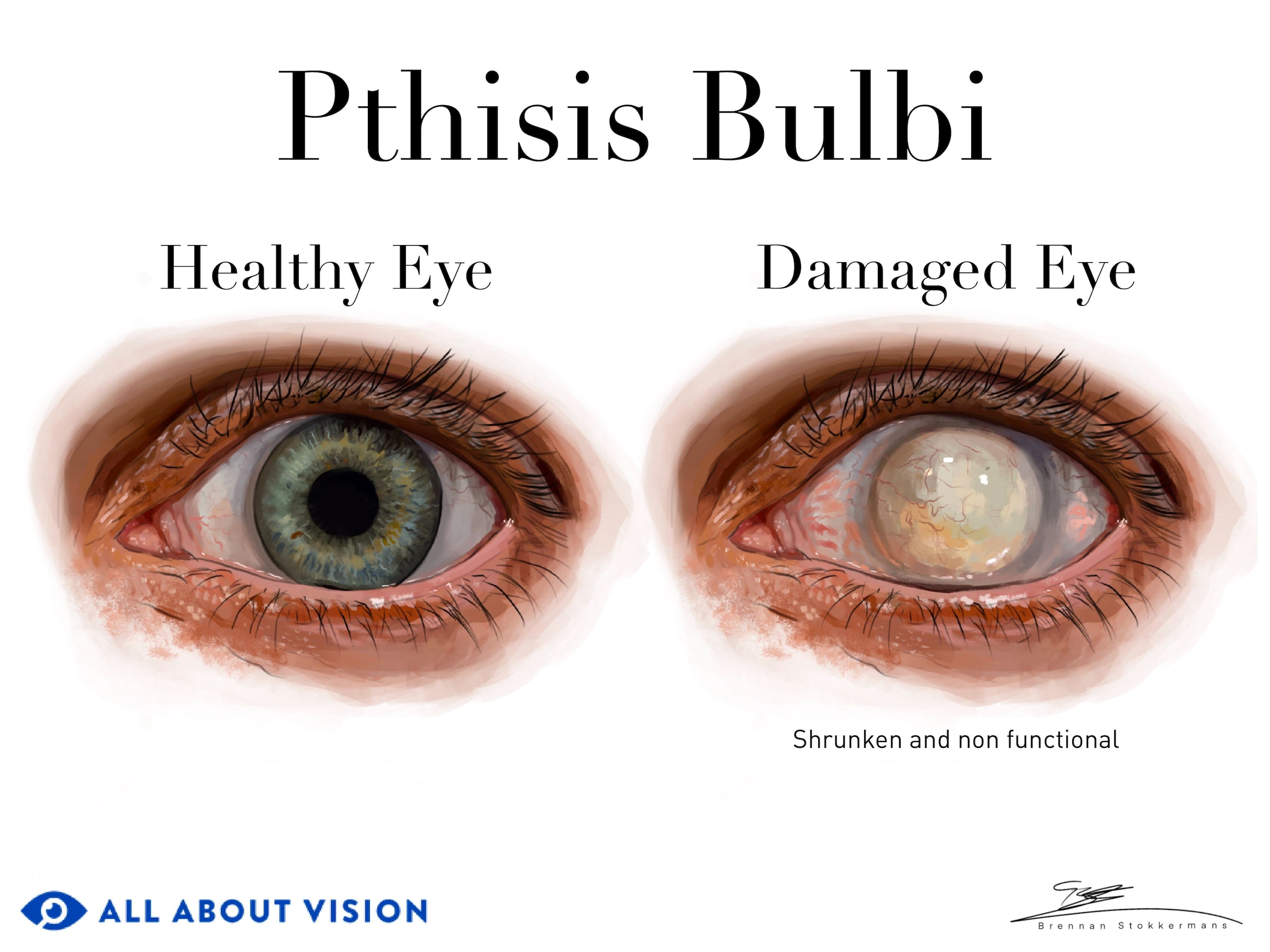
- Phthisis bulbi – Phthisis bulbi is the medical name for when eye injury or disease damages the eye to the extent that the eye permanently stops functioning. It is also called end-eye stage. This means that the eye will become permanently blind. The eye may also go through physical changes like shrinking and scarring.
What causes hypotony?
There are two principal causes of hypotony: a higher than normal outflow of aqueous humor and the underproduction of aqueous humor. Low IOP can also be caused by a combination of the two.
Hypotony due to increased aqueous outflow is the more common cause and can result from:
An overfiltering bleb – A trabeculectomy is a surgery to lower IOP. It does this by creating a filtering bleb. This bleb filters out excess aqueous to lower IOP. A bleb is like a fluid-filled blister.
An overfiltering bleb occurs when too much aqueous humor filters through the conjunctiva. It either pollutes the tear film or becomes absorbed into the conjuctiva’s blood or lymphatic vessels. This increased outflow of aqueous humor lowers IOP.
Around 1.3 to 18% of these surgeries are reported to lead to hypotony maculopathy development. The risk of hypotony maculopathy increases if antifibrotic drugs are utilized for the surgery.
A leaking bleb – Like an overfiltering bleb, a leaking filtration bleb is a common complication of trabeculectomy. It can develop any time from days to years after the surgery. A leaking bleb occurs if the filtration bleb does not properly seal. A faulty seal can allow too much aqueous humor to leak from the eye and lower IOP.
A cyclodialysis cleft – This rarely occurs after surgery or blunt trauma. A cyclodialysis cleft forms after fibers of the ciliary muscle separate from the scleral spur. This separation creates an opening between the anterior chamber and the space above the choroid.
The most common causes are trauma and surgery. It’s not uncommon for this separation to close on its own. But if it doesn’t, it can lead to chronic hypotony and eventually hypotony maculopathy.
A scleral rupture – Also called a globe rupture, a scleral rupture can be caused by either blunt trauma or an eye-penetrating object. When fluid leaks through the rupture, IOP can drop and result in hypotony.
A surgical wound leak – This can occur when ocular fluid leaks through surgical wounds, such as after cataract surgery, resulting in lowered IOP.
Hypotony due to underproduction of aqueous humor can also be caused by eye inflammation. Certain aqueous suppressant medications can limit aqueous humor production and lead to lower IOP. In addition, ciliary body damage can decrease aqueous humor production.
Treatment
Treatment for hypotony varies depending on its cause. The underlying goal for treatment is to raise the IOP.
Nonsurgical treatments for an overfiltering bleb include:
- Topical steroids
- Autologous blood injection
- Laser stimulated inflammation
- Diathermy
- Trichloroacetic acid
- Compression sutures
Nonsurgical treatments for a leaking bleb include:
- Aqueous suppressants
- Topical antibiotics
- Bandage contact lens
Surgery should be undergone immediately in cases of trauma, such as a globe rupture or retinal detachment. Otherwise, non-surgical options like the ones above should be attempted first.
If those do not fix the low IOP, surgery could be necessary. Possible surgical treatments include:
- Bleb excision and revision
- Vitrectomy
- ILM peel
When to see a doctor
Hypotony can develop after surgery or trauma. It can also occur due to long-term inflammation. If you’ve recently had eye surgery, experienced blunt trauma to the eye or have chronic eye inflammation and your vision starts to decline, call your eye doctor right away.
If you haven’t experienced any kind of trauma or surgery, but your vision suddenly declines, you should still call a doctor immediately.