What is papilledema?
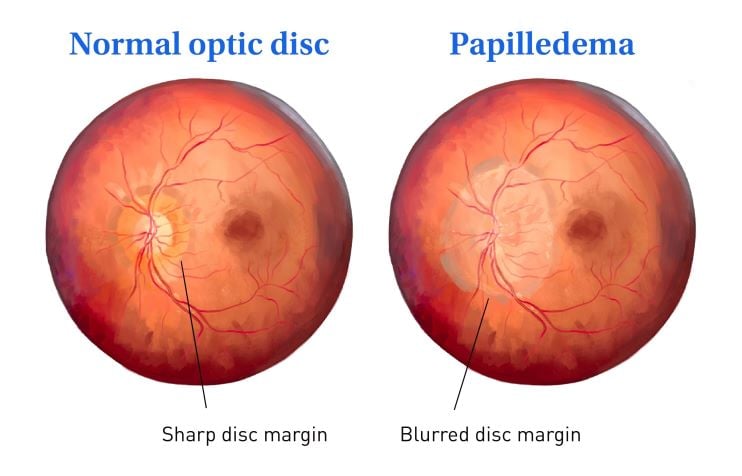
Papilledema is swelling of the optic disc, the front part of the optic nerve that connects the eye to the brain. It usually affects both eyes and can cause vision problems and headaches. Because it signals increased pressure in the brain, it is a medical emergency needing urgent care.
What causes the optic disc to become swollen?
The optic disc becomes swollen in papilledema because of high pressure inside the skull. This high pressure is called increased intracranial pressure (ICP) or intracranial hypertension.
How the eye connects to the brain
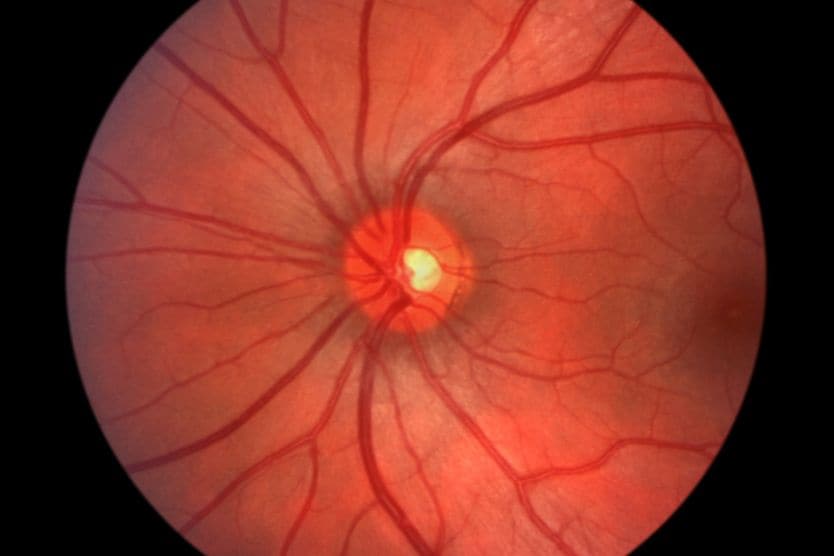
The retina is the light-sensitive layer at the back of the eye that detects light. The optic disc is where over a million nerve fibers in the retina come together and leave the eye as the optic nerve. The optic nerve carries the signals from the retina to the brain. The optic disc can be seen during an eye exam as a circular shape on the retina.
How high ICP causes optic disc swelling
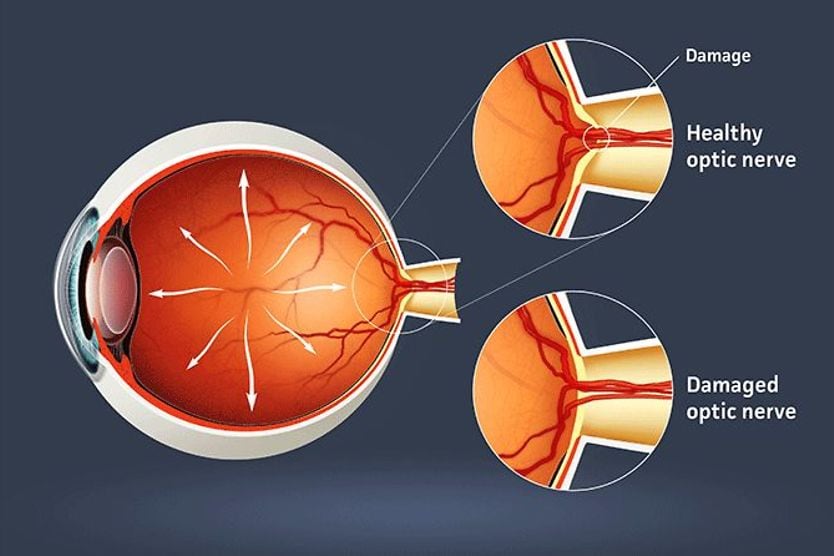
Cerebrospinal fluid (CSF) is a clear liquid that surrounds and protects the brain and spinal cord. The body constantly produces and reabsorbs this fluid. When ICP gets too high, the fluid-filled space around the optic nerve fills with pressurized CSF. This can cause the optic disc to become swollen.
How papilledema disrupts vision
The swelling and high pressure disrupt the signals traveling along the optic nerve. At first, there may be no noticeable symptoms. Later, episodes of vision disturbances can occur. If left untreated, papilledema could cause permanent damage to the optic nerve. This may result in irreversible vision loss.
True papilledema is different from other types of optic disc swelling. These include:
- Optic disc edema – This refers to any swelling of the disc. The swelling is not specifically from increased intracranial pressure.
- Pseudopapilledema – This appears as disc swelling during an exam. However, it’s due to normal anatomical variations. There is no true fluid buildup in the optic nerve.
Papilledema is more common in women aged 20 to 44 who are overweight. This is because they are at higher risk for increased ICP. For the general U.S. population, the incidence is much lower.
Causes of papilledema
The cause of papilledema is increased intracranial pressure. It can become elevated when there is an increase in the normal volume of:
- Cerebrospinal fluid
- Brain tissue
- Blood in the brain
Idiopathic intracranial hypertension
Most cases of papilledema result from a condition called idiopathic intracranial hypertension (IIH). It is also known as pseudotumor cerebri. It is caused by the buildup of cerebrospinal fluid around the brain. Idiopathic means that a specific cause cannot be identified. But some factors can increase the risk of IIH, such as:
- Obesity
- New weight gain
- Polycystic ovarian syndrome (PCOS)
- Certain medications (such as tetracyclines, high doses of vitamin A and steroids)
- Endocrinological diseases (such as thyroid disease)
- Sleep apnea
- Anemia
Additional underlying causes
Other causes of high intracranial pressure include:
- Brain tumors
- Blood clots in the brain
- Infections in the brain
- Inflammation in the brain
- Dangerously high blood pressure
Symptoms and signs
The symptoms of papilledema can vary in severity. Some people may not notice any symptoms at all, especially in the early stages. This is why regular comprehensive eye exams are important, as your eye doctor may be the first to detect the condition.
Vision symptoms
Early on, there may be no noticeable vision changes. Symptoms often develop as the optic disc swelling progresses. Peripheral vision may be lost at first. Central vision may follow without treatment. Vision is almost always affected in both eyes. Vision symptoms of papilledema can include:
- Episodes of vision disturbances lasting a few seconds
- Enlarged blind spot
- Arc-shaped flashing light
- Double vision (diplopia) from pressure affecting the nerves controlling eye movement
- Peripheral vision loss (tunneling of vision) that progresses to central vision loss in long-standing cases
About one in four people with advanced papilledema experience vision symptoms, initially as brief episodes. They last less than 30 seconds. During this time, vision in both eyes may become blurry, gray or completely dark. This can happen with a change in posture, like standing up quickly from a seat. It can also happen during activities that increase pressure. This includes coughing or straining your abdomen.
Systemic symptoms
People with papilledema often experience symptoms from high intracranial pressure that affect the entire body. These are called systemic symptoms. They can include:
- Headache
- Pulsatile tinnitus (“whooshing” or rhythmic sound in the ears)
- Nausea and vomiting (often accompanied by severe headaches, especially in the morning)
- Difficulty thinking clearly
- Trouble moving parts of the body
- Problems with speech
- Breathing pattern is shallow
- Behavior changes
- Drowsiness and fatigue
- Loss of responsiveness
When to seek immediate medical attention
Elevated intracranial pressure is a medical emergency. Any symptoms of this condition need immediate medical evaluation. If you experience these warning signs, seek emergency care right away:
- New or worsening headaches
- Nausea and vomiting
- Vision disturbances
This is especially critical if you also:
- Have a fever
- Have high blood pressure
- Recently started birth control pills
- Are pregnant
Diagnosis and tests
A prompt diagnosis of papilledema begins with a thorough eye exam. Your eye doctor may also order specialized tests to identify the underlying cause.
Examination
Your eye doctor will start by asking you about your health history. They will examine your eyes thoroughly. During the exam, they will pay special attention to the optic disc, where the nerve fibers leave the eye. They will look for signs of swelling, such as:
- Blurred borders of the optic disc
- A raised appearance of the optic disc
- Blood vessel changes
Your blood pressure will also be checked. This helps rule out severe high blood pressure, known as malignant hypertension. This condition can lead to swelling of the optic disc.
The severity of the swelling will be classified using the Frisén Scale. This grades papilledema from Stage 0 (normal) to Stage 5 (severe swelling). At Stage 5, blood vessels are obscured.
Specialized vision testing
Specialized tests can help measure the amount of swelling and the extent of vision loss.
Visual field testing
This test can create a map showing blind spots or areas of vision loss. Visual field testing can:
- Help assess the severity of optic disc damage
- Monitor changes during treatment
- Detect subtle visual changes
Advanced diagnostic testing
Doctors may order special imaging tests of the eye and brain. These can include optical coherence tomography (OCT) and magnetic resonance imaging (MRI) scans. The tests help measure parts of the eye and brain. This lets doctors check for swelling and find problems that a basic eye exam might miss.
Optical coherence tomography
This technology uses light waves to create detailed images of the optic disc. OCT provides:
- A way to measure optic disc swelling
- A method to track how effective the treatment is
- The ability to detect subtle changes before they become visible during regular exams
Magnetic resonance imaging
An MRI is used to image the brain. This scan helps identify underlying causes. It can detect:
- Brain tumors
- Bleeding or blood clots in the brain
- Structural abnormalities
- Indirect signs of increased pressure
Lumbar puncture (spinal tap)
In some cases, imaging doesn’t identify a clear underlying cause. A spinal tap can check cerebrospinal fluid (CSF) pressure and the fluid’s composition.
Treatment options
Treating papilledema usually starts by addressing what is causing the high pressure. Management will depend on the severity of symptoms and vision loss.
Emergency management
- Hospital stay – Needed for severe papilledema or very high blood pressure that could be dangerous
- IV steroids – May be given to help reduce swelling and inflammation
- Lumbar drain – A small, temporary tube placed in the lower spine to drain excess spinal fluid and quickly lower pressure
Treating underlying causes
- If caused by a brain tumor, treatment can include surgery, radiation and chemotherapy.
- For blood clots in the brain, treatment usually includes blood thinners or surgery.
- For severely high blood pressure, blood pressure-lowering medications will be given.
- For infections causing papilledema, antibiotics will be prescribed.
- To reduce inflammation associated with ICP, steroids may be prescribed.
- Medications may be given that increase CSF absorption or decrease production.
- Lifestyle changes for IIH, such as weight loss, are often recommended.
- Discontinuing medications that might worsen intracranial pressure is recommended.
In some cases, medication and lifestyle changes aren’t enough to decrease ICP. A series of spinal taps or surgery may be needed to relieve pressure or divert excess CSF from the brain.
When ICP returns to normal, papilledema will usually improve gradually over six to eight weeks. Symptoms may last longer with IIH and may require prolonged treatment.
Long-term management and living with papilledema
Management of papilledema can require ongoing medical care and lifestyle adjustments. It’s possible to have mild papilledema for a long time without losing much vision. However, if vision worsens, the damage can become permanent in days or weeks. Quick treatment is crucial to protect eyesight.
Regular monitoring and follow-up care
Management is usually focused on preventing recurrence and preserving vision. How closely you need to be monitored will depend on how severe your condition is. This typically involves:
- Routine and follow-up eye exams
- Imaging to monitor changes
- Medication adjustments
- Coordination between specialists
Recent research and technological advances
Research to improve the detection, diagnosis and treatment of papilledema focuses on:
- Improving imaging techniques
- Enhancing detection accuracy and speed with advanced OCT scans and AI systems
- Noninvasive methods for monitoring intracranial pressure
Lifestyle adaptations and management strategies
Changing your lifestyle can help manage symptoms. Weight management can help to reduce the risk of recurrence for people with IIH. This is because weight gain is the most common cause of relapse. Recommended modifications include:
Lifestyle adaptations
Simple modifications can help manage symptoms:
- Follow the sleep guidelines recommended by your health care team.
- Restrict activities that increase pressure, including heavy lifting or straining.
- Perform low-intensity exercise for overall health and weight management.
- Manage your stress with mindful activities.
- Make household adaptations to improve safety if vision changes have occurred.
- Limit caffeine and ensure you stay hydrated.
Weight management
Weight control is especially critical for people with IIH-related papilledema. Guidelines include:
- Avoiding crash diets while eating healthy and exercising
- Working with a registered dietitian if needed
- Weight loss of 15% to 25% of total body weight (per most recent clinical recommendations)
Medication management
If your doctor has prescribed a medication regimen, be sure to:
- Take the medications as directed
- Work with your health care team to make adjustments to medication if needed
- Speak to your doctor about any side effects
Support and rehabilitation
If vision loss occurs despite treatment, services and support systems are available. Vision rehabilitation services include:
- Low vision aids
- Adaptive techniques
- Orientation and mobility instruction
- Workplace accommodations
Emotional and social support is also available through counseling and support groups.
FAQs
Is papilledema hereditary?
Papilledema itself is not inherited from parents to children. However, some underlying conditions that can cause papilledema may have genetic components. For example, certain rare genetic syndromes can affect brain structure or fluid drainage. Family members may share risk factors, such as obesity or sleep apnea. These can raise the risk of papilledema.
Do migraines cause papilledema?
Migraines do not cause papilledema. Both conditions can cause severe headaches. Headaches from papilledema usually feel worse in the morning and when lying down. In contrast, migraine patterns can vary greatly from person to person.
Does papilledema cause blindness?
Untreated papilledema can lead to permanent vision loss and even complete blindness. Papilledema requires quick evaluation. Early treatment can often prevent significant vision loss. Delayed care raises the risk of lasting damage.
How is papilledema graded?
Doctors use the Frisén Scale to grade papilledema severity from 0 to 5. Grade 0 means the optic disc looks normal. Grade 5 shows severe swelling and complete blockage of blood vessels. The grade doesn’t always reflect the severity. For example, mild papilledema (Grade 1) could be the result of a brain tumor. In contrast, severe swelling might be the result of a more manageable issue.
Optic neuritis vs. papilledema
Optic neuritis is when the optic nerve itself gets inflamed. This can happen due to autoimmune conditions, such as multiple sclerosis. Papilledema results from increased pressure within the skull. This causes the optic disc — where the nerve enters the eye — to swell.
Another difference is that optic neuritis is typically present in one eye, while papilledema is in both eyes. There are rare instances where optic neuritis can be in both eyes, such as neuromyelitis optica spectrum disorder (NMOSD).
How quickly can papilledema develop?
The time it takes for papilledema to develop varies greatly, depending on how fast ICP rises. Sudden pressure from bleeding or blockages can lead to optic disc swelling. This can happen within hours or days. Tumors or fluid buildup can slowly cause visible swelling over weeks.
Maintaining your vision and eye health
Papilledema is swelling of the optic disc due to increased ICP. It requires immediate medical evaluation. Quick diagnosis, along with early treatment, can help prevent permanent damage and vision loss. Managing weight and making lifestyle changes are critical for those with IIH. Once the increased pressure returns to normal, papilledema should gradually improve over the next few months. If you have any concerns about papilledema, reach out to your eye doctor or health care team.