Where does eye mucus come from?
Eye discharge (rheum) is a function of your tear film and a necessary component of good eye health. It primarily consists of thin, watery mucus produced by the conjunctiva (called mucin) and meibum — an oily substance secreted by the meibomian glands that helps keep your eyes lubricated between blinks. (Meibum also helps keep the tear film’s surface smooth and keeps it from evaporating.)
Causes of eye discharge
Sleep in your eyes usually isn’t cause for alarm. But if you notice a difference in consistency, color or quantity of eye gunk, it could indicate an eye infection or disease.
Common eye conditions associated with abnormal eye discharge include:
Conjunctivitis
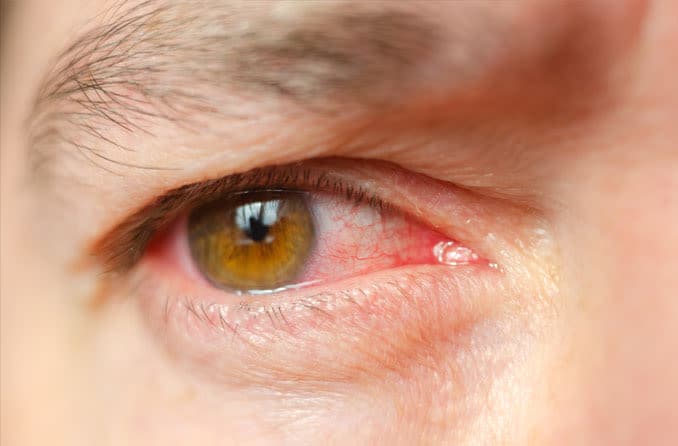
Eye discharge is a common symptom of conjunctivitis (pink eye). This is inflammation of the conjunctiva — the thin membrane that lines the “white” of the eye (sclera) and the inner surface of the eyelids.
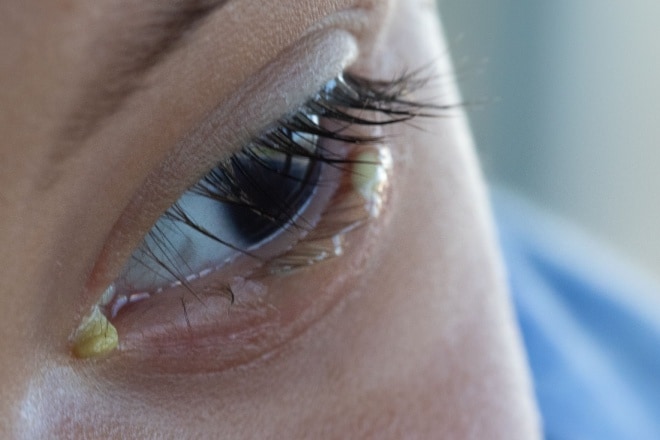
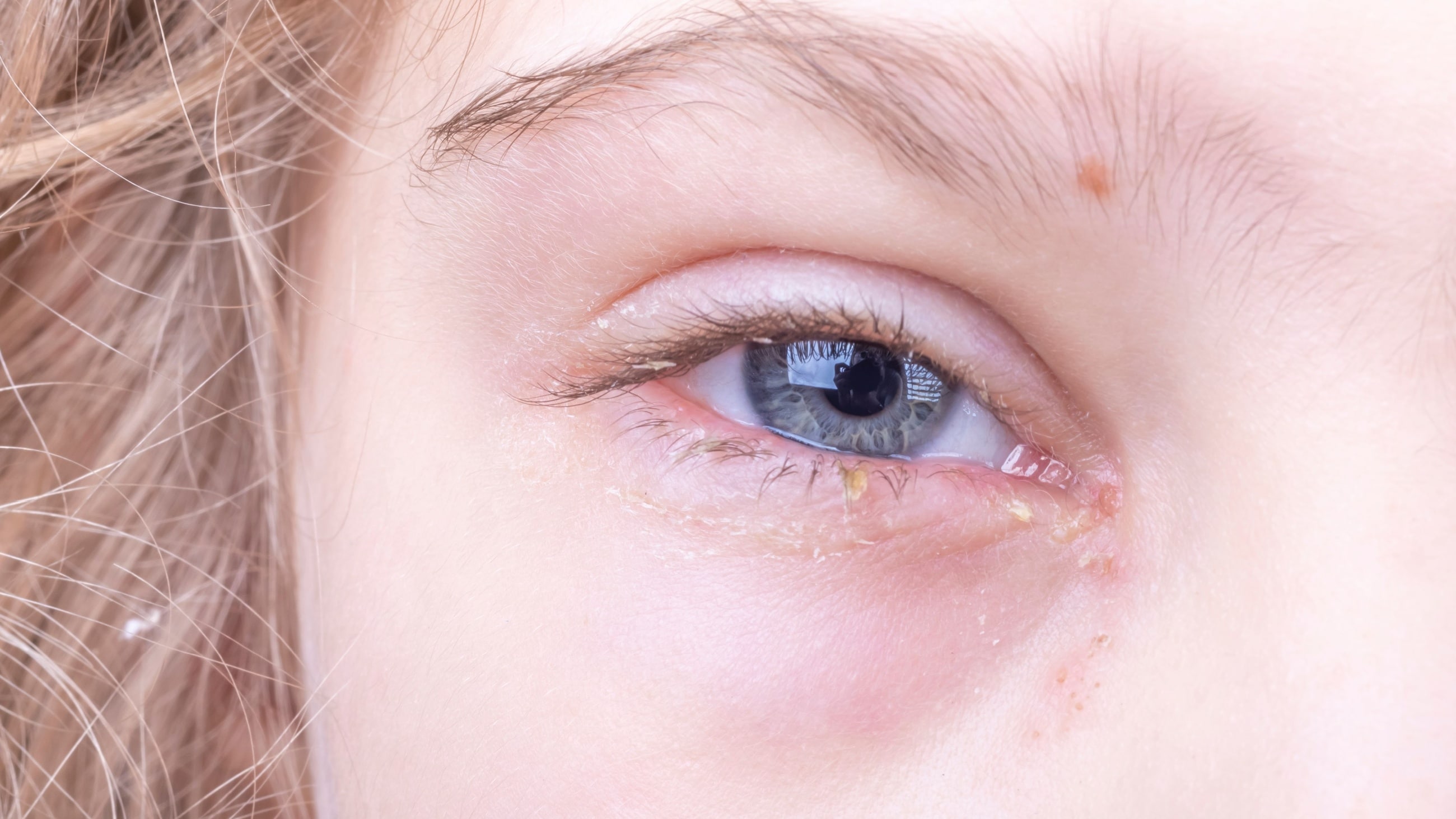
Thick, yellow eye discharge can be caused by an eye infection.
In addition to itchy, gritty, irritated and red eyes, conjunctivitis typically is accompanied by white, yellow or green eye mucus, which can form a crust along the lash line while you sleep.
In some cases, eyelid crusting can be so severe that it temporarily seals your eye shut.
There are three common types of pink eye: viral, bacterial and allergic.
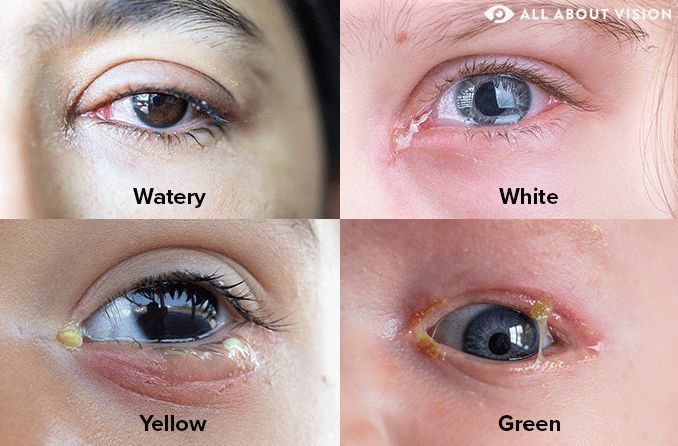
Viral conjunctivitis is highly contagious and is caused by a virus, such as adenoviruses and herpes viruses. Eye discharge associated with viral pink eye is typically clear and watery but may include a white or light yellow mucus component.
Bacterial conjunctivitis, as the name indicates, is caused by a bacterial infection and is also contagious. In some cases, it can be sight-threatening if not treated promptly. Eye discharge is usually thicker and more pus-like (purulent) in consistency than with viral pink eye and is commonly yellow, green or even gray. Often, the sticky mattering may cause your eyelids to feel completely glued shut upon waking in the morning.
Allergic conjunctivitis is triggered by allergens — pollen, dander, dust and other common irritants that cause eye allergies. It can also be caused by an allergic reaction to substances, like chemical pollutants, makeup, contact lens solutions and some eye drops. Eye discharge associated with allergic conjunctivitis is typically watery. However, the discharge can also contain mucus (which is stringy and white), depending on whether the allergy is acute or more chronic.
Unlike viral and bacterial pink eye, allergic conjunctivitis is not contagious and generally affects both eyes.
Other eye infections
In addition to conjunctivitis, there are many eye infections that cause abnormal eye discharge. These include eye herpes (a recurrent viral eye infection), fungal keratitis (a rare but serious inflammation of the cornea) and Acanthamoeba keratitis (a potentially blinding infection typically caused by poor contact lens hygiene or swimming while wearing contacts).
Discharge from an eye infection varies considerably. It could be clear and watery, white and stringy or thick, goopy, green-yellow and sticky. So make sure you see your eye doctor promptly for an accurate diagnosis and treatment.
Blepharitis
A chronic disorder of the eyelids, blepharitis describes inflammation of the eyelid margins that may involve the eyelash hair follicles or abnormal oil production from the meibomian glands at the inner edge of the eyelids. A related condition called meibomian gland dysfunction (MGD) can cause foamy eye discharge and eyelid crusting, among other irritating and occasionally painful symptoms.
Stye
A stye is an infection of an oil gland at the base of the eyelid, typically involving a clogged meibomian gland or an infected eyelash follicle. Also called a hordeolum, it resembles a pimple on the eyelid margin and is commonly accompanied by redness, swollen eyelids and pain or tenderness in the affected area. Yellow pus, eyelid crusting and discomfort while blinking can also occur.
An eye stye usually resolves on its own, but there are also some home remedies for styes you can try. It’s important to refrain from squeezing the pus from a stye to reduce the risk of the infection spreading to other areas of the eye and to avoid damaging the infected oil gland more.
Dry eyes
Insufficient tear production or dysfunction of the meibomian glands can lead to dry eye syndrome. This is often a chronic condition in which the surface of the eyes is not properly lubricated and becomes irritated and inflamed.
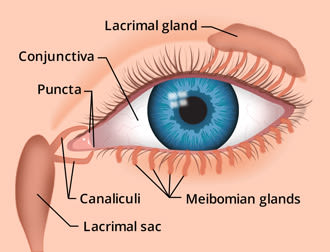
The tear drainage system keeps the eye moist and protected.
Symptoms of dry eyes include:
Sometimes, dry eyes can also cause a very watery eye discharge to occur.
Contact lenses
If you wear contact lenses, you may find more sleep in your eyes than normal. This can be due to a number of reasons, including:
- A contact lens-related eye infection
- Contact lens discomfort resulting in dry and irritated eyes
- Rubbing your eyes more while wearing contacts
- Eye allergies from your contact lenses/giant papillary conjunctivitis
If you experience an increase in eye discharge when wearing contacts, remove your lenses and see your eye doctor to rule out a potentially serious eye condition.
Eye injury
A foreign body in the eye (such as dirt, debris or a chemical substance) or an eye injury can cause your eyes to secrete a watery discharge as a natural protective response.
If eye pus or blood in the eye occurs after an eye injury, see your eye doctor immediately for treatment. All eye injuries should be treated as a medical emergency.
Corneal ulcer
A corneal ulcer is a sight-threatening, open wound on the cornea, usually caused by trauma to the eye or an eye infection. If not treated promptly, corneal ulcers can lead to complete vision loss. Eye pain, redness, swollen eyelids and thick eye discharge are characteristic of a corneal ulcer. Eye pus can be so severe that it clouds the cornea and impairs vision.
Dacryocystitis
When a tear duct is blocked, the lacrimal sac in the tear drainage system leading to the nose can become inflamed and infected, causing a tender and swollen bump to appear where the eyelids come together on the side of the nose. In addition to pain and redness, common symptoms of dacryocystitis include watery eyes and a sticky eye discharge.
Eye discharge treatment
A small amount of eye discharge can be harmless, but if you notice changes in the color, frequency, consistency and amount, consult your eye doctor.
If an eye infection is the cause of the eye discharge, your eye doctor may prescribe medications, such as antibiotic or antiviral eye drops, ointments and pills. If eye allergies are making your eyes watery and irritated, over-the-counter antihistamine eye drops and decongestants may relieve symptoms.
Warm compresses placed over your eyes may help relieve symptoms of itching and general eye discomfort, as well as help remove eye goop.
If your eyelids are stuck together, the proper way to “unglue” your lids is to wet a washcloth in warm water and place it over your eyes for a few minutes before gently wiping away the eye gunk.
At-home checklist
Follow these simple tips to help avoid or manage eye discharge:
- Refrain from touching your eyes to avoid the onset or spread of an eye infection.
- Wash your hands frequently, especially if you have contagious pink eye.
- If you experience eye discharge when wearing contacts, remove your lenses and see your eye doctor. Sometimes switching to daily disposable contacts or a different contact lens material can reduce the risk of contact lens-related discharge.
- If you have an eye infection, discard any potentially contaminated cosmetics, such as mascara and eyeliner, as well as current contacts, which may be contaminated.
- If allergies are the cause of your watery eyes, investigate your environment and try to remove or minimize your exposure to the irritants. And if you’re sensitive to eye drops, try using preservative-free drops.
Note for Parents
Babies and blocked tear ducts
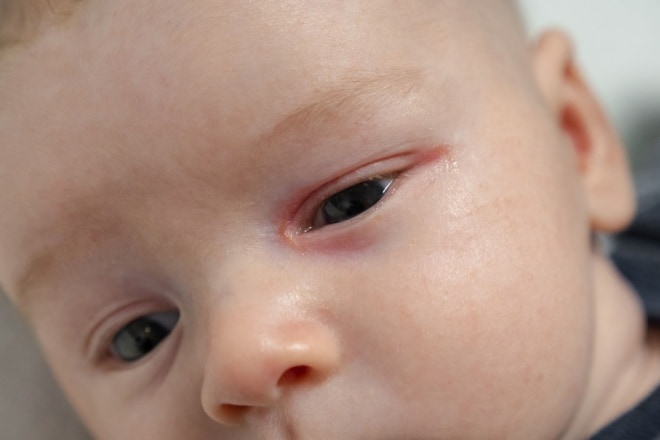
Some babies are born with obstructed tear ducts — the tubes that drain tears from the surface of the eyes to the nasal cavity. This can cause watery eyes and (sometimes) eye discharge.
Symptoms of a blocked tear duct include a constant pooling of tears in the eye (even when the child isn’t crying), which can spill onto the cheek. Sticky eye mucus also may be present, especially collecting on the eyelid margin and causing the eyelashes to stick together.
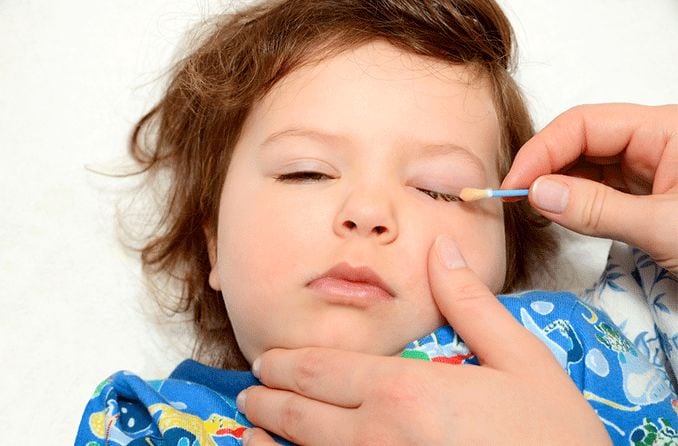
To help relieve symptoms, keep the area clean by regularly wiping your baby’s eyes with a clean, moist cloth. Their doctor may provide guidance on gently massaging the inner corner of your infant’s eyes to help open or unblock the tear duct.
The majority of cases of blocked tear ducts resolve over the first several months of a child’s life. But at the first signs of a blocked tear duct, see your baby’s doctor to rule out a more serious problem.
If your infant’s eyes are producing a thick yellow or green discharge, or there is redness and swelling around their eyes, this could indicate an eye infection that should be evaluated by their eye doctor or pediatrician as soon as possible.
SEE RELATED: Eye discharge in toddlers and babies