What is pink eye?
If you woke up with a red, crusty eye, you might have pink eye. Whether it's caused by a virus, bacteria or allergies, this common condition can disrupt your day with itchy, swollen eyes and uncomfortable discharge. While some types spread quickly, not all forms are highly contagious.
The medical term for pink eye is conjunctivitis. It means swelling or irritation of the conjunctiva. This is the thin, clear layer that covers the white part of the eye (the sclera) and the inside of the eyelids.
Pink eye is uncomfortable but usually not serious.
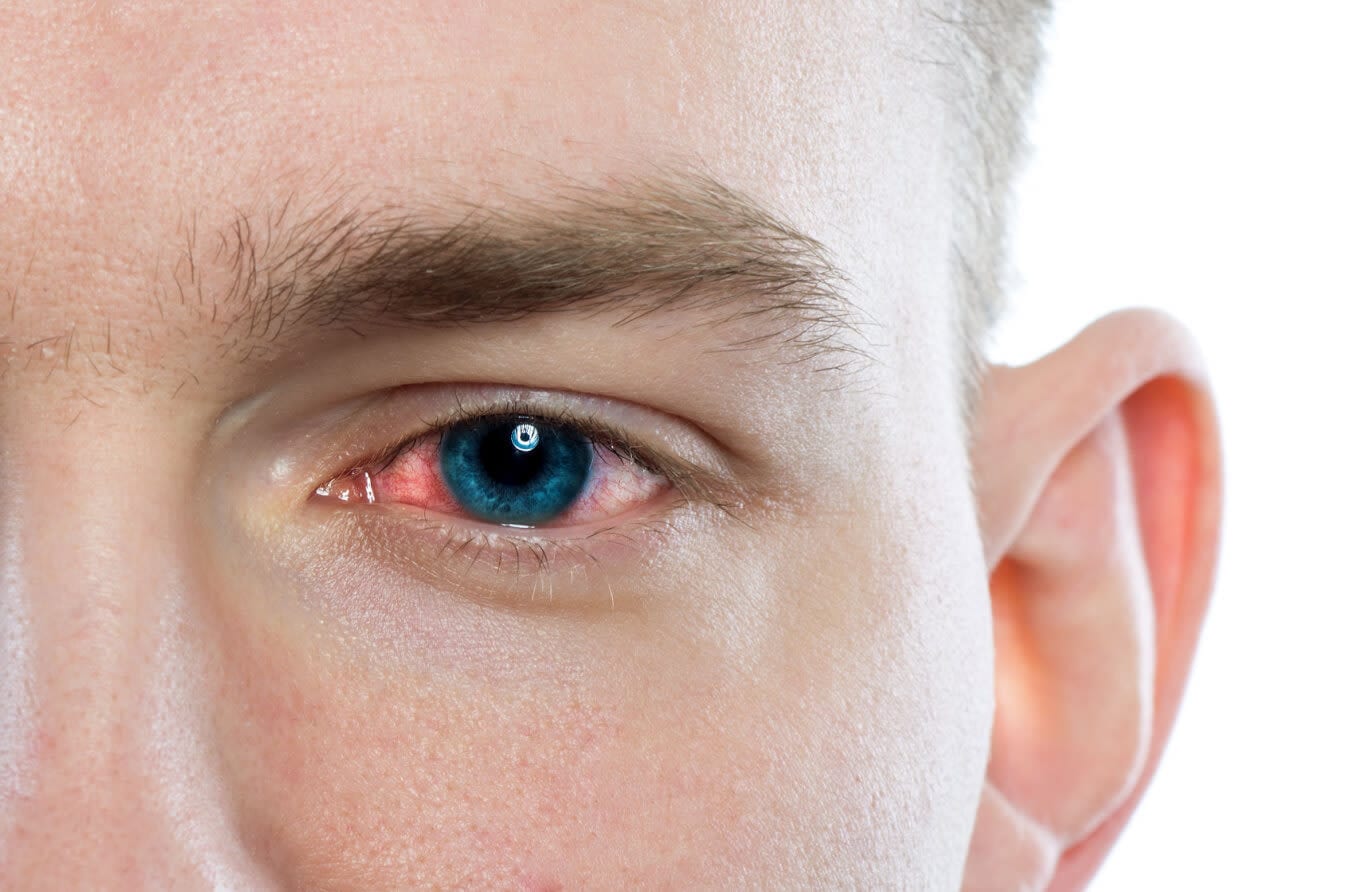
What does pink eye look like?
You may notice the white part of your eye turning reddish or light pink, hence the name pink eye. Your eyes develop a pink hue because the tiny blood vessels in the conjunctiva become irritated and swollen. This makes them more visible and gives the sclera a pink or red appearance.
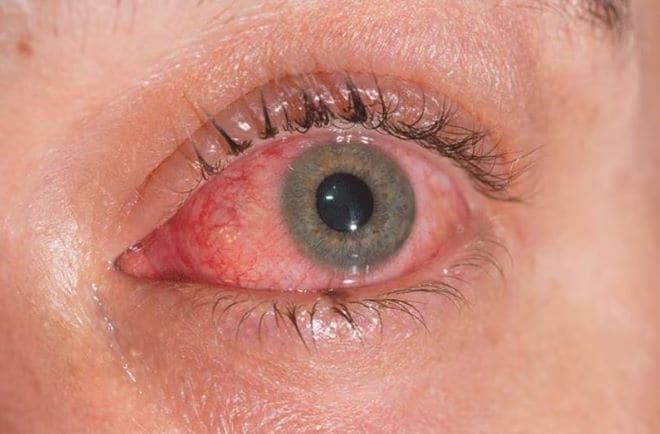
When the conjunctiva swells, it may also cause:
- The inner eyelids appear to redder than usual
- Soreness
- Puffiness
- Crusting
- Discharge
Pink eye signs and symptoms
Conjunctivitis is the most common cause of a red eye. Symptoms — such as discomfort and discharge — can vary depending on the cause. Generally, pink eye symptoms clear up within one to two weeks. Sometimes, however, they can last longer. One way doctors classify conjunctivitis is by how long the symptoms last:
- Acute conjunctivitis – If symptoms last for four weeks or less
- Chronic conjunctivitis – If symptoms last longer than a month
Early-stage symptoms
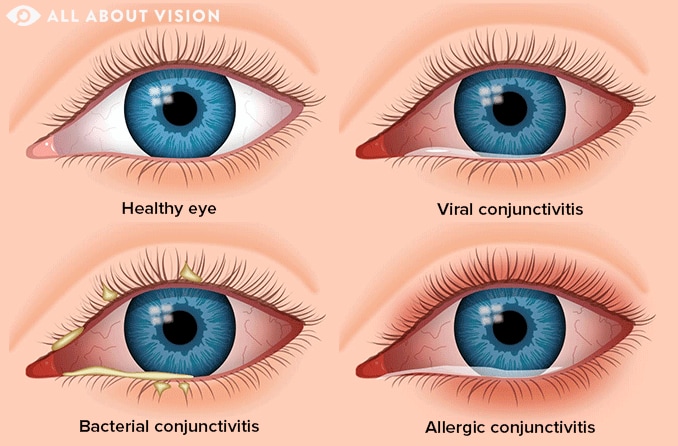
The onset of pink eye can look slightly different depending on whether it is viral, bacterial or allergic. A correct diagnosis can help you begin prompt treatment and get your symptoms under control.
Diagnosing the type of conjunctivitis involves determining:
- What the symptoms are and when they began
- Whether one eye or both eyes are affected
- The type of fluid or discharge coming from the eye
- The degree and location of any swelling
- Whether there were any prior illnesses
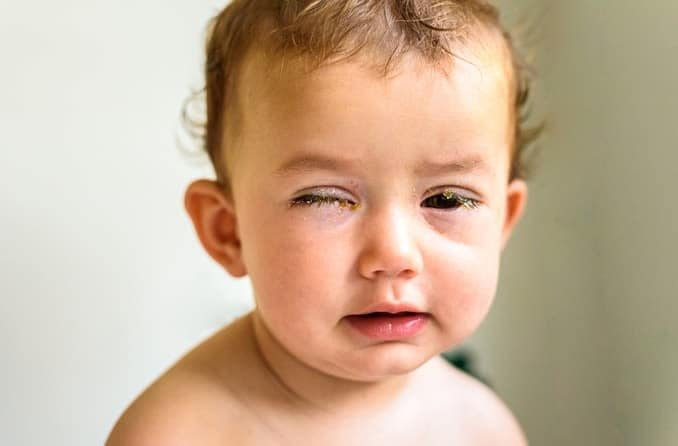
Bacterial pink eye
Bacterial pink usually begins in one eye and can spread to the other eye in a few days. It may occur at the same time as an ear infection. It’s most commonly seen between December and April.
Bacterial pink eye symptoms develop relatively quickly after exposure, within 24 to 72 hours. Early symptoms include:
- Discharge that is thick and yellowish-green in color
- Soreness
- Redness with some swelling of the eyelid
- Eyelids sticking together during sleep
It usually does NOT have significant:
- Itching
- Light sensitivity
- Lymph node swelling near the ear
Viral pink eye
Viral pink eye is the most common cause of infectious conjunctivitis in adults. It begins in one eye and spreads very quickly to the other. It may occur at the same time as a cold or other virus. It’s more common in the summer.
Viral pink eye symptoms can take one to 12 days to develop after a person is exposed. Early symptoms include:
- A clear, watery discharge
- Discomfort (feeling like something is in the eye) and burning sensation
- Redness with some minimal swelling of the eyelid
- Light sensitivity
- Swollen lymph glands in front of the ears
- Development of follicles, tiny raised areas on the inside of the eyelid, as an immune response to the virus
When viral conjunctivitis affects only the eyes without other symptoms, it's most often caused by adenoviruses, the same family of viruses responsible for a typical cold.
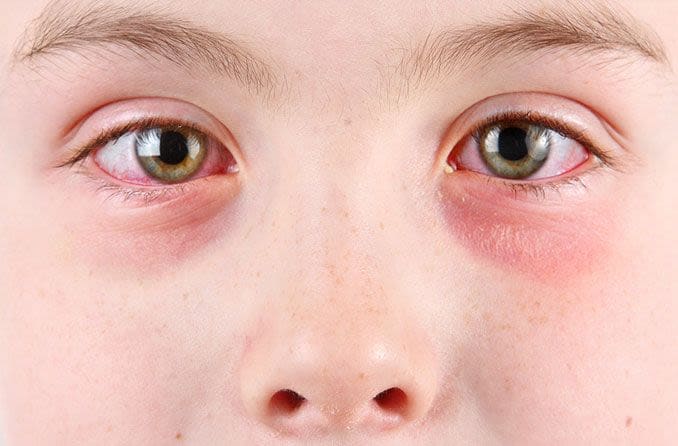
Allergic pink eye
If pink eye is caused by an allergy, both eyes are usually affected at once. This is not an infectious condition. It is the result of an allergic reaction to pollen, dust, mold or another trigger. Early symptoms include:
- Intense itching (in contrast to viral and bacterial pink eye)
- Clear and stringy discharge
- Moderate to severe eyelid swelling
Risk factors and complications
Most cases of pink eye improve without causing other problems. However, rare complications of untreated pink eye may lead to permanent eye damage. Complications may include:
- Keratitis – Inflammation or infection of the cornea, the clear layer at the front of the eye
- Keratoconjunctivitis – Inflammation or infection of both the cornea and the conjunctiva
- Corneal ulcer – Painful, open sore that forms on the cornea and can lead to vision loss
- Trachoma – Caused by Chlamydia trachomatis, it leads to scarring of the inner eyelid and eventually the cornea
- Uveitis – Swelling of the eye's middle layer (the uvea) that causes severe pain and blurred vision
- Recurrent corneal erosions – The surface layer of the cornea repeatedly breaks down, causing pain and blurry vision
Prompt treatment helps lower the risk of serious complications. Contact your eye doctor if symptoms persist or worsen after several days, and especially if they include:
- Severe pain and redness
- Blurry vision
- A large amount of discharge
- Significant sensitivity to light
Who is at higher risk?
Certain groups of people are at higher risk for complications. If you or a family member has pink eye (or pink eye symptoms) and belongs to one of these groups, contact an eye doctor as soon as possible:
- Contact lens wearers – If you wear contact lenses or have recently scratched your eye.
- Immunocompromised individuals – If you have a medical condition that lowers your body's ability to fight sickness, such as cancer or HIV.
- People who may have measles – If someone with pink eye is also suspected of having measles, complications can cause permanent vision loss.
- Newborn babies – Exposure to bacteria and viruses during birth can lead to neonatal conjunctivitis (from chlamydia, gonorrhea, herpes simplex virus or streptococcus) and serious complications.
Causes of pink eye
Pink eye is most often caused by viruses, bacteria or allergens. It is important to know that:
- The types of pink eye caused by viruses and bacteria are highly contagious and easily spread from person to person.
- Pink eye caused by allergens or irritants, such as chemicals or smoke, is not contagious.
- It can sometimes be difficult to determine which type of pink eye someone has.
Viral conjunctivitis
Viral pink eye is highly contagious. In general:
- It is usually acute, meaning symptoms last for four weeks or less.
- When it occurs without other illnesses in the body, it is usually caused by adenoviruses, which account for up to 90% of cases.
- It may occur along with common colds or other widespread viral infections, such as measles, mumps, rubella or chickenpox.
- Antibiotic drops do not help.
Epidemic keratoconjunctivitis (EKC) is a severe, highly contagious form of viral pink eye caused by certain adenoviruses. It is different from regular pink eye in that it affects both the conjunctiva and the cornea (the clear front part of the eye). This corneal inflammation, called keratitis, typically develops around four days or more after your symptoms first appear.
Adenoviruses can infect various parts of the body, including the:
- Eyes – Resulting in severe conjunctivitis
- Respiratory system – Resulting in the common cold and other respiratory infections
- Digestive system – Resulting in the stomach flu and gastrointestinal illnesses
Important note
People who are not vaccinated for measles can develop pink eye. It can occur before a rash appears or while someone has a rash. If you suspect pink eye related to measles, contact an eye doctor immediately. Complications can lead to permanent vision loss, and treatment is critical.
Bacterial conjunctivitis
Bacterial pink eye is a very common eye condition that spreads easily. Most cases clear up on their own in about 10 days. Bacteria can infect the eye by direct contact with the hands or be introduced from the nose or sinuses.
Some strains of bacteria can cause long-lasting symptoms, so antibiotics may be needed to prevent complications. Antibiotics have been shown to reduce symptoms more quickly by helping to eliminate the bacteria from the eye.
Acute bacterial conjunctivitis is typically caused by:
- Staphylococcus aureus
- Streptococcus pneumoniae
- Haemophilus influenzae
It is less commonly caused by:
- Moraxella catarrhalis
- Chlamydia trachomatis
- Neisseria gonorrhoeae
Allergic conjunctivitis
Chronic eye itching is usually due to eye allergies, also known as allergic conjunctivitis. People with eye allergies often experience nasal allergies at the same time, such as sneezing and a runny, stuffy nose. Allergic conjunctivitis is usually seasonal and not contagious.
What causes allergic conjunctivitis?
Allergic conjunctivitis develops when the immune system mistakenly identifies an allergen or allergens as harmful. Here’s how the body responds:
- During the first exposure to an allergen, the body produces an antibody called immunoglobulin E (IgE).
- IgE antibodies bind to specialized immune cells called mast cells, preparing them to respond to the next exposure.
- Repeated exposure triggers mast cell activation, releasing a compound called histamine.
- Histamine causes the typical symptoms of allergic conjunctivitis: itching, redness and swelling. It also dilates the blood vessels in the conjunctiva, causing redness in the eye.
Two phases of allergic reactions exist:
- The fast reaction phase – Occurs within minutes, causing intense itching, watery eyes and redness.
- The late reaction phase – Develops hours later, resulting in prolonged inflammation and discomfort.
Seasonal and year-round allergies
Seasonal allergies occur at specific times, mainly in spring and summer. They are often due to airborne allergens such as:
- Tree pollen
- Grass pollen
- Weeds
Year-round allergies cause symptoms throughout the year from indoor allergens such as:
- Dust mites
- Pet dander
- Mold
Rare conditions like atopic keratoconjunctivitis (AKC) and vernal keratoconjunctivitis (VKC) can cause severe year-round symptoms.
Environmental irritants
Environmental irritants can also trigger symptoms. These include:
- Airborne pollutants – Smoke, smog, dry weather and strong winds blowing particles in the air
- Foreign body in the eye – Sand, dirt, an eyelash or even eyelash extensions
- Eye and makeup products – Mascara, eyeliner, eyeshadows, creams and lotions
- Chlorinated pool water – Pool chemicals can irritate the outer layers of the eye
- Eye drop preservatives – Preservatives such as benzalkonium chloride (BAK)
Other causes
Giant papillary conjunctivitis (GPC) is usually caused by eye irritation associated with contact lens use. Although allergies can worsen the condition, GPC primarily results from the contact lens rubbing against the eyelid.
Symptoms of GPC include:
- Increased itching
- Mucus discharge
- Difficulty wearing the contact lenses
- Sensation of a foreign object in the eye
- Development of large bumps (papillae) on the inner upper eyelid
Diagnosing pink eye
To diagnose conjunctivitis, your eye doctor will look at your eye and ask about your history. For example, they may ask:
- About any itching, pain, vision changes or discharge
- When you first noticed the symptoms
- Whether you’ve been in contact with other people with pink eye
- If you’ve had a cold or other illness recently
- Whether you’ve had any recent eye injuries
- Whether you’ve started using any new products
- If you wear contact lenses
- If you have any other health conditions
The exam will include a vision check. Your eye doctor will use a slit lamp to examine your eyelids, eye surface and the conjunctiva inside your eyelids as part of the evaluation. They may take a swab of the fluid from your eye for lab tests. The results can help determine your treatment.
Treatment options for pink eye
When treating pink eye, doctors focus on three main goals:
- To help you feel more comfortable
- To shorten the time to recovery
- To stop an eye infection from spreading to others
Medical treatments
Most cases of pink eye clear up on their own within one to two weeks. However, if your symptoms are severe or worsening, it is important to see an eye doctor.
Viral pink eye
Viral pink eye cannot be treated with antibiotics. These drugs are only effective against bacterial infections. Fortunately, most people who develop viral pink eye have mild symptoms that resolve within two weeks. Occasionally, it may take two to three weeks or longer to fully clear.
For more severe cases of viral conjunctivitis, a doctor may prescribe antiviral medication to help the infection clear up more quickly. This is usually recommended for:
- Herpes simplex virus (this also causes sores or blisters)
- Varicella-zoster virus (this also causes chickenpox and shingles)
Bacterial pink eye
Mild bacterial pink eye may resolve on its own and usually improves in two to five days, though complete recovery might take up to two weeks.
Your doctor may prescribe antibiotics in the form of eye drops or ointments. They will determine the medication based on the type of infection. These medications can:
- Shorten the infection duration
- Minimize complications
- Reduce the risk of transmission
Contact your doctor if they have prescribed antibiotics for bacterial conjunctivitis and your symptoms have not improved after 24 hours.
Allergic pink eye
When symptoms of eye allergies are chronic or severe, your doctor may need to prescribe allergy eye drops to control the itching and discomfort. Prescription medication can work quickly and provide longer-lasting relief. These include:
- Combination eye drops – Many prescription eye drops contain both an antihistamine to relieve immediate itching and a mast cell stabilizer to help manage symptoms long-term.
- Mast cell stabilizers – These drops inhibit the release of histamine and other inflammatory mediators. They help prevent flare-ups and help manage symptoms long-term.
- Corticosteroid eye drops – For short-term relief of severe eye allergies, they reduce swelling, redness and itching quickly.
- Nonsteroidal anti-inflammatory drugs (NSAIDs) – These help relieve symptoms of itching and discomfort.
Home remedies for temporary symptom relief
Home remedies can often ease eye discomfort and help prevent mild irritation from turning into a more serious infection.
First, resist the urge to rub your eyes. This pressure triggers immune cells to produce additional histamine. This can make itching and redness worse.
Try these at-home treatments to see whether they provide relief. If symptoms persist or worsen, it’s important to consult your doctor:
- Apply a clean, cold cloth or compress to your closed eyes to reduce swelling and irritation.
- Use a wet washcloth to clear crusting from your eyes.
- Wear sunglasses to help with light sensitivity.
- Stop wearing contact lenses and avoid eye makeup.
- Use only the eye drops or ointment prescribed by your doctor.
- Use preservative-free artificial tears.
- Take an over-the-counter painkiller like ibuprofen.
In addition to these remedies, if you have allergic conjunctivitis:
- Limit exposure to allergy triggers.
- Take an oral antihistamine to help manage allergy symptoms.
- Wash your hands after spending time outdoors or touching pets.
- Shower at night to remove pollen.
- Stay indoors when the air quality is poor.
- Wear wraparound sunglasses to prevent airborne allergens from bothering your eyes.
- Keep your windows closed and use air conditioning instead.
- Wash bedding and pillowcases frequently and use allergy-reducing covers.
- Keep pets out of your bedroom to reduce dander exposure.
- Minimize carpets and use damp rags or mops for cleaning.
Some home remedies for pink eye can be harmful. Only use safe, doctor-recommended treatments. Avoid the following:
- Unsterilized herbal treatments and foods
- Redness-reducing drops
- Breast milk in the eyes, which can introduce bacteria that worsen the infection.
Does pink eye go away on its own?
Most cases of pink eye clear up on their own within a few weeks. How fast it clears up depends on the underlying cause. Contact your eye doctor if your symptoms are severe or getting worse.
Viral pink eye
Most cases of viral pink eye are mild and do not need medical treatment. The infection typically clears up within seven to 14 days, though it can take two to three weeks.
Bacterial pink eye
Mild cases generally clear up in two to five days without antibiotics. They typically do not lead to other complications. However, antibiotics are sometimes necessary, and it may take up to two weeks for symptoms to completely resolve.
Allergic pink eye
Allergic pink eye usually improves once individuals are no longer exposed to the allergen(s) causing the conjunctivitis.
How to prevent pink eye from spreading

Pink eye caused by a virus or bacteria can spread easily, especially when discharge is present. The first step to prevention is taking precautions. To stop the infection from spreading:
- Wash your hands often and thoroughly.
- Avoid rubbing your eyes.
- Use hand sanitizer if soap and water are not available.
- Avoid sharing towels, personal eye care products and eye makeup.
- Change pillowcases often.
- Do not reuse tissues or hand towels on your face.
- Follow your eye doctor's specific directions for using and taking care of your contact lenses.