What is scleritis?
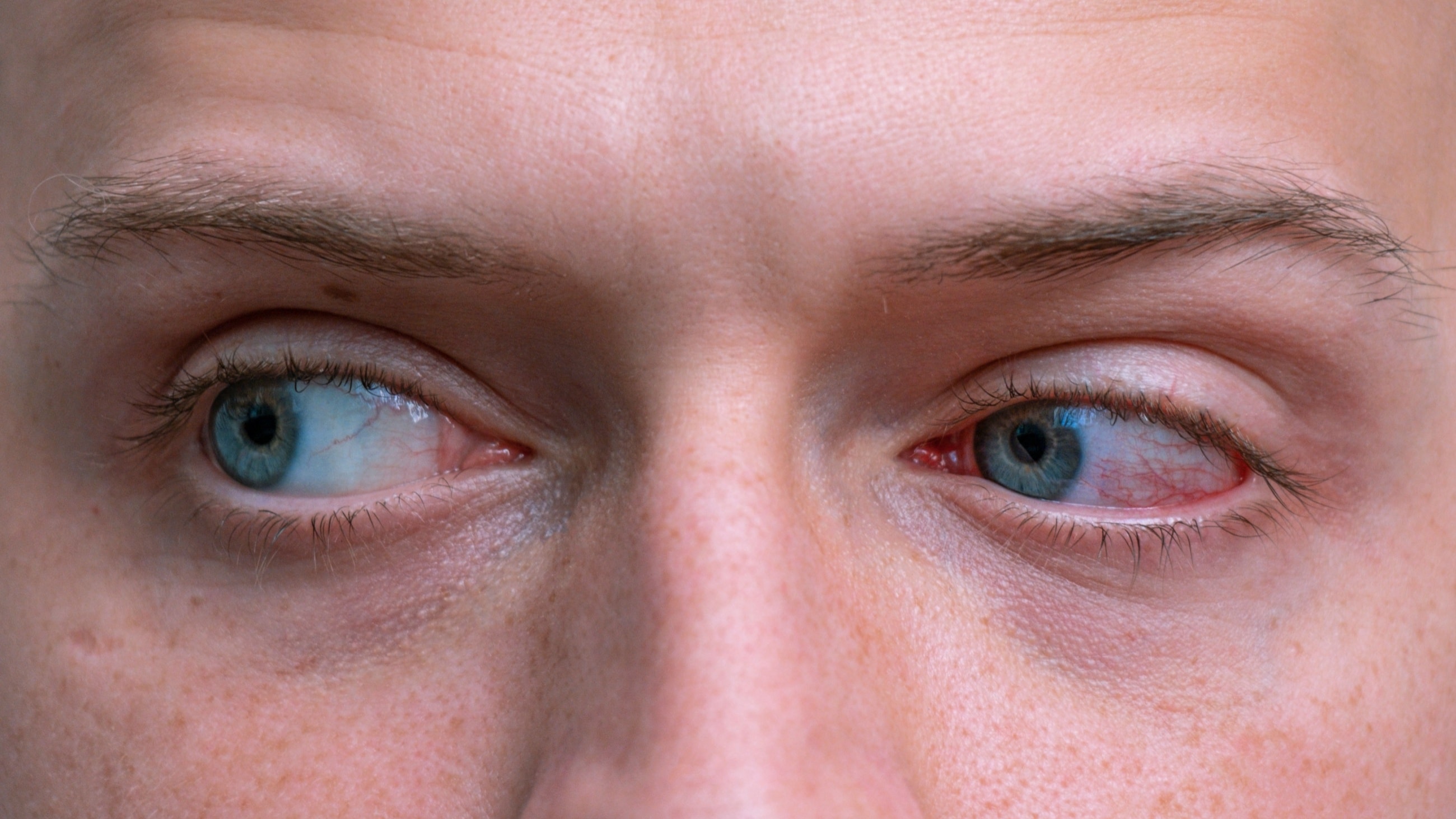
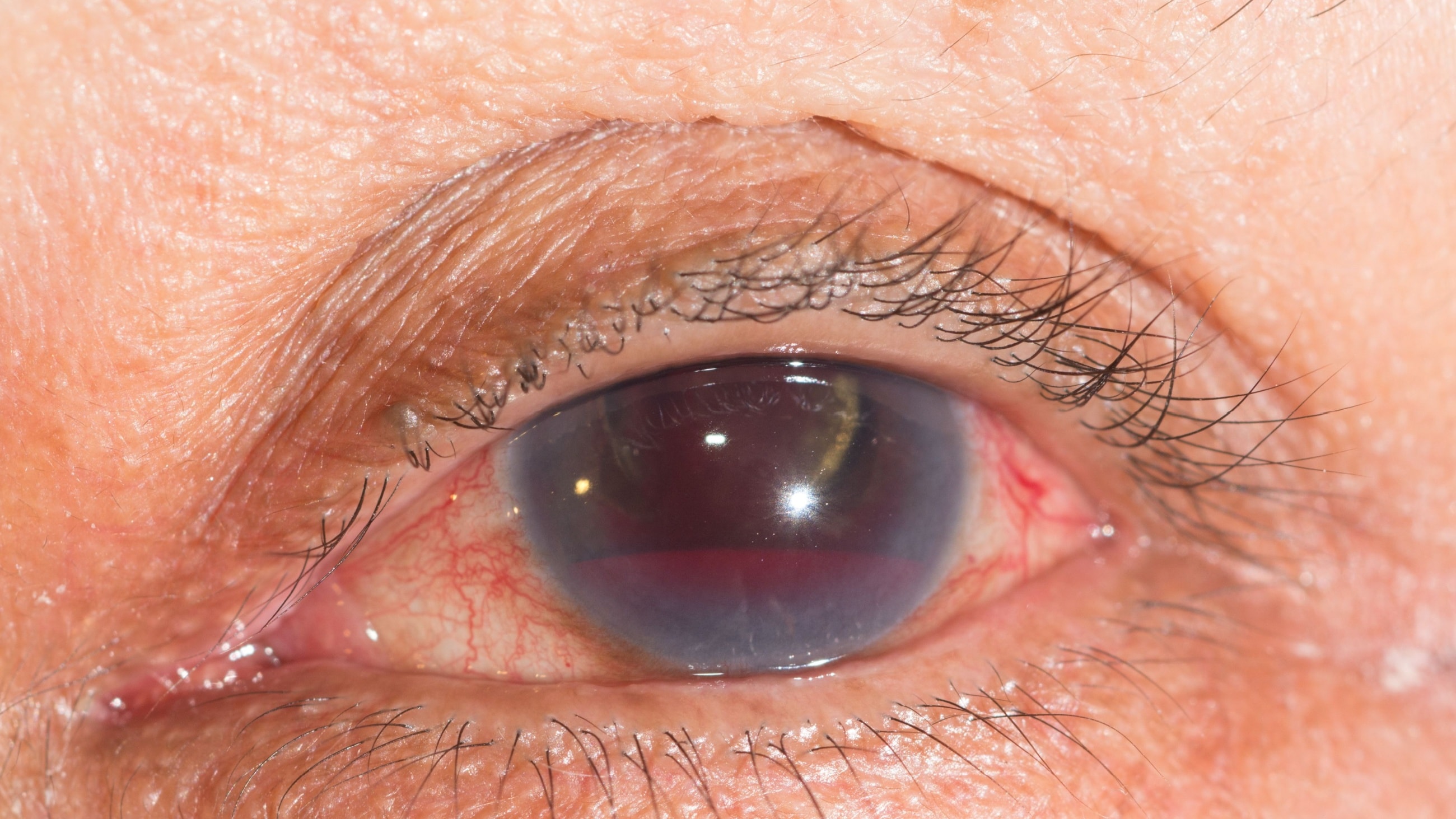
Scleritis occurs when the white of the eye (the sclera) becomes significantly inflamed. While often associated with autoimmune diseases, it can be caused by eye trauma, infections or other conditions. Prompt care is essential to prevent this inflammation from affecting other parts of the eye and potentially causing vision loss.
Scleritis is a type of inflammatory eye disease — a condition that causes inflammation in the eye. It specifically affects the sclera, which is made up of strong, dense tissues that help keep the eye round and protect its more delicate internal structures.
The sclera begins on the front side of the eye, where it meets the cornea (the clear dome-shaped structure on the eye’s surface). It then wraps around to the back of the eye to connect with the optic nerve (the structure linking the eye to the brain).
How common is the condition?
Scleritis affects about 10,500 people in the United States each year, according to some studies. Women are more likely to experience the condition than men. It can affect people of all ages, but it most often occurs between the ages of 47 and 60. Scleritis is rarely found in children.
Signs and symptoms of scleritis
Scleritis can affect one or both eyes. It’s usually slow to develop but can become severe over time. Signs and symptoms of the condition can include:
- Eye pain or tenderness, which can be described as “boring” pain
- Eye redness
- A blue or purplish discoloration of the sclera
- Swelling of the sclera
- Blurry vision
- Watery eyes
- Light sensitivity (photophobia), typically described as “extreme”
Pain with scleritis can be severe, especially when moving the eyes, and may be more intense at night. The pain can also radiate to other parts of the face, jaws and head.
When to seek medical attention
Scleritis can lead to vision loss and other issues without timely care. If you experience eye pain, redness or other scleritis symptoms, contact an eye doctor promptly to schedule an eye exam.
The condition can go through periods of remission (when the disease is inactive) and flare-ups (when it’s active). It’s very important to visit your eye doctor if you have any new or recurring eye-related symptoms.
Types of scleritis
The types of scleritis are categorized based on whether they occur in the anterior (front) or posterior (back) of the eye. You could have both anterior and posterior scleritis at the same time.
Anterior scleritis
Anterior scleritis affects the front portion of the sclera. It’s the most common type, with over 90% of cases involving this form.
Anterior scleritis is further classified into three subtypes:
- Diffuse – Inflammation occurs across the entire surface or a portion of the sclera. This is the most common type of anterior scleritis. Signs and symptoms generally include redness and irritation of the sclera.
- Nodular – One or more distinct nodules develop on the sclera, often in a localized area. These raised areas can be tender or painful to the touch.
- Necrotizing – Inflammation damages the scleral tissues and can spread to other parts of the eye. This is the most severe form and is often extremely painful.
Posterior scleritis
Posterior scleritis affects the back portion of the sclera and is much rarer than the anterior form. Symptoms can include eye pain and tenderness, especially with eye movement, along with decreased vision. Posterior scleritis can lead to other serious acute eye conditions and chronic eye diseases, such as retinal detachment and glaucoma.

Causes of scleritis
Scleritis often occurs alongside autoimmune disorders and can indicate an underlying systemic condition. It can also result from eye diseases, eye surgery and use of certain medications. In some cases, the cause might be idiopathic, meaning it’s unknown.
Autoimmune connections
Around half of the people diagnosed with scleritis have an autoimmune disorder. This is a type of condition where the body’s immune system, which normally fights off germs and helps prevent diseases, mistakenly targets healthy tissues. Many autoimmune conditions can cause inflammation throughout the body, including the eyes.
Autoimmune diseases commonly associated with scleritis include:
- Rheumatoid arthritis
- Lupus
- Sjögren’s syndrome
- Inflammatory bowel disease (IBD)
- Scleroderma
- Granulomatosis with polyangiitis
- Sarcoidosis
- Vasculitis
Other causes
While scleritis is commonly linked to autoimmune conditions, additional factors may contribute to its development, including:
- Eye injuries
- Other types of eye trauma (such as surgical procedures)
Rarer causes of the condition involve:
- Eye infections – Pathogens such as bacteria, viruses, parasites and fungi might be responsible for a small percentage of scleritis cases.
- Bisphosphonates – These are medications prescribed to treat osteoporosis and other bone conditions. A rare side effect of these drugs can include eye (and scleral) inflammation.
Which eye diseases are similar to scleritis?
Several eye diseases share symptoms with scleritis, such as eye inflammation and redness. Because these conditions can look and feel alike, it’s important to visit your eye doctor for an accurate diagnosis.
Scleritis vs. episcleritis
The episclera is a thin layer of tissue that sits on top of the sclera. When this layer becomes red and inflamed, it’s referred to as episcleritis. Some of the autoimmune diseases linked to scleritis can also be associated with episcleritis.
The main difference between these two conditions is that episcleritis usually goes away on its own within three weeks. In contrast, scleritis is a more serious condition that requires careful follow-up care. Scleritis typically results in significant pain and swelling and can lead to vision loss and other problems.
Scleritis is also often painful, whereas episcleritis could be described as having symptoms of discomfort.
Scleritis vs. conjunctivitis
The conjunctiva is the layer of tissue that covers the sclera and the inner surfaces of the eyelids. When it becomes inflamed, it is referred to as conjunctivitis (pink eye). Allergies, infections and chemical irritants are the most common causes of this condition.
Both scleritis and conjunctivitis cause eye redness and inflammation. But conjunctivitis typically causes milder discomfort rather than severe pain, and blurry vision is less common unless the cornea is involved.
Scleritis vs. uveitis
Uveitis occurs when the uvea (the middle part of the eye) becomes inflamed. The uvea is located between the sclera and the retina (the light-sensitive membrane at the back of the eye). Some of the autoimmune conditions linked to scleritis may also be associated with uveitis.
The uvea has three segments:
- Iris – The colored portion of the eye
- Ciliary body – A muscular ring of tissue located behind the iris
- Choroid – The layer of blood vessels between the sclera and the retina
Uveitis develops when one or more of these structures becomes inflamed. It’s classified into different types based on where in the uvea the inflammation occurs.
Uveitis tends to cause many of the same symptoms as scleritis, including eye pain, redness and blurry vision. However, they might affect different parts of the eye. An eye exam can help a doctor determine which condition is present.
Diagnosis
Because scleritis can damage your vision if left untreated, it’s imperative if you experience any symptoms to get checked as soon as possible.
Diagnosing scleritis usually begins with a health history review and a comprehensive eye exam. This can help eye doctors differentiate between scleritis and other inflammatory conditions. Ocular imaging, such as an ultrasound or magnetic resonance imaging (MRI), may be performed to detect whether scleritis is affecting deeper tissues.
If scleritis is present, your eye doctor may collaborate with your primary care doctor or an autoimmune disease specialist (rheumatologist). Blood tests and other medical evaluations may also help confirm a diagnosis.
Treatment options
Doctors typically treat scleritis according to the type, severity and causative factor(s). Treatment is aimed at reducing inflammation and typically involves the following:
Medications
One or more types of medications may be prescribed to treat scleritis. These can include:
Oral medications
- Corticosteroids – Reduce inflammation throughout the body.
- Nonsteroidal anti-inflammatory drugs (NSAIDs) – Help control pain and swelling.
- Antibiotics – Used if a bacterial infection is present.
- Antiviral medications – Used when a viral infection contributes to scleritis.
- Immunosuppressive drugs – Prescribed when scleritis is linked to an immune system response.
Topical (eye drops)
- Corticosteroid eye drops – Reduce inflammation in the eye.
Injections and intravenous (IV) medications
- Corticosteroid eye injections – May be recommended in more severe cases or when topical or oral steroids cannot be used.
- Biologic agents – Given via a subcutaneous (under-the-skin) injection or intravenously for more severe or resistant cases that have not responded to conventional treatments.
- IV immunosuppressive drugs – May be used in severe cases or when oral medications are ineffective.
Surgical interventions
The most serious cases of scleritis may lead to thinning of the sclera or openings in the tissue (called perforation) that expose underlying structures. Surgery may be needed to graft healthy tissue onto these areas to further strengthen and re-support the sclera.
Living with scleritis
Scleritis can cause vision and daily life challenges. You could help ensure an optimal long-term prognosis by:
- Getting prompt treatment.
- Managing symptoms and any underlying health conditions.
- Taking steps to reduce the risk of scleritis flare-ups.
Managing symptoms
Your eye doctor may prescribe treatments to help manage the condition and control inflammation. The following tips can also help control your symptoms and improve your comfort:
- Take medications as directed – Use prescribed medications, including eye drops, exactly as recommended by your doctor.
- Use cool compresses – Placing a cool, damp washcloth over your closed eye may help relieve swelling and discomfort.
- Avoid contact lens use – Don’t wear contacts (if you use them) until your eye doctor tells you it’s safe to do so.
Visit your eye doctor right away if you experience any new or recurring symptoms.
Preventive measures
You may not always be able to prevent scleritis from developing. But the following steps could help keep your eyes healthy and lower your risk of disease flare-ups:
- Protect your eyes – Wear proper eyewear to protect your eyes from injuries during sports and other high-risk activities.
- Reduce your risk of eye infections – Wash your hands thoroughly before touching your eyes. Follow proper contact lens hygiene protocols as recommended by your eye doctor, and avoid touching the tip of any eye drop bottle to your eye.
- Manage underlying health conditions – Work with your primary care doctor or rheumatologist to keep any autoimmune conditions under control.
- Follow treatment recommendations – Attend all follow-up appointments and follow your doctors’ treatment instructions closely.
Your eye doctor may suggest other measures to help keep your eyes healthy, manage the condition and reduce the risk of vision problems.
Long-term outlook
The prognosis for scleritis is generally good when it’s treated in the early to moderate stages. However, the risk of vision loss may be higher with certain forms, such as necrotizing anterior scleritis and posterior scleritis, especially if the inflammation affects other parts of the eye.
Early treatment of the disease and proper management of any underlying factors are crucial for protecting your vision.
Future research and developments
Research is ongoing to explore precise methods of detecting, monitoring and treating scleritis. Current studies focus on factors such as:
- Identifying biomarkers – Researchers are studying certain proteins in the blood and tears that could serve as biomarkers for scleritis. This could potentially allow for minimally invasive diagnostic tests and assist doctors in monitoring the condition.
- Ongoing research on biologic agents – Scientists continue to study the use of new and existing biologic therapies for treating certain types of scleritis.
- Repurposing existing drugs – Researchers are investigating certain existing drugs for their potential to treat scleritis. They may help reduce inflammation and regulate the immune system.
When to see a doctor
Scleritis is a potentially serious condition that can affect your eyesight without prompt care. Contact your eye doctor right away if you develop significant eye pain, redness, swelling, blurry vision, light sensitivity or other symptoms. Early intervention could help protect your eye health and vision.