Get help right away if you have:
- Had an object pierce the eye
- Extreme pain
- Unusual discharge, such as yellow, green or bloody pus, from your eye
- Significant vision loss, flashes or new onset of floaters in your vision
- Developed a fever
- A white or cloudy spot develop on your cornea
- Blood or pus visible inside the eye
- A chemical splashed in the eye
- A sudden return of severe pain
How do you treat a corneal abrasion?
Small scratches typically heal quickly on their own, often within a day or two. But if you continue having issues, you should see an eye doctor to make sure the injury heals properly.
First steps for relief
Follow these guidelines to relieve symptoms and prevent the injury from worsening. Remember first to wash your hands and do not rub your eye.
What to do
- If a chemical splashes into your eye – Rinse your eye immediately with saline or clean water (in the shower or sink) for at least 10 minutes. Then go to the emergency room.
- If dirt or debris scratches your eye – Gently rinse your eye with clean water or sterile saline. You can use an eye cup from a drug store or a small, clean glass. Try gently pulling your upper eyelid over the lower lid to help remove any trapped debris.
- If you wear contact lenses – Rinse your eye first. After several minutes of gently flushing with clean water, if the lens hasn’t come out on its own, you can then carefully try to remove it.
- Use artificial tears – Applying artificial tears can help keep the eye comfortable.
- Use a cool compress – Placing a moist, cool compress over your closed eye can soothe pain and reduce irritation.
- Wear sunglasses – If your eye is sensitive to light, sunglasses can make you more comfortable.
What not to do
- Don’t rub your eye – This can make the eye scratch worse or push debris deeper into the eye.
- Don’t try to remove a stuck object with your fingers or tools – Let an eye doctor do it safely.
- Don’t wear contact lenses – Wait until an eye doctor tells you it’s safe.
- Don’t use eye drops that reduce redness – These do not help heal the eye and can make the pain worse.
Medical care and recovery
Treatment for corneal abrasion focuses on easing pain, helping your eye heal and preventing infection. At your appointment, your eye doctor will look for any particles or deeper injuries.
If something is stuck in your eye, the eye doctor will remove it carefully using special drops and instruments. After your eye is cleaned and the diagnosis is confirmed, you’ll get a recovery plan specific to your needs.
Your treatment may include:
- Infection prevention – Antibiotic eye drops or ointment are often prescribed to prevent an infection.
- Pain relief – Your eye doctor may recommend over-the-counter pain medicine like ibuprofen to help with discomfort from a mild abrasion. For severe pain, stronger medication or special pain-relieving eye drops may be prescribed for a short time.
- Managing light sensitivity – If you have severe sensitivity to light, your eye doctor may use special drops (called cycloplegic eye drops) to relax your eye muscles. These drops can blur your vision temporarily.
- Eye patch or bandage contact lens – In some cases, an eye patch or a special bandage contact lens may be used to shield your eye and make it more comfortable.
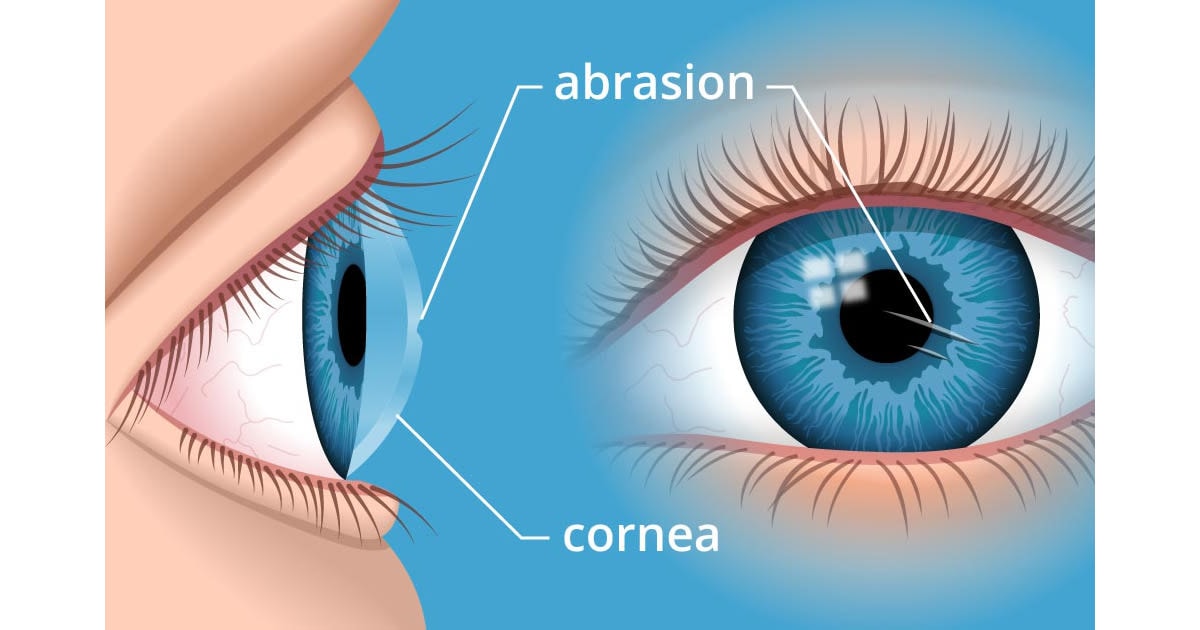
Superficial vs. deep corneal abrasions
All corneal abrasions are painful, but the impact on long-term vision can vary. The cornea consists of five distinct layers, and your recovery depends on the type of injury and the layers that are affected.
How the depth of a corneal abrasion affects vision
The depth of the injury — and which layers of the cornea are damaged — determines whether vision is affected temporarily or permanently.
Epithelium
This is the thin, sensitive outermost layer of the cornea that is most vulnerable to injury. It keeps out foreign material and absorbs nutrients (such as oxygen) from tears.
How the epithelial layer is affected by injury:
- Corneal abrasions are shallow epithelial scratches that heal quickly.
- The epithelial layer heals rapidly, so minor abrasions typically heal in just 24 to 48 hours without lasting effects.
- This layer has many nerve endings — hundreds of times more than in the skin — so even a minor scrape can cause severe pain.
Bowman's membrane
This tough, protective film lies just beneath the epithelium. It is made of collagen. Together, this layer and the epithelium make up only about 10% of the cornea's thickness.
How Bowman's membrane is affected by injury:
- Deeper abrasions that penetrate through Bowman’s membrane are more likely to cause lasting vision damage.
Stroma
This is the central, thickest part of the cornea. It is mostly made of water and collagen. The stroma is crucial for maintaining the cornea's spherical shape, which is necessary for light to focus correctly. Pre-Descemet’s layer (or Dua’s layer) lies below the stroma and is sometimes considered a separate layer due to its distinct features.
How the stromal layer is affected by injury:
- Injuries that reach the stroma can cause opaque, whitish scar tissue to develop on the cornea.
Descemet's membrane
This thin layer, located deep within the cornea, protects the eye's internal structures from infection and trauma.
How Descemet's membrane is affected by injury:
- Descemet's membrane can repair itself fairly easily after injury.
- However, an injury at this depth can cause scarring.
Endothelium
This innermost layer of the cornea is a single sheet of cells. The endothelium plays a critical role in keeping the cornea clear by pumping excess fluid out of the stroma.
How the endothelial layer is affected by injury:
- These cells do not regenerate well, so damage can lead to ongoing vision issues.
How does the body protect the cornea?
The brain quickly responds to potential danger by triggering protective reflexes, such as:
- A blinking response so the eyelids and eyelashes can shield the cornea’s delicate tissue
- An upward rolling of the eyes to minimize the cornea’s exposure to impact
- Movement of the head and arms into a defensive position to block injury
Your reflexes and instinct to protect your cornea make sense when you consider its role in vision. The cornea:
- Allows light to pass freely to the retina, the light-sensitive layer at the back of the eye.
- Helps focus incoming light rays precisely on the retina for sharp, clear vision.
- Acts as a protective barrier, shielding the inner eye from germs, dust and debris.
- Filters out part of the sun’s harmful ultraviolet (UV) radiation.
What are the symptoms of a corneal abrasion?
Despite the body's protective mechanisms, corneal abrasions can still occur. A common symptom of a scratched cornea is the feeling of something stuck in the eye, like sand or dirt.
Additional symptoms include:
- Extreme eye pain
- Excessive tears
- Puffy eyes or eyelids
- Light sensitivity
- Redness
- Blurry vision
Be aware of warning signs that could indicate a serious problem such as an infection or deeper injury.
Signs of potential infection or complications include:
- Worsening symptoms – Increasing pain or redness
- Discharge – Yellow, green or bloody pus coming from the eye
- Corneal opacity – A white spot or cloudy area on the cornea
If the injury penetrates the cornea’s surface layers, it can cause permanent scarring and affect your vision. Injuries from fingernails and tree branches carry a small but serious risk of fungal infection.
Any recurring or worsening symptoms after initial healing should be checked right away. If you suspect something has pierced your eye or you see signs of serious internal injury, seek emergency care immediately.
What causes a corneal abrasion?
A corneal abrasion is a common eye injury. Knowing what causes corneal scratches can help you prevent them. Common causes include:
Foreign objects and debris
Dust, sand, dirt and other airborne particles can land on your cornea. More serious threats include metal fragments, wood shavings and debris from activities like gardening, grinding and welding. Sometimes, particles get trapped under your eyelid, scratching your cornea each time you blink.
Physical trauma
Accidental pokes and scrapes are common culprits. This includes scratching your eye with a fingernail, walking into a tree branch, and getting poked by paper edges and other sharp objects. Even makeup brushes and mascara applicators can scratch your cornea.
Contact lens issues
Wearing contacts increases your risk of corneal abrasions. Scratches can happen if you don't clean your lenses properly, wear them too long or if they don't fit correctly. A rough lens edge or debris trapped under a lens can also cause injury.
Chemical exposure
Chemicals such as soap, cleaning solutions and disinfectants can cause intense pain if they splash into your eye. In addition to the stinging and irritation, these substances can damage the cornea and surrounding tissues if not rinsed out quickly.
Vigorous eye rubbing
Rubbing your eyes too hard can scratch your cornea. This is especially true when trying to remove something irritating.
Who's at higher risk?
Some people have a greater risk of corneal scratches. Those with dry eye syndrome have less natural protection. People with trichiasis (eyelashes that grow inward) may experience chronic irritation. People who work in manufacturing and construction and those who participate in contact sports are also at higher risk.
How does an eye doctor diagnose a corneal abrasion?
An eye doctor will typically begin by asking about what you were doing when the injury occurred, along with your symptoms and medical history.
Your eye doctor will then use a slit lamp to carefully examine your eye. The slit lamp lets your eye doctor closely examine the front parts of your eye, including the cornea. If you're in severe pain, they might use numbing drops to make the exam easier to tolerate.
To see the abrasion, your eye doctor will apply a special dye called fluorescein to your eye’s surface. This yellow-orange dye comes in drops or on a small paper strip. It washes harmlessly over healthy tissue but sticks to damaged areas.
When your provider shines a cobalt blue light on your eye, the dye-covered scratch glows bright green. This helps them see the corneal abrasion.
Your eye doctor will then:
- Examine the pattern of the eye scratch revealed by the fluorescein stain (straight lines may mean physical trauma, while multiple small marks could suggest a contact lens injury).
- Check for any particles stuck in or under your eyelids.
- Check for complications like corneal swelling, haziness or blood.
- Test your visual acuity, as significant vision loss may indicate a more serious injury.
How long does it take to heal?
The amount of time it takes for a corneal abrasion to heal depends largely on the size and depth of the scratch, along with other factors.
Healing timeline for corneal abrasions
In general, uncomplicated superficial abrasions heal quickly because the cornea’s surface cells regenerate rapidly.
- Minor abrasions – Noticeable improvement often occurs within 24 to 48 hours.
- Mild abrasions – Typically heal within three days.
- Moderate abrasions – Usually show recovery within three to five days.
Note: For severe abrasions and injuries, seek medical care right away. For minor abrasions, if symptoms don't get better or if pain, redness or vision issues worsen, contact your eye doctor.
Factors that affect recovery time:
- Severity of damage – Smaller, superficial scratches heal fastest, while larger or deeper abrasions take longer.
- Size of the scratch – The extent of the scratch and where it's located on the cornea influence healing speed.
- Overall corneal health – A healthy cornea recovers more efficiently.
- Promptness of care – Getting medical treatment quickly supports faster healing.
Potential complications and long-term effects
When an injury pierces Bowman's membrane — the layer beneath the epithelium — it can lead to permanent scarring, which may affect vision. Deep scratches in the central part of the cornea are also more likely to cause vision problems. Untreated corneal injuries can result in infections, which can result in permanent vision loss.
A small number of people with a corneal abrasion may develop recurrent corneal erosion syndrome. This happens when the healed epithelial layer fails to attach properly to the underlying layers. It can cause severe pain upon waking. This condition can occur months or years after the injury.
How can you prevent eye scratches?
It's important to adopt simple habits to keep your eyes safe. This includes wearing proper eye protection whenever necessary. Always wear safety glasses, goggles or eye shields during risky tasks. Research shows that protective eyewear can cut eye injury risks by over 90%.
When to wear protective eyewear:
- At work – In construction, manufacturing, farming or jobs with flying debris or chemicals. The eyewear must fit well and cover the eyes completely, blocking dust and small particles.
- At home – When using power tools, sanders or grinders; cutting wood or metal; mowing the lawn; or trimming bushes.
- During sports – In basketball, soccer, baseball, racquetball, badminton or activities with fast objects or physical contact, use sports goggles with polycarbonate lenses.
- Around intense UV exposure – During welding, skiing and other activities with intense exposure to ultraviolet light.
Daily habits to protect your eyes
Simple habits and safeguards can help reduce the risk of corneal scratches. It’s important that you:
- Don't rub your eyes – Rubbing can worsen irritation and push debris deeper into the cornea.
- Rinse with clean water if something gets in your eye – This is the appropriate way to remove debris.
- Practice good contact lens hygiene – Wash your hands before handling your lenses. Clean and disinfect them as directed. Don’t wear them longer than recommended. Avoid forcing lenses in or out of your eyes. Use only prescribed contact lenses.
- Manage dry eyes – If your eyes are dry, consider using artificial tears or lubricating drops to keep your corneas moist and less likely to get injured.
- Take simple preventative steps – Trim your fingernails to avoid eye scratches. Be careful when playing with your pets. Cut low-hanging tree branches along walkways to remove eye-level hazards.
Frequently asked questions about corneal abrasions
Can a corneal abrasion heal on its own without treatment?
Mild scratches on the cornea can heal without treatment. Small abrasions typically clear up in one to two days. Uncomplicated superficial corneal injuries usually resolve within three to five days.
If your symptoms don't improve within 24 to 48 hours, it's important to see an eye doctor. They can:
- Confirm the injury is healing properly.
- Check for deeper injuries or debris trapped in or under your eyelids.
- Prescribe antibiotics to reduce the risk of sight-threatening infections.
What’s the difference between a corneal abrasion and a corneal ulcer?
A corneal abrasion is a scrape or scratch that affects the surface cells of the cornea. If it becomes infected, it can develop into a corneal ulcer. This is an intensely painful open sore on the cornea.
A corneal ulcer:
- Appears as a white or cloudy spot.
- Increases the risk for permanent vision loss.
- Requires same-day treatment.
What’s the difference between a corneal abrasion and a corneal erosion?
A corneal abrasion is an injury that occurs when something scratches the surface of the eye. This scratch usually heals fully as the surface cells of the cornea grow back.
A corneal erosion occurs when the outermost layer of corneal cells — the epithelium — fails to adhere properly to the tissue below. This condition causes significant pain and can make your vision appear blurred or cloudy. It can occur due to a previous corneal abrasion.
When to see an eye doctor
Remember get medical help immediately if you have:
- Had an object pierce your eye
- A chemical splashed in your eye
- Severe acute pain (or a sudden return of severe pain)
- Unusual discharge from your eye
- Significant vision loss, flashes or new floaters in your vision
- A white or cloudy spot develop on your eye’s surface
- Blood or pus visible inside your eye
- Developed a fever
Some corneal abrasions can lead to major infections, so it’s important to get prompt and proper care. If an injury is deep or doesn’t heal correctly, it can permanently affect a person’s vision.