Roth spots: Causes, diagnosis and treatment

What are Roth spots?
When blood vessels leak or discharge blood, this is called a hemorrhage. A Roth spot is a type of hemorrhage that occurs in the retina — the eye structure that absorbs light and allows us to see. Roth spots are identified by their white center and can be a sign of an underlying illness.
What causes Roth spots?
Roth spots were first observed by Swedish pathologist Moritz Roth in 1872. At the time, they were seen in patients with septicemia (blood poisoning). Studies by Moritz Litten in 1878 also observed that Roth spots were found in roughly 80% of patients with bacterial endocarditis. Endocarditis is a bacterial infection that occurs in the inner layer of the heart or heart valves.
This finding set the future precedent for the association of bacterial endocarditis with Roth spots. However, more recent research has shown that only 2% of people with bacterial endocarditis have Roth spots present on the retina. It’s still a common misconception that Roth spots are indicative of bacterial endocarditis.
Roth spots have also been linked to a number of diseases other than bacterial endocarditis. These include but aren’t limited to:
Leukemia: Cancer that typically forms in the white blood cells
Myeloma: Cancer that forms in plasma cells specifically
Anemia: Deficiency in healthy red blood cells
Anoxia: Complete loss of oxygen in the body or brain
Lymphoma: Cancer that forms in the lymphatic system
Connective tissue diseases: These include RA (rheumatoid arthritis) and lupus
Diabetes: A disease characterized by having too much glucose, or sugar, in the blood
Hypertension (high blood pressure): Excess force against the walls of blood vessels when blood circulates
Hypertensive retinopathy: Develops when high blood pressure leads to retinal damage
Diabetic retinopathy: Develops when uncontrolled blood sugar leads to retinal damage
HIV retinopathy: Develops when HIV (human immunodeficiency virus) causes retinal damage
Pre-eclampsia: High blood pressure during pregnancy
Vitamin B12 deficiency
Diseases like high blood pressure and diabetes can result in the growth of new, fragile blood vessels in the retina. This in turn raises the risk of a rupture or hemorrhage.
It’s also been noted that people who have a hereditary predisposition to leukemia or lymphoma run a higher risk of developing Roth spots.
READ MORE: 8 things your eyes can reveal about your health
What do Roth spots look like?
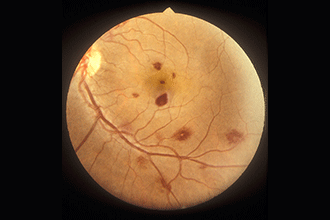
A Roth spot has a distinct appearance with a white spot in the center. It can indicate underlying disease such as diabetes, leukemia hypertension and endocarditis. [Image credit: "Roth spots and retinal haemorrhage" by International Centre for Eye Health is licensed under CC BY-NC 2.0]
Most retinal hemorrhages look like dark red splotches. However, Roth spots usually stand out from other types of retinal hemorrhages. They are identifiable by their characteristic appearance. Roth spots look like small, flame-shaped lesions with a white spot at the center.
These white spots at the center of the hemorrhage are composed of fibrin and form a fibrin-platelet plug at the center. This plug acts as a clot to restrict further blood loss from the damaged vessel.
How are Roth spots diagnosed?
Roth spots are most commonly detected during a comprehensive eye exam. This is because they occur on the retina, which is located on the back of the eye.
In order to identify the underlying disease, diagnostic tests such as a blood panel and a review of a person’s medical history and symptoms may be needed. Depending on your symptoms, you could be given an HIV antibody test or have your blood pressure, temperature and pulse recorded.
Your eye doctor will typically perform a fundoscopic exam to diagnose a Roth spot. This exam is a procedure that uses a bright light and magnification to get a clear view of the back portion of the eye. This will give them a good look at your retina, blood vessels and optic nerve to see if a hemorrhage is present.
A Roth spot is usually indicative of an underlying health issue. In general, symptoms you experience that accompany Roth spots are most likely caused by this condition rather than as a result of the retinal hemorrhage.
How are Roth spots treated?
Treatment for Roth spots typically focuses on addressing the underlying condition that causes it. This is because Roth spots are largely asymptomatic. Roth spots may cause vision-related issues when the macula is involved, but this is rare.
The main goal when it comes to Roth spot treatment is identifying the systemic illness that is causing it. Treatment of the primary disease can reduce any other ocular complications that may develop. In most cases, Roth spots resolve on their own, commonly over a period of six weeks.
When should I see a doctor?
There are many diseases that can impact the overall health of your eyes. This is why having routine eye exams every year or every other year is important. Roth spots can only be identified during a comprehensive eye exam.
Roth spots are generally not damaging and rarely cause any symptoms to develop. But identifying this issue and understanding your other symptoms could help to diagnose an underlying illness or disease. Roth spots may resolve on their own. The underlying condition that has caused them, however, will likely require management and treatment.
SEE RELATED: How often should you have an eye exam?
Roth spots. Eye Wiki. January 2022.
Roth spots. American Academy of Ophthalmology. August 2021.
Hemorrhage. Merriam-Webster. Accessed March 2022.
Moritz Roth. Life in the Fastlane. January 2022.
Bacterial endocarditis. Cedars Sinai. Accessed March 2022.
Roth spots. StatPearls. July 2021.
Roth spot. Kellogg Eye Center. Accessed March 2022.
Leukemia. National Cancer Institute. Accessed March 2022.
Myeloma. National Cancer Institute. Accessed March 2022.
Anemia. Cleveland Clinic. April 2020.
Cerebral hypoxia. Cleveland Clinic. May 2021.
Lymphoma. National Cancer Institute. Accessed February 2022.
Connective tissue diseases. Cleveland Clinic. December 2019.
What is diabetes? Centers for Disease Control and Prevention. December 2021.
High blood pressure. Centers for Disease Control and Prevention. May 2021.
Pre-eclampsia. Cleveland Clinic. October 2021.
Fevers, mild confusion and this retinal finding… Diagnosis? Stanford Medicine. March 2016.
How to determine treatment for a patient with a Roth spot. Optometry Times. November 2019.
Page published on Wednesday, April 13, 2022
Medically reviewed on Wednesday, February 23, 2022






