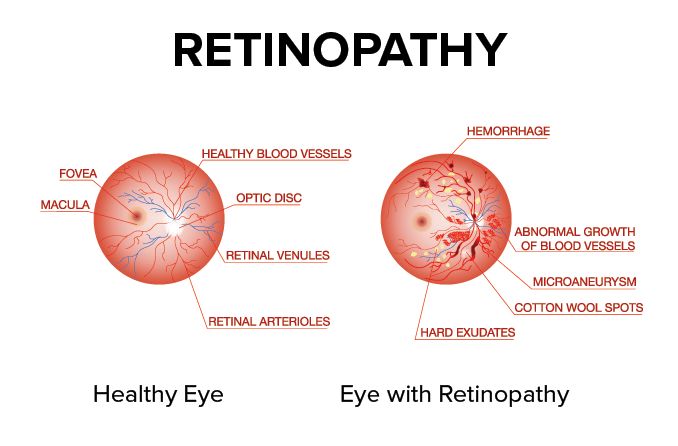
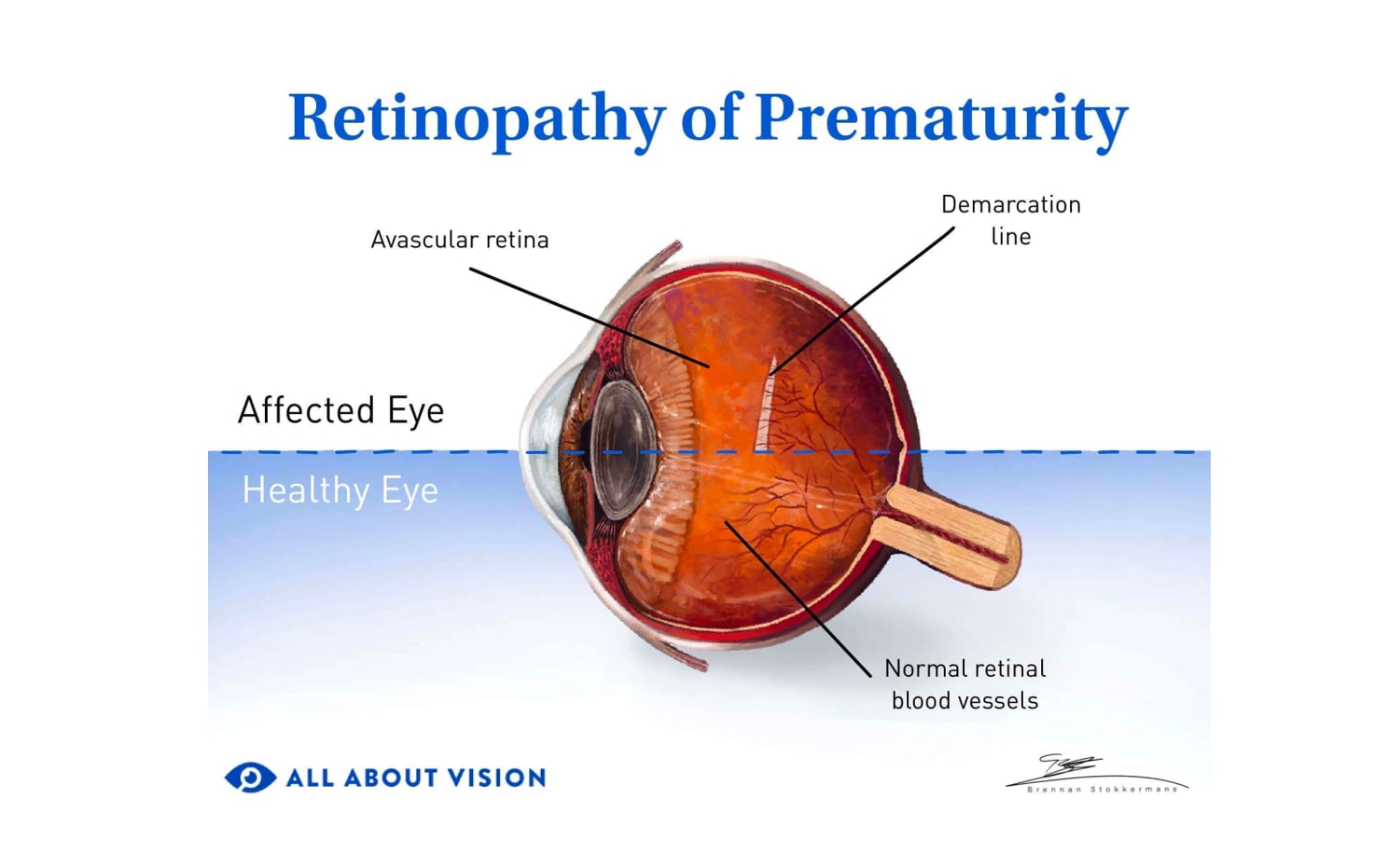
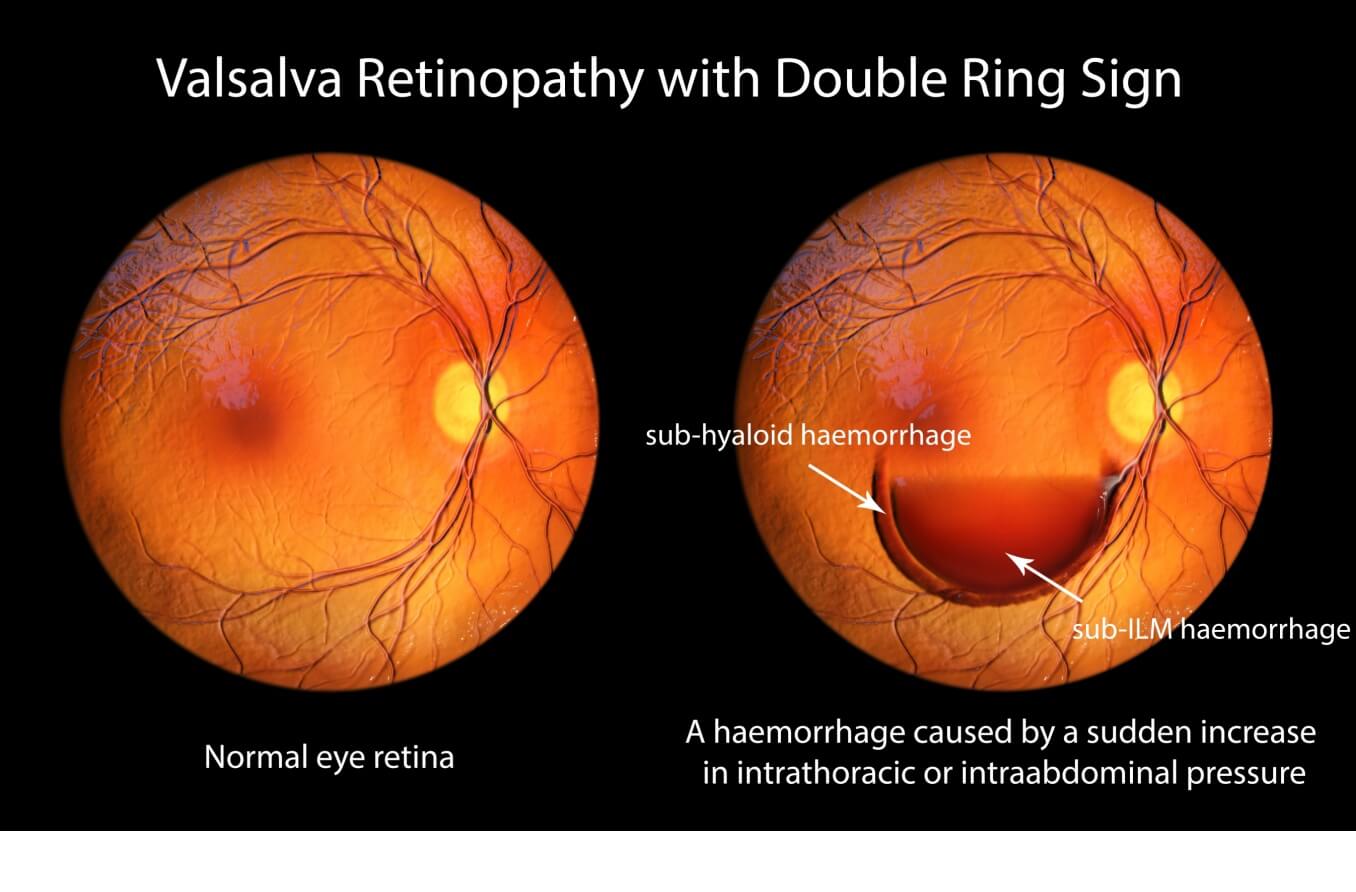
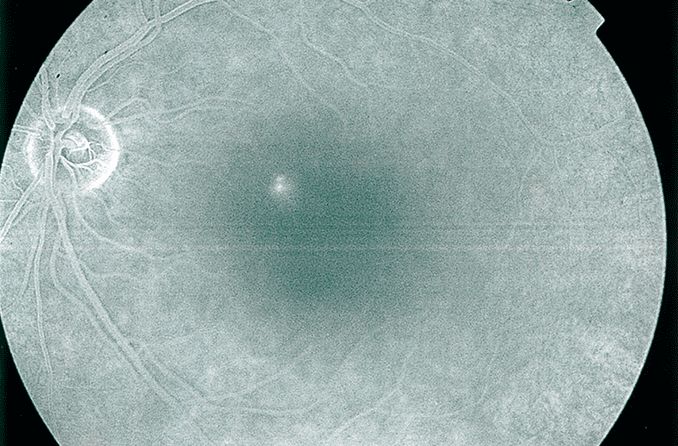
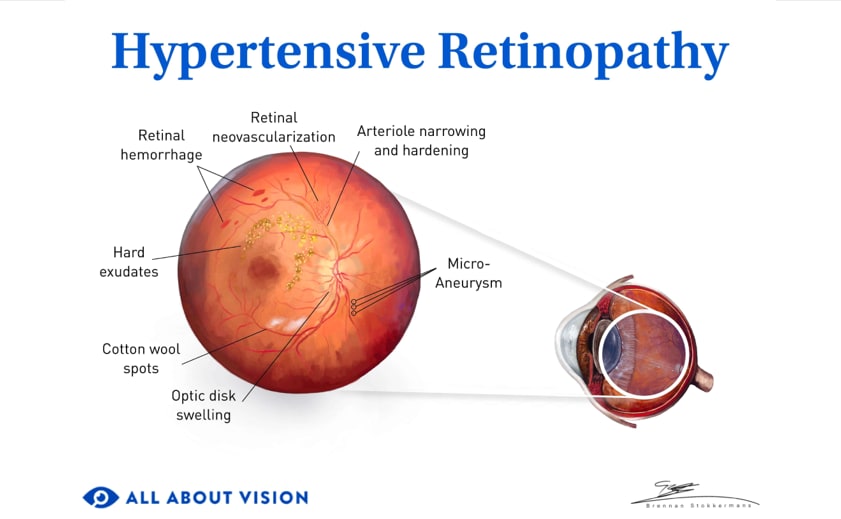
Retinopathy
Understanding the types of retinopathy can help protect your vision and maintain your eye health. Read about their causes, symptoms and treatments and how they are diagnosed.
Related Articles
All About Vision and AllAboutVision.com are registered trademarks of Essilor Laboratories of America, Inc © 2000-2026 Essilor Laboratories of America, Inc. The content on this site is for informational purposes only. All About Vision does not provide medical advice, diagnosis or treatment. Contact an eye doctor if you need medical attention.