What is a retinal hemorrhage?
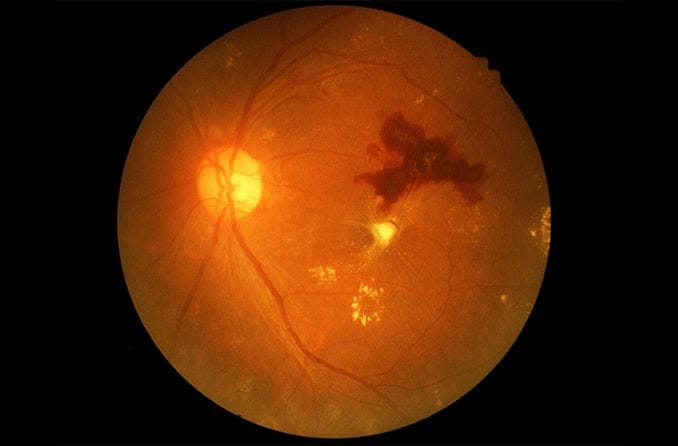
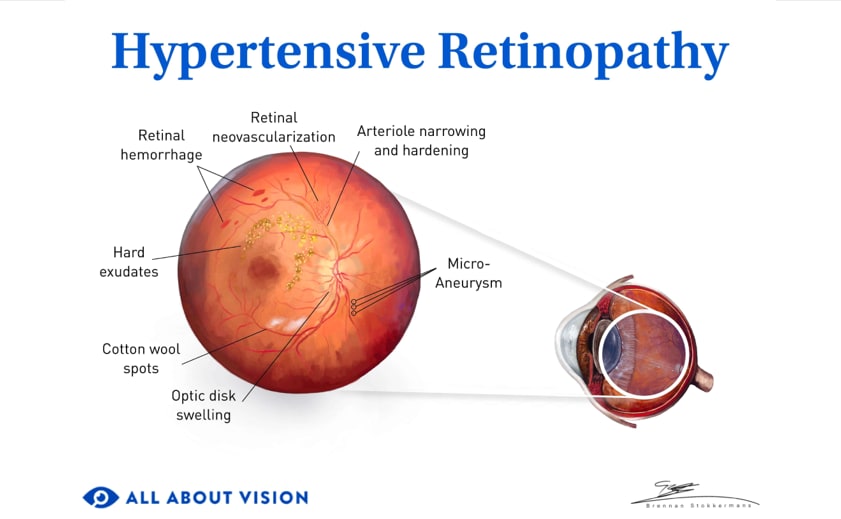
A retinal hemorrhage occurs when blood vessels in the retina begin to bleed. A hemorrhage, or bleeding, happens when these tiny blood vessels are damaged by injury or disease. Retinal hemorrhage can be caused by diabetes, high blood pressure, head injuries and even sudden changes in air pressure.
The retina is the sensory membrane that lines the inner back surface of the eyeball. It contains millions of light-sensitive cells called rods and cones and a dense network of small blood vessels. A hemorrhage, or bleeding, occurs when these tiny blood vessels are damaged by injury or disease.
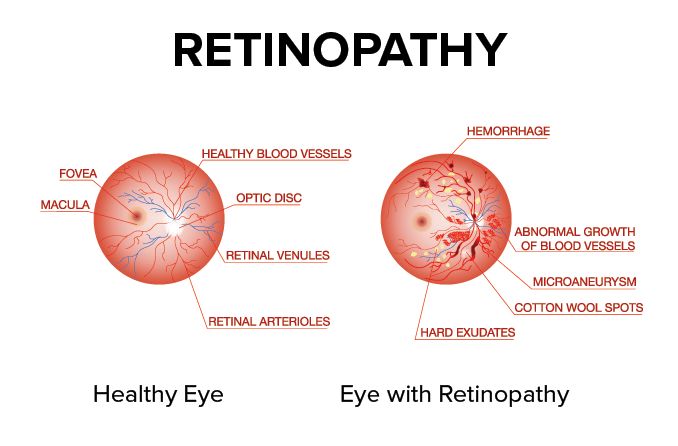
SEE RELATED: Retinopathy: Definition, causes and treatment
What can cause retinal hemorrhage?
Retinal hemorrhage can have many causes, including:
- Medical conditions, such as hypertension, diabetes, lupus, anemia, infections and leukemia.
- Eye diseases, such as macular degeneration, which is also known as age-related macular degeneration (AMD or ARMD). The macula is the small area at the center of the retina that is responsible for our sharpest vision.
- Head injuries caused by accidents.
- Shaken baby syndrome or other forms of child abuse.
- A sudden change in air pressure during activities such as mountain climbing or scuba diving. The change in air pressure may decrease the amount of oxygen available to the retina.
- Some medications, such as blood thinners.
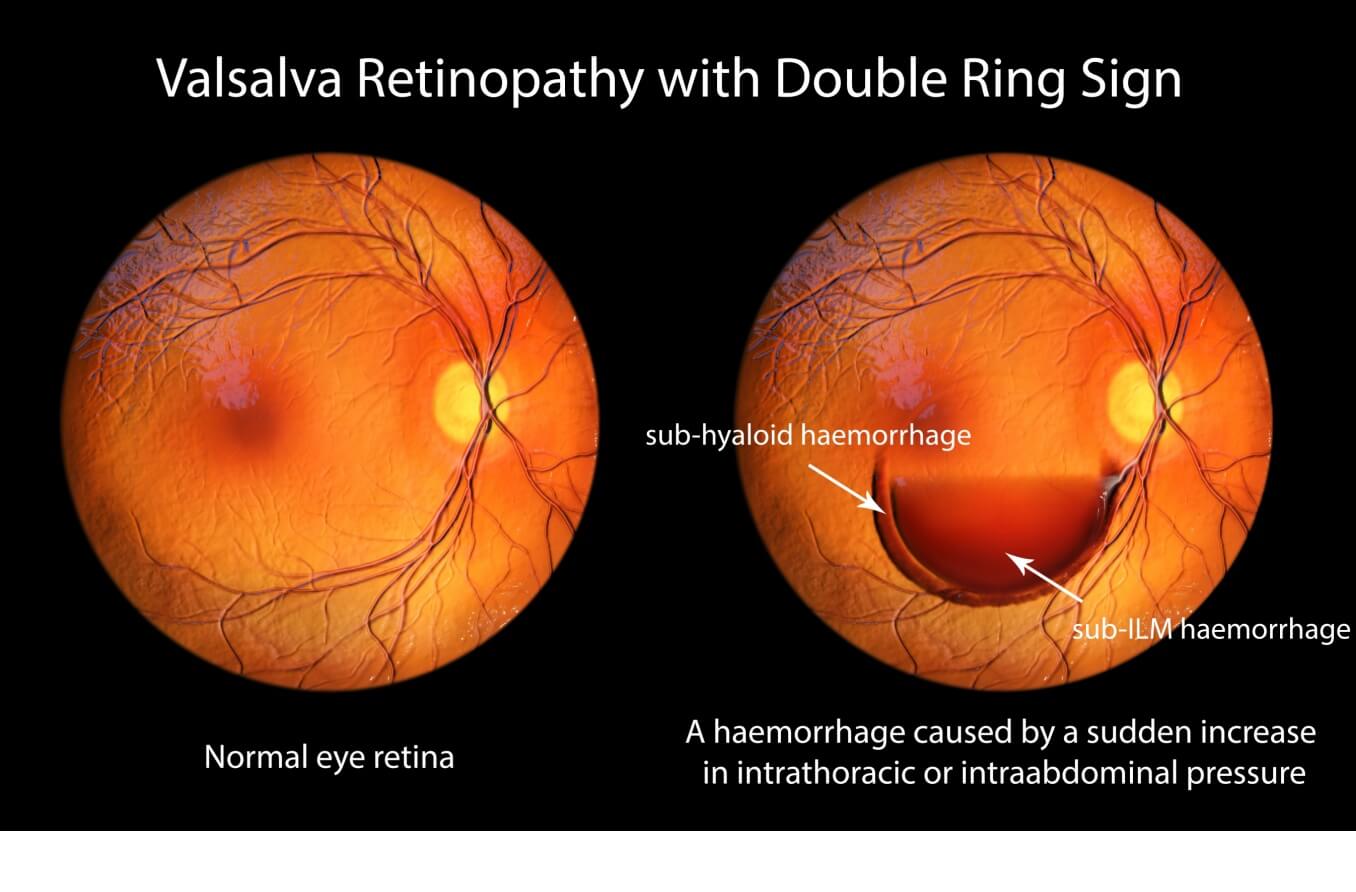
- On very rare occasions, straining due to constipation, severe coughing or vomiting.
Retinal hemorrhage symptoms
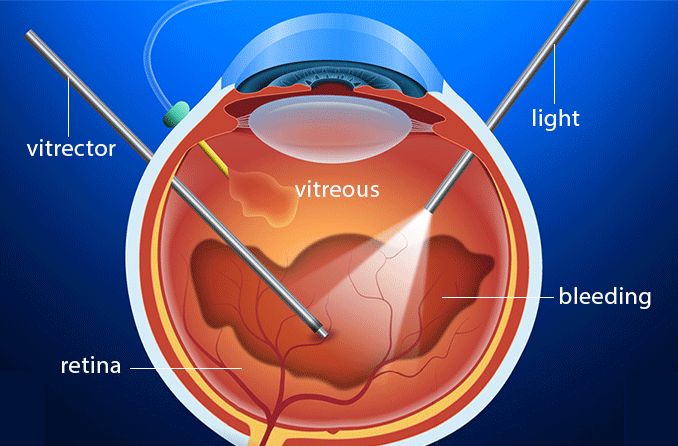
Because the retina is critical for vision, even small injuries and minor bleeding can lead to vision problems such as blurred vision, blind spots, or perceiving streaks and lines. Both eyes can be affected. If the blood leaks into the vitreous humor (the colorless, gel-like material located between the retina and the lens), it is known as vitreous hemorrhage.
Though a minor retinal bleed may have few or no symptoms, a significant retinal hemorrhage can have symptoms that include the following:
- Floaters in the field of vision.
- Seeing cobwebs, streaks or lines.
- A hazy or blurred quality to vision.
- Vision that has a red tint.
- Vision that is worse in the morning.
Types of retinal hemorrhage
The shape, location and severity of a retinal hemorrhage can offer clues to what type it is and the possible origin and cause. Here are the main types of retinal hemorrhages:
- Vitreous and preretinal hemorrhages – Blood diffuses through the vitreous membrane of the eye and may collect toward the bottom of the eye as it settles. Your eye doctor will see this on an exam. Causes can include high blood pressure, trauma or excessive blood vessel growth in the retina due to diseases like diabetes. Sometimes, there is no known cause.
- Flame-shaped hemorrhage – Retinal flame hemorrhages will show up on an eye exam as thin shapes, like feathers, flames or splinters. Researchers believe that flame-shaped hemorrhages are linked to artery-based diseases such as hypertension, blood disorders and certain anemias.
- Dot or blot hemorrhages – These hemorrhages are found in the deeper layers of the retina and form round, uniform hemorrhages. Conditions such as diabetes, rare disorders of the eye or veins, or sickle cell disease can cause this type.
- Roth spots – A Roth spot is a type of hemorrhage that occurs in the retina. It has a distinct appearance with a white spot in the center. It can indicate underlying disease such as diabetes, leukemia, hypertension and endocarditis.
- Other types of hemorrhages – Other kinds of hemorrhages can be associated with diabetes, hypertension, leukemia, radiation treatments and other illnesses.
SEE RELATED: Retinal vasculitis
Child abuse and shaken baby syndrome
When an infant or young child has a retinal hemorrhage, it can, unfortunately, be due to child abuse. Shaken baby syndrome and abusive head trauma, in particular, can cause a retinal hemorrhage.
In shaken baby syndrome, an infant is shaken violently by an adult and can be severely injured. The doctor may find severe, multilayered retinal hemorrhages, often along with head trauma. These factors are considered indicative of abuse.
How is retinal hemorrhage diagnosed?
Eye doctors are familiar with the different types of retinal hemorrhage. A dilated eye exam using an instrument called a slit lamp can reveal a retinal hemorrhage.
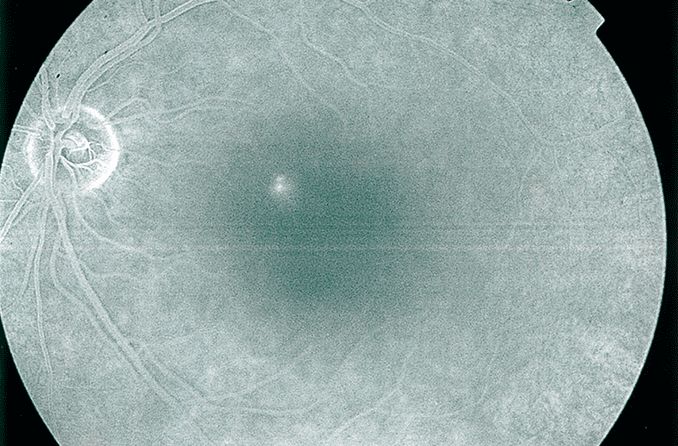
Your eye doctor can also use special tools to take a picture of the inside of your eye. Sometimes a dye will be injected into a vein in your hand or arm. The dye will flow into the blood vessels of your retina, allowing the doctor to take a very clear picture. An imaging technique called OCT also helps eye doctors better see the retinal hemorrhage.
Your eye doctor will take a thorough history, asking about trauma, injury, medication, flashes or floaters, and activities such as scuba diving or high altitude climbing. They will also ask about any illnesses or underlying conditions you have.
They may also want to have a specialist order blood tests or other diagnostic procedures to see if you have an underlying illness, such as diabetes, hypertension, infection or blood vessel disorders, that may have caused the retinal hemorrhage. Your eye doctor will want to work with your primary care doctor or your specialist to help guide treatment.
Retinal hemorrhage treatment
Treatment of retinal hemorrhage depends on the severity and the cause. In some cases, the hemorrhage is small and can be monitored while it heals on its own over a period of weeks or months. In other cases, underlying conditions will need to be treated to help the patient recover.
Importance of routine eye exams
It's essential to protect your retina so you can enjoy a lifetime of good eyesight. Many problems with the retina can be detected by your eye doctor before you notice symptoms.
Routine eye exams enable your eye doctor to examine your eyes for signs of retinal hemorrhage and other serious retina problems so treatment can begin as soon as possible.