What is diabetic eye disease?
Diabetic eye disease refers to a group of eye conditions that can result from diabetes mellitus, a chronic health condition. Diabetic eye problems range from blurry vision to more serious concerns. They may lead to vision loss or blindness without proper and timely care.
Understanding diabetes and its effect on the eyes is the first step in protecting your vision from potential impairment and blindness. Read on to learn more about diabetes, the eye problems it can cause and how to reduce your risk of experiencing these eye concerns.
How does diabetes develop?
Diabetes develops when the body does not produce enough insulin or does not respond properly to it (called insulin resistance). Insulin, a hormone produced by the pancreas, regulates glucose (sugar) levels in the blood. When the body cannot control the amount of sugar in your blood, glucose levels can become too high. This is another serious condition called hyperglycemia.
Hyperglycemia can affect many aspects of your health, including your nerves, kidneys, blood vessels and eyes, among others. This makes managing blood sugar levels and the condition of diabetes crucial to your general health and vision.
There are three primary types of diabetes:
- Type 1 – Type 1 diabetes is when a person’s pancreas does not produce insulin. It develops when a virus or other factors trigger an autoimmune response that attacks the pancreas. Injury, inflammation, or cancer of the pancreas can also lead to loss of insulin-producing cells.
- Type 2 – Type 2 diabetes is when too little insulin is produced or the body does not use it properly. The exact factors that cause insulin resistance to develop are unknown.
- Gestational diabetes – This type of diabetes may develop during pregnancy. It affects women who were not diabetic before becoming pregnant. Gestational diabetes generally resolves upon giving birth. However, it may increase a woman’s risk of developing Type 2 diabetes later in life.
Diabetes is a significant health concern around the world and in the United States. It affects around 422 million individuals globally and approximately 38 million Americans. It is the leading cause of blindness in American adults.
In the United States, nearly 98 million other adults have a condition known as prediabetes. This is when glucose in the blood is approaching the level of a Type 2 diabetes diagnosis.
Hyperglycemia and hypoglycemia
Hyperglycemia and hypoglycemia are blood sugar conditions that can be complications of diabetes.
Hyperglycemia occurs when there is too much sugar in the bloodstream. Diabetes is its most common cause. It arises when the body is unable to regulate blood sugar and its levels reach the following:
- Over 125 mg/DL when fasting
- Over 180 mg/DL two hours after eating
Hypoglycemia results when blood sugar levels are too low (below 70 mg/dL). In diabetics, hypoglycemia most often occurs when diabetes medications cause blood sugar levels to drop too low.
How does diabetes affect your vision?
Diabetes can affect your eyes and vision in various ways. High glucose levels may affect different parts of the eye, including the:
Blood vessels and retina
High blood sugar levels damage the small blood vessels that bring oxygen and nutrients to your retina (the light-sensing membrane in the back of your eye). These damaged vessels become leaky and can cause fluid and/or blood to seep out into the retina. The lack of circulation can cause new blood vessels to grow in and on top of the retina. These blood vessels can cause a retinal detachment or bleed into the vitreous cavity.
The retina contains the macula, which is crucial to your central vision. Your central vision involves your ability to see objects in sharp detail. When damage to the retina or retinal vessels occurs, permanent visual impairment may result — especially if the damage goes untreated.
Lens
Diabetes may also cause the eye’s lens to swell. The lens’s shape helps direct light that enters the eye onto the retina. When it swells, its size and shape changes. This may cause large changes in refractive error (the eye’s focus) and result in blurry vision.
Diabetes is also a significant risk factor for cataracts (clouding of the lens). This includes a type of fast-growing cataract called posterior subcapsular cataract (PSC).
Vitreous fluid
Diabetes can cause the blood vessels in the eye to leak blood and fluid. The leakage may seep into the vitreous (the clear, jelly-like fluid in the eye). Bleeding from blood vessels into the vitreous fluid is called a vitreous hemorrhage. If it is large enough, it can cause vision loss.
Diabetes may cause changes in the eye that increase the risk of serious eye concerns. These conditions can lead to vision loss and even blindness in some cases.
Blurry vision and diabetes
Blurry vision is a common symptom of eye problems in diabetics. Blurry vision from diabetes may be temporary or permanent, depending on the extent of damage that occurs and whether blood sugar is properly controlled. It may develop in the following ways:
- High blood sugar levels damage blood vessels in the retina, causing them to swell, leak or become blocked.
- Fluid buildup in the macula may lead to macular swelling and thickening.
- High blood sugar levels can cause the lens to swell, causing vision to become blurred.
Diabetic vision changes are often associated with blood sugar levels that are too high. However, studies show that rapid lowering of blood sugar levels may cause diabetic eye issues to worsen. Controlling blood sugar is key to preventing or managing eye problems with diabetes.
Speak with your eye doctor to learn more about the relationship between high or low blood sugar and blurry vision.
Can blurred vision from diabetes be corrected?
Blurred vision from diabetes may be resolved in some cases. Blood sugar may fluctuate at times, causing blurry vision. Once your blood sugar stabilizes, however, your blurred vision can improve and return to normal.
But when blurry vision results from retinal damage due to diabetic eye disease, some of it may be permanent. This makes it very important to get diabetic eye care and regular exams when you have diabetes.
LEARN MORE: Diabetes and blurred vision
Signs and symptoms of other diabetic eye problems
Signs of a condition are what an eye doctor might see when examining your eyes or performing eye tests. Symptoms of a condition are what you, as the patient, experience or feel. Diabetic eye issues can cause both signs and symptoms that affect your eyes and vision.
Signs
Diabetes can cause changes in the eye structures. These changes are signs of eye conditions and may be visible during eye exams or imaging procedures.
Signs of diabetes in the eyes may include:
Bulges in eye blood vessels (microaneurysms)
- Blood vessel leakage
- Blood in the retina (retinal hemorrhage)
- Swelling in the macula
- Fatty deposits (hard exudates) in or around the retina
- Cotton wool spots (soft exudates) in the retina
- Blood in the vitreous (vitreous hemorrhage)
- Blood vessel blockage
- Retinal scarring
- Vitreous traction or detachment
- New blood vessel formation (neovascularization)
- Clouding of the eye’s lens
- Increase in eye pressure
- Damage to the optic nerve

Symptoms
In the early stages of diabetic eye disease, you may experience no symptoms. When symptoms develop, however, they may include one or more of the following:
- Blurry, distorted or wavy vision
- Double vision (diplopia)
- Eye floaters (new or an increase in)
- Flashes of light (photopsia)
- A dark curtain or shadow in your vision
- Blank spots in your vision (scotoma)
- Eye pain
- Eye redness
- Changes in color vision
- Fluctuating vision
- Poor night vision
- Central vision loss
- Tunnel vision (peripheral vision loss)
Getting annual eye exams is important for identifying signs of diabetic eye problems as soon as possible. But if you notice diabetic eye disease symptoms or have any changes in your vision, contact your eye doctor promptly to have your eyes examined.
Types of diabetic eye problems
Diabetes may cause several types of issues in the eye. Four of the most common diabetic eye conditions are discussed below.
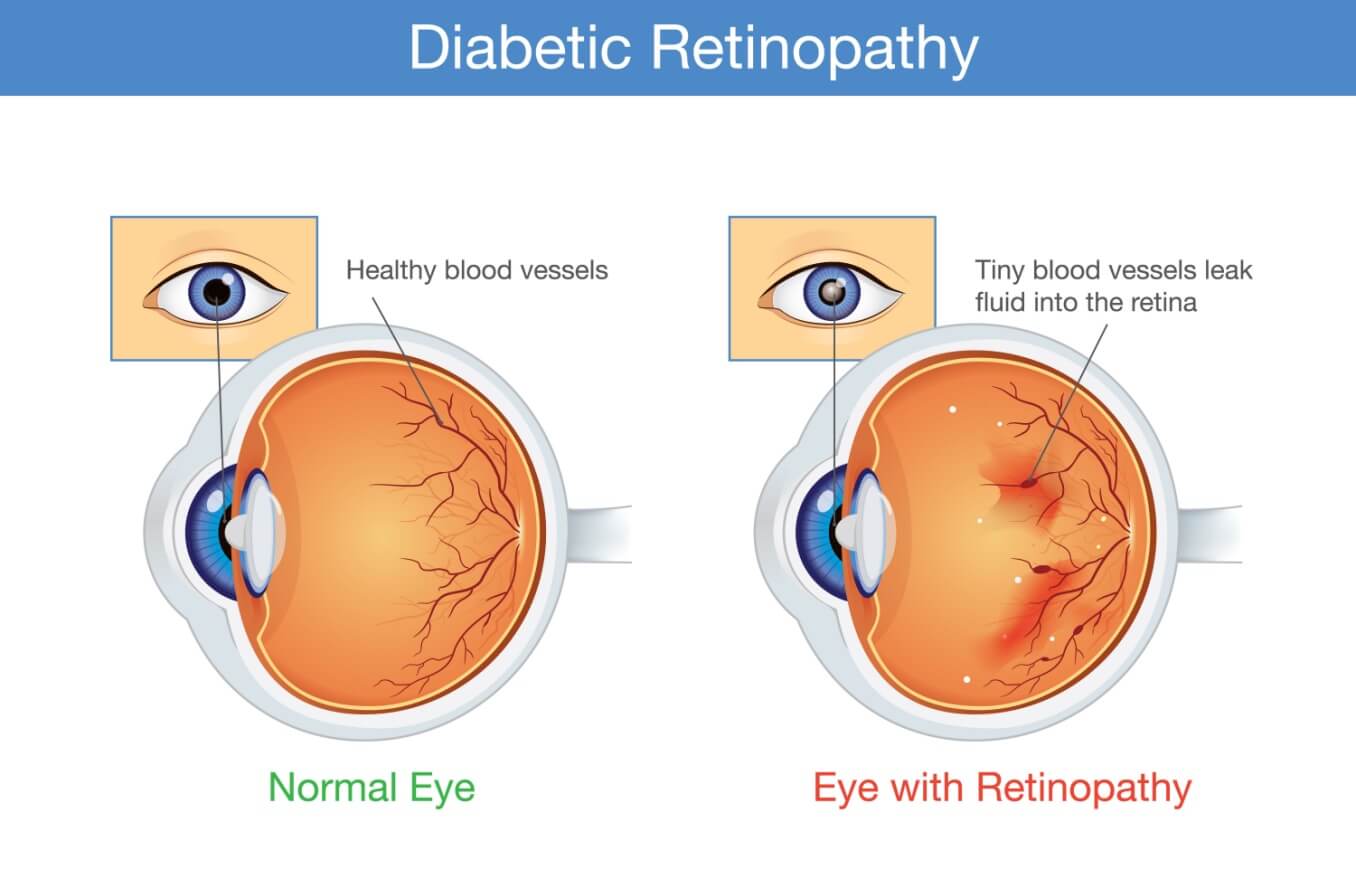
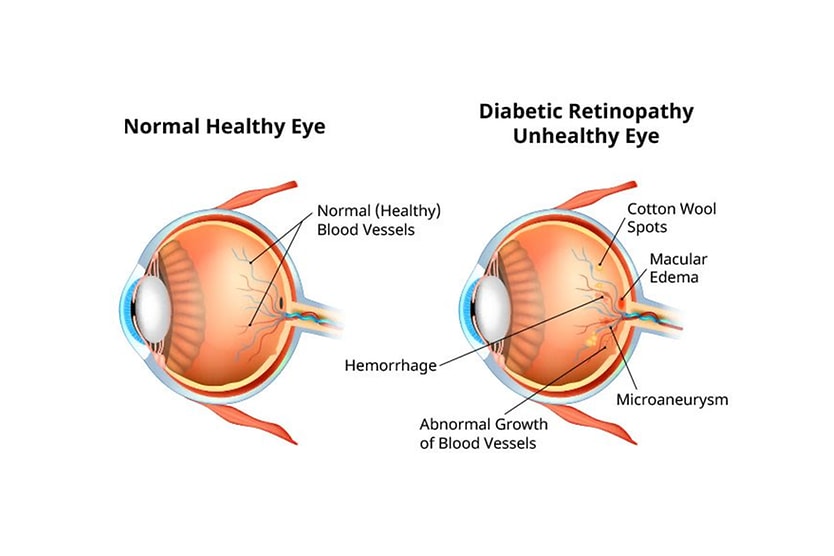
Diabetic retinopathy
Diabetic retinopathy (DR) is a diabetic eye disease that poses a significant threat to a person’s vision. DR is the most prevalent eye complication among diabetics. It occurs when high blood sugar levels cause changes in or damage to the blood vessels and nerve cells in the retina.
The vessels may swell, leak blood or fluid, or become blocked. When this occurs, the vessels are unable to provide the oxygen and nutrients the retina needs to function properly.
As the condition advances, new and abnormal blood vessels may develop in the retina. This is triggered by the release of a substance in the body called vascular endothelial growth factor (VEGF). The growth of these new vessels is the body’s way of trying to get blood to flow throughout the retina.
However, these new vessels are weaker and may also swell or leak. They can also cause scar tissue to form on the retina, leading to other retinal and vision problems.
Diabetic retinopathy is generally classified into two primary forms:
- Non-proliferative diabetic retinopathy (NPDR) – This is the early stage of the condition. It is characterized by the swelling, leakage or blockage of retinal blood vessels. NPDR may progress into three different stages. These are classified as mild, moderate or severe.
- Proliferative diabetic retinopathy (PDR) – PDR is the advanced stage and occurs when new, abnormal blood vessels develop in the retina.
Early on, DR may cause no vision changes or noticeable symptoms. But as the condition progresses, you may experience symptoms, such as:
- Blurry vision
- Double vision
- Eye floaters
- Flashing lights
- Dark areas in your vision
- Sudden vision loss in one eye
It may not be possible to prevent diabetic eye problems like DR. But managing your diabetes and having regular diabetic eye exams can help keep it from advancing and preserve your sight.
LEARN MORE: Diabetic retinopathy causes, symptoms and treatments

Among other problems, diabetes can damage blood vessels in the retina, causing them to leak blood into the posterior of the eye. Click image to enlarge.
Diabetic macular ischemia
Diabetic macular ischemia (DMI) is a later stage of diabetic retinopathy. It develops when the retina does not have adequate circulation to function normally. This occurs when blood vessels in the macula become occluded, break down or are obliterated. Depending on how far it has advanced, DMI can cause blurred vision and minor to significant vision loss.
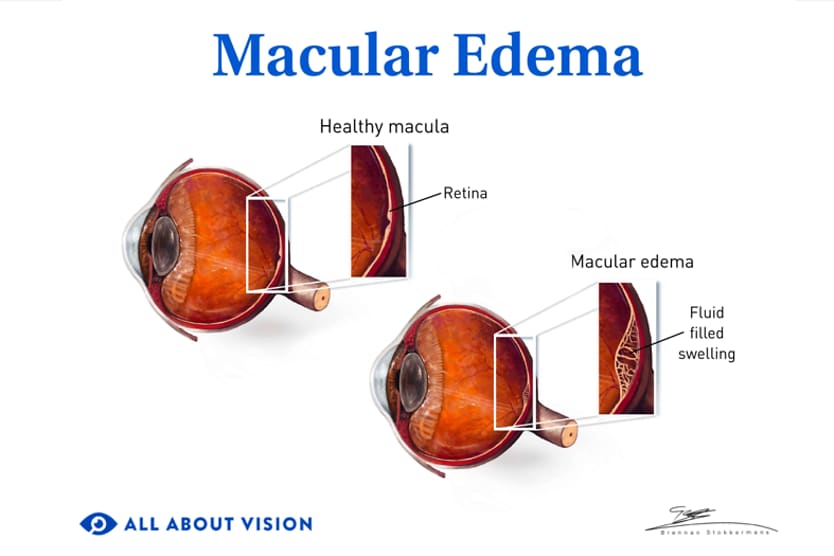
Diabetic macular edema
Diabetic macular edema (DME) is a condition that occurs as a result of diabetic retinopathy. It develops when fluid leakage from damaged blood vessels causes the macula to swell or thicken. This thickening impairs central vision, affecting your ability to see fine details, such as those needed for reading or driving.
Diabetic macular edema is more likely to occur during the advanced stage (PDR) of DR. However, it can occur at any stage.
Symptoms of DME include:
- Wavy or blurry vision
- Loss of visual acuity
- Changes in color vision
Doctors may use various systems to classify DME. The condition may be referred to as focal (limited to a focal area) or diffuse (more widespread). It may also be classified according to whether or not edema (swelling) involves the center of the macula.
Controlling your diabetes — and your risk factors for diabetes — can help reduce your risk of developing diabetic eye problems, such as DME. It is also important to have your eyes examined yearly and to see your eye doctor if you notice any DME symptoms or vision changes.

Click image to enlarge.
Cataracts and diabetes
A cataract is a condition that involves the clouding of the eye’s natural lens. The lens, which is normally clear, helps bend the light that enters your eye onto the retina. It also allows you to focus for near vision, such as when reading or seeing objects up close.
Those with diabetes are between two and five times more likely to develop cataracts than non-diabetics. They are also more likely to experience cataracts at a younger age.
When a cataract develops, you may have difficulty seeing things clearly, and your vision may be affected in other ways, as well. Other cataract symptoms may include:
- Blurry vision
- Dulled color vision
- Double vision
- Poor night vision
- Light sensitivity
- Glare sensitivity
- Seeing halos around lights
- Changes in refractive errors
High glucose levels associated with diabetes can increase the risk of developing cataracts.
The use of steroids, such as for the treatment of other diabetic eye problems, is also a risk factor for cataract formation.
It is believed that osmotic stress and oxidative stress may additionally contribute to cataract formation in diabetics.
Osmotic stress
Osmotic stress in the lens may occur in the following way:
The lens receives nutrients from the aqueous humor. When glucose levels rise in the aqueous humor, they also increase in the lens. This buildup of glucose causes the lens to swell, causing vision to appear blurry.
Glucose in the lens may be transformed into a sugar alcohol called sorbitol. When sorbitol levels increase in the lens, it causes a breakdown of the lens.
This osmotic stress (fluid imbalance) can lead to cataract formation.
Oxidative stress
The buildup of sorbitol in the lens may lead to the production of free radicals, which are harmful to the body. However, diabetes impairs the body’s ability to fight free radicals with antioxidants. This can lead to oxidative stress in the lens.
Oxidative stress can damage proteins and other structures in the lens, leading to cataract formation.
People with diabetes may have fewer protective enzymes in the body than usual, particularly when blood sugar levels are returned to a normal level rapidly. These enzymes normally help reduce the risk of oxidative damage in the lens. When the level of enzymes is insufficient, there is an increased risk of cataracts.
SEE RELATED: Types of cataracts

Click image to enlarge.
Glaucoma and diabetes
Glaucoma is an eye condition that can lead to blindness. It often develops when fluid in the front of the eye does not drain properly, causing the fluid to accumulate. This buildup increases pressure within the eye (intraocular pressure). High intraocular pressure can harm the optic nerve, which may impair vision and cause blindness.
In some cases, glaucoma may develop when pressure within the eye is in the normal range. This is called normal tension glaucoma (NTG).
While glaucoma is more common when you have diabetes, you can still get it even if you do not have diabetes. However, people with diabetes are twice as likely to develop glaucoma as non-diabetics.

Diabetes may increase the risk of developing certain types of glaucoma. These include:
Primary open-angle glaucoma
Primary open-angle glaucoma (POAG) results when the aqueous fluid in the front of the eye does not drain properly. Most of the fluid should drain naturally through the eye’s drainage angle to help maintain normal eye pressure. This “angle” is located around the outer edge of the iris, where it meets the cornea. With POAG, the drainage angle remains open, rather than narrowed or closed like with other glaucoma types.
People with Type 2 diabetes have an increased risk of developing primary open-angle glaucoma. This is believed to result from increased eye pressure due to high blood sugar levels. However, the cause in which this happens is not clear.
POAG usually does not cause symptoms, especially in the early stage. But when symptoms develop, they may include peripheral vision loss (tunnel vision).
Neovascular glaucoma
High blood sugar levels may damage the blood vessels in the retina and cause new, abnormal vessels to develop on the retina and iris. This is a severe form of diabetic retinopathy.
These new vessels (called neovascular) on the iris can then start growing into the drainage angle in the eye, limiting fluid drainage. This causes pressure to rise within the eye and can lead to open-angle neovascular glaucoma. Blood vessel growth over the angle may also cause a scar to form, narrowing or totally blocking the angle. This is a type of angle-closure glaucoma.
Early neovascular glaucoma may not carry any symptoms. As the condition progresses, symptoms may involve:
- Halos around lights
- Vision loss
- Eye pain or pain in the brow area
- Eye redness
People with DR have a higher risk of developing neovascular glaucoma.

Click image to enlarge.
Steroid-induced glaucoma
Diabetic macular edema may be treated with steroids in some cases. However, the use of steroid medications may lead to increased intraocular pressure, causing steroid-induced glaucoma.
Some people may experience no symptoms of steroid-induced glaucoma. Others may have symptoms that include:
- Blurry vision
- Changes in vision
- Eye pain or pain in the brow area
SEE RELATED: Glaucoma: Types, causes, symptoms and treatment
Other potential diabetic eye problems
Diabetes is commonly associated with DR, DME, cataracts and glaucoma. But it may also increase the risk of developing other eye conditions. These include:
Dry eye and diabetes
Dry eyes result when there is a disruption in the tear film layer. This may happen when the tears evaporate too quickly or when not enough tears are produced to keep the eyes lubricated. While people with diabetes often experience dry eye, the reasons for this are not well understood.
However, some eye doctors and researchers believe it may be due to the following factors:
- High blood sugar – When blood sugar in the body becomes too high, nerves within the eyes may become damaged. This includes the nerves in the lacrimal gland and cornea. If these nerves are damaged, it can diminish the quality and amount of tears produced.
- Low insulin – Low insulin levels in the body can prevent the lacrimal gland in the eye from producing adequate tears.
- Inflammation – Elevated blood sugar can cause an inflammatory response in the body. This can impact the lacrimal gland and interfere with its ability to work properly. It can also hinder oil flow from the eyelid glands, which is necessary for preventing tear evaporation.
Common dry eye symptoms include:
- Blurry vision
- Eye redness or irritation
- Burning or stinging in the eyes
- A gritty or scratchy sensation in the eyes
- Mucus buildup around the eyes
- Excessive tear production
Retinal vein occlusion and diabetes
When the veins that transport blood away from the retina become fully or partially blocked, a condition known as retinal vein occlusion (RVO) occurs. Increased glucose levels in the eye may cause vascular changes, including the narrowing or blockage of blood vessels. This can lead to RVO.
There are two types of RVO, both of which are associated with diabetes:
- Branch retinal vein occlusion (BRVO) – Blockage of one or more branches of the retinal vein
- Central retinal vein occlusion (CRVO) – Blockage of the central (main) retinal vein
Symptoms of RVO may include:
- Blurry vision
- Eye floaters
- Vision loss (sudden or gradual)
- Eye pain
- Eye pressure
Idiopathic juxtafoveal telangiectasia and diabetes
Diabetes is also associated with idiopathic juxtafoveal telangiectasia. Commonly called macular telangiectasia type 2 (MacTel), this condition results from small, abnormal blood vessels in the fovea.
Found in the center of the macula, the fovea allows for our sharpest central vision. Its blood vessels may dilate and leak, causing the macula to swell. This can damage the retina and impact vision. In severe cases, MacTel can lead to macular holes and subretinal neovascularization.
There are three primary types of macular telangiectasia:
- Type 1 – This type generally affects one eye and is congenital (present at birth). It is rare (compared to Type 2) and may potentially be associated with Coats disease.
- Type 2 – This form often affects both eyes and is acquired (develops at some point in life). Type 2 is the most common of all variations and is the one most closely associated with diabetes.
- Type 3 – This is the rarest and most severe form, and it generally affects both eyes.
MacTel may cause no symptoms early on. As it progresses, however, symptoms may include:
- Distorted or blurred vision
- Difficulty seeing in low light
- Central vision loss
Diabetic nerve palsies
Diabetic nerve palsies are a rare type of diabetic neuropathy. They are due to microvascular damage to cranial nerves rather than damage within the eye. This damage typically affects the eyes’ motor nerves, so the eyes cannot move the way they need to (ophthalmoplegia).
Symptoms of diabetic nerve palsies can include:
- Strabismus (misaligned or crossed eyes)
- Diplopia (double vision)
- Ptosis (drooping eyelid)
- Pupil dilation (enlargement)
- Headache or pain around the eyes
Diabetic nerve palsies usually happen suddenly and only affect one eye. They tend to heal on their own within a few months.
Diabetes and blindness
High blood sugar levels can cause changes in the eye that lead to diabetic eye problems, such as those discussed above. These changes can cause vision loss and blindness in some cases. Controlling your blood sugar and managing your diabetes is essential for protecting your eyes from damage. Speak with your eye doctor to learn more about the relationship between diabetes, vision loss and blindness.
Diagnosis, management and treatment
The potential damage diabetes can cause makes the early diagnosis, management and treatment of diabetic eye disease essential. You may be referred to a retina specialist for diabetic eye problems.
Diagnosing diabetic eye conditions
Diagnosing diabetic eye disease begins with a comprehensive eye exam. Your eye doctor may also review your medical history, including information about your diabetes. They may ask how the condition is controlled (such as through insulin or oral medication) and inquire about diabetes testing, such as your last A1C blood test. (Used to screen for or monitor diabetes, the A1C test provides details about your blood sugar levels over the previous two to three months.)
Several ocular tests may be performed to diagnose diabetic eye problems. These may include:
- Visual acuity test – Your doctor may use this standard test to evaluate the clarity of your vision at specific distances.
- Tonometry – Tonometry may be used to measure intraocular pressure (or pressure within your eye).
- Visual field test – A visual field test may be used to determine if your peripheral (side) vision has been affected and to what degree. It can also help determine if blind spots (scotomas) are affecting your vision.
- Amsler grid test – This test involves a chart that looks like graph paper. It is used to evaluate for symptoms, such as wavy or distorted vision, which may indicate issues with your central vision.
- Dilated eye exam – Your doctor will use special eye drops to dilate (widen) your pupils. This allows them to gain a better view of your retina and other eye structures to check for concerns.
- Slit-lamp exam – During a slit-lamp exam, your doctor will use a magnifying microscope with a focal light to examine various structures within your eye.
- Ophthalmoscopy – Your doctor may use this technique to examine different parts of your eye, including the retina and optic nerve. It may also be used to help determine how far diabetic eye issues may have progressed.
- Gonioscopy – Your doctor may perform a gonioscopy to check for glaucoma. This technique involves a special lens used to evaluate the drainage angle in the eye.
- Pachymetry – This test involves an instrument used to measure the thickness of the cornea. It may be used to help screen for glaucoma.
- Optical coherence tomography (OCT) – OCT is an imaging technique that uses light waves to take cross-sectional pictures of your retina. These images allow your doctor to examine the retinal layers and optic nerve to check for damage or other concerns.
- Fluorescein angiography – For this test, a special dye (called fluorescein) will be given through a vein. The dye will move through your bloodstream to the vessels in your retina. Your doctor will take pictures of your eye while the dye circulates throughout your retinal vessels. They will then review the pictures to identify any areas of fluid buildup, blockage or vessel leakage.
Artificial intelligence and teleophthalmology are being used in some instances to screen for certain diabetic eye problems. Teleophthalmology involves eye care provided via digital methods. These screening tools allow doctors to identify early signs of eye disease in a remote capacity. This earlier detection can result in timelier diagnosis and treatment, which may further reduce the risk of vision loss from diabetes.
Other exams and imaging techniques may be used to further screen for or diagnose diabetic eye disease.
Treatment for diabetic eye disease
Your eye doctor will recommend treatment for diabetic eye problems according to the type of eye condition that has developed. In some instances, the condition may not require treatment and might just be monitored.
Diabetic eye disease treatment may include the following:
Diabetic retinopathy
One or more of the following options may be used to treat DR:
- Anti-VEGF drugs – These medications are given via injection into the eye. Several anti-VEGF drugs are available for treating DR.
- Laser photocoagulation – Laser surgery may be used to target leaky blood vessels and decrease the formation of abnormal vessels. The two main laser treatments for DR are focal/grid laser photocoagulation and scatter (pan-retinal) photocoagulation.
- Vitrectomy – This surgery removes the vitreous from within the eye. It may be performed when the retina has detached, scarring has developed or blood has leaked into the vitreous fluid.
Diabetic macular edema
When treatment for DME is needed, it may involve one or more of the following:
- Anti-VEGF drugs – The first treatment option recommended for DME is usually anti-VEGF eye injections. There are several anti-VEGF medications that may be used.
- Corticosteroids – These medications may be given in the form of an eye injection or an implant surgically placed within the eye.
- Laser surgery – Laser options may be used to target abnormal blood vessels in the retina and treat the damage they cause.
- Vitrectomy – Vitrectomy may be performed to treat DME when scar tissue pulls on the retina or when anti-VEGF drugs are ineffective.
A combination of DME treatments might be given in some cases.
Cataracts
Cataracts may be treated with traditional or laser cataract surgery. During surgery, the clouded lens is removed from the eye and replaced with a clear, artificial intraocular lens (IOL).
Glaucoma
Medication may be used to treat glaucoma and decrease eye pressure. This commonly includes eye drops. Some of these eye drops decrease the amount of fluid produced in the eye, while others help fluid drain from the eye. Although less common, oral medications may be used to treat glaucoma.
Glaucoma surgery may be performed to decrease eye pressure, manage the condition and help preserve your sight. The surgery used will depend on the type of glaucoma present and other factors. Glaucoma surgeries may be conventional (incisional) or laser-based.
READ MORE: Glaucoma treatments
Dry eye
Treatment for dry eye disease may involve palliative care or lifestyle changes, such as using warm compresses or avoiding dry environments.
In other cases, dry eye treatments may include:
- Eye drops – Eye drops may provide relief from dry eye. These can include artificial tears or anti-inflammatory medicated drops.
- Punctal plugs – When dry eye disease is more advanced, plugs might be placed in the tear ducts. These plugs help your eyes stay lubricated by preventing the drainage of tears. The plugs may remain in place temporarily or for a longer period of time.
- Surgery – In some cases, surgery may be performed to block the tear ducts permanently.
- Eyelid therapy – Eyelid therapies, such as intense pulsed light (IPL), thermal pulsation techniques and low-level light therapy (LLLT), may help treat dry eye disease due to meibomian gland dysfunction. They can use red light and heat-based therapy to potentially reduce inflammation in the eye, improve gland function and address other factors. This can help improve overall tear production.
Retinal vein occlusion
Treatment for RVO generally involves addressing the effects of the condition, as retinal vein blockage cannot be reversed. Anti-VEGF injections and steroid injections or implants may be used to treat macular swelling caused by vessel blockage or new blood vessel growth. Laser photocoagulation may be used in some cases, such as to treat macular swelling that occurs with BRVO.
Idiopathic juxtafoveal telangiectasia
Many cases of MacTel may not require treatment. However, in some instances, the effects of the condition may be treated with a recently FDA-approved one-time implantable therapy called revakinagene taroretcel. It's a tiny capsule, about the size of a grain of rice, that an eye doctor places inside the eye. The capsule contains living cells that have been specially designed to continuously produce a protein called recombinant human ciliary neurotrophic factor (rhCNTF), which is released directly into the retina. CNTF helps protect the cells in the retina that allow you to see, possibly slowing the loss of vision caused by MacTel.
Management of diabetes and eyesight problems
Managing diabetes and vision issues involves maintaining control of blood sugar, blood pressure and cholesterol levels. It also involves getting your eyes examined annually or more frequently if your doctor recommends it.
Eating a healthy diet and getting regular exercise as recommended by your primary physician can help keep your diabetes in check. This can ultimately have a positive effect on your vision.
Preventing diabetic eye disease
Diabetes does increase your chances of developing diabetic vision issues. But you may be able to reduce your risk or prevent these issues from progressing. The following may help protect your vision from diabetic eye problems:
- Control your blood sugar – Keeping your blood glucose levels in the range recommended by your doctor helps manage your diabetes. Stable blood sugar levels lower your chance of experiencing diabetic eye disorders.
- Take medications as prescribed – If you have diabetes, your physician may prescribe oral medication or insulin use. Taking medications as prescribed can help protect your eyes from diabetic eye problems.
- Monitor your A1C – The A1C test can help you manage your blood sugar levels and diabetes. Your medical doctor can help you determine what your goal A1C percentage should be. This is usually 7% or lower for most diabetics. Knowing your A1C so you can tell your eye doctor is also important. They may ask for it to assess your risk for developing diabetic eye disease.
- Control your cholesterol and blood pressure – High blood pressure and cholesterol levels increase your risk of diabetic eye issues. Talk with your doctor to learn how to keep these factors well-managed.
- Avoid smoking – Quitting or avoiding tobacco use is good for your eye health and general wellness. It also reduces your chances of experiencing blood vessel damage in your eyes, which may lead to diabetic eye disease.
- Protect your eyes from the sun – Wearing sunglasses with 100% ultraviolet (UV) protection reduces your risk of vision problems, including diabetic eye issues.
- Eat a nutritious diet – When you have diabetes, your doctor may recommend you follow a certain diet to help control your blood sugar. What you eat may play a role in protecting your eyes and vision against sight-threatening diabetic eye disease.
- Get plenty of exercise – Staying active and exercising regularly can help keep your blood sugar levels under control. It may also lower your risk of diabetic eye problems.
- Schedule annual eye exams – Getting yearly eye exams is an important part of comprehensive diabetic eye care. This also allows your eye doctor to find problems earlier, which can help preserve your eye health and vision.
- Get eye exams during pregnancy – If you are pregnant and have diabetes, you may need to have your eyes examined more frequently. This includes throughout the three trimesters and for a year following the birth.
When to call an eye doctor
Diabetes and eye problems are often connected. It is very important to undergo regular comprehensive eye exams so that any problems can be found as early as possible.
If you have any changes in your vision, even if it is within a year of your last exam, visit an eye doctor right away. Diabetes can affect your eyes before you are even aware you have the condition. In fact, many people first learn of their diabetes during a routine eye exam.
It is also important to schedule an eye exam if you have been diagnosed with diabetes since your last eye care visit.
Early diagnosis, treatment (if recommended) and routine eye exams are key components of diabetic eye care. Your eye doctor can test for diabetic eye problems and determine if treatment is necessary. They can also discuss tips for prevention and answer questions about diabetes and vision changes, such as:
- How does diabetes affect the eyes?
- Is my blurry vision from diabetes?
- What does diabetes-related blurred vision look like?
- Can diabetes cause blindness?
- How can you protect your vision and prevent blindness from diabetes?
If you notice any changes to your vision, however minor or significant, contact your eye doctor immediately. Prompt care can help you preserve your sight and maintain your quality of life. Visit your eye doctor to learn more about the relationship between diabetes and your eyes.
READ NEXT: How heart disease affects eye health