What is optical coherence tomography?
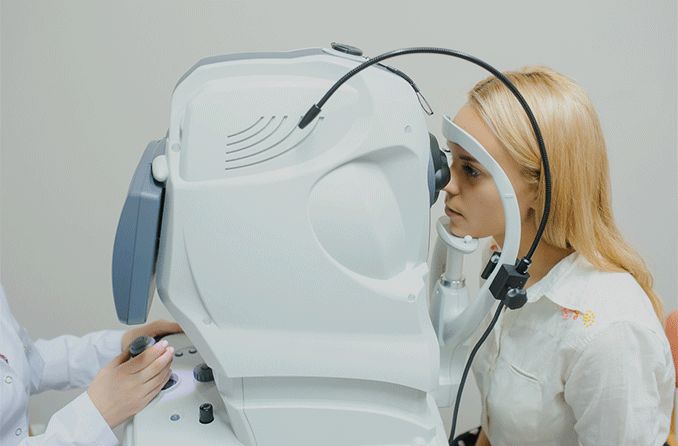
Optical coherence tomography (OCT) is a painless, non-invasive imaging method (similar to an ultrasound) used to observe and gather detailed images of the retina. This imaging is important for detecting and monitoring changes in the retina and optic nerve.
OCT can help detect a number of retinal diseases, such as glaucoma, diabetic retinopathy, Alport syndrome and age-related macular degeneration (AMD). Additionally, OCT can be used to monitor some neurological conditions such as multiple sclerosis (MS).
OCT is an important component in both diagnosing and determining the best treatment for these among other conditions.
What is optical coherence tomography used for?
OCT is used for diagnosing and monitoring retina and optic nerve conditions, as well as some neurological conditions. The exam helps ophthalmologists get a clear view of each layer of the retina and measure its overall thickness.
Apart from detecting and observing certain eye conditions, OCT plays an important role in helping eye doctors decide on treatment plans for patients at any stage of the particular condition that is present.
SEE RELATED: What part of the brain controls vision?
What conditions can be detected with OCT?
Several eye conditions can be diagnosed using OCT, including:
- Glaucoma
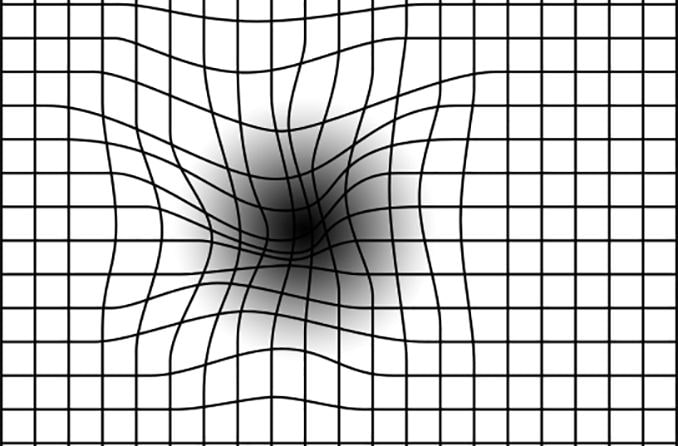
- Age-related macular degeneration (AMD)
- Diabetic retinopathy
- Central serous retinopathy
- Macular hole
- Macular edema
- Macular pucker
- Vitreous traction
- Optic nerve disorders
Not only can OCT help diagnose eye conditions, it can also monitor certain problems that are already present. Glaucoma is one such condition that can be monitored with OCT, as the exam helps ophthalmologists detect changes that occur in the optic nerve fibers.
Although OCT can be used for many different eye conditions, it is not useful for those that affect the way light passes through the eye, such as cataracts. This is because OCT technology depends upon light waves for proper exam readings and results.
OCT and multiple sclerosis
In addition to ocular conditions, OCT is now being considered as a way to monitor neurological conditions — particularly multiple sclerosis (MS). MS is an autoimmune disease that affects the central nervous system, which includes the optic nerves.
The protective covering of nerves is called myelin, and it works to surround and insulate nerves (also known as axons). In patients with MS, the myelin can become damaged due to inflammation in parts of the central nervous system.
Myelin does not protect retinal nerve fibers, and research has shown that these fibers actually thin out in patients with MS. Because of this lack of protection, clinicians are able to get a better look at isolated axons during OCT exams (and evaluate the retinal nerve fibers at the same time).
Although MS is usually monitored with magnetic resonance imaging (MRI), clinicians have found that OCT technology can provide additional imaging of the retinal nerves in MS patients and provide a greater assessment of the disease.
What to expect during an OCT exam
Before beginning the exam, your ophthalmologist may give you eye drops to dilate your pupils. This will make it easier for them to examine your retina during the process.
You will be seated in front of the OCT machine, where you will be able to rest your chin to ensure there is no movement that interferes with the exam. Your eyes are then scanned (without being touched) and imaging is completed within 5 or 10 minutes.
If your pupils were dilated for the exam, your eye doctor will give you special sunglasses to protect your eyes from sunlight and lessen any light sensitivity you may experience.
OCT angiography
Optical coherence tomography angiography (OCTA) is a relatively new imaging technique that provides more advanced photos of the retina. OCTA is derived from OCT technology. An OCTA scan provides just as much information as OCT, but with more advanced, three-dimensional images.
The imaging is particularly useful in detecting and treating inflammatory conditions such as uveitis because of the technology. The three-dimensional capabilities provide ophthalmologists with highly in-depth information about a condition, which can help design more targeted treatment.
OCTA also provides detailed images of the blood flow within both the retina and the choroid (the layer of tissue between the sclera [white of the eye] and retina).
Although OCTA provides great detail for eye doctors (and their patients), there are still some limitations due to its newness. Drawbacks can include its restricted field of view, inability to view leaky blood vessels and the need for repeat imaging. The instrument’s scanning speed is also slow.
Eye doctors may continue to recommend traditional imaging as a result of these limitations.
Ensure eye health with regular eye exams
Not everyone needs specialized exams like OCT and OCTA, but it is important for everyone to keep up with routine comprehensive eye exams. This is the best way to ensure your eyes are healthy and learn if any changes (whether mild or significant) have occurred with your overall eye and vision health.
Always talk to your eye doctor if you have concerns about your vision, even if you are not due for your annual eye exam, as even minor problems can be a sign of an underlying condition.
SEE RELATED: Eye exams: 5 reasons why they are important