What is an epiretinal membrane?
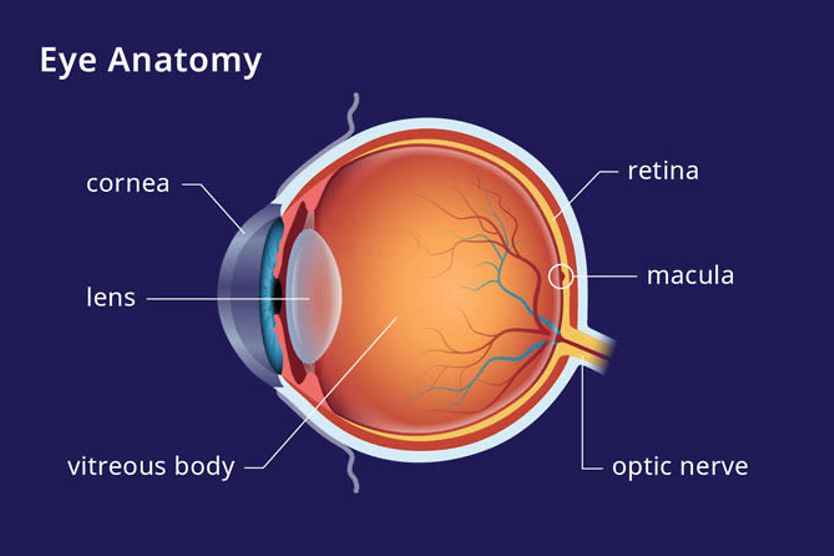
Epiretinal membrane (ERM)refers to a thin, semi-opaque layer of fibrous tissue that forms over the macula, the part of the retina that is responsible for processing sharp details and colors.
This eye condition, also known as cellophane maculopathy or macular pucker, is different from macular degeneration and macular holes. When an ERM develops, a cellophane-like scar tissue forms over the macula, which may cause vision to become distorted or blurry. Many people who develop an ERM do not have symptoms and do not need treatment. Their vision can be monitored at routine eye exams to watch for progression.
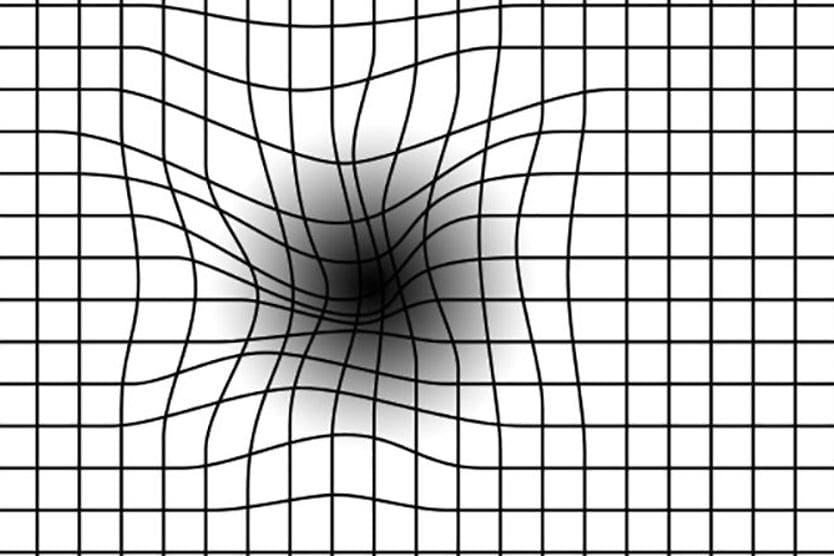
An ERM can shrink and pull on the macula, causing the macula to wrinkle or pucker, which is why an ERM is also known as macular puckering. Macular puckering can cause central vision to be distorted (metamorphopsia). That is, straight lines may look wavy, flat objects may appear round, and shapes may seem smaller than normal (micropsia)or larger than normal (macropsia).
Daily activities, such as driving, reading and identifying small details, may be affected due to this lack of visual clarity. At this point, epiretinal membrane surgery (vitrectomy) is recommended to stop the progression of the condition. This procedure also includes an epiretinal membrane peel (membranectomy).

Macular pucker, also known as epiretinal membrane, is a thin, film-like tissue that can form over the macula and cause distorted, blurry vision. [Image credit: Macular pucker. Permission granted by © 2022 American Academy Ophthalmology]
What causes an epiretinal membrane?
The exact cause of an epiretinal membrane is unknown, but you can develop an ERM even if you don't have any history of eye problems or any of the risk factors listed below.
Underlying factors that may contribute to ERMs include:
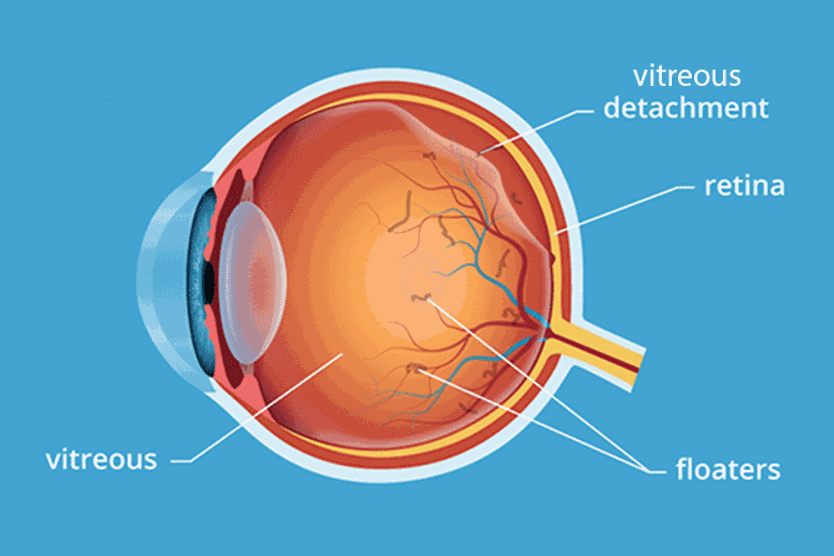
- Posterior vitreous detachment, a very common condition associated with ERMs
- Aging, especially age 50 and older
- Previous eye surgeries, including procedures for cataracts or retinal detachments or tears
- Head or eye injury or trauma
- Inflammation inside the eye (uveitis)
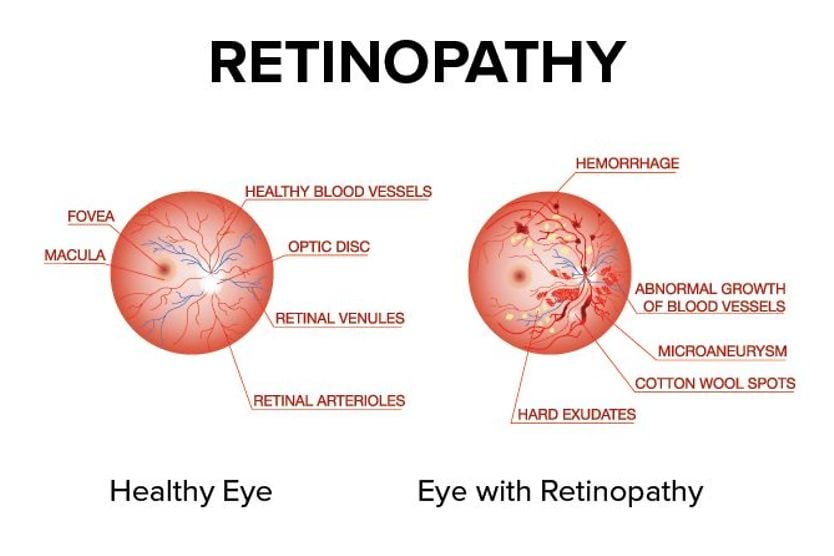
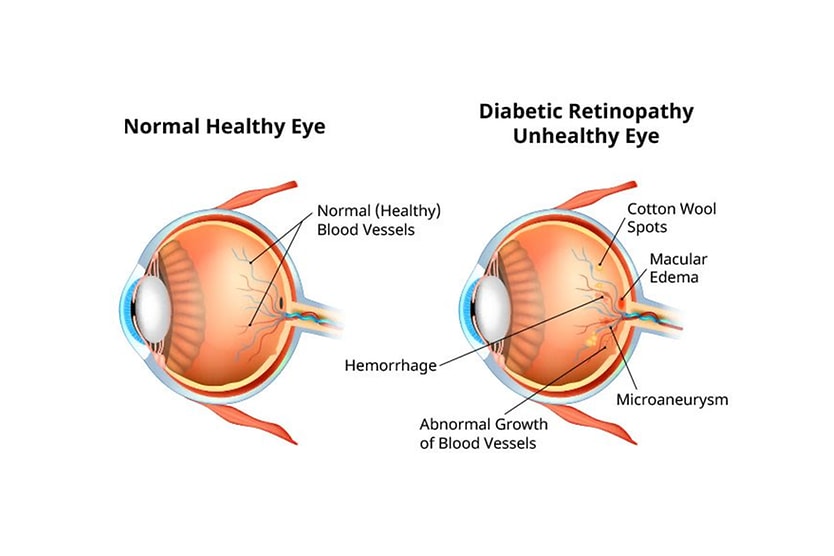
- Diabetes or diabetic retinopathy
- An existing ERM in the other eye
Signs and symptoms of an epiretinal membrane
The majority of people with an ERM show no signs or symptoms, so having an annual eye exam is important for early detection and monitoring as ERMs slowly get worse over time.
If symptoms of an epiretinal membrane are present, they may include:
- Distortion – A straight line appears crooked or bent.
- Difficulty reading – The letters of reading material seem unusually small or large.
- Blurry vision – The features of a person's face aren't sharp or easily distinguishable.
- Double vision (diplopia) – A single object looks like two objects.
- Decrease in visual acuity – Less visual sharpness than in the past.
It’s important to visit an eye doctor if you notice any signs and symptoms associated with an ERM — or if symptoms persist, worsen or change.
An epiretinal membrane can happen to anyone but it is more commonly found in the older population, specifically 2% in those over age 50 and 20% over age 75. The majority of the time, an ERM presents in one only eye, but in about 10% to 20% of cases, it can occur in both eyes. However, having an ERM in one eye can increase the likelihood of getting it in your other eye.
Epiretinal membrane surgery
When an epiretinal membrane interferes with your vision, surgery may be advised by your eye doctor. A vitrectomy improves vision in 80% to 90% of people and is done in conjunction with an epiretinal membrane peel.
During a vitrectomy, tiny cuts are made in the eyeball, and the transparent gel-like fluid in the eyeball (the vitreous humor) is removed and replaced with saline. Using miniature forceps, the surgeon peels off the ERM from the macula, and an air or gas bubble may be inserted to encourage healing.
Afterward, the macula becomes smoother and relaxes to lie back into position. It can take from three months up to a year for visual acuity to be restored.
As with all medical procedures, complications can occur following a vitrectomy, although the risk is low. These include:
- Infection (endophthalmitis)
- Bleeding
- Retinal detachment or tear
- Accelerated progression of cataracts
Typically, recovery after this outpatient surgery is slow, but improvements in vision typically begin within three to six months. Reoccurrence of ERMs may happen in a small percentage of people.
Only surgical treatment can improve vision and remove distortions caused by epiretinal membranes. Nonsurgical treatments — such as glasses, eye drops, medications or vitamins — do not help.
Many people who have an ERM usually don't need treatment, especially if it doesn’t affect their visual acuity and it doesn't progress.
If you have an ERM in only one eye, you may opt to rely on your other eye to see rather than undergo surgery. If untreated, though, an ERM can progress to the point where your everyday activities and quality of life are affected. Then, you may want to talk to your eye doctor about surgery.
Your eye doctor can diagnose epiretinal membranes
Since many people with epiretinal membranes have no noticeable symptoms, it may not be discovered until an annual eye exam.
If your eye doctor suspects you have an epiretinal membrane, they may use or perform any of the following tests to diagnose the ERM, measure its severity, and later to monitor its progression:
- Dilated eye exam – After dilating your pupils, the eye doctor uses a slit lamp with a highly magnified lens to look at the back of the eye for the presence of an ERM.
- Amsler grid – The Amsler grid, a grid with a dot at the center, may indicate metamorphopsia if you're seeing distorted or blurry lines.
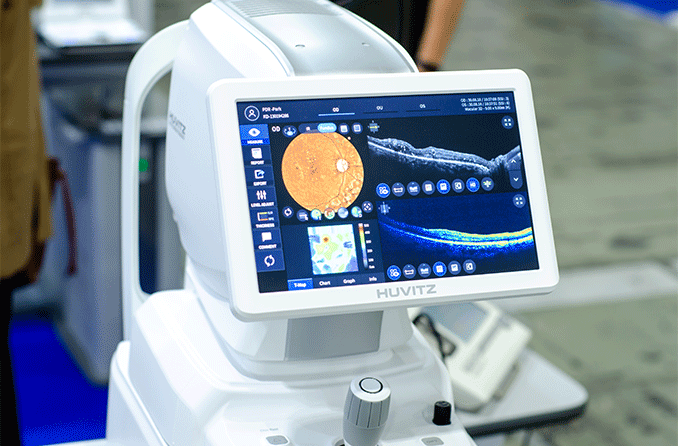
- Optical coherence tomography angiography (OCT/OCTA) – Using light waves, the OCT machine takes cross-sectional images of your retina's tissue layers for further evaluation.
- Fluorescein angiography – After injecting a fluorescent dye into your bloodstream, an ophthalmic photographer takes photos to assess blood flow as the dye travels through the retina's blood vessels.
If a year or more has passed since your last eye exam, it's time to schedule an appointment with an eye doctor near you.