What is the Schirmer test?
The Schirmer test is used to help diagnose dry eye syndrome, a common condition caused by a lack of tear production or a deficiency in the makeup of the tears. Eye doctors perform the test by using a small paper strip to absorb tears and evaluate the amount of moisture the eyes produce.
The test works through a process called capillary action, where a liquid (tears, in this case) flows through a narrow space due to natural forces. The distance the tears move along the filter paper strip within a set time reflects a person’s tear production rate.
Named after German ophthalmologist Otto Schirmer, the test was created in 1903 to measure tear production. However, it can also be used to detect an overproduction of tears.
The Schirmer test is sometimes referred to as the dry eye test, the tear (or tearing) test, the basal secretion test and the Schirmer tear test. It offers a quick, simple way to measure your eyes’ moisture level and determine if they make enough tears to keep them adequately lubricated.
How tears work
Tears are produced by:
- Goblet cells (special cells in the conjunctiva)
- The meibomian glands
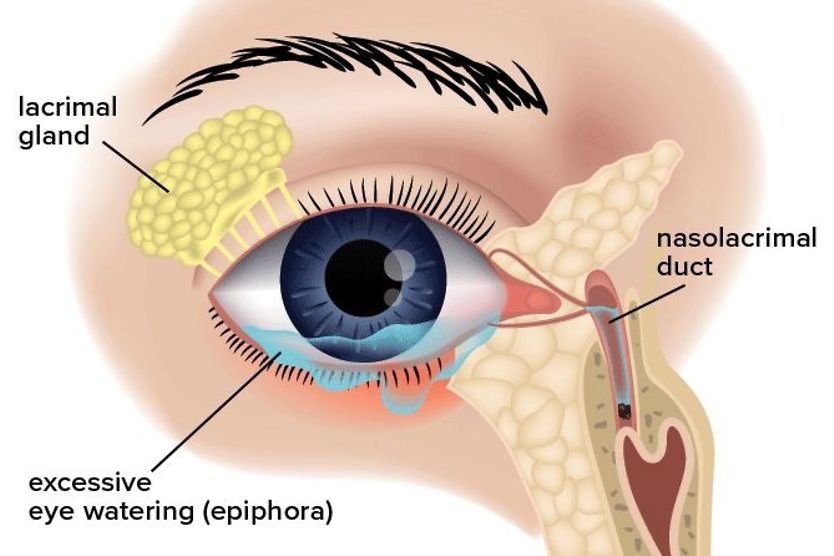
- The lacrimal glands
The goblet cells produce mucus while the meibomian glands make a special oil called meibum. The lacrimal glands produce the “salty, watery tears” with help from accessory lacrimal glands known as Glands of Krause and Wolfring.
Together, these cells and glands generate and release the watery, oily and mucus components of the tear film that keep your eyes moist and comfortable. They also help flush out debris and foreign bodies that may enter the eye.
If any of these glands isn’t working properly, your tears may fail to clean and moisturize your eyes. This can lead to eye redness, burning and grittiness — all symptoms of dry eye syndrome.
Why Schirmer’s test is performed
During an eye exam, your eye doctor may detect symptoms of dry eye or excessive tearing. If these symptoms are observed, they may use a Schirmer’s test to help determine if there’s a problem with tear production and how severe it is. This test isn’t usually part of a routine eye check unless symptoms like these are noticed.
Once the test results are received, your eye doctor will begin investigating the potential cause of your dry or over-tearing eyes and establish a treatment plan.
Potential reasons for having dry eyes include:
- Diabetes
- Aging
- Eye or eyelid inflammation
- Eye surgery (such as cataract surgery or LASIK)
- Thyroid conditions
- Specific cancer treatments
- Certain medications (such as decongestants or antihistamines)
- Sjögren’s syndrome
- Certain autoimmune diseases (such as rheumatoid arthritis or lupus)
- Vitamin A deficiency
Potential reasons for an overproduction of tears include:
- Eye allergies
- Eye irritation
- Extremely cold or windy climates
- Dry eye syndrome
- Conjunctivitis (pink eye)
- Blocked tear ducts
- Eye infections
Who should have the Schirmer’s test?
The Schirmer’s tear test may be performed on patients who are experiencing dry eye symptoms, such as:
- Red eyes
- A gritty, stinging or burning sensation in the eyes
- Blurred vision
- Watery eyes
- Discomfort when wearing contact lenses
- Light sensitivity
If you consistently have one or more of the symptoms listed above, schedule an eye exam so your eye doctor can determine the cause and provide options for relief.
Types of Schirmer testing
Different versions of the test may be performed based on your needs and your eye doctor’s assessments. The main types of Schirmer testing include:
Schirmer test 1
This is the Schirmer test commonly used during comprehensive eye exams. It measures normal and reflex tear secretion. (Reflex tears are those produced in response to a stimulus or irritant.)
The test may be performed with or without anesthesia, each of which measures different aspects of tear production:
- Without anesthesia – This version measures both normal tear production and the tear reflex resulting from eye irritation. The irritation is caused by the paper filter strip touching the eye.
- With anesthesia – This form measures normal tear secretion without the reflex tears caused by eye irritation. Numbing drops are placed in the eyes before the test. The anesthesia helps keep the eyes from tearing excessively.
Note: The Schirmer test performed with anesthesia is also referred to as Schirmer test 1. When performed without anesthesia, it’s referred to as Schirmer test 2.
Schirmer test 2
This version is not as widely used during comprehensive eye exams. It involves rubbing the mucus lining inside the nose with a cotton-tip applicator to trigger the secretion of reflex tears.
Schirmer test 3
Also not widely used, Schirmer test 3 evaluates reflex tear secretion that occurs after looking at the sun for a certain period of time.
How is Schirmer’s test performed?
Schirmer’s test 1 is simple to perform and doesn’t take very long to complete. It typically follows the process below:
Preparing for the test
Before starting the test, your eye doctor will ask you to remove your glasses or contact lenses (if you wear them). They will apply numbing eye drops in both of your eyes if the Schirmer test with anesthesia is being done.
The testing procedure
Your eye doctor will then place a strip of nontoxic filter paper inside the lower eyelid of each eye. They will instruct you to gently close your eyes and keep them closed for five minutes. (Some test processes may require keeping your eyes open during the test.) As your eyes produce tears, the strips of paper will soak them up, wetting the strip.

After five minutes have passed, the paper strips will be removed from your lower eyelids. The amount of moisture on each strip will be measured in millimeters.
After the test
Your eye doctor will discuss any post-test instructions. Generally, you should avoid rubbing your eyes for about 30 minutes. It is recommended to wait at least two hours before putting your contact lenses back in.
What your Schirmer test results mean
Your eye doctor will discuss your test results with you and what they could mean for your eye health. A lower score indicates a greater chance of reduced tear production, which may signal dry eye syndrome or other conditions.
Normal vs. abnormal results
The area of the test strip that is wet with tears will be measured in millimeters. The test results are usually categorized as follows:
- More than 15 millimeters – Typically considered normal tear production. Dry eye syndrome is unlikely.
- 10 to 15 millimeters – Slightly reduced tear production. Dry eye may be possible.
- 5 to 10 millimeters – Moderately reduced tear production. Dry eye is likely.
- Less than 5 millimeters – Extremely reduced tear production. Severe dry eye is likely.
In many instances, measurements of fewer than 10 millimeters are considered abnormal and could indicate that your eyes may not be making enough tears. If your results are over 15 millimeters, your eye doctor will likely let you know if you’re producing an excessive amount of tears.
Factors affecting test results
Certain factors can affect the accuracy and interpretation of Schirmer test results, such as:
- Type of test performed – The use of anesthesia in Schirmer test 1 can reduce the tear reflex. This may result in lower tear secretion and influence test results.
- Open vs. closed-eye testing – Closed-eye test results may show lower test scores than open-eye tests. Reduced exposure to factors like blinking and environmental irritants decreases the likelihood of tear secretion.
- Age – Older people tend to have lower Schirmer scores, as tear production naturally decreases with age.
- Gender – Women, particularly those who are post-menopausal, tend to have lower Schirmer scores. Changes in hormone levels can affect tear secretion.
- Certain medications – Some medications, such as anticholinergic drugs, can affect tear production, causing the eyes to make fewer tears.
- Environmental factors – External factors like climate and temperature can impact test results. For example, low humidity, wind and dry climates can result in a lower Schirmer score.
Your eye doctor may perform other tests to confirm a dry eye diagnosis and pinpoint the cause of your symptoms. They can also discuss dry eye treatment options to help manage the condition.
Similarly, if your eyes are watery, they will investigate potential causes and establish a treatment plan from there.
Alternatives and advancements in tear testing
While the Schirmer test has been used in ophthalmology and optometry for over a century, it may not be favored in certain cases because of its variability. As a result, eye doctors may perform alternative methods to assess tear secretion. Common methods include:
Tear break-up time (TBUT) test
This test measures how long tears stay in your eyes after you blink. To perform the TBUT test, your eye doctor will place drops containing a special dye into your eyes to temporarily stain the tear film. You’ll be asked to blink once and then look straight ahead without blinking or moving your eyes.
Your eye doctor will observe how long it takes for a dry spot to appear in the stained tear film in your eye. This is referred to as the “tear break-up time.” A TBUT of less than 10 seconds could indicate dry eye syndrome.
Tear meniscus height (TMH) assessment
Eye doctors use this test to measure the tear meniscus (the accumulation of tears that gathers at the edge of your eyelid). This helps them determine if your eyes are making enough tears.
The assessment may be performed in various ways. For example:
- Your eye doctor may use a special microscope called a slit lamp to examine the thickness of your tear meniscus. They then compare it to the edge of your eyelid or a light beam.
- Your doctor may use a technique called optical coherence tomography (OCT) to scan the tear film and produce a digital image that allows them to measure the meniscus.
Tear osmolarity test
Tear osmolarity testing measures the amount of salt in your tears compared to their water content. To perform the test, your eye doctor will place a special device on the edge of your lower eyelid. A special card on the tip of the device will collect a sample of your tears.
The device will provide a readout of your tear concentration. An osmolarity reading of greater than 308mOsm/L could indicate dry eye syndrome.
Phenol red thread (PRT) test
During this test, the end of a thin yellow-colored thread is placed in the lower eyelid, similar to how paper strips are used in the Schirmer tear test. The thread contains phenol dye, which turns red when coming into contact with tears.
The thread is left in the eyelid for 15 seconds. After removing the thread, your eye doctor will measure the length of the red-dyed portion in millimeters, which indicates the amount of wetting by your tears. Fewer than 10 millimeters of moisture could indicate dry eye syndrome.
Future prospects in tear testing
Emerging technologies are changing the landscape of diagnostic capabilities in tear production assessment. Recent advancements in analyzing tears include:
- Digital imaging – Digital images taken of the cornea (the eye’s outer surface) allow eye doctors to examine the tear film layers in greater detail.
- Biosensing technology – Contact lenses equipped with special biosensors, when worn on the eyes, could enable the real-time detection of tear composition and production.
- Artificial intelligence (AI) – AI-driven tools are helping experts to analyze eye images, measure tear secretion and predict dry eye severity with potentially greater accuracy.
These advanced technologies, along with others, show promise in improving the diagnosis and management of dry eye syndrome.