Do I have to get the air puff test during my eye exam? No, the air puff test is not the only option these days for measuring your eye pressure. In fact, your eye doctor might have stopped using the air puff test.
It's easy to understand why you and others might rather skip the air puff test. For decades, that quick "poof" sound of air being shot into your eye may not have been your favorite part of a comprehensive eye exam.
But what is the air puff test, how does it work and are there alternatives? We've got the answers to frequently asked questions about the air puff test.
What is the air puff test?
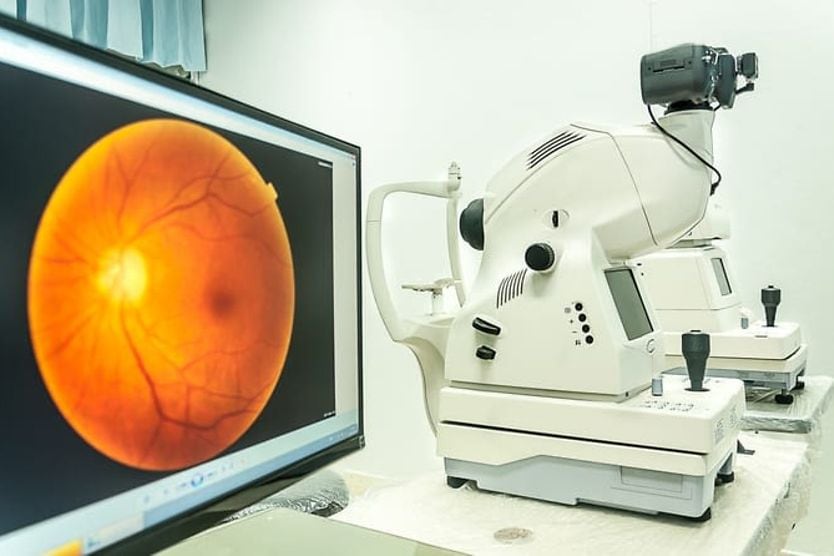
Traditionally, ophthalmologists and optometrists have gauged the pressure inside your eyes using the air puff test, formally known as “non-contact tonometry” or “air puff tonometry.”
The test helps determine whether you are at higher risk for developing glaucoma, a condition that harms the optic nerve and can cause blindness.
It’s important to know that glaucoma may occur when fluid builds up in the front part of your eyes, causing your eye pressure (known as intraocular pressure, or IOP) to go up.
How does the air puff test work?
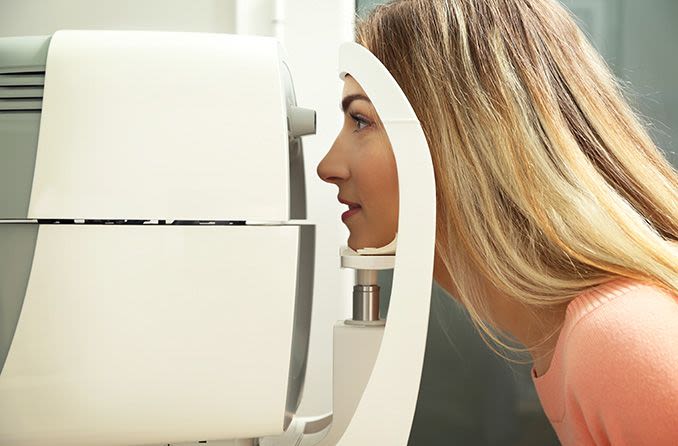
The air puff test typically starts with a patient seated at the tonometry machine with their chin atop the equipment’s chin rest. As the patient looks at a light inside the machine, a small burst of air is “puffed” into each open eye.
Although this might be a little uncomfortable and unnerving, it’s typically not painful; nothing but the puff of air touches the eye. Numbing eye drops aren’t required for the air puff test.
The puff of air slightly flattens the cornea. How much the cornea flattens depends on your eye pressure.
Based on your eyes’ response to the puffs of air, the tonometer calculates the pressure inside each eye. A high level of pressure might mean you’re at risk of developing glaucoma or already have the condition.
Since glaucoma may not be accompanied by symptoms, it’s quite possible to have the condition without realizing it.
It is estimated that more than 3 million Americans have glaucoma, and about half of them are unaware of it.
That’s why it’s critical for an eye doctor to perform a glaucoma test as part of a comprehensive eye exam, and to get eye exams regularly.
WHEN WAS YOUR LAST EYE EXAM? Find an eye doctor near you and schedule an appointment.
How effective is the air puff test?
The air puff test is a simple way to check eye pressure, especially in children.
Are there alternatives to the air puff test?
The majority of eye doctors have adopted other methods of tonometry to measure eye pressure and help detect glaucoma.
One of these methods is applanation (Goldmann) tonometry. Here's how this test for measuring eye pressure works:
- An eye doctor numbs the surface of each eye with eye drops.
- You rest your chin and forehead against the tonometer to keep your head still during the procedure.
- The eye doctor asks you to keep your eyes open and look directly ahead.
- The eye doctor touches your cornea with the tip of the tonometer.
- The eye doctor looks through an eyepiece and adjusts a dial on the machine to read your eye pressure.
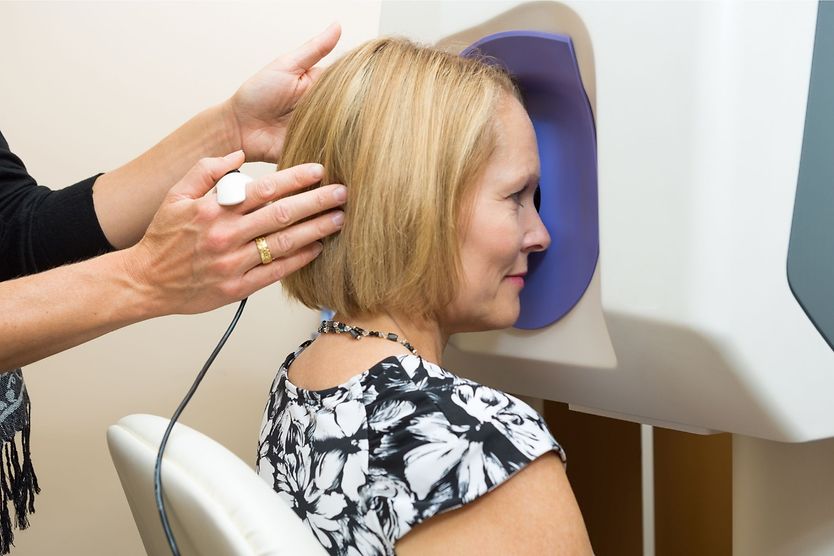
The second alternative to the air puff test is called electronic indentation tonometry.
In this test, an eye doctor measures your eye pressure with a handheld, pencil-shaped device after numbing eye drops have been administered to ease discomfort. The eye doctor touches the surface of your cornea with the device and records your eye pressure. The results might differ from those supplied by applanation tonometry.
Is just one of these tests enough to diagnose glaucoma?
No. Checking your eye pressure isn’t enough to determine whether you have glaucoma. An eye doctor also may:
- Look at the drainage angle of your eye to see whether it’s blocked. That blockage can cause a buildup of fluid, leading to a potential increase in eye pressure.
- Examine your optic nerve for damage.
- Take a picture or computer measurement of your optic nerve.
- Test your peripheral (side) vision.
- Measure the thickness of your cornea.
DOES GLAUCOMA RUN IN YOUR FAMILY? Find an eye doctor near you and book a comprehensive eye exam.