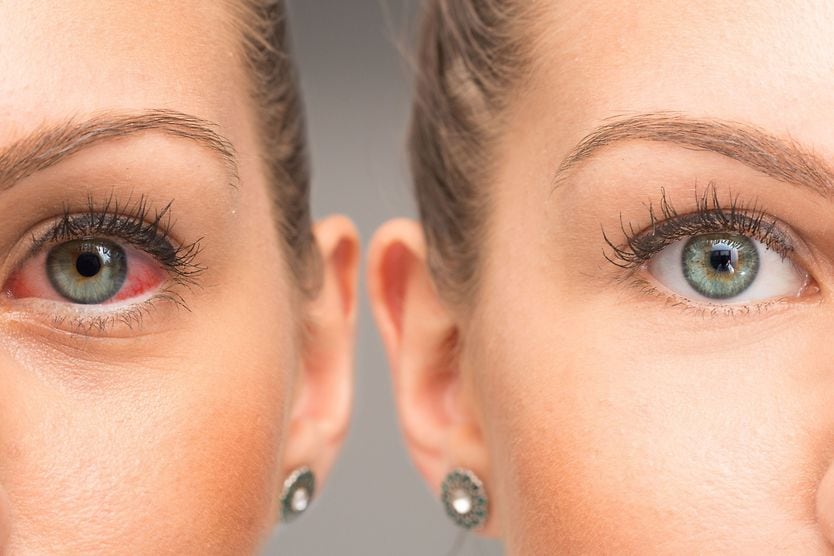
How to relieve dry eyes
The optimal way to treat dry eyes is to find out what’s causing them. There are three main layers to a healthy tear film: water, oil and mucin. A problem with one or more of these tear components can cause temporary dryness or chronic dryness, called dry eye disease (DED).
To determine which part of your tears is causing issues, an eye doctor will need to perform a complete eye exam and dry eye evaluation. Based on how each eye’s surface looks, as well as this dry eye testing, your eye doctor will be able to recommend treatment options.
Some options they may recommend include artificial tears, other types of eye drops, eyelid treatments or specific vitamins and supplements. They may also suggest different therapies you can do at home. Some cases of DED may need prescription medication or surgery to effectively treat the problem.

Click photo to enlarge.
Treating symptoms of dry eyes
If your dry eye symptoms only last a short period of time, you may be able to treat them from the comfort of your home. Frequent or persistent dryness may need prescription treatment from an eye doctor.
Over-the-counter artificial tears, ointments and eye drops
There are many types of lubricating eye drops (also called artificial tears) that you can buy and use without a prescription. These eye drops can often treat mild, temporary dryness.
Lubricating eye drops are made with similar elements that your natural tears contain. When applied, the drops work with your tear film to provide comfort, hydration and protection for your eyes.
Some eye drops contain preservatives that help prevent bacteria and other microorganisms from forming in the bottles after they’re opened. Preservatives are not usually harmful to the eye when used fewer than four times per day.

Artificial tears usually are the first step in dry eye treatment.
However, eye doctors often recommend using preservative-free artificial tears to avoid potential irritation or allergies. The packaging should specify whether the product is preservative-free.
It’s important to know that eye drops are not a one-size-fits-all solution. Different types of eye drops address different sources of dry eye. This depends on what part of your tear film is lacking. Some people may require a mixture of two or more artificial tears to treat DED.
If artificial tears don’t seem to do the trick, you may find relief with lubricating eye gels or ointments. These have a thicker consistency than artificial tears, which helps them stay in your eyes longer.
Because they’re thicker, ointments or gels may cause temporary blurred vision. For this reason, many users prefer to apply them before they go to sleep for the night.
SEE RELATED: What are artificial tears used for?
Prescription medications
Severe or chronic DED may need more than what an over-the-counter eye drop can provide. In this case, your eye doctor can prescribe medicated eye drops as dry eye treatment.
Cyclosporine ophthalmic emulsion 0.05%
Cyclosporine 0.05% eye drops, do more than lubricate the surface of your eyes. They include an agent that reduces inflammation associated with dry eye syndrome and help your body produce more natural tears.
But it's important to know that the therapeutic effect is not immediate. You must use the drops daily for at least 90 days (about three months) to get the full benefits of this dry eye treatment. This therapy was shown to help the eye make more tears and heal dry eye signs and symptoms for at least two years.
The dosage recommendation for cyclosporine 0.05% is one drop in each eye, twice per day, 12 hours apart. Some people experience burning eyes and redness during the first few weeks of use.
Cyclosporine ophthalmic solution 0.09%
These eye drops also work to reduce inflammation that leads to dry eye symptoms and help you produce more tears naturally.
This formulation contains about double the dose of cyclosporine. It uses a type of technology that allows for a higher concentration of the medicine to be used in the eye. The consistencies of the eye drop solutions are also different.
For best results, which may take a few months to notice, apply one eye drop in each eye two times per day.
Lifitegrast ophthalmic solution
Lifitegrast ophthalmic solution is another prescription eye drop for dry eye treatment. Lifitegrast helps reduce the inflammation associated with DED.
The most common side effects reported in studies were eye irritation, altered taste sensation and reduced visual acuity, which occurred in 5% to 25% of participants.
The recommended dosage for lifitegrast ophthalmic solution is also one drop in each eye twice per day. Ideally, the drops should be administered around 12 hours apart.
Perfluorohexyloctane ophthalmic solution
This is a newer eye drop for DED symptoms caused by meibomian gland dysfunction (MGD). It claims to target excessive tear evaporation to help the eyes stay hydrated.
The drops are 100% perfluorohexyloctane, a non-steroidal formula that does not contain water or preservatives.
Steroid eye drops
Inflammation has been recognized as a significant cause of DED. It frequently causes redness and burning associated with dry eye disease.
Artificial tears don’t usually address these inflammatory changes. Your doctor may recommend steroid eye drops to better manage the underlying inflammation associated with dry eyes.
Steroid eye drops like loteprednol etabonate ophthalmic suspension 0.25% are used short-term to quickly manage symptoms. They are often used in addition to artificial tears and cyclosporine-based eye drops. This cocktail of eye drops combines the short-term solution with the long-term dry eye treatment strategies.
Steroid eye drops (especially if used for long periods) have the potential to cause side effects. It's important to make your eye doctor aware of your full medical history before starting steroid eye drops.
Hydroxypropyl cellulose ophthalmic insert
A hydroxypropyl cellulose ophthalmic insert is a sterile, slow-release lubricant. It is placed under the lower eyelid where the inner eyelid meets the eye.
It is a solid insert composed of a preservative-free lubricating agent that slowly liquefies over time. This provides an all-day moistening effect.
This option is typically recommended for patients with moderate to severe DED symptoms — especially if artificial tears alone are unsuccessful. A single insert should be applied once a day for all day relief.
Punctal plugs
Both the upper and lower eyelids contain a punctum (the opening of the tear duct). The punctum allows the tears to drain away from the eye through the lacrimal duct into the back of the nose. Punctal plugs, also called punctum or lacrimal plugs, are inserted into the opening of the punctum to help maintain a better tear film.
Since about two thirds of the tears drain through the lower punctum, this is the one that is generally treated. In this way, the eye is able to retain more of its own tears.
Punctal plugs are biocompatible and about the size of a grain of salt. They can be inserted into the eyelid in the outpatient clinic during a dry eye evaluation. The process does not hurt, and you typically will not feel the punctal plug in the eyelid afterward.
Varenicline solution
Varenicline solution is a prescription nasal spray that can help treat symptoms of chronic dry eye syndrome. The spray works through the nerve endings inside your nose to activate tear film production.
This should allow users to create more of their own natural tears rather than relying on artificial tears. The most common side effects are sneezing, coughing and irritation in the nose and throat.
For the optimal results, varenicline solution should be sprayed once into each nostril twice per day. The medication should just touch the inside of the nostril and not be inhaled or squirted up into the nose.
Be sure to follow your eye doctor’s directions about which eye drops to use and how often you use them. Using a different brand or multiple brands of artificial tears will make it difficult to assess the success of the dry eye treatment your doctor recommended.
Nutrition for dry eyes
Dry eye treatment consists not only of what you put into the eyes, but also of what you put in your body. Incorporating certain vitamins, supplements and foods into your diet can reduce eye dryness.
Vitamins and supplements
For a long time, omega-3 fatty acids were considered the best nutritional supplements to reduce or treat dry eye. This is because omega-3s are anti-inflammatory in nature.
However, recent studies have challenged this belief. One study examined eye dryness of participants who took omega-3 supplements daily compared to those who took olive oil instead. Results showed that both omega-3 supplements and olive oil helped reduce DED.
Since olive oil contains no omega-3s and still reduced DED, this study has raised questions about the helpfulness of omega-3s. But many doctors still recommend trying them to see if they work for you.
It’s important to note that omega-3s aren’t a fit for everyone. For example, people who are on blood thinners should avoid omega-3s due to an increased risk of bleeding. Talk to your doctor before adding any new medicines or supplements to your regimen.
Other vitamins and supplements your eye doctor may recommend to improve or treat dry eyes include:
- Vitamin A – can help protect the cornea by forming a barrier against bacteria
- Vitamin B12 – can help repair the nerve layer of the cornea, which may reduce eye pain and burning
- Vitamin D – can reduce inflammation and improve the quality of tears produced
Foods
There is evidence that the optimal foods for dry eye treatment are those that are rich in omega-3 fatty acids and the vitamins listed above. Superior sources of omega-3s and Vitamins A, B12 and D include:
- Cold-water fatty fish including salmon, tuna, sardines, mackerel and herring
- Plant oils such as canola oil, soybean oil and flaxseed oil
- Fortified foods, including certain brands of infant formula, milk, yogurt, eggs, juices and soy beverages
- Seeds and nuts such as walnuts, chia seeds and flaxseed
- Leafy green vegetables such as kale, broccoli and spinach
- Orange and yellow produce including carrots, squash, cantaloupe, pumpkin, mango and sweet potatoes
- Red produce such as tomatoes and red bell peppers
- Liver or cod liver oil
- Red meat
- Poultry
- Cheese
- Orange juice fortified with Vitamin D
- Fortified breakfast cereals
- Dairy and plant milk fortified with Vitamin D
The optimal way to modify your diet to help treat dry eyes is to replace high-sugar and processed foods with many of the eye-healthy foods listed above. Sugary and processed foods tend to increase inflammation that contributes to dry eyes.
SEE RELATED: How better nutrition can improve your vision
Warm compress
Dryness can occur when the eyelid glands that release oil-based tear film become stagnant. These glands, called the meibomian glands, may benefit from warm compresses.
The warmth and humidity of the compress can help loosen clogged or stagnant oil from the glands. Warm compresses also stimulate meibum production, which can soothe irritated eyes.
To do this, it's often recommended to wet a clean washcloth with very warm (not hot) water. Wring out any excess water, then gently press the washcloth against closed eyelids.
It’s important for the eyelids to get consistent warmth for at least five to 10 minutes. Washcloths don’t stay warm this long, so you need to rewarm them about every two minutes.
Store-bought options are often designed to stay warm longer. The recommended way to prepare at-home warm compresses is with the washcloth “bundle method.”
Some things to consider when using a warm compress on the eyes:
- Only place warm compresses over the eyes, not hot. Excessive heat can scald or burn the delicate skin on and around the eyelids.
- Use a new, clean washcloth every time you do a warm compress. This helps prevent the spread of bacteria and potential infection.
- Warm compresses may need to be applied daily for chronic dry eye treatment. However, overuse can cause irritation, especially when a wet cloth is used. Ask your doctor for recommendations on how often and how long you should use warm compresses.
Eye massage
An eyelid massage can help release the oil that was loosened with the compress. This can also promote new oil production. However, you should always massage the eyelids gently, especially after a warm compress. The corneas are even more susceptible to distortion while they are warm.
Eye doctors often recommend this method: After washing your hands with soap and water, use your fingers to softly massage the upper and lower eyelids. Massage downward on the upper eyelid, and massage upward on the lower eyelid. Do this starting at the inner corner of the eye and moving outward toward the ear.
It’s recommended to massage each eyelid for about 30 seconds while keeping the eyes closed. Repeat five to 10 times on each eye.
Eyelid heating and massage treatments
Various treatments are available to help dry eyes caused by meibomian gland dysfunction. Some of these treatments are done using thermal pulsation systems, which combine the features of warm compress therapy and meibomian gland expression. Other systems deliver heat therapy and rely on the doctor to massage the eyelid.
Eyelid heating and massage systems go by different names depending on the manufacturer. However, the treatment they provide is generally the same, with the exception of one treatment that has an automated massaging system built into the procedure.
A device fits over the eyelids and applies precisely controlled heat to the lids. This softens hardened meibum trapped in the meibomian glands. At the same time, the pulsation system (or the eye doctor) applies pulsed pressure to the eyelids. This opens and expresses the clogged glands, restoring the balance of oils in the tear film.
While the duration of each system varies, some treatments take approximately 12 minutes per eye. Patients often notice an improvement in symptoms within two weeks of treatment. However, it can take a few months for improvements to become apparent. Results of certain procedures were shown to last three months to a year or longer.
Potential side effects from treatments like these may include corneal abrasion, eye pain, swollen eyelids and eyelid irritation or inflammation. Other side effects can include chalazia, transient blurred vision, itching and red eyes. The eyes may also feel dry for a day or so after the treatment. It removes the oil from the meibomian gland, so the oily layer of the tear film needs time to restore itself.
These treatments are not typically covered by health insurance, but coverage may vary.
Lifestyle changes
There are many lifestyle choices that could cause eye dryness without you realizing it. Adjusting these choices can help reduce or eliminate your symptoms.
Personal circumstances that may cause or worsen dry eyes include:
- Smoking or being around smoke
- Living in an extremely cold, dry or windy climate
- Spending long periods of time staring at a screen
- Being dehydrated
- Taking certain medications
- Lacking adequate sleep each night (7 to 8 hours)
While some of these things are out of your control, making small changes where you can may improve your dry eyes.
SEE RELATED: How to find the best eye drops for your symptoms
Treatments for underlying causes of dry eye
Besides lifestyle choices, there could be several underlying causes for your dry eye problems. Underlying causes can range from contact lens wear to certain medical conditions or medications.
It’s also possible for other eye-related problems to cause dryness. In this case, an eye exam can lead to proper treatment.
Contact lenses
Technically, wearing contact lenses does not cause DED. But it can make the condition worse. Studies estimate that half of contact lens wearers complain of eye dryness and discomfort at the end of the day. Additionally, 25% to 30% of wearers stop using contact lenses due to the dryness and discomfort they experienced when wearing them.
Experts believe that the irritation felt by certain contact lens wearers is due to having a weak or thin tear film. When you add contact lenses to the mix, it emphasizes the tear film problem and creates discomfort.
Lubricating eye drops can soothe the irritation felt when wearing contact lenses. It’s not recommended to apply most eye drops while wearing contacts. But certain formulas are safe to use while wearing contacts.
There are also specific contact lenses for dry eyes that may reduce grittiness and irritation. Scleral contact lenses, which are larger than typical contacts, rest over the white parts of the eye. This tends to be more comfortable for users — especially for those with extreme dry eye.
Medical conditions
Underlying medical conditions can cause inflammation, leading to DED. The most common conditions related to dry eyes include:
If you’ve been diagnosed with one or more of these conditions, talk to your doctor about dry eye treatment options. Other biological changes that can cause DED include aging, pregnancy and menopause.
SEE RELATED: Risk factors that can affect women’s vision
Check your medications
Specific medicines taken can cause your eyes to become gritty and irritated. Taking the following categories of medications may cause or worsen dry eyes:
- Antihistamines and decongestants (Antazoline, Brompheniramine, Carbinoxamine, Pyrilamine)
- Beta blockers (Propranolol, Oxprenolol, Metoprolol)
- Pain relievers (Morphine)
- Antidepressants (Amitriptyline, Desipramine, Imipramine, Protriptyline, Nortriptyline)
- Anxiety medications (Alprazolam, Diazepam, Clonazepam, Lorazepam)
- Anti-nausea medications (Trifluoperazine, Thiethylperazine, Tetrahydrocannabinol, Scopolamine)
- Gastrointestinal medications (Atropine, Methscopolamine)
- Antipsychotic medications (Acetophenazine, Carphenazine, Chlorpromazine, Fluphenazine, Methotrimeprazine, Mesoridazine)
- Medications used to treat Parkinson’s disease (Ethopropazine)
- Acne medications (Isotretinoin)
- Hormone treatments (Birth control pills, hormone replacement therapy, medical fertility such as in vitro fertilization (IVF))
- Chemotherapy medicines
If you feel your dry eye has worsened since starting a particular medicine, discuss this with your doctor. They may be able to suggest an equally effective alternative that won’t cause dry eyes.
Consider your screen time
Spending time in front of a screen, whether it be a smartphone, tablet or computer, can cause the eyes to become dry, irritated and fatigued. This is a condition known as digital eye strain or computer vision syndrome.
The main reason screen time leads to DED is because we blink less when focusing on a screen. Blinking spreads tear film across the surface of the eyes, which keeps them hydrated.
Without computer use, people blink an average of 18.4 times per minute. When focusing on a digital screen, that number drops to 3.6 blinks per minute. Blinking only three times per minute is not nearly enough to keep the eyes clear and hydrated.
When using a screen, it’s important to blink frequently and to take regular breaks. Eye care experts recommend the “20-20-20 rule.”
The rule encourages screen users to take a break every 20 minutes. During the break, focus on an object at least 20 feet away for at least 20 seconds. You can also close the eyes for a few seconds to allow the eyes to rest.
See an eye doctor
Problems within the eye itself may also cause eye dryness. Regular eye exams can help your eye doctor detect, treat and manage these conditions. Addressing any underlying conditions can ultimately help to treat dry eye.
Three common eye conditions that can cause dry eyes include meibomian gland dysfunction, blepharitis and lagophthalmos.
Meibomian gland dysfunction
The meibomian glands are small glands in the eyelids that produce the oil component of tear film. When these glands become clogged or inflamed, it can reduce the amount of oil (called meibum) in your tears. This is a common condition called meibomian gland dysfunction (MGD).
The oil layer of tears keeps the water layer from evaporating, which helps lock in moisture. When the oil layer is lacking, the water layer evaporates, leaving the eyes feeling dry.
Treatment for MGD can consist of at-home therapies, like warm compresses and eyelid massages. There are also in-office therapies that use machines to help meibomian gland function. If you think you have MGD, talk to your eye doctor about treatment recommendations.
Blepharitis
Blepharitis is a condition that affects the eyelids, causing them to become swollen, itchy and red. It often occurs due to excess bacteria on the eyelids or when oil glands become irritated.
Dry eyes are a complication of blepharitis that happens when oil and/or flakes from the eyelid build up in your tear film. This buildup can cause the eyes to feel dry.
Blepharitis is often treatable with frequent eyelid cleansing. Some studies also suggest using tea tree oil or hypochlorous acid to aid in dry eye symptoms. Lotilaner ophthalmic solution 0.25% is a newer eye drop that was shown in clinical trials to successfully treat Demodex blepharitis.
Over-the-counter eye drops and antibiotics can also be helpful when dealing with blepharitis. Keep in mind that treatment for underlying conditions, such as rosacea or dandruff, may also be needed.
Lagophthalmos and floppy eyelid syndrome
Lagophthalmos is a condition in which a person cannot completely close the eyelids. This may occur when blinking or sleeping (nocturnal lagophthalmos).
Floppy eyelid syndrome (FES) is caused by a softening of the eyelids that allows them to come open during sleep. This exposure dries out the eyes and leaves them vulnerable to rubbing on the pillow.
As mentioned earlier, blinking is important for maintaining healthy eyes and tear film. When the eyes cannot close completely, or they come open during sleep, the tear film becomes unstable and evaporates faster than normal.
Serious problems with the cornea can occur if left untreated. Complications include keratopathy, corneal ulcers and corneal protrusion. Treatment for lagophthalmos may include artificial tears, eye ointment or gel, eyelid taping at nighttime and moisture chamber glasses. Several surgical options are also available to treat severe cases.
Before trying any treatment for dry eye, get professional insight from an eye doctor. They can assess your symptoms and suggest the optimal dry eye treatment for you.
READ MORE: Corneal erosion