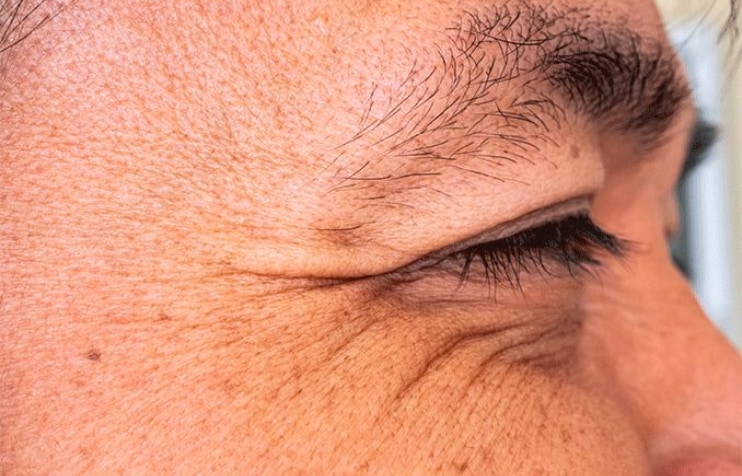
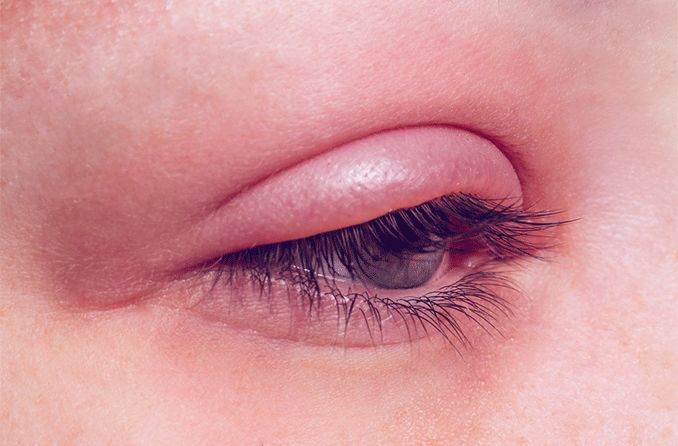
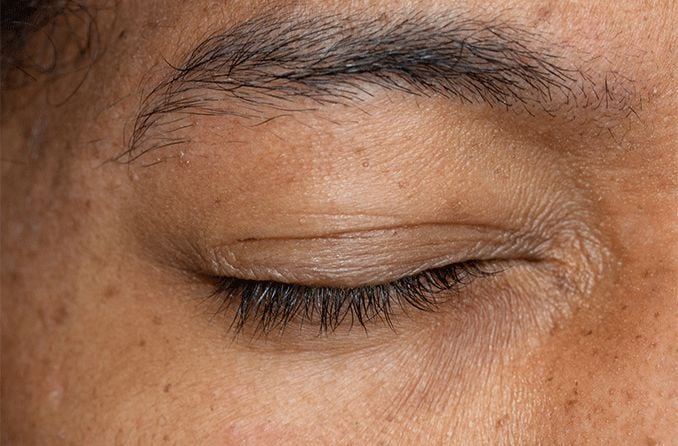
What is lagophthalmos?
If you struggle to close your eyes all the way, you may have a condition called lagophthalmos. With lagophthalmos, the eyelids are unable to close completely. This condition can have a variety of causes, from eyelid problems to facial paralysis.
Types of lagophthalmos (la-guhp-THAL-mowz) include paralytic, mechanical and cicatricial (scarring of the eyelids). Lagophthalmos that occurs during sleep is called nocturnal lagophthalmos.
Lagophthalmos is not a dangerous condition in itself, but it can lead to serious eye problems. When your eyelids don’t close all the way, it leaves your corneas exposed to the outside environment. (The cornea is the clear, dome-shaped area of the eye in front of the iris and pupil.) Over time, this can lead to irritation, scarring, disruptions in the tear film and even vision loss.
Lagophthalmos could also indicate a serious medical condition that requires treatment. This includes facial nerve paralysis or an autoimmune disorder like thyroid eye disease (also known as Graves’ disease).
Symptoms of lagophthalmos
The primary symptom of lagophthalmos is the inability to close your eyes. Additional symptoms may include:
- Burning
- Redness
- Eye pain
- The sensation of having a foreign object in your eye
- Increased tearing
- Dry eyes
- Blurry vision
Nocturnal lagophthalmos may be more difficult to identify since it only occurs during sleep. If you experience any of the above symptoms — including after waking up in the morning or after a nap — contact your eye doctor.
Causes of lagophthalmos
Lagophthalmos can be caused by damage to the facial nerve or other nerves that control the eyelids. The cause could be an underlying disease or another condition, such as:
- Stroke – Bleeding or blood flow blockage in the brain that damages the nerves to the eyelid
- Tumors – When a mass presses on or damages the nerves or muscles of the eyelid
- Moebius syndrome – A rare condition in babies that affects facial nerves
- Bell’s palsy – A temporary facial paralysis on one side of the face
- Eye trauma – Injury to the eye, such as from blunt force trauma or a penetrating object
- Autoimmune diseases – Conditions in which the body’s defense system attacks healthy cells, such as multiple sclerosis, Guillain-Barré syndrome or temporal arteritis
Conditions or factors that affect the positioning or health of the eyelids can also cause lagophthalmos. These may include:
- Floppy eyelid syndrome
- Scarring due to surgery, injuries or burns
- Medical treatments such as Botox
- Infections involving the eyelids
- Symblepharon (where the membranes lining the whites of your eyes and your eyelids stick together)
The underlying causes of lagophthalmos can range from mild to severe. In any case, it is important to see an eye doctor for an evaluation so the cause can be determined and treated.
RELATED READING: Parts of the eyelid and how they work
Diagnosis
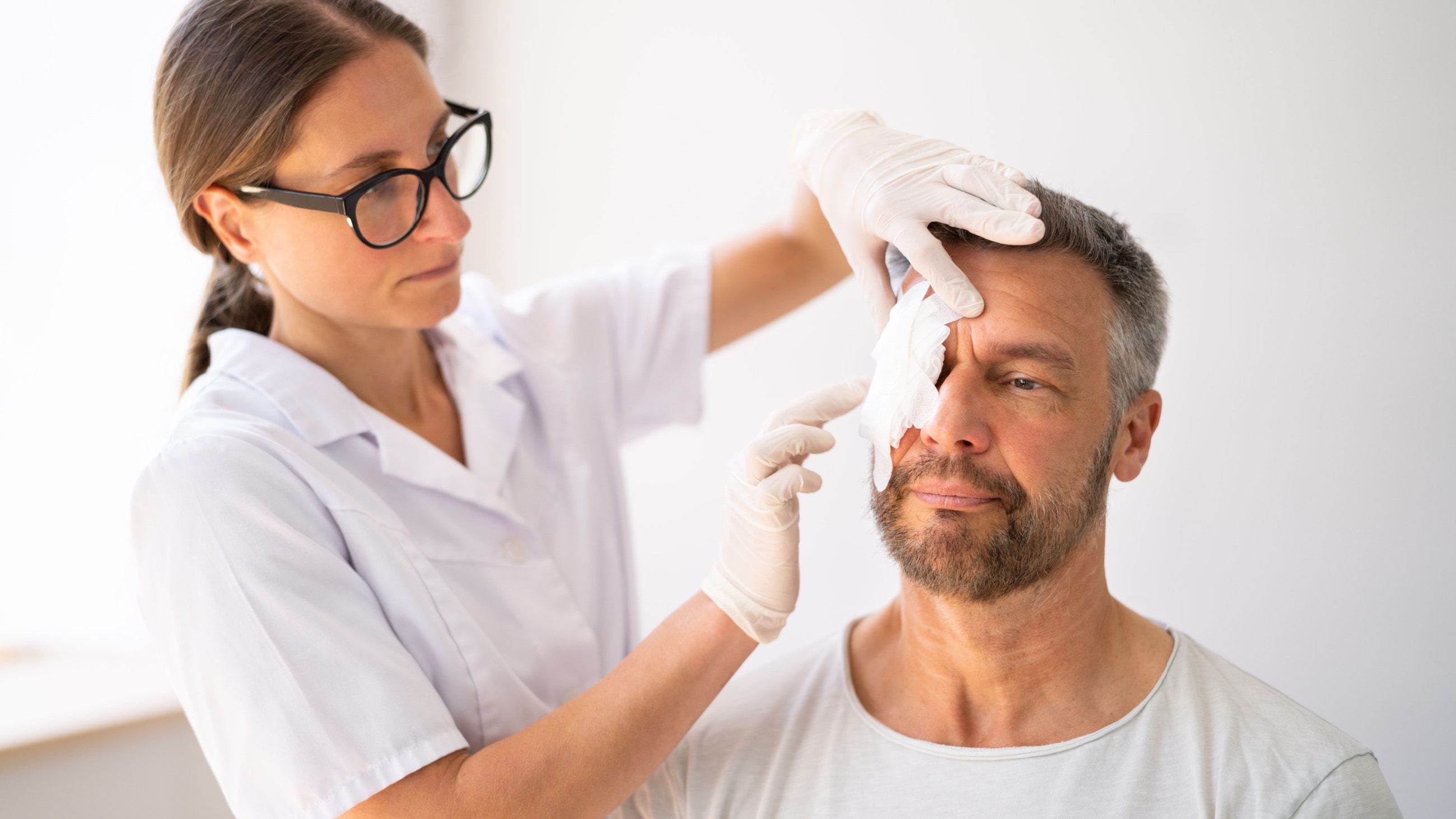
To diagnose lagophthalmos, an eye doctor will first discuss any recent medical problems. This will be followed by a thorough examination, including evaluating your eyelids and how you blink and close your eyes.
Your doctor will first review your medical history. You should let your eye doctor know if you’ve had a recent eye infection or injury or other general medical issues. It is especially important to tell your doctor if you have an autoimmune disorder or any sleep problems.
Your eye doctor will then examine your eyelids and eyes. During this exam, you will be asked to look down and close your eyes. If there is a space between your upper and lower eyelids, lagophthalmos is likely present. They may also use a special light test by placing a bright light against your closed eyelids. This allows them to see if any light escapes between your eyelids and check how well your eyelids close.
You may also be asked to blink your eyes. Your doctor may record the speed or slowness of your blinks as well as the force needed to close your eyes. This information is important as it can help determine if an underlying nerve problem exists.
Your eye doctor will shine a bright light in your eyes to perform a slit lamp exam. This exam helps your doctor identify damage to different parts of the eyes. A fluorescein eye stain test, which helps identify damage to the cornea, may also be conducted.
Treatment of lagophthalmos
Treatment for lagophthalmos depends on the underlying cause, how severe it is and how long it has been going on. Although not always necessary, surgery may be recommended if other treatments do not help.
Non-surgical treatment
Lagophthalmos is often treated by targeting the symptoms, such as eye dryness and discomfort. Treatment options may include:
- Lubricating eye drops (artificial tears) to help maintain the tear film
- Topical eye ointment (applied to the cornea as directed) to treat corneal dryness
- Antibiotics to treat infected corneal ulcers associated with lagophthalmos
- Botulinum A injection to induce temporary ptosis (eye drooping)
- Bandage contact lenses to offer protection from the outside environment, as well as hydration and pain relief
- Moisture chamber goggles to help keep the eyes from drying out
SEE RELATED: How to find the best eye drops for your symptoms
Surgical treatment
Surgery may be required if lagophthalmos symptoms do not improve over time. There are various procedures available, from adding weights to the eyelid to helping the eyelids stay closed with sutures.
Weight implantation
Gold or platinum weight implantation involves placing special weights in the upper eyelid. These weights keep the eye closed through gravity and are curved to fit the eyelid. They can be removed if needed.
Gold is typically used because it does not cause reactions with living tissue and does not interfere with MRI screening. However, platinum weights have grown more popular recently, as this material is smaller, thinner and less visible than gold.
Eyelid surgery
Surgically repositioning or tightening the eyelids could improve lagophthalmos. These procedures include surgeries aimed to tighten the eyelids or elevate the lower lid.
LEARN MORE about eyelid surgery.
Tarsorrhaphy
A tarsorrhaphy involves placing sutures in the outer corners of the eyelids. This treatment can be temporary if healing is expected in the short term (over several weeks). It can also be permanent if a longer time frame is needed. Both modes are reversible, even the “permanent” one.
Other surgical options for lagophthalmos
The surgical treatment of lagophthalmos can include procedures that don’t directly involve the eyelid but address complications or underlying causes, such as:
Keratoplasty
A keratoplasty can help address damage to the cornea caused by lagophthalmos.This procedure replaces a damaged cornea with healthy corneal tissue. Keratoplasty may help preserve sight in cases where vision is impaired or worsening.
Facial reanimation
Facial reanimation restores movement to the face. This procedure may be recommended in cases where facial nerve paralysis is the cause of lagophthalmos.
Nerve transfers, muscle transpositions or muscle grafts may also be recommended in these cases. Another option for facial reanimation is free flap surgery. During this procedure, tissue and blood vessels are taken from one part of the body and moved to a different area to help restore function.
Treating nocturnal lagophthalmos
For some people, treating nocturnal lagophthalmos may be as simple as using a fabric sleep mask. Others may need moisture chamber goggles or to tape their eyes shut at night.
Complications
Nocturnal lagophthalmos can have negative effects on sleep. It can also contribute to symptoms of dry eye syndrome — or make existing symptoms worse.
The corneas are exposed in cases of lagophthalmos, as the eyelids cannot fully close to protect the eyes. This can result in scratches (corneal abrasions), tears and ulcers, which are open wounds or sores on the surface of the cornea. Lagophthalmos may also lead to diseases of the cornea, known as keratopathies.
Some surgical procedures can also lead to complications. If your condition requires surgery, consult your eye doctor about the risks and management.
Living with lagophthalmos
Lagophthalmos can be a sign of — or lead to — more complex eye problems. If you experience symptoms, contact your eye doctor for an evaluation. It’s important to do this early so that any serious consequences can be avoided.
Living with lagophthalmos means making sure your eyes are protected and adequately lubricated. Artificial tears, eye ointments and physical coverings like dry eye masks or moisture goggles can be helpful. Eye protection can also include safety equipment, sunglasses and avoiding touching your eyes.
Regular eye exams are important for monitoring the progression of eye conditions and maintaining overall eye health. Comprehensive eye exams should be scheduled at least once a year or as recommended by your eye doctor.
READ NEXT: Eye pain: Causes of pain in, around or behind your eyes and treatment options