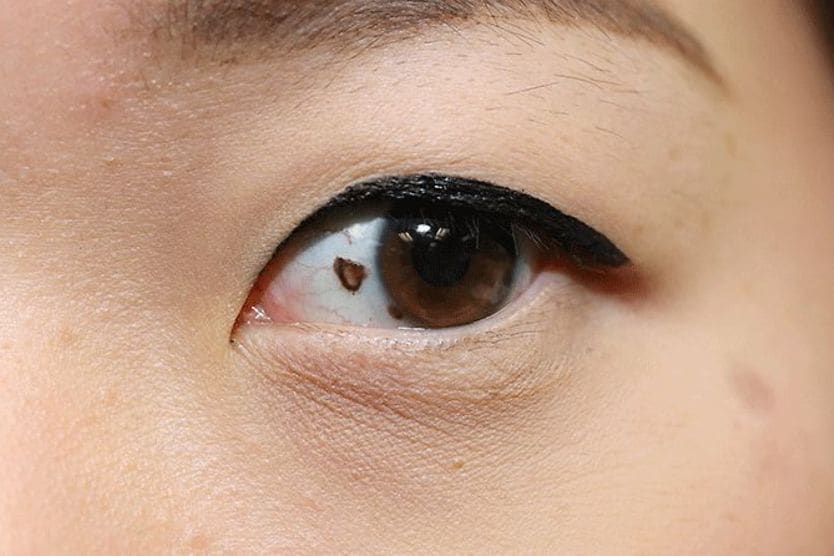
What are Bitot spots?
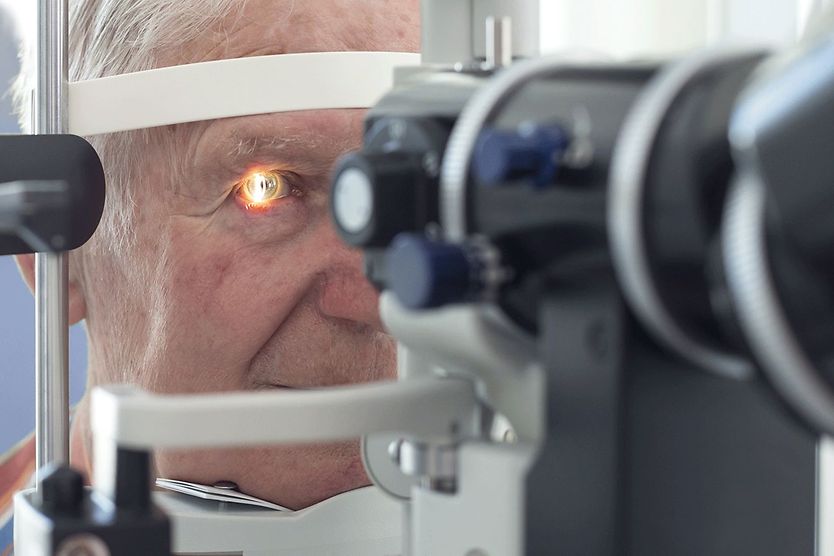
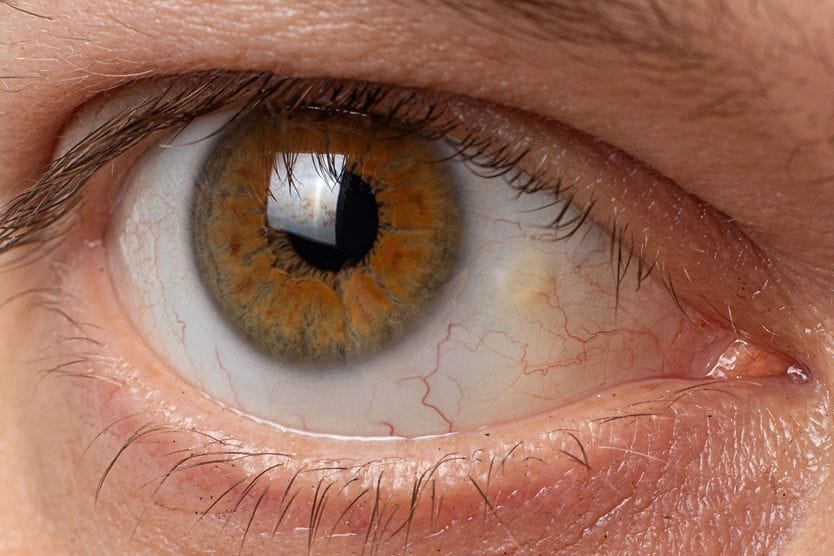
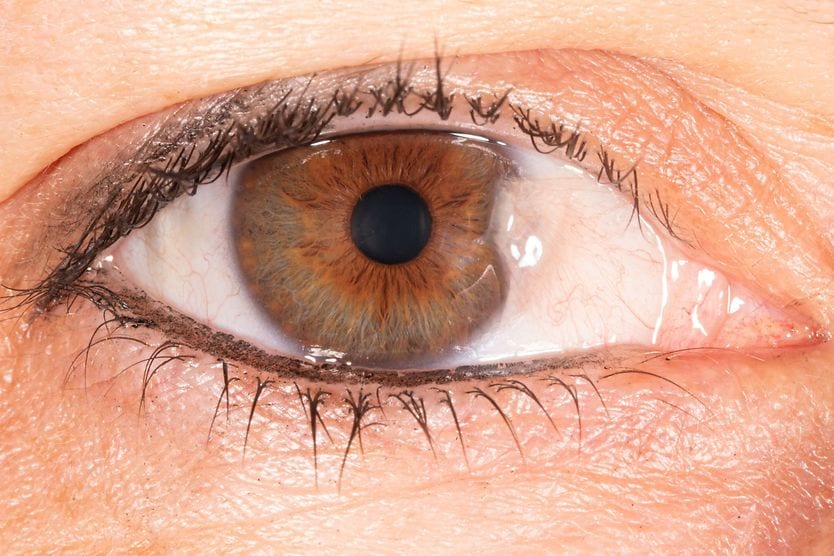
Bitot’s spots (also called Bitot or Bitôt spots) are triangular deposits that can form on the conjunctiva (the thin, clear layer that lines the inside of your eyelids and covers the white part of your eye, called the sclera). They are made up of dried conjunctiva, and often appear foamy and whitish.
Bitot spots are a sign of vitamin A deficiency (VAD), one of the major causes of preventable blindness in young children. They were first described by Pierre Bitôt in 1863.
What causes Bitot spots?
Bitot spots are caused by a lack of vitamin A. VAD is most commonly found in preschool-aged children in developing countries. VAD can affect organs in different parts of the body. When it impacts the eyes, it is called xerophthalmia.
Vitamin A deficiency

[Image credit: "Bitot's spot" by © Murray McGavin. International Centre for Eye Health is licensed under CC BY-NC 2.0 ]
Vitamin A is a fat-soluble vitamin. This means that it can dissolve in fats and is stored in fatty tissue and the liver. It is an antioxidant nutrient important for vision, growth, reproduction and immunity. Vitamin A can be found in foods like spinach, dairy products and liver.
A lack of vitamin A can impede the development of goblet cells in the conjunctiva. Goblet cells are responsible for secreting mucins onto the surface of the eye. Mucins are the proteins that make up mucus, which help lubricate surfaces. This, then, causes the conjunctiva to dry out.
VAD can cause the cells of the conjunctiva to shift their form, a process called metaplasia. It can also cause keratin, a protein found on these cells, to mix with a bacteria called Corynebacterium xerosis. This bacteria releases gasses, causing the foamy surface associated with these spots.
Malnourishment is the main cause of VAD in developing countries. The highest risk is for young children, and pregnant or lactating females. This is because all three populations have a higher nutritional demand.
VAD found in developed countries usually impacts those with gastrointestinal disorders. This is because liver, bowel and pancreatic diseases can prevent the body from absorbing, storing or delivering vitamin A. VAD is also associated with alcohol abuse, as well as strict vegetarian or vegan diets.
Exposure
Bitot’s spots are generally worse in areas of the eye not covered by the eyelids when exposed to the elements (ultraviolet light, wind, smoke and dust). In some cases, Bitot’s spots may appear after prolonged exposure to the elements, even in patients who do not have VAD.
What symptoms appear alongside Bitot spots?
Along with Bitot spots, there are several conditions that are associated with VAD, including:
Night blindness
Night blindness, also called nyctalopia, occurs when a person struggles to see well at night or in dim lighting. It is usually caused by problems in the retina, the retina is the tissue at the back of the eye that contains rods and cones. These are what allow the eyes to adjust to light and see color.
Conjunctival and corneal xerosis
Xerosis is the medical term for dryness. VAD can cause the conjunctiva and cornea to dry out. This is due to the loss of goblet cells and mucin. Conjunctival xerosis may cause the conjunctiva to wrinkle and appear dull. When the cornea (the clear part of the eye covering the pupil and iris) dries out, it will look dull and hazy.
Keratomalacia
In severe cases of VAD, the cornea may soften, a condition called keratomalacia. This can cause infections and ulcers, and even cause the cornea to rupture, which can result in blindness. If keratomalacia develops, it can destroy the cornea in just a few days.
If you suspect you or someone you know has keratomalacia, seek immediate medical attention.
Xerophthalmic fundus
Xerophthalmic fundus refers to small, deep lesions, or damaged areas, that appear on the retina.
Corneal Scarring
Damage to the cornea may cause it to develop scar tissue. The resulting corneal scarring can potentially interfere with vision, depending on its location.
SEE RELATED: Symblepharon
How are Bitot spots diagnosed?
An eye exam is often the first step in diagnosing Bitot spots. An eye doctor may look for signs of symblepharon — when one area of the conjunctiva becomes glued to another area of the conjunctiva. They may also look for conjunctival fibrosis, which occurs when the conjunctiva hardens, thickens or scars.
The eye doctor will likely use one of the following tests to check the surface of the eyes:
- Schirmer's test – This test uses a special strip of paper inserted beneath the lower eyelid to check if the eye is producing enough tears.
- Lissamine green – This is a diagnostic dye that may be applied to the surface of the eye. It will stain dying and damaged cells and mucus, which can help measure the level of dryness on the conjunctiva.
- Rose bengal – This is a dye with a similar application and use as lissamine green. It can help detect disorders on the surface of the eye.
- Impression cytology – This process involves the use of a filter applied to the surface of the eye. The filter will remove the topmost layer of eye tissue so the doctor can analyze it.
The eye doctor will look at the patient’s history to look for signs of malnutrition or lowered vitamin A absorption. They may also perform a blood test to look at levels of vitamin A.
How are Bitot spots treated?
Bitot spots can typically be treated with high doses of vitamin A, which can be given as an oral medication (taken by mouth) or as an intramuscular injection. The dose of vitamin A is determined by the patient’s age and specific symptoms. Bitot spots often improve within two weeks of vitamin A treatment.
When should you see a doctor?
If you notice gray or silvery patches when you look at your eyes, reach out to your eye doctor. It is important to test your ability to see in dim light since night blindness often develops before the appearance of Bitot spots. Both may be signs that you have vitamin A deficiency.
If you have a history of malnutrition, alcohol abuse or a gastrointestinal disorder, be sure to work with a doctor to address a possible lack of vitamin A.