Phakic IOLs (implantable lenses)

Phakic intraocular lens (phakic IOL or pIOL) implants are an alternative to LASIK and PRK eye surgery for correcting moderate to severe myopia (nearsightedness). In some cases, phakic IOLs produce better and more predictable vision outcomes than laser refractive surgery.
Phakic IOLs are clear implantable lenses that are surgically placed either directly in front of the iris (the colored portion of your eye) or just behind it, without removing your eye’s natural lens. Phakic lenses enable light to focus properly on the retina for clearer vision without corrective eyewear.
Implantable lenses function like contact lenses to correct nearsightedness. The difference is that phakic IOLs work from within your eye instead of sitting on the surface of your eye.
Also, phakic IOLs offer a permanent correction of myopia, unless the lens is surgically removed.
Unlike contact lenses, you can't feel a phakic intraocular lens in your eye and, apart from regular eye exams, phakic IOLs typically do not require any maintenance.
Phakic IOL types
Two FDA-approved phakic IOLs are currently available in the United States to correct moderate to severe nearsightedness.
Visian ICL
The Visian ICL (Implantable Collamer Lens) marketed by Staar Surgical is a posterior chamber phakic IOL, meaning it is positioned behind the iris and in front of your natural lens. The Visian ICL is approved for correcting nearsightedness ranging from -3.00 to -20.00 D.
Because the Visian ICL is placed behind the iris, it is undetectable to the naked eye and can only be seen through a microscope.
The Visian ICL is made of a soft, biocompatible collagen copolymer. Due to its flexibility, the lens can be folded during implantation, requiring only a small surgical incision.
Verisyse
The Verisyse (Johnson & Johnson Vision) is an anterior chamber phakic IOL, meaning it is positioned in front of the iris. The Verisyse phakic IOL is approved for correcting nearsightedness within the range of -5.00 to -20.00 diopters (D).
The Verisyse lens is made of medical-grade plastic (polymethyl methacrylate, or PMMA) and is rigid in form. In Europe, it is approved and marketed under the trade name Artisan.
Verisyse phakic IOLs typically aren't noticeable in the eye, though you may see the lens if you look closely in the mirror.

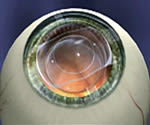
The Visian ICL (Implantable Collamer Lens).
Phakic IOLs vs. LASIK eye surgery
LASIK currently is the most popular type of refractive surgery in the United States. It is safe and effective, and technology advances such as custom LASIK and bladeless LASIK have made visual outcomes even better.
But not everyone is a good candidate for LASIK surgery. Potential reasons for not being a good LASIK candidate include:
Having too much nearsightedness, farsightedness or astigmatism
Having an unusually thin or irregularly shaped cornea
Having eye conditions such as keratoconus or dry eye syndrome
People with moderate to severe nearsightedness may be better suited for phakic IOLs than LASIK surgery. For many people who are outside the treatment range of LASIK, phakic IOLs can produce excellent results.
One study that evaluated LASIK versus phakic IOL surgery for the correction of -6.00 to -20.00 D of myopia revealed that the two procedures produced essentially equal odds of attaining 20/20 vision without corrective lenses one year after surgery.
The study also found that patients who underwent phakic IOL implantation had better contrast sensitivity and were more satisfied with their outcome than LASIK patients. Neither technique caused significant complications that permanently affected vision.
"Our findings suggest phakic IOLs are safer than excimer laser surgery [LASIK or PRK] for correcting moderate to high levels of short-sightedness," said study author Allon Barsam, an ophthalmologist at Moorfields Eye Hospital in London.
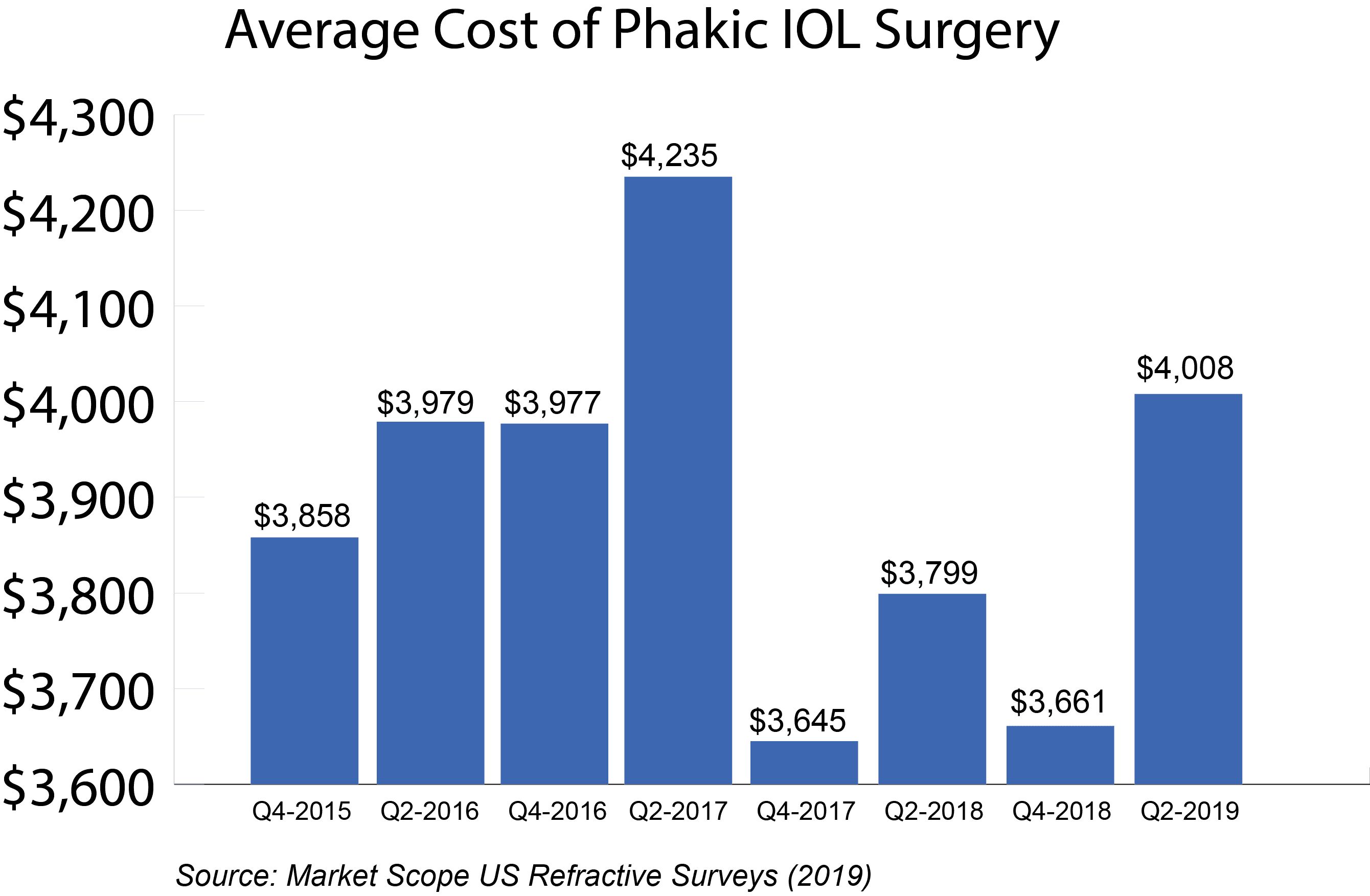
The cost of phakic IOLs also should be taken into consideration; implantable lenses typically are somewhat higher than the cost of LASIK.
If your surgeon recommends a phakic IOL over LASIK, it may be prudent to not let the cost cloud your decision to follow your surgeon's advice.
After a thorough eye exam and health evaluation, your eye surgeon will advise on the best type of surgery for you.
What to consider
Are you a candidate for phakic IOLs?
Not all patients are candidates for phakic intraocular lens implantation, just like not all patients are candidates for LASIK.
Some questions to help determine whether phakic IOLs are right for you include:
Is your myopia within the range for which the phakic IOL has been approved (up to -20.00 D)?
Have you had a comprehensive eye exam and surgical consultation to determine that your eye can safely accommodate an implantable lens?
Are you between the ages of 21 and 40? Even if you are outside this age range, you may still be a candidate for phakic IOLs and should discuss it with your eye surgeon.
Has your eyeglass or contact lens prescription changed in the past year? For vision correction surgeries, you must have had stable vision for at least a year.
Are your eyes healthy? Conditions such as cataracts, glaucoma, and untreated eye infections generally will prevent you from having phakic IOL surgery.
Are you in good health? Certain degenerative or autoimmune diseases such as Sjogren's syndrome, rheumatoid arthritis, type 1 diabetes, HIV and AIDS, as well as certain medications such as steroids and immunosuppressants, may interfere with healing and final outcomes.
Will the cost of phakic IOLs — from pre-screening to ongoing regular check-ups — be covered by your vision insurance?
Phakic IOLs: What to expect
Before. If you wear contact lenses, you should stop wearing them at least one week before your preoperative eye exam and/or consultation. Contacts can alter the shape of your cornea and therefore make your refractive error reading less accurate.
A week or two before your phakic IOL surgery, your eye surgeon may perform a laser iridotomy on each eye to prepare your eye for lens implantation. An iridotomy creates a small opening at the outer edge of your iris, allowing fluid to circulate and helps to prevent a possible increase of intraocular pressure after phakic IOL surgery.

Insertion of the Verisyse phakic IOL.
The iridotomy procedure typically is performed in-office and is relatively quick, taking only a few minutes for each eye. It is important that you follow your surgeon's instructions after the procedure to minimize any possible complications.
Some surgeons have incorporated the iridotomy procedure on the same day as the phakic IOL surgery.
During. Numbing eye drops are first applied to your eye to alleviate any discomfort during the procedure. Your doctor may also give you some medication to help you relax.
An instrument called a lid speculum is used to keep your eyelids open and a tiny incision is made in the cornea. The incision length for a Verisyse lens is around 6 mm; the Visian ICL incision is as little as 3.2 mm due to the flexible and foldable material of the lens.
With the Verisyse, the lens is attached to the front of the iris. Tiny dissolvable stitches often are used to close the wound and an eye shield is placed over your eye.
The Visian ICL is positioned in the posterior chamber of the eye behind the iris and pupil and in front of your natural lens. Once inserted, the artificial lens unfolds to its full width and typically does not require any stitches. An eye shield is then placed over your eye and needs to be worn for a day or two after the procedure.
The phakic IOL procedure typically takes 10 to 30 minutes and is performed on an outpatient basis, although you will need to have someone drive you home after surgery. Your doctor will prescribe antibiotic and anti-inflammatory drops for you to use at home.
After. Most people notice improved vision immediately following the phakic IOL procedure, but vision may be hazy or blurry with an increased sensitivity to light for the first few days. For some people, it can take two to four weeks for their vision to stabilize.
Vision with the Visian ICL tends to stabilize in about one to seven days, which can be quicker than with the Verisyse lens.
There typically is minimal discomfort after phakic IOL surgery, but you may have a mild scratching sensation, like something is in your eye. If required, your doctor can prescribe medication to make you more comfortable during the first few days following surgery.
You will need to return for a follow-up visit with your doctor the next day. It's essential that you follow your eye surgeon's post-operative instructions carefully and attend frequent check-ups to help avoid any complications.
Refrain from rubbing or squeezing your eye, lifting heavy objects and participating in strenuous activities until your eye has completely healed, which could take several weeks.
Most people can return to work and resume driving within a couple of days, after their eye doctor checks their vision and approves.
Phakic IOL Vision Outcomes
In a study of three-year outcomes of the FDA clinical trial of the Verisyse lens, 84% of patients achieved uncorrected vision of 20/40 or better, which is the legal limit for driving without prescription eyewear in most states. And 31% achieved uncorrected vision of 20/20 or better.
In FDA trials of the posterior chamber Visian ICL, 81% of patients achieved uncorrected visual acuity of 20/40 or better. Forty-one percent attained uncorrected vision of 20/20 or better.
Patient satisfaction with the quality of vision with both types of phakic IOLs was generally high.
Some patients, particularly those with very severe myopia, elect to undergo LASIK as a follow-up to further improve vision after phakic IOL surgery.
Phakic IOLs are an effective option for people with moderate to severe nearsightedness who fall outside the treatment range of LASIK. When considering implantable lenses — or any refractive surgery — be sure to discuss all the benefits and risks with your eye surgeon.
Aimee Rodrigues also contributed to this article.
Page published on Wednesday, February 27, 2019






