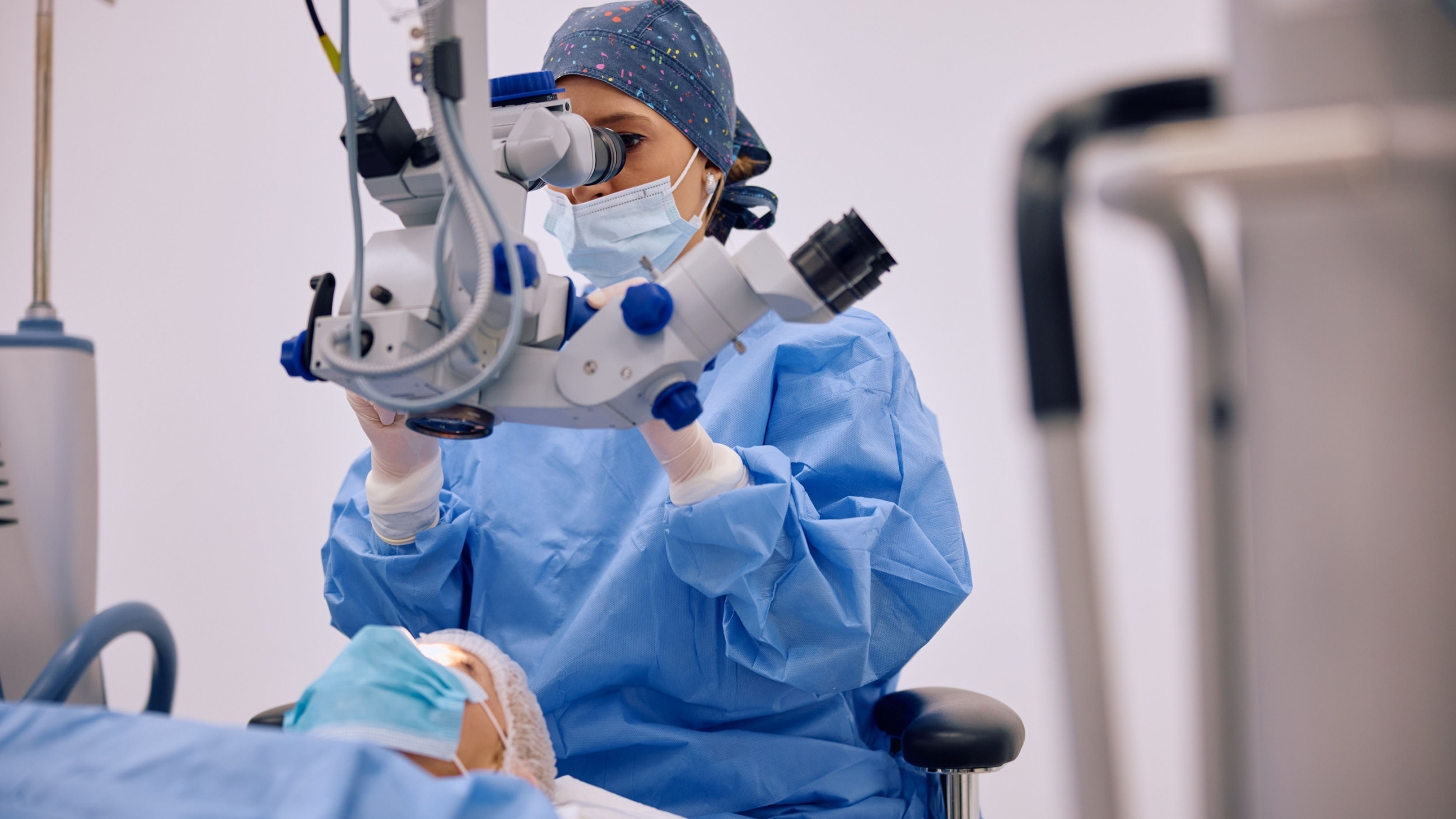
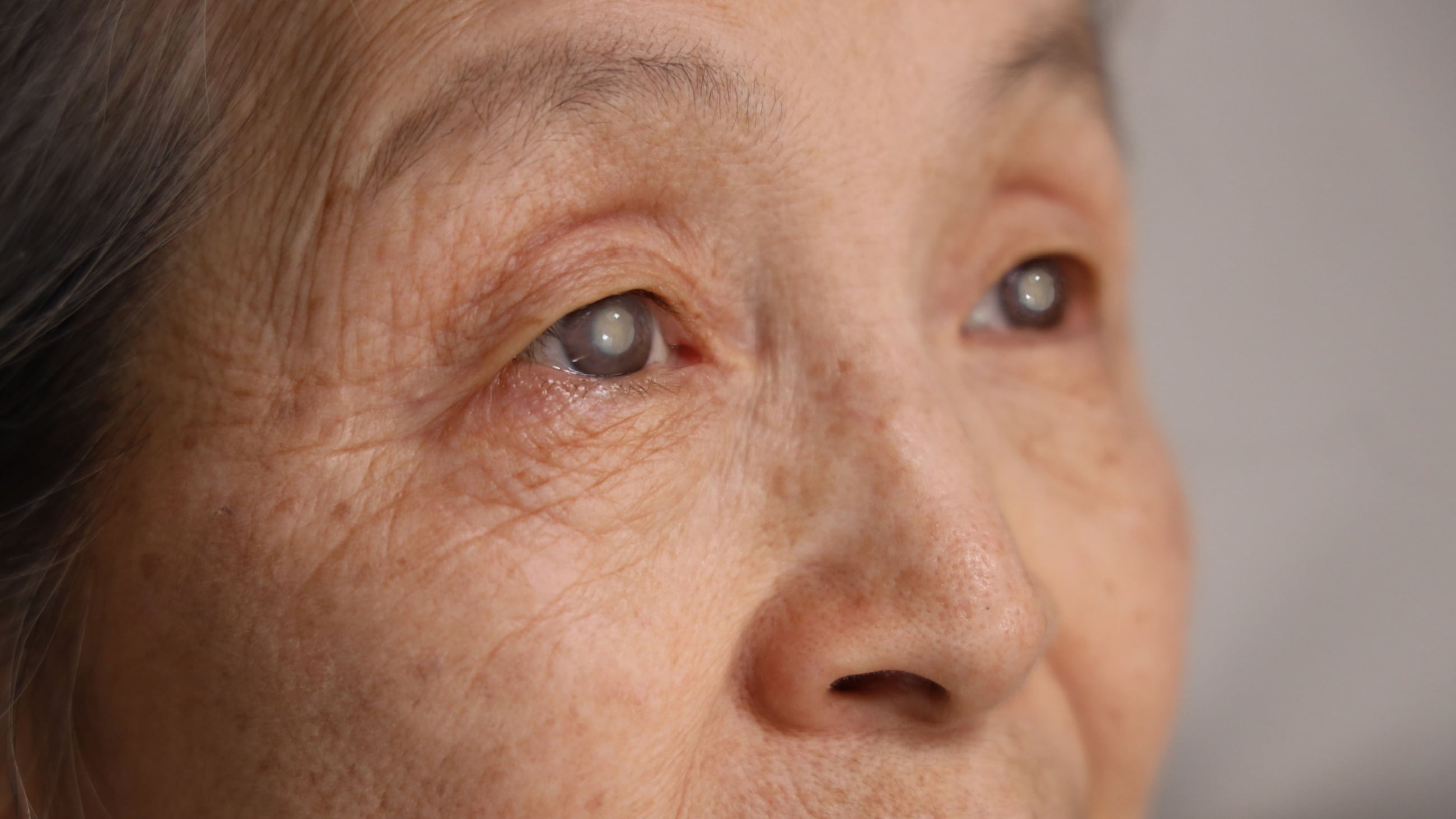
What is cataract surgery?
Cataract surgery is a procedure that helps manage vision problems caused by a cataract. During surgery, the cloudy lens inside your eye will be replaced with a clear artificial lens. It's an outpatient procedure, which means you can usually go home the same day.
Surgery is the only way to treat a cataract.
It might sound overwhelming at first, but cataract removal surgery is a safe common procedure. You typically won't feel any pain during the procedure, and it usually only takes 10 to 15 minutes.
You're more likely to need treatment for cataracts as you get older. That's when the majority of cataracts develop or get worse.
A cataract diagnosis doesn't always mean you need surgery right away. Many people decide to wait until their vision problems get worse, while others prefer to be more proactive with treatment.

According to the experts, cataracts affect:
- About 1 in 20 people aged 50 to 54
- Around half of people aged 75 to 79
- More than 2 in 3 people aged 80 or older
Millions of people in the United States have cataracts removed every year. About 97% of people who have surgery will see more clearly after their procedure.
How is cataract surgery done?
Cataract treatment involves removing your cloudy natural lens and replacing it with a clear artificial one.
The new lens is called an intraocular lens, or IOL. The IOL helps restore the clear vision you had before your cataract developed.
An eye surgeon called an ophthalmologist will perform your cataract surgery procedure.
During an average surgery, the ophthalmologist will:
- Place numbing eye drops in your eye so you don't feel pain. They may also give you medicine to help you relax.
- Make painless, small incisions along the sides of your cornea (the clear part of your eye).
- Use an ultrasound or laser to carefully break up the cloudy lens into small pieces.
- Gently remove the lens pieces from the eye.
- Place an artificial lens in the spot where your natural lens used to be.
- Close any incisions.
The incisions tend do heal on their own without stitches. A protective shield or patch will be placed over your eye to keep it safe until your follow-up exam (usually the next day).
If you need cataract treatment in both eyes, your surgeon will probably wait one or two weeks between procedures. That gives your first eye a chance to heal. But in some circumstances, both eyes can be treated on the same day.
LEARN MORE: Congenital cataracts: Types, causes and treatment
Types of cataract surgery
Eye doctors can use different types of cataract surgery to help their patients see better.
Traditional or conventional cataract surgery
In the U.S., traditional or conventional cataract surgery uses phacoemulsification, or "phaco" for short, to perform the standard procedure. in the U.S. is called phacoemulsification, or "phaco" for short.
Phacoemulsification involves ultrasound waves to break up the cloudy lens and remove it.
Laser cataract surgery
Laser cataract surgery uses newer technology. During the procedure, the eye doctor uses a femtosecond laser to make incisions, soften the hardened cataract, then break up the cataract into small pieces.
Laser surgery for cataracts is usually more expensive and may not be covered by insurance. Your eye doctor can help you decide which surgery options are appropriate for you.
SEE RELATED: How monovision cataract surgery can help people with presbyopia