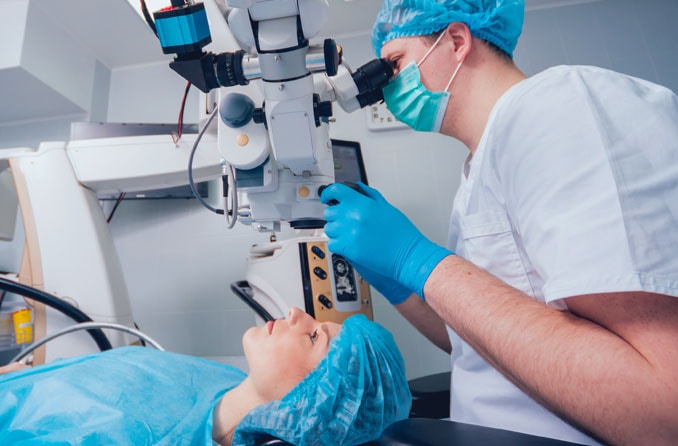
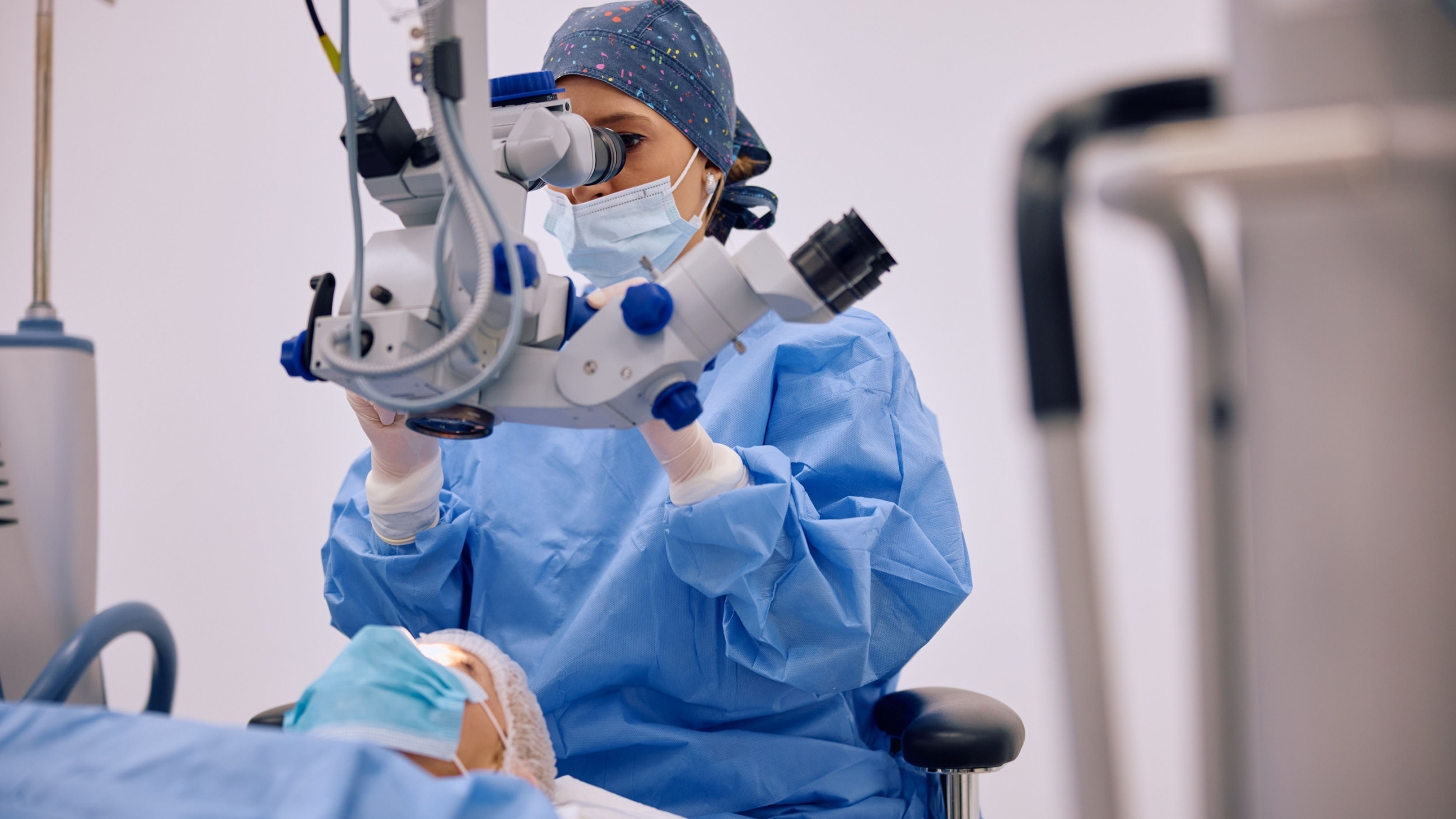
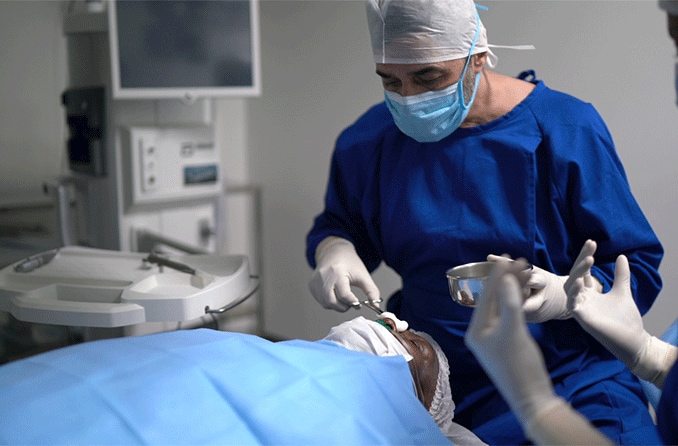
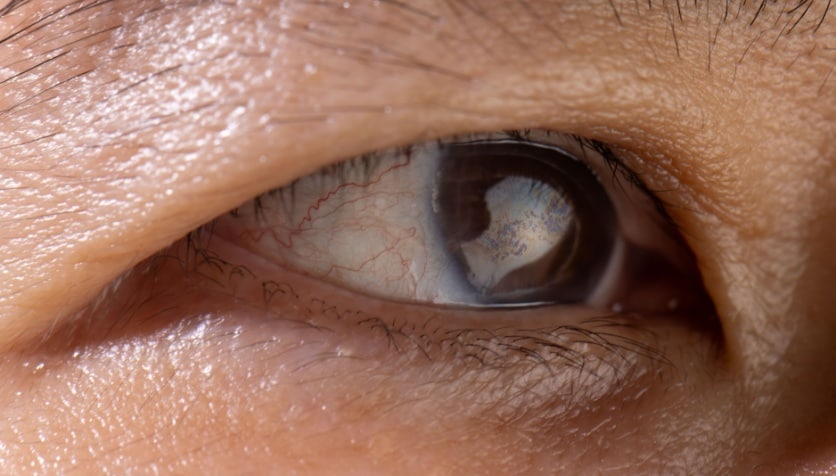
What is laser cataract surgery?
During laser cataract surgery, the surgeon uses a laser to help with certain parts of a cataract removal procedure. The computer-guided laser replaces some of the handheld tools used in traditional surgery. It's also known as laser-assisted cataract surgery.
The laser can also treat lower degrees of astigmatism at the same time as cataracts.
Studies have shown that laser surgery may reduce the risk of complications in some people but not everyone. Laser and traditional cataract surgery appear to be equally safe for people with normal eye health.
How lasers are used
Your surgeon may use a laser to:
- Create a 3D image scan of your eye
- Make small incisions in the front of your eye
- Open the thin pouch that holds your cloudy lens
- Soften your cloudy lens before they break it into small pieces
- Make other incisions to treat some degrees of astigmatism
Astigmatism is a common problem with how the clear "window" of your eye (the cornea) is shaped. It can cause blurry vision, eye strain and problems seeing at night.
It isn't always possible to treat astigmatism during laser cataract surgery. Your doctor can give you more information during your consultation appointment.
Benefits of laser cataract surgery
Cataract surgery is safe and effective, even when lasers aren't involved. It's one of the safest procedures in use today.
In certain situations, cataract laser surgery can have benefits like:
- It allows the surgeon to treat mild astigmatism with tiny incisions during the same procedure.
- It can help the surgeon insert a premium lens for astigmatism (toric) or presbyopia (multifocal).
- Certain parts of the procedure take less time to finish.
- It can improve results for some people whose eyes are harder to operate on.
- It can reduce risk for people who have problems with endothelial cells in their cornea (including Fuchs' dystrophy).
Laser surgery doesn't have benefits for everyone.
In a recent study, both laser-assisted and traditional cataract surgeries produced similar long-term results in terms of vision improvement, surgical success, complication rates and patient satisfaction.
You may also need to pay several thousand dollars out of pocket if it isn't covered by your health insurance.
Your eye doctor can talk to you about the pros and cons of each type of surgery. This should help you decide whether it's worth any extra costs.
Cost
Insurance providers rarely cover laser surgery for cataracts, so you can expect to pay more than you would for a traditional procedure.
Laser cataract surgery can cost several thousand dollars for each eye if it isn't covered by your health insurance (or if you don't have insurance). This is one of its biggest disadvantages for the time being.
Your final out-of-pocket cost will depend on insurance coverage, doctor fees, facility fees and other factors.
Medicare may cover laser surgery for cataracts in some cases. But it will not cover:
- A premium artificial lens (if selected)
- The part of surgery used to help astigmatism (if selected)
Preparing for surgery
You'll need to schedule a comprehensive eye exam with your eye doctor sometime before surgery. During the exam, the doctor will do certain tests to check your eye health and help you pick an artificial lens.
In the time between your appointment and your procedure, your surgeon may ask you to:
- Start using medicated eye drops
- Stop taking certain medicines
- Avoid eating at least six hours before the procedure
The day of surgery
The surgery itself usually takes 15 to 30 minutes, but you'll be at the facility longer. Your surgeon will talk to you about your specific procedure beforehand.
Someone will need to drive you home after surgery.
During your procedure, the surgeon will generally follow these steps:
1. Scan your eye
They use a machine to make a detailed map of your eye. Not only does this give your surgeon important information, it also serves as a guide for the laser during the next step.
2. Dilate and numb your eye
Your doctor will use dilating eye drops to make your pupil bigger. They'll use different eye drops to numb your eye so you don't feel pain.
They may also give you medicine through an IV to help you relax.
3. Make incisions and soften the lens
A laser creates small incisions along the surface of your eye. It can also be used to correct astigmatism at the same time.
Inside your eye, the laser is used to make an opening in the lens capsule, the thin layer of tissue around your lens. This helps the surgeon access your cloudy lens.
4. Break up and remove the cloudy lens
During traditional surgery, ultrasound energy is used to break up the natural lens. Lasers let the surgeon soften the cloudy lens before they break it up with ultrasound.
A softer lens means they don't need as much ultrasound power as they normally would, which may be safer for people with harder cataracts.
The lens pieces are then carefully removed with a probe using ultrasound.
5. Insert the clear artificial lens
The surgeon inserts the new lens into your eye. A standard monofocal lens will help you see at one distance, while a premium lens can sharpen your eyesight at multiple distances.
READ MORE: The many different types of artificial lenses
Recovery
Your eye should be healed within three months of laser cataract surgery, but your vision will recover much sooner.
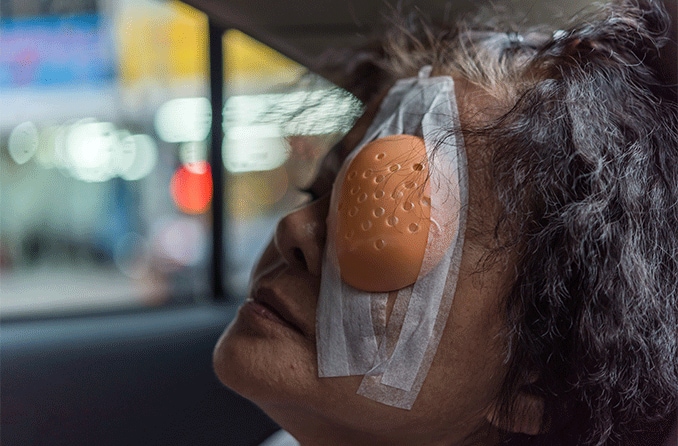
You may need to temporarily wear an eye patch to protect your eye while it heals.
Recovery time can vary from patient to patient. Some people can see better almost right away after surgery. It's also normal to have blurry vision for a day or two.
In some cases, it can take a week or two for things to look normal again.
Other side effects
Normal side effects can also include:
- Dry eye
- Eye redness or a small red spot on your eye
- Increased glare or halos around bright lights
- Sensitivity to light
- A feeling that something is stuck in your eye
Complications are rare, but they can happen. You can reduce your risk by carefully following your doctor's instructions and using any prescribed eye drops as directed.
Tell your doctor right away if you experience any unexpected or severe symptoms.
Things to avoid
Your doctor may tell you to avoid certain activities for a little while. These can include:
- Driving
- Swimming
- Exercising
- Bending over or lifting heavy things
- Wearing makeup around your eyes
Schedule an appointment
Laser cataract surgery uses advanced equipment, but it may not make the most sense for you. Fortunately, traditional and laser surgery are both safe and effective.
A cataract surgeon can examine your eyes and help you make the most informed decision. Find an eye doctor near you and schedule an appointment to learn more.