What is a stye (sty)?
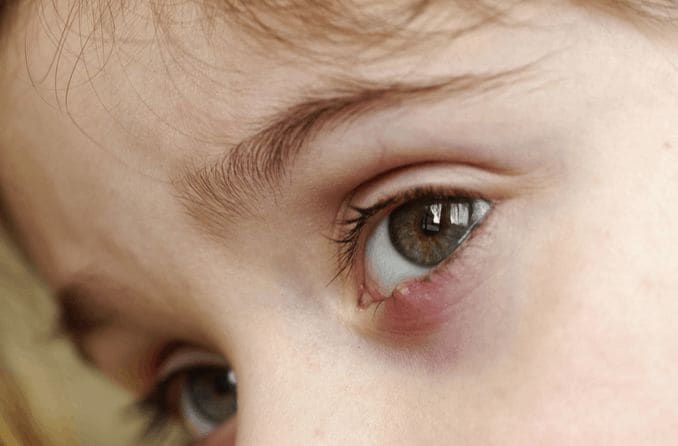
A stye, or hordeolum, is a common, painful, pimple-like bump on the eyelid usually caused by an infection of an oil gland in or near the lashes. Although a stye can be painful, it is rarely serious. It usually heals on its own with warm compresses and good eyelid hygiene.
Styes are usually caused by a bacterial infection, mainly Staphylococcus aureus. These bacteria commonly live on the skin but can sometimes invade the eyelid glands, resulting in a stye.
Risk factors for styes include:
- Insufficient eyelid cleansing
- Chronic blepharitis (eyelid inflammation)
- Weakened immune system
- Diabetes
- Not cleaning contact lenses properly or wearing them longer than prescribed
- Certain skin conditions
Styes can occur in people of any age. Most styes develop fairly quickly and typically go away within about a week. Some last only a few days. Pus may build up inside the stye, but it often drains on its own or with the help of warm compresses, relieving pain and promoting healing.
Types of styes
There are two main types of styes, classified by where they occur on the eyelid:
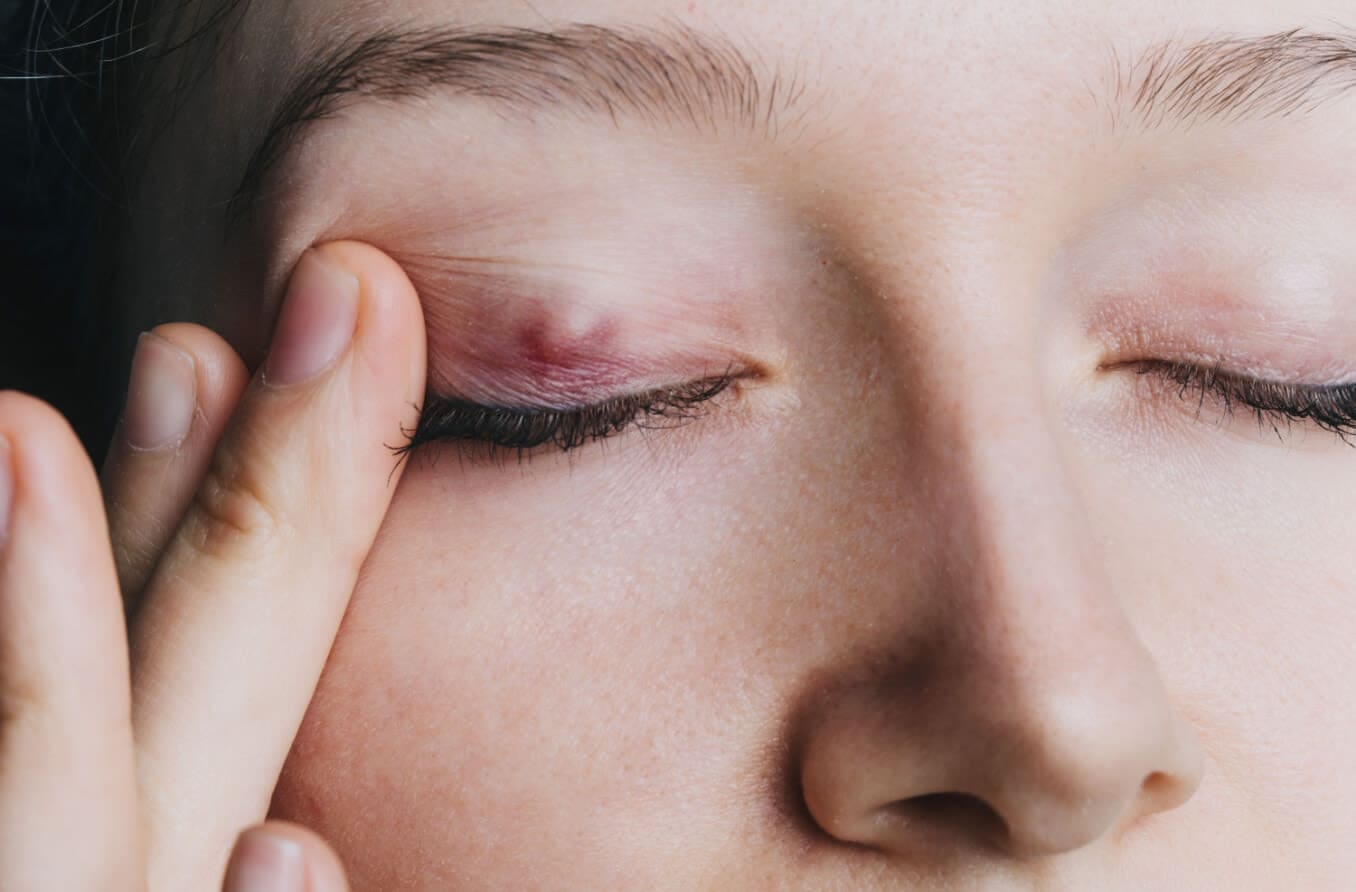
External stye
This is the more common type of stye. An external stye (hordeolum):
- Forms on the outer edge of the eyelid and is directed outward.
- Resembles a small pimple.
- Usually heals within 1 to 2 weeks with home treatment such as warm compresses and eyelid scrubs.
- Develops from an infection of the glands at the base of the eyelash follicle. These are called the glands of Zeis or Moll.
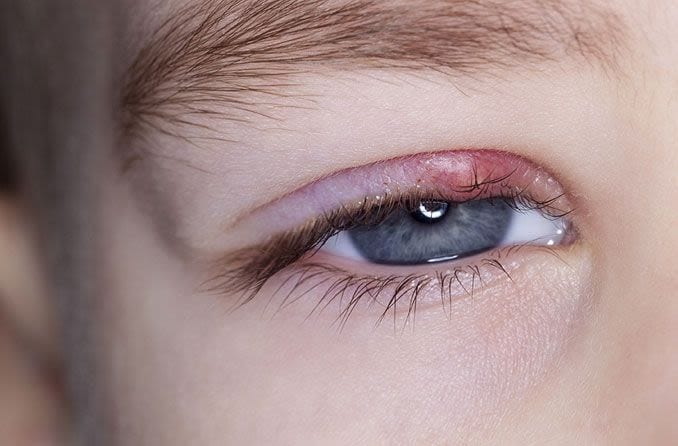
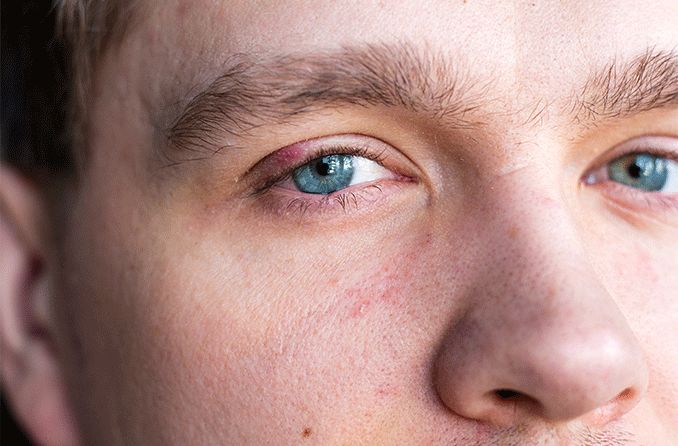
Internal stye
This is the less common type of stye. An internal stye (hordeolum):
- Forms on the inner surface of the eyelid, directed inward toward the eyeball.
- Looks like a small whitish or yellowish bump.
- May cause more pain or take longer to heal than an external hordeolum.
- Develops from an infection of deeper oil glands, called meibomian glands. These are located inside the firm part of the eyelid (the tarsal plate).
Are styes common?
Styes are very common and can affect anyone, regardless of age. Most people will likely get a stye at some point in their life. Much like pimples on the skin, styes form when a small oil-producing gland becomes blocked and infected with bacteria.
Since they rarely lead to serious issues or vision problems, styes are considered minor annoyances that usually go away on their own.
Are styes contagious?
Styes are usually not contagious, so you don't have to worry about spreading the infection through casual contact. It's generally okay to go to work or school while you have a stye.
However, the bacteria that cause the infection — often Staphylococcus aureus — can spread from the bump. The pus can carry some bacteria. To minimize the spread of germs, discontinue contact lens use and avoid sharing personal items like washcloths, towels and eye makeup.
You can get multiple styes at the same time, affecting one or both eyelids. A stye typically affects only one eye. However, because the lower lid has 20 to 25 meibomian glands and the upper eyelid has 40 to 50, it's possible to have more than one at a time and on both eyes.
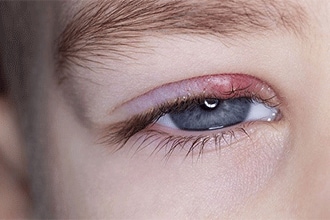
What are the signs and symptoms of a stye?
If you notice a sore, pimple-like bump along the edge of the eyelid with the following signs and symptoms, you may have a stye:
Signs:
- The bump appears to have a pus-filled center.
- The surrounding area is inflamed and sensitive, with possible swelling of the entire eyelid.
- There is discharge or yellowish crust on the eyelid edge.
Symptoms may include:
- Pain and discomfort
- A scratchy sensation, as if something is in the eye
- Increased sensitivity to light (photophobia)
- Tearing (watery eyes)
- Redness
A stye can be located near the eyelashes (external) or deeper inside the eyelid (internal). While the bump may start small, the whole eyelid can swell. If the swelling is severe, it can affect your vision or the movement of your eyelid. Although both types can cause discomfort and other symptoms, internal styes tend to be more painful than external.
How can you tell if it's a stye or a chalazion?
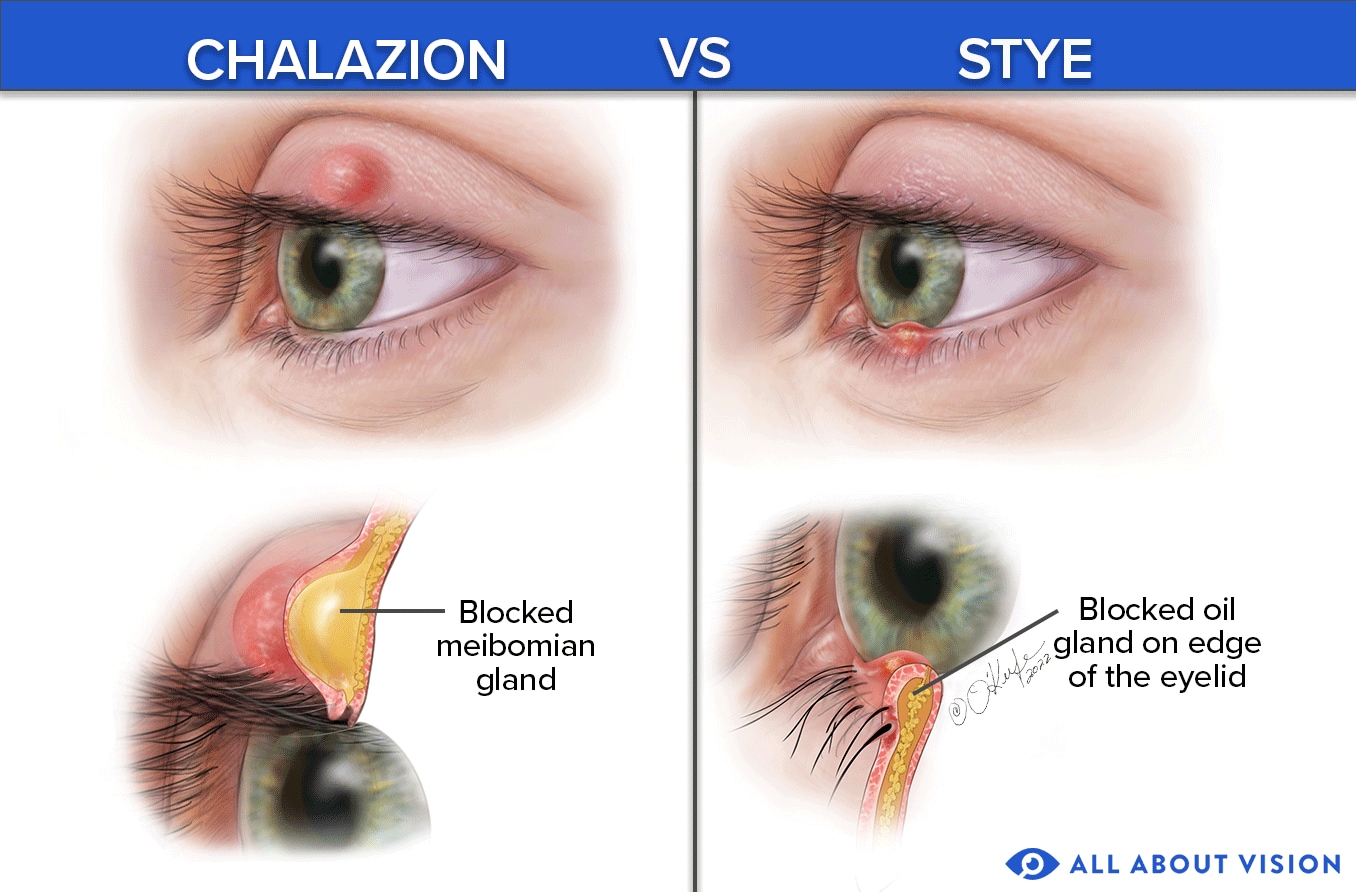
Illustrated by Laurie O'Keefe
Because both cause eyelid swelling, it can be difficult to distinguish between a stye (hordeolum) and a chalazion, also known as a tarsal cyst. However, there are differences that can help distinguish between these conditions.
Doctors tell them apart by:
- How quickly the swelling developed
- How painful it is
- The location and appearance of the bump
A stye and a chalazion have different underlying causes:
- Stye – Caused by a bacterial (often Staphylococcus) infection of an oil gland at the base of the eyelashes.
- Chalazion – Caused by a chronic, non-infectious inflammation due to trapped oil in the meibomian gland.
The underlying causes of these conditions also result in different signs and symptoms:
- Stye – Develops rapidly along the eyelash line, causes pain and tenderness, and resembles a pus-filled pimple.
- Chalazion – Develops slowly and is usually farther from the eyelid edge. It feels like a firm bump deeper in the eyelid tissue. It usually doesn't hurt when touched.
The best way to differentiate between these conditions is to understand how each type forms.
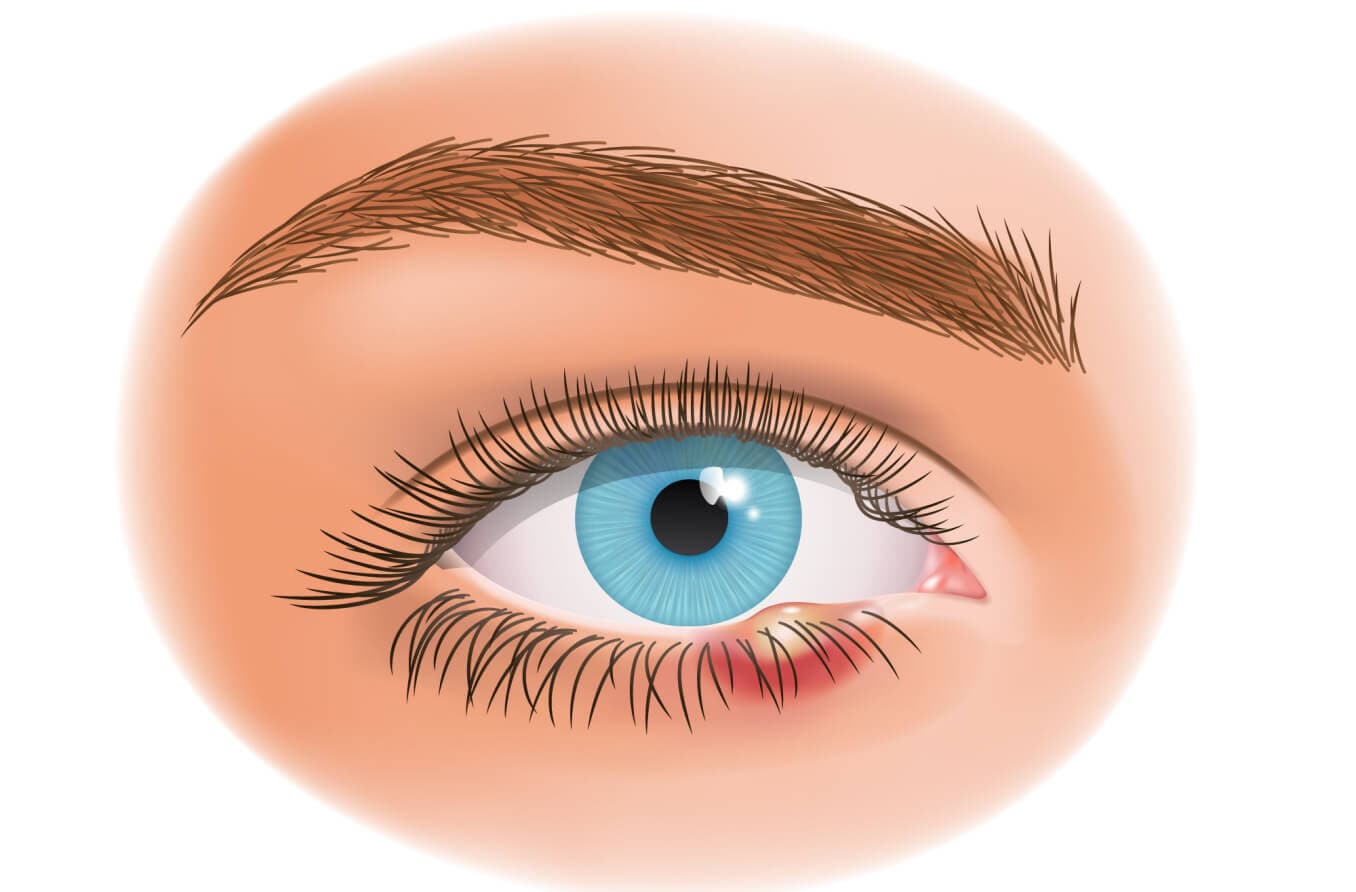
How an external stye forms:
- Bacteria, often Staphylococcus, infect the glands at the base of the eyelashes (glands of Zeis or Moll).
- The infection causes inflammation and the formation of pus at the site.
- A small pimple-like and painful red bump develops at the edge of the eyelid.
How an internal stye forms:
- Bacteria, often Staphylococcus, infect a meibomian gland inside the eyelid (the firm tarsal plate).
- This infection causes blockage and inflammation of the gland, leading to the buildup of pus within the eyelid.
- The swelling and infection cause pain, tenderness and redness on the inside surface of the lid.
How a chalazion forms:
- Meibum glands release an oily substance, called meibum, that keeps the eye surface moistened.
- When the gland’s opening becomes blocked, meibum begins to build up within it.
- The accumulation of the trapped meibum causes the gland and surrounding tissues to swell.
- Redness, sensitivity and irritation develop as the chalazion forms, but discomfort improves after a few days
- As it grows, the chalazion becomes a painless, firm bump under the eyelid skin
If a chalazion gets very large, it may change the shape of the eyeball, causing slight blurriness. Some small chalazia go away on their own, while others can last for weeks or months. People with a history of styes, chronic eyelid inflammation (blepharitis) or skin conditions like acne rosacea are more likely to get a chalazion.
What causes an internal stye vs. a chalazion if both involve the meibomian glands?
An internal stye and chalazion both affect meibomian glands, but a chalazion is due to blockage and inflammation of a meibomian gland. An internal stye is an infection of the meibomian gland.
Can an internal stye develop into a chalazion?
A stye usually forms over a few days when one of the eyelid glands gets blocked, allowing bacteria to grow and cause a painful, swollen bump filled with pus. Most styes heal after they drain on their own or with simple home care, such as warm compresses.
If a stye does not clear up or keeps coming back, it may turn into a longer-lasting, non-infectious bump in the eyelid — a chalazion.
What causes styes?
Most styes develop from a staph infection. These bacteria are found on our skin, especially on the eyelids and around the nose. While usually harmless, they can cause infections if they enter the skin or glands of the eyelid.
Styes form when tiny oil glands along the eyelid get blocked, allowing bacteria to grow. These glands produce oil to prevent tears from evaporating too quickly, keeping the eyes moist. When the ducts are blocked by oil, debris or dead skin, bacteria multiply.
As the infection develops and spreads, the area becomes swollen and a central point of pus becomes visible. External styes affect hair follicles or glands near eyelashes, while internal styes occur deeper in the meibomian glands.
Certain habits can increase the risk of styes:
- Touching or rubbing the eyes with dirty hands
- Not washing hands before handling contact lenses
- Using contaminated or expired eye makeup
- Not replacing mascara and similar products regularly (experts recommend replacement every 2 to 6 months to reduce bacterial growth)
Who is most at risk for styes?
Anyone can get a stye, but certain conditions and habits increase the risk. Factors that increase the chance of developing a hordeolum include:
- History of styes – If you've had a stye or chalazion before, you're more likely to get another.
- Chronic eyelid inflammation – Conditions like blepharitis raise the risk of styes.
- Dry eyes – Styes are more likely if you have dry eyes.
- Improper contact lens care – Not cleaning lenses properly or wearing them overnight can introduce bacteria into and near the eyes.
- Poor eyelid hygiene – Not cleaning the eyelid margins daily allows bacteria and debris to build up, blocking glands.
- Skin conditions – People with rosacea or seborrheic dermatitis are more likely to develop styes.
- Systemic conditions – Issues like diabetes can weaken the immune system, making infections more likely. High cholesterol may also play a role.
- Age – Styes can affect anyone, but they are most common in school-aged children and adults aged 30 to 50.
- Other triggers – Hormonal changes, chronic dry eye, and stress or fatigue can weaken the immune system, increasing the risk.
How do you treat a stye at home?
Most styes are not serious. They usually disappear within 1 to 2 weeks. While they often resolve on their own, simple self-care techniques can help. These methods can ease discomfort, reduce swelling and speed up recovery. Home treatment mainly involves warmth and gentle cleansing.
The following home treatments can help you get rid of a stye. These remedies promote drainage of the affected gland. If the stye is not improving after a week or so, consult an eye doctor.
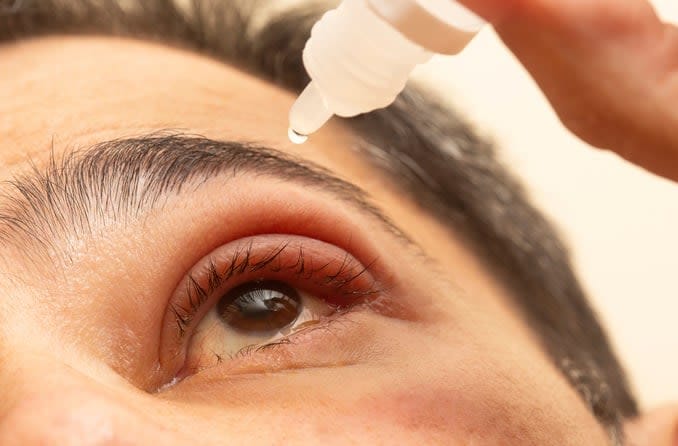
Use a warm compress
Applying warmth to the affected eye is the key step in home treatment. Heat softens the blockage in the oil gland, encouraging the stye to drain. This relieves pressure and speeds the healing process.
To create a warm compress:
- Wet a clean, soft cloth with warm water. Ensure the water is warm but not too hot. This will help avoid burning your delicate eyelid skin.
- Squeeze out excess water and place the cloth over your closed eyelid.
- Do this for about 15 minutes. If the cloth cools, resoak it in warm water to maintain heat. Repeat this about four times throughout the day.
Clean your eyelid
Keeping the eyelid clean plays an important role in fighting the existing infection and preventing future ones. Gentle eyelid cleaning helps remove debris, oils and bacteria that block glands.
You can make a gentle wash using mild soap such as watered-down baby shampoo mixed with warm water. Baby shampoo is mild and less likely to irritate the eyes. Use a clean cotton swab or fingertip dipped in this solution to scrub the eyelid margins along the base of the eyelashes.
You can also find specialized eyelid cleaning wipes online and in local stores.
What not to do
To ensure a safe and quick recovery, you should avoid certain habits that can worsen the stye or infection. It’s important that you:
- Do not squeeze the stye – Never try to pop a stye yourself. Squeezing can push bacteria deeper into the eyelid, worsening inflammation and spreading the infection.
- Avoid touching or rubbing the stye – This can transfer more germs to the site, especially if you haven’t cleaned your hands. This can lead to irritation.
- Do not wear old or expired makeup – Throw away expired or old makeup, as it can become contaminated and further clog oil glands. Don’t share your makeup with others.
- Stop wearing contact lenses if possible – Switch to glasses until the infection is gone.
Can you prevent future styes?
To prevent styes, maintain good eye hygiene. This includes using lid scrubs and applying a warm compress regularly to soften oils and improve drainage from the eyelid glands.
If you’ve had styes, blepharitis or dry eyes, you’re more likely to have them again. Adopting simple habits can significantly reduce your chances of future styes:
Wash your hands often, especially before touching your face or eyelids.
If you wear contact lenses:
- Always wash your hands before putting in or removing contact lenses.
- Follow your lens cleaning and disinfecting instructions carefully.
- Avoid wearing contact lenses overnight unless your eye doctor has approved it.
When you wash your face:
- Gently clean along the base of your eyelashes, where oil and debris can build up.
- Use a mild cleanser, such as diluted baby shampoo or eyelid scrub, to prevent blocked glands.
If you wear eye makeup:
- Remove eye makeup before bed to keep your eyelids clean.
- Replace mascara, eyeliner and other eye cosmetics every 3 to 6 months.
- Never share your makeup with others.
Manage underlying conditions, such as:
- Blepharitis
- Dry eyes
- Diabetes
- Any other conditions that can increase the risk of styes or other eyelid problems
When should you see an eye doctor?
Most styes are minor and resolve with home care. However, you should make an appointment if the stye doesn't improve after 1 to 2 weeks or if symptoms are worsening. Frequent styes may indicate an underlying issue, like chronic blepharitis or diabetes, that needs attention. In such cases, a doctor might take a small tissue sample to rule out serious concerns.
Contact your eye doctor as soon as possible if you notice the following symptoms:
- Eyelid swelling that shuts the eyelid
- Changes in your vision
- Worsening redness and swelling that have spread beyond the stye
- Blisters on the eyelid
- Pus or blood in the stye drainage
- A warm feel to the eyelid
If you notice redness, swelling and warmth spreading across your eyelid or to nearby areas of your face, along with increased pain, fever or chills, seek immediate medical attention. These symptoms could indicate a serious infection, such as cellulitis.
Possible medical treatments
If warm compresses and gentle eyelid cleaning do not help your stye improve, your eye doctor may prescribe medication or recommend a quick, in-office procedure.
Prescription treatment options
- Antibiotic ointment – Your doctor may prescribe antibiotic ointment to apply directly to the eyelid. These help control infection and speed up healing.
- Oral antibiotics – If the redness or swelling spreads to the surrounding skin, your doctor may prescribe antibiotic pills to treat the infection more thoroughly.
- Steroid injection – If a stye has become a firm, lingering bump (chalazion), a steroid shot — such as cortisone — can reduce inflammation and swelling.
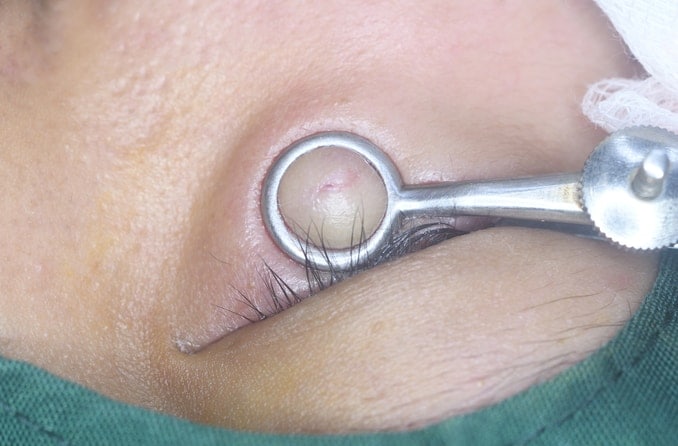
Procedures
For large, very painful or long-lasting styes, your doctor may need to perform a procedure in the office. It usually provides quick relief from pressure and pain. The procedure involves:
- Local anesthesia – This will allow you to be more comfortable.
- Incision – A tiny opening will be made.
- Drainage – This allows the pus to be removed.
Biopsy (rare)
If an eyelid lump keeps recurring in the same spot, your doctor may take a small sample to test for and rule out other conditions. This is called a biopsy.
What to know about a stye
While a stye can be painful, it is a common, temporary eye condition. Most styes heal on their own, usually within 1 to 2 weeks.
To speed up healing, apply warm compresses often and gently clean the eyelid edges. Heat helps with drainage. Most importantly, never squeeze or pop the stye. Avoid wearing eye makeup and using contact lenses until it fully heals. Continued makeup and contact lens use can spread the infection or worsen inflammation.
To prevent future styes, maintain good hygiene. Always wash your hands before touching your eyes and replace old makeup regularly. While home care usually works, see an eye doctor right away if pain increases, vision changes or redness spreads to your face.
Regular eye exams allow your eye doctor to spot any eyelid bumps early, helping prevent discomfort or complications before they become serious.