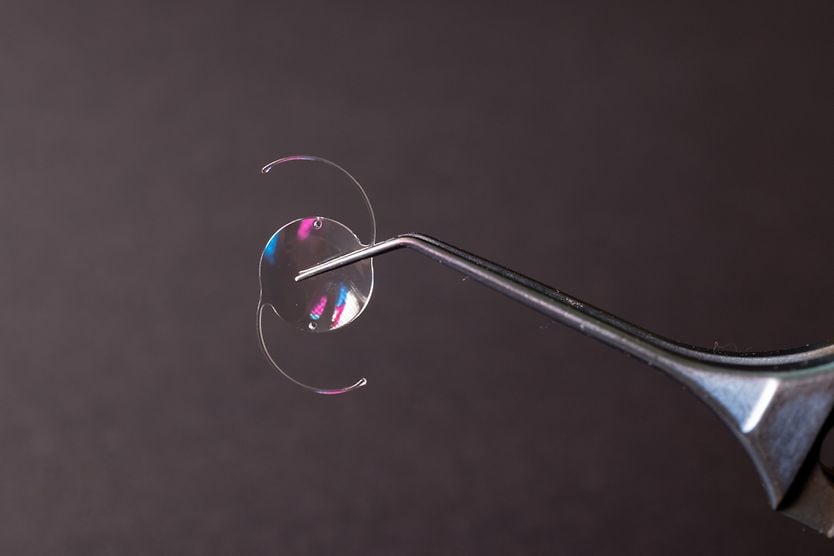
On average, cataract surgery can cost anywhere from $3,000 to $6,000 per eye. But a lot of factors can affect the final price. Most insurance companies, including Medicare, cover standard cataract surgery. How much of the total cost you pay will depend on your insurance status and provider.
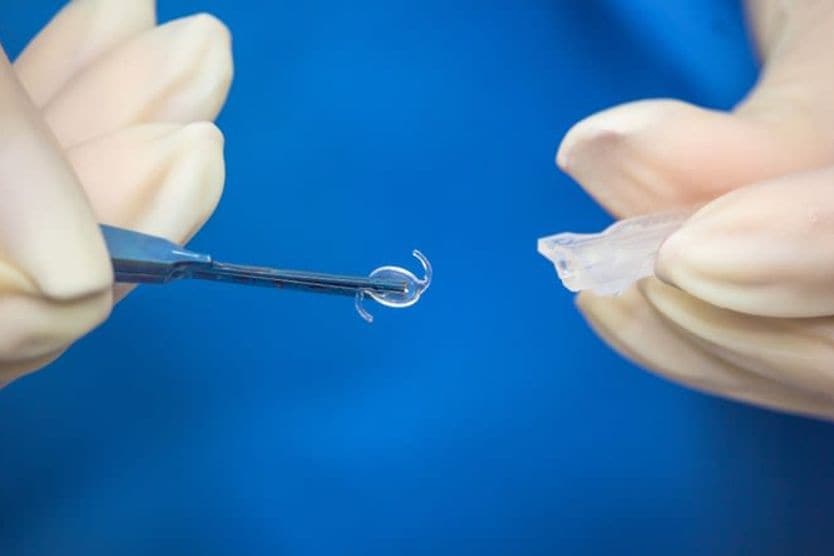
The actual amount paid for cataract surgery without insurance can also depend on the type of intraocular lens (IOL) implanted in the eye during the procedure, the type of technology used during surgery, and the skill and experience of the surgeon.
If you choose standard cataract surgery with a standard monofocal IOL, it may be fully covered by insurance, but you will often still need to pay any deductibles, copayments and coinsurance set by your insurance coverage.
If you choose laser cataract surgery and/or need a premium toric IOL for astigmatism or a presbyopia-correcting IOL, you likely will be required to pay the added costs associated with these advanced techniques and lenses with your own money.
WANT TO LEARN MORE ABOUT CATARACT SURGERY? Find a cataract surgeon near you.
Determining Cataract Surgery Cost (no insurance)
Since most people who undergo cataract surgery in the U.S. have Medicare or private medical insurance, it can be somewhat challenging to determine the cost of the procedure for someone with no insurance coverage.
In some cases, surgeons will charge similar fees for cataract surgery that they charge for an elective vision correction procedure called refractive lens exchange (RLE).
Refractive lens exchange is essentially the same procedure as cataract surgery, but the eye's natural lens that is removed in RLE has not yet become clouded by a cataract. By replacing the eye's natural lens with an IOL, the surgeon can correct significant amounts of nearsightedness or farsightedness, reducing the patient's need for eyeglasses or contact lenses.
Cataract Surgery Costs (Co-Pay with insurance)
Basically, "out-of-pocket" expenses for cataract surgery are those costs that are not covered by Medicare or private medical insurance, in addition to any deductibles, copayments and coinsurance. They can also include costs for procedures or products that aren't considered medically necessary by the insurance carrier.
For example, implanting a standard monofocal IOL during cataract surgery would be considered the standard of care and medically necessary. This is because your eye's natural lens is removed as part of a cataract procedure, and you need an artificial lens as a replacement to restore your sight.
You likely would have very good distance vision with this type of IOL, but usually you would need reading glasses for near vision. Also, if you had astigmatism prior to cataract surgery, you would still need prescription eyeglasses to correct astigmatism unless an additional procedure called limbal relaxing incisions (LRI) is performed.
Today, people who need cataract surgery may want to be as free from glasses as possible after surgery. And thanks to advances in intraocular lens and surgical technology, it's now often possible to make this happen.
But this added technology typically comes with added costs, and in most cases Medicare and private medical insurance will not pay the added cost of these "premium" products and procedure.
If you want to reduce your need for glasses after surgery, you will likely have to pay the added cost yourself ("out-of-pocket") — even if you have insurance that covers the costs of standard cataract surgery.
SEE RELATED: Does vision insurance cover cataract surgery costs?
Insurance providers typically don't cover these costs because:
- Reading glasses are much less expensive than premium IOLs and can provide you with functional vision.
- Many people must pay for and wear eyeglasses that correct common refractive errors such as nearsightedness and farsightedness. Unless you have supplemental vision insurance, regular health insurance typically doesn't cover these kinds of vision problems.
- People undergoing refractive surgery such as LASIK to correct common vision errors also must pay full costs that typically aren't covered by insurance. As with cataract surgery add-ons, surgical vision correction of this nature is considered cosmetic or medically unnecessary because you have the option of wearing much less expensive eyeglasses.
While the costs of a basic cataract procedure and standard IOL usually are covered by Medicare and private medical insurance, you will likely need to pay the added cost of the following premium IOLs and advanced surgical techniques out-of-pocket:
Presbyopia-correcting IOLs
These advanced intraocular lenses expand your range of vision, reducing vision loss caused by presbyopia so you can read and see clearly up close without reading glasses. The two most popular types of presbyopia-correcting IOLs approved for cataract surgery in the United States are multifocal IOLs and accommodating IOLs.
Toric IOLs
These astigmatism-correcting IOLs enable a person who had astigmatism prior to cataract surgery to see clearly for driving, computer use, reading and other tasks without eyeglasses after cataract surgery.
Laser-assisted cataract surgery
In this advanced procedure (also called "laser cataract surgery"), a femtosecond laser is used to perform steps in cataract surgery that typically are performed with manual surgical tools, adding a higher degree of precision.
Laser cataract surgery also can reduce stress on the retina and other delicate tissues of the eye during cataract extraction.
Laser cataract surgery usually is performed when a premium presbyopia-correcting or astigmatism-correcting IOL is implanted. The added cost of the laser procedure typically is included in the price of the premium IOL.
Limbal relaxing incisions
Also called LRI or corneal relaxing incisions, this is an additional surgical procedure that can be performed during cataract surgery to correct astigmatism. One or more small, arc-shaped incisions are made in the periphery of the cornea, and as these incisions heal (without stitches), the cornea takes on a more spherical shape.
Laser arcuate incisions
This minor surgical procedure is very similar to LRI, but the incisions are made with a femtosecond laser rather than a hand-held surgical tool.
The Cost of Cataract Surgery with Medicare
In uncomplicated procedures, Medicare coverage is typically straightforward in terms of standard reimbursements paid to the eye surgeon and surgical center.
When it comes to cataract surgery, private health insurance providers may choose to follow Medicare's lead regarding allowable charges that will be covered.
Reimbursements from private insurance can vary widely, depending on your responsibility for your copay and your annual deductible.
You may need to pay other related costs that aren't directly associated with the cataract procedure itself. For example, Medicare patients pay 20% of fees for the following types of products and services:
- An EKG to determine your heart health before you undergo a cataract procedure.
- A comprehensive eye exam, including precise measurements of your eyes' refractive errors.
- Charges related to anesthesia personnel such as an anesthesiologist or nurse anesthetist.
- Standard prescription eyeglasses, if needed, to enhance near vision after you've had surgery.
- Any follow-up procedures or medical care due to cataract surgery complications outside a standard period designated for post-operative care.
Questions for Your Insurance Provider
You should speak in-depth with your insurance provider or Medicare representative before having cataract surgery to understand exactly how much is covered and how much you ultimately may need to pay out-of-pocket.
Terms of policies vary widely from one insurance company to the next. Questions to ask include:
How much is the copay or coinsurance?
In other words, will you be required to pay a certain amount — such as 20% — of all related costs, even though they are covered by your health insurance?
How much is the deductible?
Many people choose to have a relatively high annual deductible for their insurance coverage to keep monthly fees low.
If you have an annual deductible of $1,700, for example, you will need to pay that amount out-of-pocket before proceeding with the cataract surgery if you haven't incurred other medical expenses that apply to the deductible.
Does your plan pay for eyeglasses?
If you need glasses following cataract surgery, find out if your coverage includes at least partial payment for a pair. Many insurance companies, including Medicare, offer a partial reimbursement for one pair of glasses in a lifetime after cataract surgery.
Does your cataract surgeon have a special arrangement as a "preferred provider" or equivalent with your insurance company?
This could make a big difference in the amount you are charged for standard cataract surgery, if you aren't already covered by Medicare.
An eye surgeon with "preferred provider" or equivalent status must charge no more than standard rates for conventional cataract surgery, with agreed-upon maximums.
If your eye surgeon is not "preferred," does your insurance company need to approve him or her before covering the procedure?
Don't forget to ask this. You don't want to schedule your procedure and then discover that you don't have the necessary approval.
Is the surgical center a preferred provider or approved by your insurance carrier?
It may not be, even if your surgeon is. It's essential that you have an understanding with your insurance provider or Medicare that the surgical center your surgeon will use is approved.
Otherwise, you could (in a worst-case scenario) be responsible for all fees charged by the surgical center. And this could add up to several thousand dollars per eye.
Does your insurance company require advance approval to validate that a cataract procedure is medically necessary?
Some do, so it’s best to know ahead of time.
Cost of cataract surgery with FSAs and HSAs
Flexible Spending Accounts (FSAs) are sometimes used to pay for eye surgery. An FSA allows you to divert pre-tax income from your job into an account for out-of-pocket health care expenses.
In 2026, the maximum annual employee contribution to an FSA is $3,400. Depending on your insurance coverage, your surgeon’s reputation and experience, the technology used, and the premium services and procedures you elected, you may need more than the FSA to pay for your surgery.
Another option is to set tax-free money aside in a Health Savings Account (HSA) to pay for cataract surgery. To be eligible for an HSA, you must be covered by a high-deductible health plan (HDHP) at work.
You can add tax-free contributions to your HSA each pay period, up to an annual limit of $4,400 for individual coverage and $8,750 for family coverage (2026 limits; includes employee and employer contributions). And, unlike an FSA, any unspent money in your HSA at the end of the year "rolls over" so you can use it the following year or even further in the future.
Depending on your budget, you could save enough money to pay the entire cost of your cataract surgery by contributing money to your HSA over a period of one or more years.