Optic disc definition
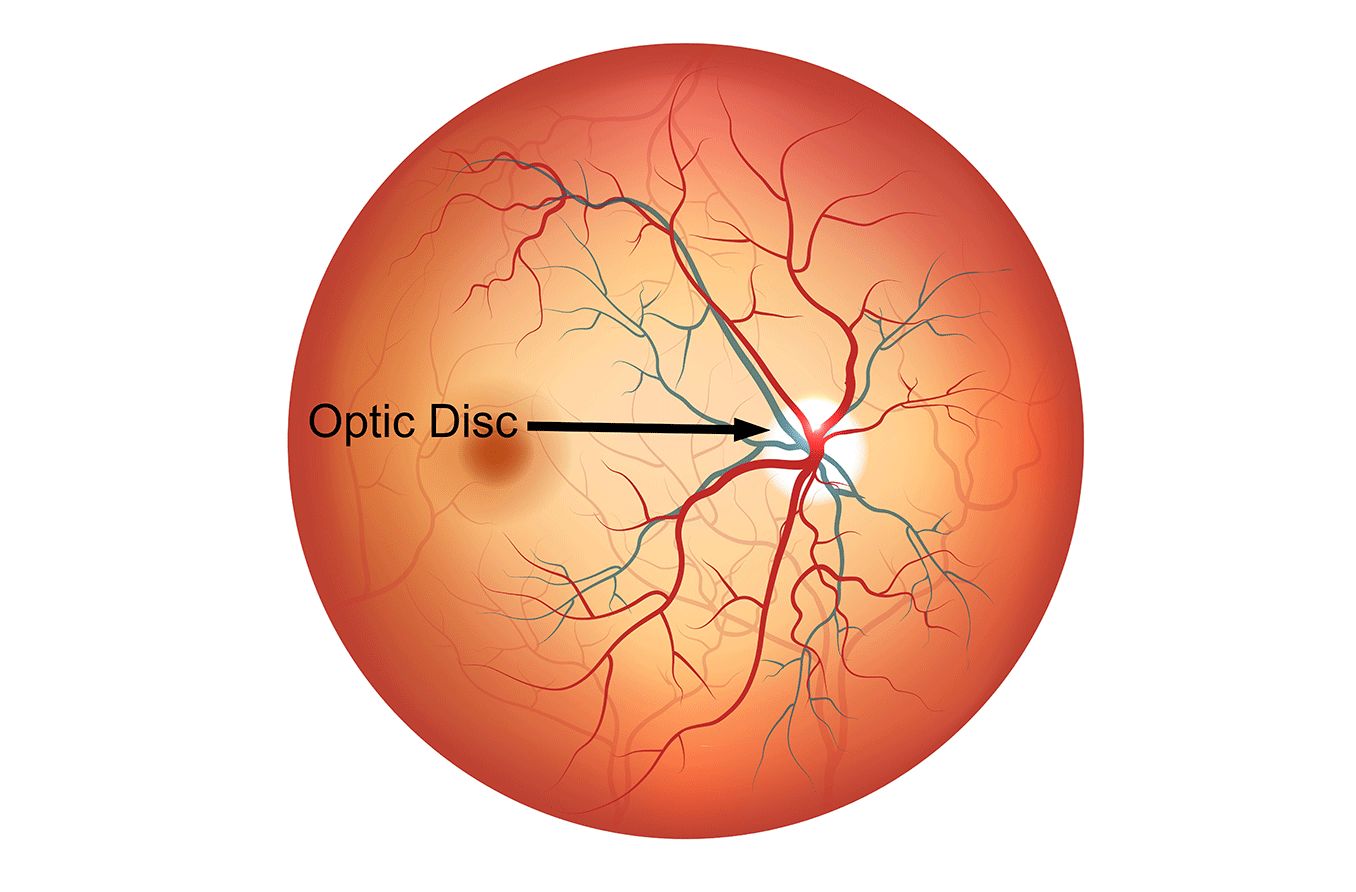
The optic disc, sometimes called the optic nerve head, is a round section at the back of the eye. It is where the retina and optic nerve connect. The optic disc is also where the retina’s main artery and vein enter the eye.
Optic disc anatomy
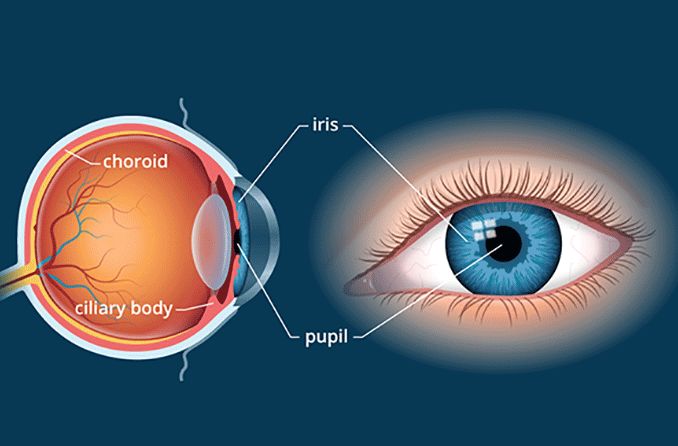
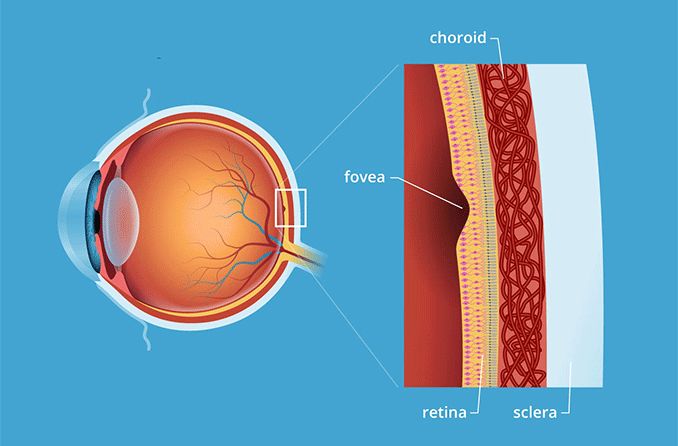
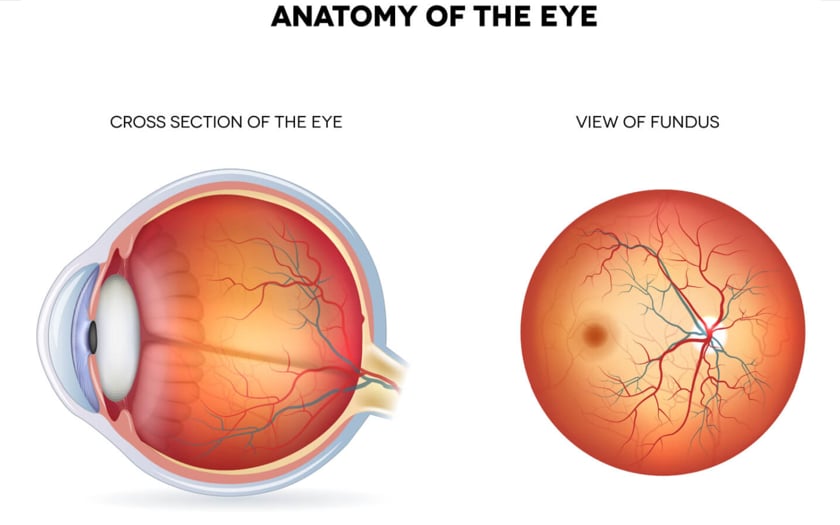
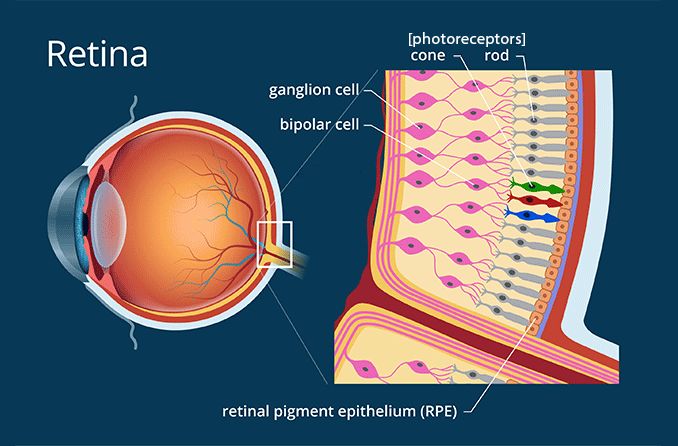
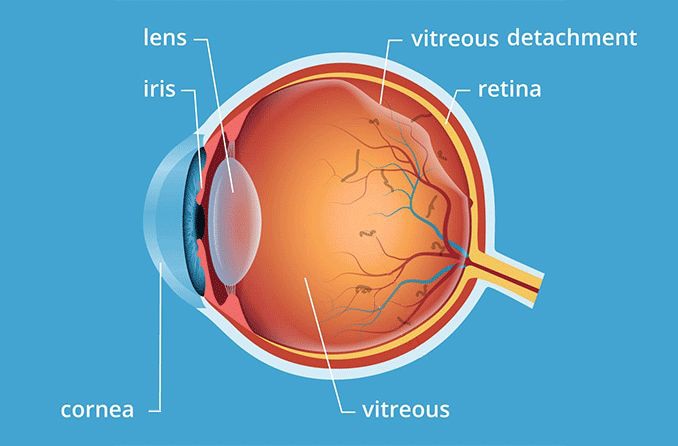
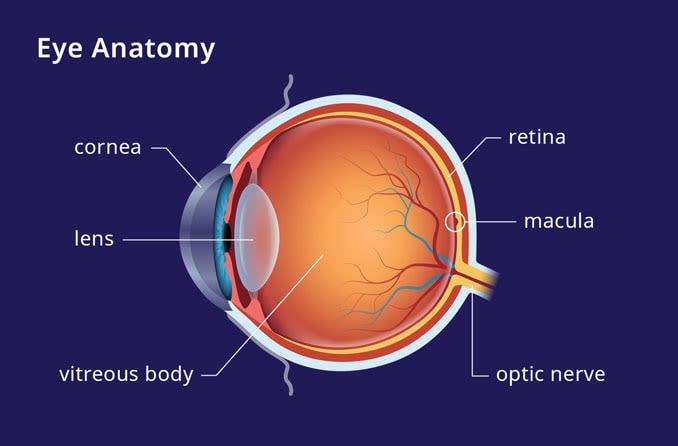
There is a layer of tissue at the back of each eye, opposite to the pupil, called the retina. This tissue is responsible for taking the light that enters the eye and turning it into the images you see.
There are two main areas in the retina: the macula and the peripheral retina. The macula, which is located in the center of the eye, is responsible for seeing images directly in front of you. The peripheral retina, which makes up the rest of the retina, is responsible for peripheral vision.
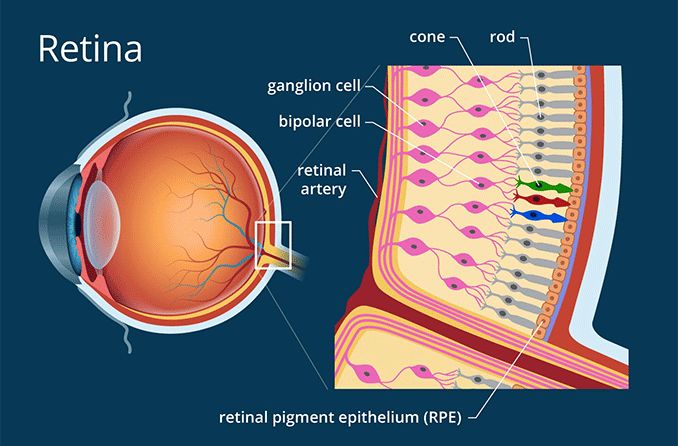
The retina contains cells called photoreceptors, which can also be broken into two categories: rods and cones. Rods are responsible for detecting the size, shape, brightness and movement of objects. Cones are responsible for processing color and fine detail. Rods help you see at night or when the light is dim. Cones help you see better when the light is brighter.
The optic disc is a round, slightly raised area at the border of the macula and the peripheral retina, and it can be yellow-orange or pink. It is the only spot on the retina that has no rods or cones, making it a “blind spot.”
There is a small indentation at the center of the optic disc, called the physiologic cup. This is where the optic nerve, made up of over a million nerve fibers, connects to the retina.
Optic disc function
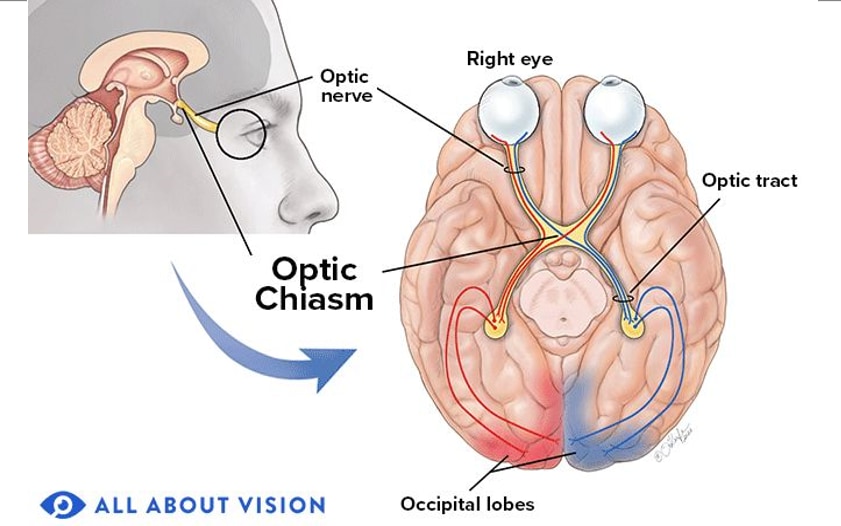
When light enters the eye through the lens, it hits the retina at the back of the eye. The photoreceptors take the light and turn it into electrical signals. These signals then travel through the retina to the optic disc. The optic nerve takes these electrical signals and delivers them to the brain, which interprets them into the images we see.
The optic disc is also where the retina and the central retinal artery and vein connect. The central retinal artery, a branch of the ophthalmic artery, is responsible for delivering blood from the heart to the retina. The central retinal vein drains blood from the retina and optic nerve back to the heart.
About 20-40% of the population also has a small extra artery coming out of the optic disc, called the cilioretinal artery. The cilioretinal artery delivers blood to the center of the macula.
Optic disc problems
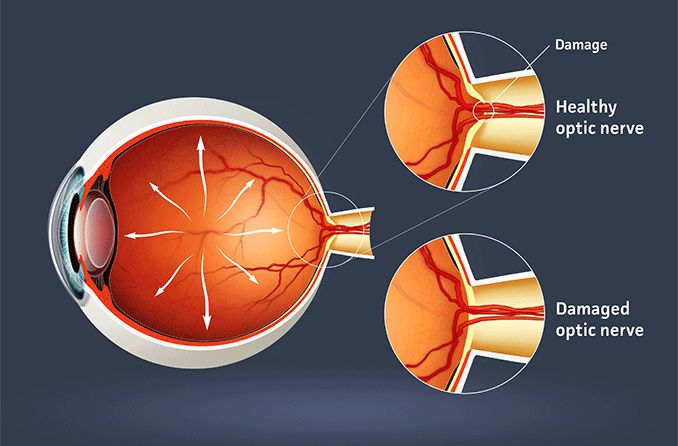
Because the optic disc houses such important connections, any damage to the disc can negatively impact vision.
Glaucoma
Glaucoma is the most common optic disc disorder. It is caused by elevated pressure of the fluid inside the eye pressing down on the optic disc and damaging the nerve fibers. A normal pressure is between 10 and 20 millimeters of mercury.
Pressure in excess of 30 will almost always cause glaucomatous damage to the optic disc. Pressure that is between 20 and 30 can still cause glaucoma but less likely. These patients need to be followed carefully. They should receive regular pressure checks, peripheral field tests and scans of the optic nerve. Pressure under 20 is usually safe except in cases of “normal tension glaucoma” in which the optic disc may still sustain damage.

It is possible for an eye doctor to look at the optic disc and predict whether it has been damaged by glaucoma. In glaucoma, the bottom quadrant of the optic disc is usually damaged first followed by the top quadrant. This causes thinning of the optic nerve tissue in these two sectors.
Glaucoma is a “silent disease” — you don’t feel or see that something is wrong until the optic nerve is almost completely damaged and you’re close to going blind. Because of this, it’s essential to see an eye doctor regularly, even if you don’t need glasses. If an eye doctor detects glaucoma, then a simple treatment with eye drops is often all that is needed.
Glaucoma is, to a large degree, inherited. For this reason, it is also advised to be evaluated for an optic disc disorder if you find out that a family member has glaucoma.
Papilledema
Papilledema occurs when the brain swells. Brain swelling causes increased intracranial pressure (ICP), which in turn causes the optic disc to swell. ICP refers to pressure that has built up inside the skull. Papilledema often leads to vision loss, brought on by damage to the optic nerve where it connects at the optic disc.
Treatment is aimed at the underlying cause of the ICP rather than the papilledema itself. ICP can be caused by:
Too much cerebrospinal fluid
Bleeding in or around the brain
Swelling of the brain
Aneurysms
Brain/head injuries
Brain tumors
Meningitis
Encephalitis
Hydrocephalus
ICP is a medical emergency. Seek immediate medical attention if you think you may be experiencing ICP.
Optic disc drusen
Optic disc drusen are small deposits that form beneath the surface of the optic disc. These deposits are made up of pieces of protein that have calcified or hardened.

Optic nerve drusen [Image credit: This image was originally published in the Retina Image Bank® website. Author: Mitzy E Torres Soriano, MD. Photographer: Mitzy E. Torres Soriano. Retina Department. Hospital Provincial del Centenario. Rosario, Argentina. Optic disc drusen. Retina Image Bank. 2016; Image Number 26681. © the American Society of Retina Specialists.]
Family members of someone with optic disc drusen are up to 10 times more likely to have optic disc drusen as well. If you have been diagnosed with optic disc drusen, it’s a good idea to have members of your family receive an eye exam.
Optic disc drusen can press on the optic nerve and cause loss of peripheral vision, but this is uncommon. There is no effective treatment for optic nerve drusen. But some eye doctors prescribe drops to lower the pressure inside the eye to reduce the risk of damage to the optic disc.
SEE RELATED: Fundus
Arteritic anterior ischemic optic neuropathy (A-AION)
A-AION is a condition caused by sudden loss of blood flow to the optic nerve. It can cause immediate vision loss in one (unilateral) or both (bilateral) eyes. Inflammation in the central retinal artery impedes blood flow. This is an issue called giant cell arteritis (GCA).
GCA can damage the entire optic disc, leading to permanent blindness if not diagnosed and treated quickly. In some cases, it can even be fatal.
In most cases, there are symptoms that precede loss of vision:
Pain in the temple
Pain while chewing and tiredness of the jaw muscles (called claudication)
Pain or tingling in the scalp
Pain in the neck
Achiness in the upper arms or legs
Fatigue
Appetite loss
Unexplained weight loss
Fever
The vision loss associated with A-AION is usually painless. It is imperative to seek immediate medical attention if you experience sudden vision loss. Permanent vision loss from A-AION can occur within minutes or hours.
A-AION is treated with high doses of corticosteroids. It is more commonly found in females and individuals over the age of 55.
Non-arteritic anterior ischemic optic neuropathy (NA-AION)
NA-AION is the more common form of anterior ischemic optic neuropathy. It is also characterized by sudden vision loss due to a lack of blood flow to the optic nerve. It accounts for around ⅓ of cases of optic disc swelling.
The vision loss is typically painless and usually only impacts one eye (unilateral). Damage to the optic nerve in NA-AION is located at the optic disc, which is also where the loss of blood flow occurs.
What distinguishes NA-AION from A-AION is the cause of blood loss. Rather than inflammation, the impeded blood flow can be caused by:
An extreme drop in blood pressure
Increased pressure in the eye
Narrowed arteries
Thickening of the blood
Drop in blood flow to the optic disc
There is no definitive cause of NA-AION. However, those with high blood pressure, sleep apnea and diabetes are most commonly impacted.
Patients often experience NA-AION early in the morning. The blood flow in the optic nerve is reduced, and the pressure of the fluid inside the eyeball that is pressing down on the optic disc is highest.
Many patients with NA-AION also have the nerve tissue bunched up inside the optic disc, which may contribute to the condition. It does not impact one gender more than another, but it is found most often in those over the age of 50.
There is no current treatment for NA-AION available.
Optic disc coloboma
Optic disc coloboma is a group of congenital (present at birth) disorders that are characterized by hollows or holes in the optic disc. While there is no treatment for this family of disorders, early detection can help prevent further complications.
Optic disc colobomas can cause large blind spots in one’s central or side-vision. Optic disc coloboma can also lead to retinal detachment. This is an emergency situation in which the retina separates from the inside wall of the eye.
Optic disc coloboma has been associated with retinoschisis. This condition occurs when the top and bottom layers of the retina separate, forming a blister-like dome.
Optic disc hemorrhage
Hemorrhages occur when blood vessels are damaged, causing bleeding. Optic disc hemorrhages, often flame- or splinter-shaped, are commonly associated with glaucoma.
However, the underlying cause of these hemorrhages is unknown. They have also been linked to conditions such as:
Diabetes
Optic disc drusen
Retinal vascular diseases
Systemic hypertension
Leukemia
The vitreous jelly pulling loose from the inside of the eye as you age
Optic disc hemorrhages do not usually impact vision but can be a sign of other serious eye problems. There is no treatment specifically for optic disc hemorrhages. However, it is important to address any underlying conditions.
Malignant hypertension
Very high blood pressure can cause the optic disc to swell. In these cases, fluid can leak into the center of the retina in the formation of a “macula star.” This is a medical emergency and requires immediate admission to a hospital.
Diabetic papillopathy
A swollen optic disc in one or both eyes in someone with diabetes mellitus — when it is not associated with significant loss of vision — can indicate diabetic papillopathy. This condition often gets better again by itself without causing permanent vision loss. It is important that tests are done to make sure the swelling is not due to a more serious cause.
Importance of routine eye exams
The health of your optic disc is critical to your overall eye health. Regular eye exams allow your eye doctor to check for damage to the optic disc, as well as signs of conditions like AION and optic coloboma.