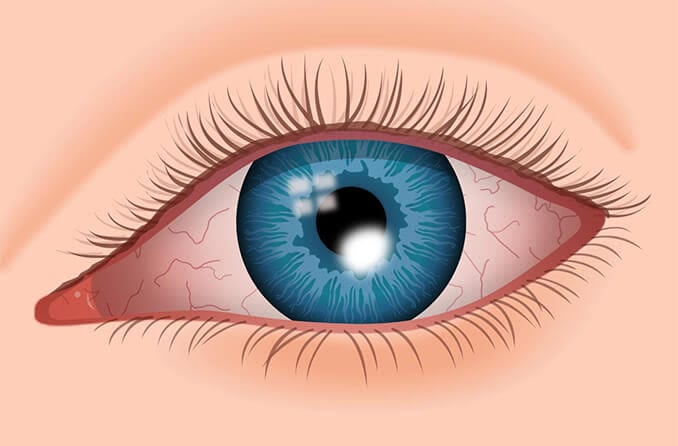
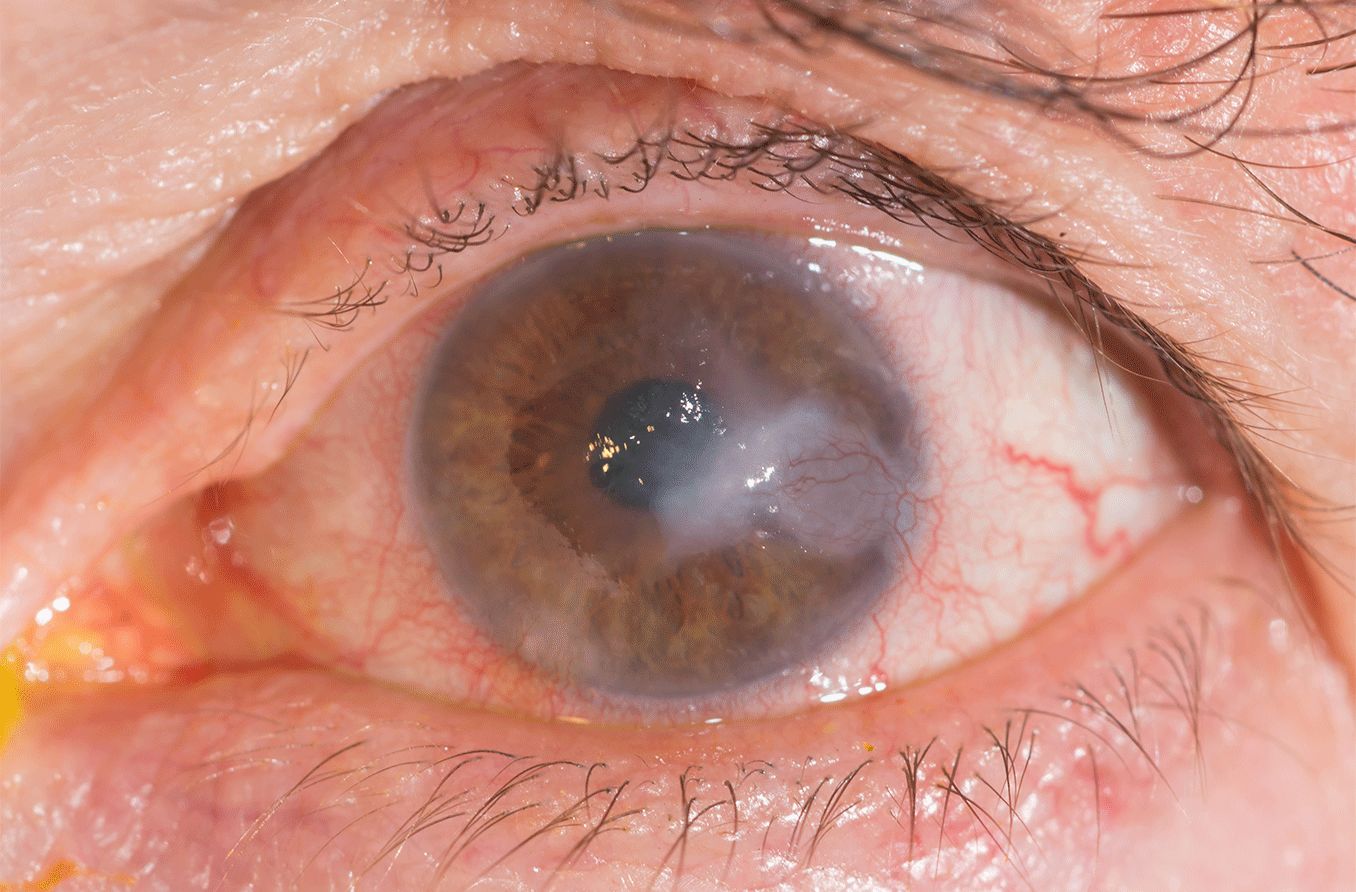
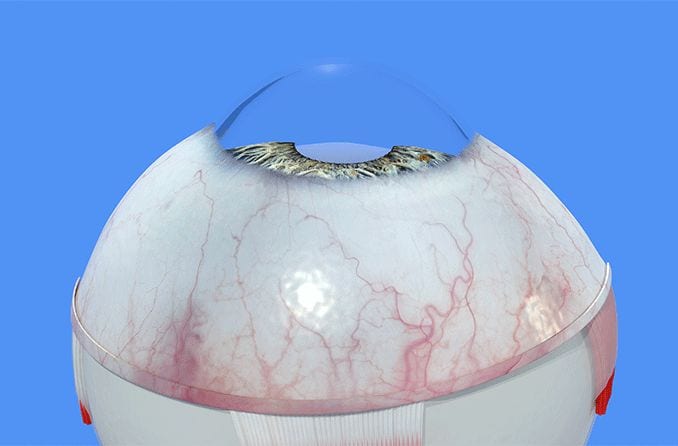
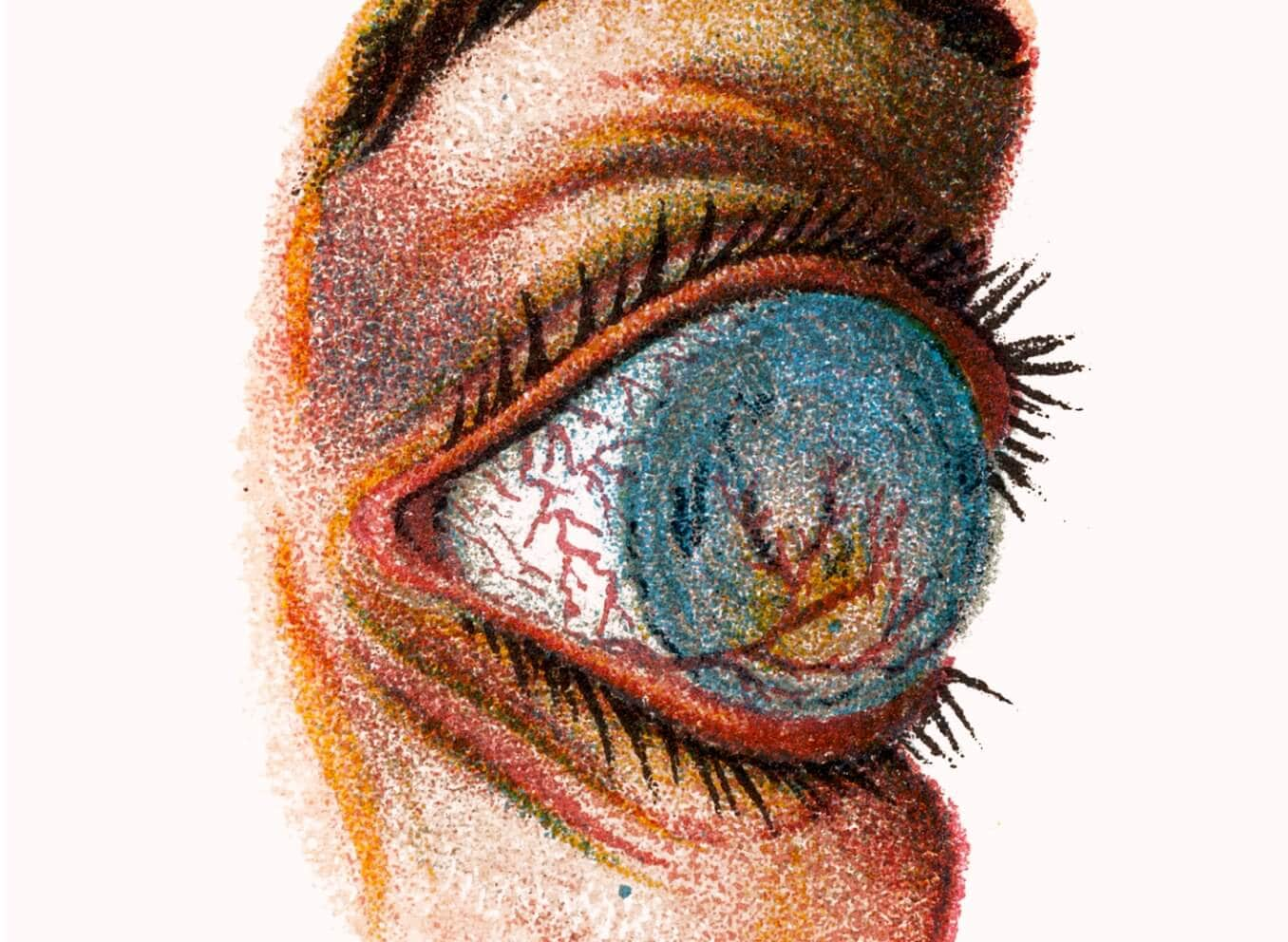
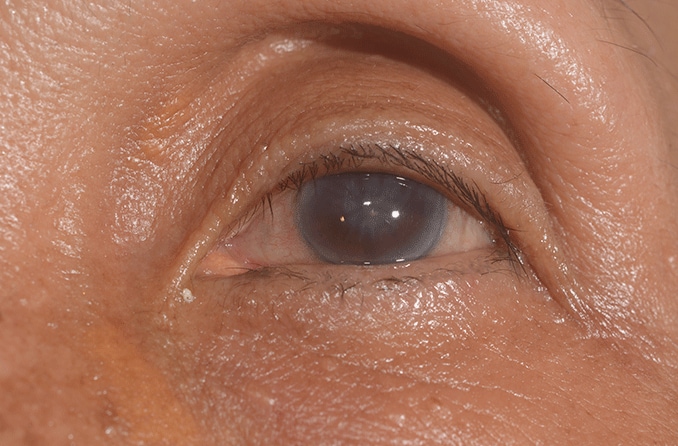
What is a corneal ulcer?
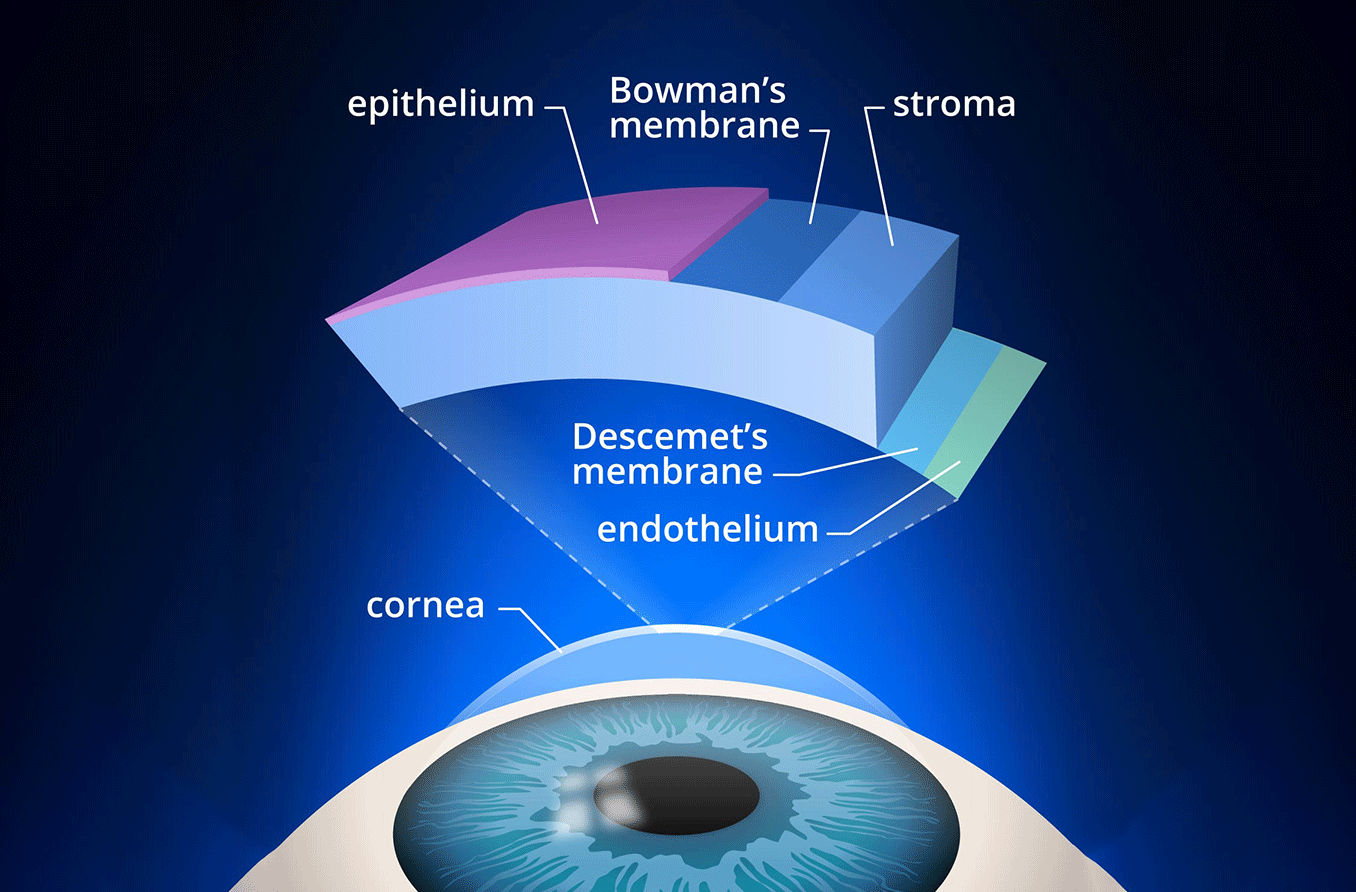
A corneal ulcer is an open sore on the cornea of the eye. It's usually due to an infection affecting the clear front surface of the eye, resulting in inflammation of the cornea (keratitis). A corneal ulcer typically causes a painful red eye, with mild to severe eye discharge and reduced vision. Medical treatment is required.
Corneal ulcer symptoms
Symptoms of corneal ulcers include:
Feeling something is "in" your eye (foreign body sensation)
Pus or other eye discharge
SEE RELATED: What is Hypopyon?
Causes of corneal ulcers
Most cases of corneal ulcer are due to a bacterial infection that invades the cornea — often following eye injury, trauma or other damage.
Contact lens wearers are particularly susceptible to eye irritation that can lead to a corneal ulcer. A contact lens may rub against the eye's surface, creating slight damage to the epithelium that may enable bacteria to penetrate the eye.
If you are a contact lens wearer, you can increase your chances of avoiding a corneal ulcer by practicing good hygiene such as washing your hands before handling lenses and following other safety tips.
Besides bacterial infection, other causes of corneal ulcers are fungi and parasites, such as:
Fusarium. These fungi have been associated with fungal keratitis outbreaks among contact lens wearers.
Acanthamoeba. These common parasites can enter the eye and cause Acanthamoeba keratitis. This is very serious eye infection that can result in permanent scarring of the cornea and vision loss. Acanthamoeba microorganisms are found in tap water, swimming pools, hot tubs and other water sources.
Wearing contact lenses while swimming significantly increases your risk of a corneal ulcer from Acanthamoeba keratitis. [Also read: Can You Swim with Contact Lenses?]
Another cause of corneal ulcer is herpes simplex virus infection (ocular herpes), which can damage the surface and deeper layers of the cornea.
Other underlying causes of corneal ulcers include:
Severe dry eyes
Immune system disorders and inflammatory diseases (such as multiple sclerosis and psoriasis)
Corneal ulcer treatment
If you suspect you have a corneal ulcer, see an eye doctor immediately. Untreated corneal ulcers can lead to severe vision loss and even loss of an eye.
Corneal ulcer treatment usually includes frequent application of topical antibiotics.
The location and size of the corneal ulcer will guide your eye doctor in determining the need for cultures to identify the type of organism involved. Most eye doctors see patients with corneal ulcers every one to three days, depending on the severity of the condition.
If the ulcer is in the central cornea, the condition usually takes longer to heal. There also is a greater risk of vision loss from a central corneal ulcer.
Eye trauma increases your risk of a corneal ulcer from fungal keratitis. This is particularly true when organic matter (such as from a tree branch) is involved in the injury.
Treatment of corneal ulcers from fungal keratitis includes use anti-fungal agents. These may be used topically to the eye and orally, depending on the severity of the ulceration. The prognosis for good vision depends on the extent of infection.
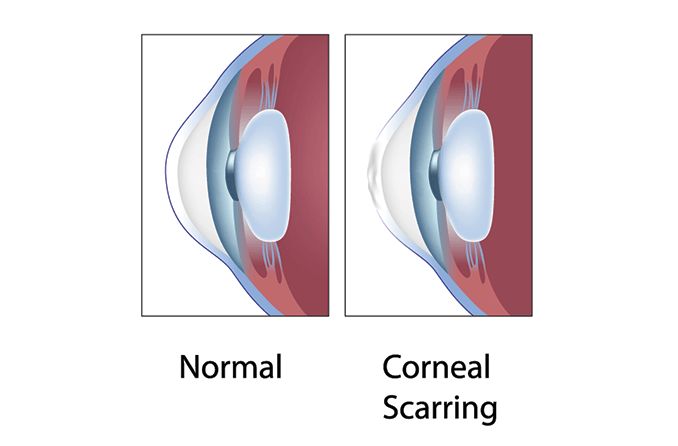
Even if detected early and managed properly, some cases of corneal ulcers will require a cornea transplant to restore lost vision from scarring.