Introduction to contact lens exams
Contact lenses are prescription lenses that can correct vision problems, similar to glasses. Unlike glasses, however, they are worn directly on the eye. A contact lens exam is necessary to determine if contacts are suitable for your eyes and to find the right ones for you.
Contact lenses are placed over the cornea, the eye’s clear outer covering that’s shaped like a dome. The cornea helps focus light as it enters the eye. Abnormalities in the shape of the cornea or eyeball can make your vision blurry, which is called a refractive error. Glasses and contacts can help correct refractive errors, such as:
- Myopia (nearsightedness) – Close objects can be seen clearly but distant objects look blurry
- Hyperopia (farsightedness) – Distant objects can be seen more clearly than close ones
- Astigmatism – Objects appear blurry at any distance
- Presbyopia – Difficulty seeing near objects clearly as you age. (Starting around age 40, the eye’s crystalline lens gradually becomes less flexible. This makes it harder to focus on things up close.)
Having your eyes examined for contacts is the first step in determining whether they’re right for your needs. You may not be able to use them if you have certain conditions (like dry eyes or allergies). If you are a candidate for contacts, your eye doctor will help determine which type is best for you. This is where the contact lens fitting of the exam comes in.
There are many different types of contacts available. They may be prescribed based on:
- The lens material
- How often you plan to wear and replace them
- The type of refractive error they are intended to correct
- Whether you need additional or special features for other eye conditions
Contact lenses are generally medical devices, and it’s important to get them prescribed and fitted specifically for you. Contacts that were not prescribed for you can scratch or strain your eyes, cause an eye infection or lead to other conditions. Even cosmetic color contact lenses may need a prescription to be purchased.
SEE RELATED: Can you buy contact lenses without a prescription?
What happens during a contact lens exam?
Your eye doctor may perform tests to assess the overall health of your eye, especially if the contact lens exam is part of a comprehensive eye exam. To examine your eyes for contact lenses, your eye doctor may:
- Take some specific measurements of your eyes
- Determine if you can safely wear contacts
- Help you find the right type of contacts based on your vision needs and lifestyle factors
- Teach you how to insert, remove, clean and store the lenses
“Contact lens fitting” refers to the overall process of matching you with the right contact lens based on these factors.
Prescriptions for contact lenses are different than prescriptions for glasses since contacts rest directly on the eye’s surface. While contact lenses should be prescribed by an optometrist or ophthalmologist, they may also be fitted by an optician.

Initial consultation
Discussing your medical and eye health history with your eye doctor is important to determine your vision correction options. During the initial consultation, your eye doctor may also ask about lifestyle factors, like your work and hobbies. Certain conditions or factors may require caution or treatment prior to fitting contacts, while others may prevent you from wearing them altogether.
In general, contacts may not be ideal if you:
- Have dry eyes
- Often get eye infections
- Suffer from allergies
- Can’t clean or take care of your contacts
- Have certain eye conditions, like strabismus (crossed eyes)
- Require safety eyewear or work in an environment that could be hazardous to your eyes
However, it is still possible to wear contacts if the condition is managed successfully.
Eye measurements and tests
Your eye doctor may examine your eyes to make sure they’re healthy in general. They will also conduct certain measurements and tests for contact lenses specifically.
Measuring pupil and iris size
Measuring the size of the pupil (the dark circle in the middle of your eye) can be important to properly fit contact lenses. Pupils should fit within the contact lens in the right way — the center of the lens should be aligned with the pupil’s center. This is especially true for multifocal lenses, which have multiple prescriptions in each lens to correct vision at different distances.
Measuring the pupil can be done using a measurement card or tool that contains black circles of different diameters. The card is held next to the eye so the pupil size can be matched.

The iris (the colored ring that surrounds the pupil) may also need to be measured, especially for scleral contact lenses. Instead of the cornea, these larger lenses rest on the sclera, the white of the eye. This measurement is called the horizontal visible iris diameter (HVID). Some ways the iris can be measured include:
- A slit lamp – A special microscope that projects a focused beam of light, allowing your eye doctor to see inside your eye
- Anterior segment optical coherence tomography – An imaging technique that produces high-resolution images of the anterior segment (the front portion of the eye)
- Magnetic resonance imaging – A technique that creates images of hard-to-see organs and tissues in the body using radio waves and magnetic fields
Evaluating the tear film and conjunctiva
The tear film covers the surface of the eye, helping to keep it lubricated and protected. It’s also what allows a contact lens to stay on the cornea, acting as a “glue” to keep the lens in place. However, a contact lens can affect the relationship between the cornea and the tear film, possibly leading to dry eye.
Having dry eye disease (when your eyes don’t produce enough tears or the film isn’t stable) might mean you can’t wear contacts. Tears will still have to get under the lens to keep the eye healthy and lubricated, and a functioning tear film is important to help prevent vision problems. Evaluating for dry eyes is an important part of the contact lens exam.
There are a few different ways to test for dry eyes or problems with the tear film, including:
- A slit lamp exam – This exam involves your eye doctor using a special microscope with a bright light to examine your eyes. It’s often performed after applying eye drops that make the tear film easier to see.
- Schirmer test – For this test, your eye doctor will place a small strip of paper inside the edge of your lower eyelid. (They may place numbing drops in your eyes before beginning the test.) After 5 minutes with your eyes closed, your eye doctor will assess how wet the paper is to determine the amount of tears produced.
- Tear break-up time – Tear break-up time tests how long it takes for your tear film to disappear after you blink. This test uses a dye to make the tear film more visible to your eye doctor.
It’s also important to make sure the conjunctiva (the membrane over the surface of the eye, just beneath the tear film) isn’t aggravated by the type of contact lens you’re using. Some people may have allergic reactions, like conjunctivitis (pink eye) or giant papillary conjunctivitis, which can affect up to 20% of lens wearers and is a common reason for contact lens dropout. Routine evaluations for allergy symptoms are important, especially in people who may be more susceptible to allergies.
Determining refraction
Vision prescriptions are typically determined with a refraction test. During this test, you will look through a device (called a refractor or a phoropter) at a chart that’s 20 feet away. Your eye doctor will change the lenses in the refractor to test your vision at different prescription powers (strengths). They may also shine a light in your eyes to see how light enters and moves through them.
Your eye doctor may modify the contact lens power compared to your glasses strength to compensate for the contact lenses sitting directly on your eye, while spectacle lenses are usually about half an inch from the eye. This is called the vertex adjustment. They will then perform an over-refraction, which is a refraction measurement done with the contact lens on the eye.
Measuring corneal curvature
Contact lenses typically sit on the cornea, which has a natural curve. This curve is measured to ensure the contact lenses fit properly. Instruments called a manual keratometer and a topographer are used to take this measurement. Reflections from the cornea are interpreted by looking at them directly (keratometer) or by a computer (topographer).
Contact lens fitting
Properly fitting the right contact lenses may involve trying different ones on your eyes and testing your vision as you look through them. Your eye doctor may put these lenses in for you, or they may teach you how to put them in and take them out. Your eye doctor may have lenses available for trial, or they may have to order different lenses, depending on the type you need.
Some lenses can take time to adjust to, and conditions in your optometrist’s office might be different from your daily surroundings. After your contact fitting, you’ll likely be able to take trial lenses home with you for a few weeks to see what works for you. There may be follow-up appointments during this time to talk with your eye doctor about any concerns.
READ MORE: Which contact lenses are right for me?
Understanding your contact lens prescription
Because contacts are worn on the eye, contact lens prescriptions are usually not the same as those for glasses. Contact lens prescriptions typically include additional measurements, such as the curve of your contact lens (called the base curve, or BC) and the width of the contact lens (called the diameter, or Dia).
Other details or measurements your prescription may include are:
- Power of the prescription
- Type of contact lens prescribed
- Contact lens material and manufacturer
- Dates of the examination, when the prescription was issued and when the prescription expires
READ MORE: Understanding your contact lens prescription
Differences between contact lens exams and regular eye exams
A comprehensive eye exam is performed to determine the overall health of your eyes. This may be a routine checkup, or it may be performed if you have eye symptoms that need to be evaluated.
In addition to other tests, comprehensive eye exams usually include assessments of:
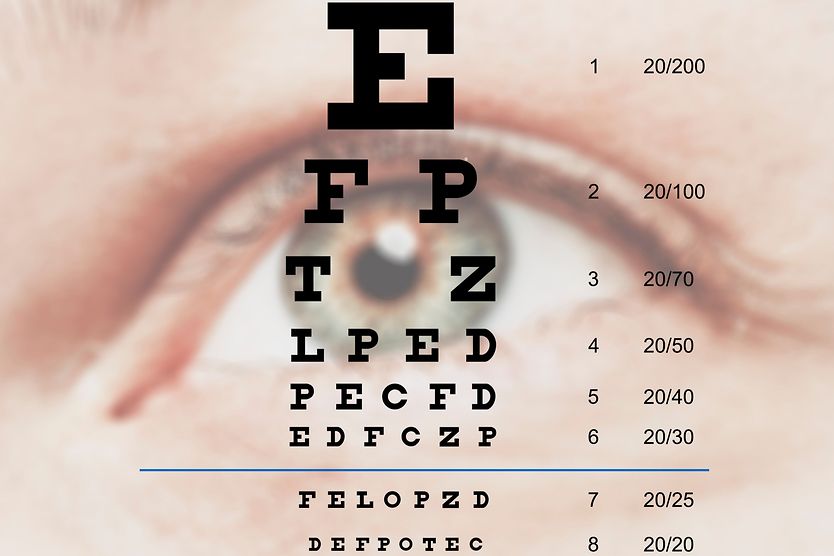
- Visual acuity – The clarity of your vision and ability to see details
- Binocular vision – The ability of both eyes to work together to see a single image
- Refraction – The lens power needed to correct a refractive error
Your eyes may also be dilated (when your pupils widen), which is usually done with eye drops. This helps your eye doctor see the inner structures of your eye to check for eye disease.
Some of these tests may occur during a contact lens exam as well. However, the focus of a contact lens exam is to help determine whether you can wear contacts and to perform specific eye measurements.
READ MORE: Eyeglasses exam vs. contact lens exam: What’s the difference?
Common conditions assessed during contact lens exams
Contact lens exams generally focus on evaluating the health of the eye’s surface and detecting refractive errors. Many conditions can be assessed during these exams to help determine the appropriate lens option, including:
Astigmatism and presbyopia
Astigmatism can be identified by measuring the cornea with a keratometer. It can also be detected through vision testing with an eye chart or a refraction test.
Astigmatism is a common refractive error. It’s often managed with specific types of contact lenses or eyeglasses.
LEARN MORE: Contact lenses for astigmatism
Presbyopia happens to most people as they age. It can be diagnosed during an eye exam through:
- Visual acuity testing
- Refraction
- A slit lamp exam
Presbyopia can also be managed with eyeglasses or contact lenses. If presbyopia occurs alongside other refractive errors, such as astigmatism, you might need glasses or contacts that have multiple prescriptions in them (like multifocal contacts). Another option is monovision contacts, where one lens corrects for near vision while the other lens corrects for distance vision. Some patients wear contact lenses to see in the distance and wear over-the-counter reading glasses to see up close.
Eye surgery can also treat astigmatism and presbyopia. For astigmatism, laser surgery can reshape the cornea to help improve vision at various distances. For presbyopia, implants called corneal inlays can be placed in the middle of the cornea to help you see more clearly close up.
Eye drops that make your pupils smaller, allowing you to focus better, are also available for managing presbyopia.
Dry eyes and tear film evaluation
Dry eyes can happen if your eyes don’t make enough tears or if the tear film isn’t stable. Sometimes, dry eyes are a reason you can’t wear contact lenses. This condition can be discovered during a contact lens exam.
The Schirmer test measures tear production to determine whether your eyes are producing enough tears (or too many). Tear break-up time is used to measure the stability of the actual tear film. This can be done with the use of a dye called fluorescein, or through technologies that use reflective images to show how the tear film breaks.
Dry eyes are often treated with eye drops called artificial tears. Procedures that help block the tear drainage system to prevent your eye from losing tears may also be done. Depending on the condition, you may need treatment before you can start wearing contact lenses.
Preparing for your contact lens exam
It’s important to tell your eye doctor how often you want to wear contacts and discuss other lifestyle factors so they can help find the right fit for you. Be sure to ask questions about how to put in contacts (if you’ve never had them) and how to keep them clean and maintained. Improper maintenance of contacts or wearing them inappropriately can lead to eye irritation, infection and other problems.
If you’ve had contacts before and want to change them, ask your eye doctor about new materials and advancements. If you want to try new ones, you should get a new fit and prescription from your eye doctor. Bring any previous prescriptions (for eyeglasses or contacts) with you to the exam.
What to expect during your follow-up exam
As with glasses, your contact lens prescription can change over time — especially as you age. The prescription will generally expire on a yearly basis. To help maintain your eye health, and to get an updated contact lens prescription, see your eye doctor at least once a year. If you’d like to change the type of lenses you wear, consult your eye doctor for a new contact lens fitting.
Even if you don’t wear contacts, comprehensive eye exams are important to stay on top of any vision changes and to help protect your eyes from disease.
READ NEXT: 5 reasons annual eye exams are important