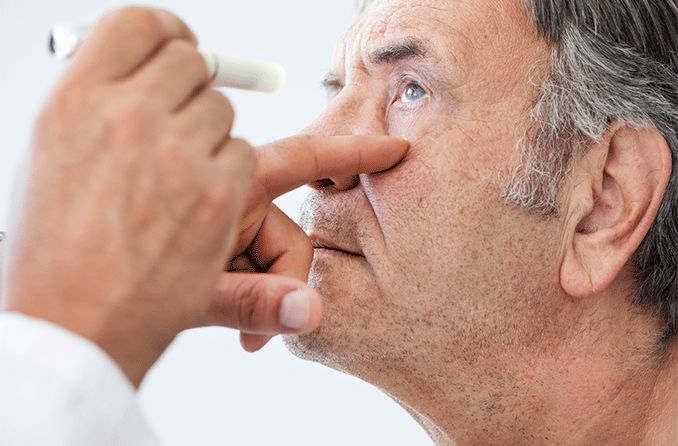
Ophthalmoplegia is characterized by paralysis or weakness in one or more eye muscles. The condition may affect any of the six external eye muscles that control eye movement or the three internal eye muscles that control pupil size and help the eye focus.
Generally, ophthalmoplegia occurs due to an issue in the brain that interferes with signals being sent to the eye muscles.
Symptoms may vary based on the type and cause of ophthalmoplegia, as well as the specific eye muscles affected. Treatment can also differ, depending on the diagnosis from your eye doctor.
Causes of ophthalmoplegia
A variety of conditions, infections or injuries can affect the brain and central nervous system and to weakness and paralysis in external or internal eye muscles. Some of these are more common while others are extremely rare.
Causes of ophthalmoplegia can include:
- Brain tumors
- Congenital conditions (being born with ophthalmoplegia)
- Gene mutations
- Head injury
- Diabetes
- Infections that affect the central nervous system
- Multiple sclerosis (MS)
- Stroke
- Rare diseases such as Tolosa Hunt Syndrome
It's usually uncommon for a head injury or a rare disease to cause ophthalmoplegia. Multiple sclerosis or a stroke, on the other hand, can be more likely to cause the condition.
Symptoms of ophthalmoplegia
The symptoms of this condition can vary and are based on the type you have (for instance, internal or external), the underlying cause and the specific eye muscles affected.
Signs and symptoms may include the following:
- Blurry vision
- Strabismus (misalignment of one or both eyes)
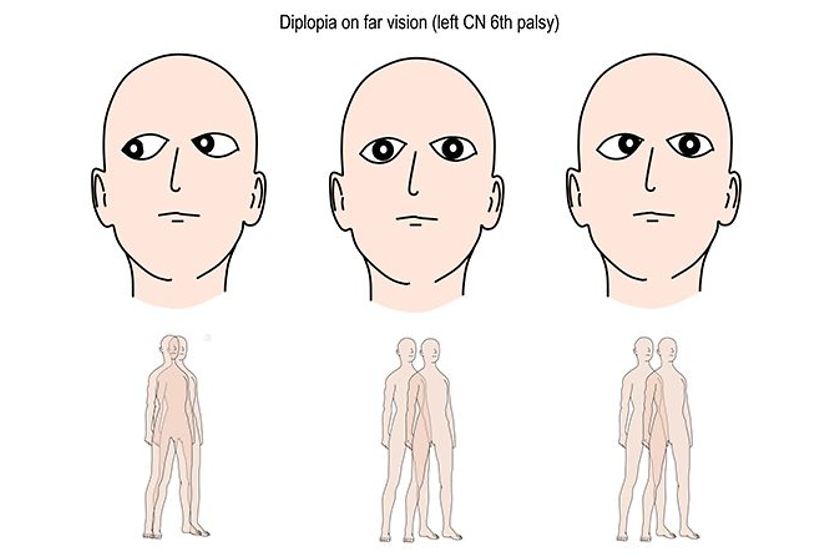
- Diplopia (double vision)
- Difficulty moving one or both eyes a certain way
- Difficulty swallowing
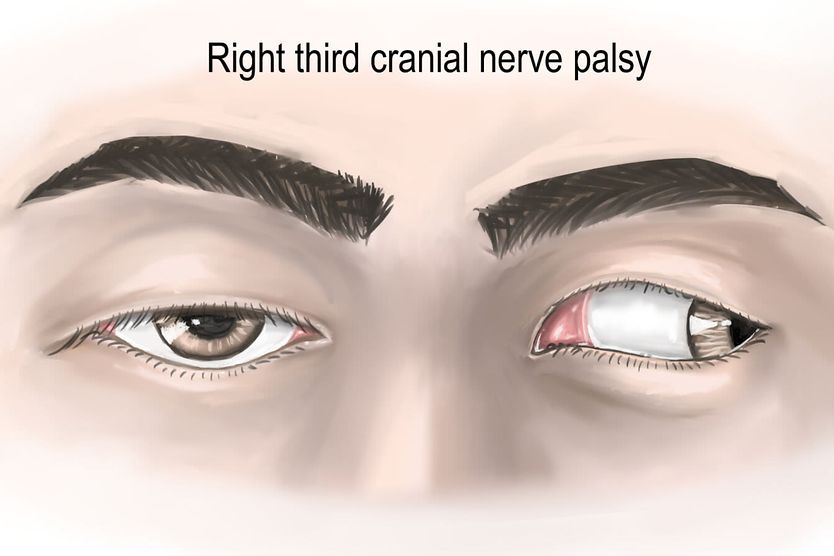
- Ptosis (droopy eyelid/s)
- General muscle weakness
It’s important to note that these symptoms may also be caused by eye conditions other than ophthalmoplegia. Your eye doctor can do an eye exam and tests to determine why you're experiencing these or other eye issues.
Types of ophthalmoplegia
An ophthalmoplegia diagnosis can sometimes be confusing to patients. That’s because doctors tend to use a number of different, lengthy words before or after the word ophthalmoplegia — these words and phrases are used to indicate various characteristics of the condition.
Such terms may tell you:
- Which eye muscles are being affected (internal vs. external ophthalmoplegia)
- What part of the brain is having problems sending signals to the eye muscles (supranuclear vs. internuclear ophthalmoplegia)
- Whether the condition is chronic or progressive (chronic ophthalmoplegia or progressive ophthalmoplegia)
- If the condition affects one or both eyes (unilateral vs. bilateral ophthalmoplegia)
If you get a diagnosis of ophthalmoplegia, the name of your condition may include one or more of these terms. Your eye doctor will explain to you what your specific diagnosis means and will answer any questions you have about your condition.
External vs. internal ophthalmoplegia
Ophthalmoplegia cases may be broken into two main groups, based on whether the condition affects the external eye muscles (external ophthalmoplegia) or the internal eye muscles (internal ophthalmoplegia).
External ophthalmoplegia is a paralysis or weakness in one of six external muscles that work together to move the eye. These muscles allow the eye to move up, down, side to side and to roll in a circle.
The external type of this condition may affect any of these six external muscles (extraocular muscles) of the eye:
- Superior rectus – muscle attached to the top of the eye that moves the eye upward
- Inferior rectus – muscle attached to the bottom of the eye that moves the eye downward
- Medial rectus – muscle attached to the inside of the eye that moves the eye toward the nose
- Lateral rectus – muscle attached to the outside of the eye that moves the eye toward the ear
- Superior oblique – muscle that rotates the eye inward and downward
- Inferior oblique – muscle that rotates the eye outward and upward
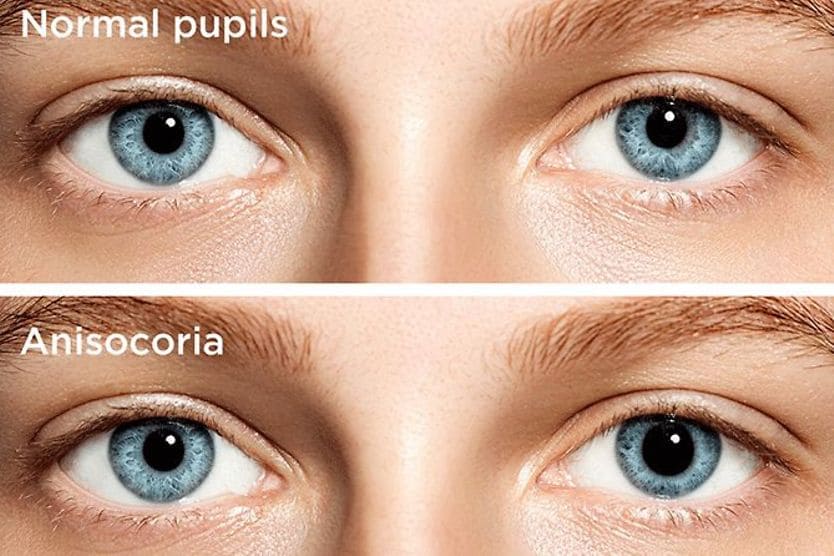
Internal ophthalmoplegia is a paralysis or weakness in one of three internal muscles that help the eye to focus and control pupil size.
This type may affect any of these three internal muscles (intraocular muscles) of the eye:
- Ciliary muscle – ring of muscle that controls the shape of the lens to allow the eye to focus on nearby or faraway objects
- Dilator pupillae – muscle that increases the size of the pupil to allow in more light
- Sphincter pupillae – muscle that reduces the size of the pupil to allow in less light
The specific type of ophthalmoplegia you may be diagnosed with will depend on factors such as: which eye muscle is affected, the cause of the condition, whether it is progressive and whether it affects one or both eyes.
Chronic progressive external ophthalmoplegia
Chronic progressive external ophthalmoplegia (CPEO) is the type of this condition that’s caused by a genetic mutation. Symptoms typically begin between the ages of 18 and 40. The condition may affect one eye (unilateral) or both eyes (bilateral).
Patients with chronic progressive external ophthalmoplegia may experience weakness in the eye muscles, droopy eyelids, difficulty swallowing (dysphagia) and general weakness in the arm, leg or neck muscles, especially after exercise.
Chronic progressive external ophthalmoplegia may be caused by different gene mutations. Inheritance patterns vary based on those mutations.
In some cases, CPEO may occur as part of another condition. For example, it may occur with two rare neuromuscular disorders: ataxia neuropathy spectrum or Kearns-Sayre syndrome. Patients with either may experience additional symptoms related to those conditions.
Internuclear ophthalmoplegia
Internuclear ophthalmoplegia is commonly caused by changes in the brain from MS or from a stroke. The term "internuclear" refers to the part of the brain that is affected, an area that serves as a pathway between the nuclei, two clusters of nerve cells in the brain.
About 23 percent of MS patients experience internuclear ophthalmoplegia. Other conditions that may lead to internuclear ophthalmoplegia include: infections (such as HIV or syphilis), trauma or tumors (such as glioma or medulloblastoma).
This type of ophthalmoplegia is caused by a lesion on a part of the brain known as the medial longitudinal fasciculus (MLF). The MLF is a tract of fiber in the brain that transmits information between the brain and the eyes. The information transmitted by the MLF helps muscles to coordinate eye movements.
Internuclear ophthalmoplegia may occur in one eye (unilateral internuclear ophthalmoplegia) or both eyes (bilateral internuclear ophthalmoplegia).
Supranuclear ophthalmoplegia
Many people with supranuclear ophthalmoplegia have progressive supranuclear palsy (PSP), a rare brain disorder that causes muscle weakness, walking difficulty and other symptoms. The term "supranuclear" refers to the part of the brain that is affected, an area above the nuclei.
Supranuclear ophthalmoplegia also may be called progressive supranuclear ophthalmoplegia to reflect the fact that the condition is progressive — that means the condition can get worse over time and there is no cure.
Treatment for ophthalmoplegia
Treatment and therapies for ophthalmoplegia can vary depending on the age of the patient, the type of ophthalmoplegia and cause of the condition.
Children or adults who have double vision from ophthalmoplegia may get an eye patch or special glasses — for example, some may wear eyeglasses with "stilts" that can hold up droopy eyelids.
Some patients may benefit from surgery to correct a specific issue; these procedures include ptosis surgery or strabismus surgery.
In some cases, treatment for the underlying condition may help to improve symptoms of ophthalmoplegia.
Regular eye exams for ophthalmoplegia
It's important to get regular eye exams to monitor eye health and catch issues early. An eye doctor can perform a comprehensive exam, do any necessary tests and diagnose ophthalmoplegia.
If you have any symptoms of this condition, make an appointment with your eye doctor as soon as possible for a comprehensive eye exam. You may also need to see a specialist (for example, a neurologist) and undergo diagnostic testing, such as an MRI, to determine the cause.
Treatment for any underlying condition may also be recommended. Your eye doctor will monitor your eye health and develop a treatment plan to address any vision issues caused by ophthalmoplegia.
READ NEXT: Bell's palsy: Causes, symptoms and treatment