What is metamorphopsia?
Metamorphopsia is vision dysfunction that causes objects — specifically straight lines — to appear warped, distorted or bent. Rather than a condition itself, metamorphopsia is a symptom. It can result from brain conditions or when there’s a problem with the macula, which is the center of the retina.
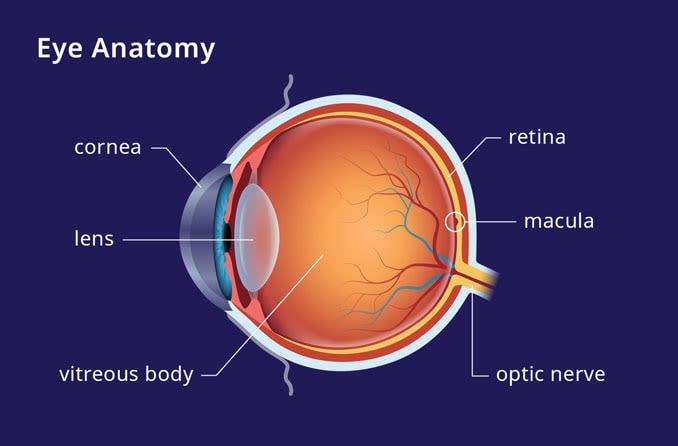
The retina is a thin layer of tissue at the back of the eye that uses light to create signals. Signals are sent to the brain through the optic nerve and registered as an image. The macula is in the middle of the retina and gives us color vision, central vision and visual acuity.
When the retina or macula are affected by age, trauma or disease, metamorphopsia can result. It may affect one or both eyes and may only involve a portion of the vision in the affected eye. Metamorphopsia can potentially indicate the presence of a serious underlying medical cause.
What causes metamorphopsia?
Metamorphopsia can be caused by a problem with the eye or the brain. Usually, when an eye-related problem is causing distorted vision, it only occurs in one eye. Some eye-related problems that could cause metamorphopsia include:
Age-related macular degeneration
Age-related macular degeneration (AMD) is a condition that affects the macula. There are two types of AMD: wet and dry.
In people with wet AMD, abnormal blood vessels grow under the retina and leak blood and fluid. In dry AMD, cells in the macula slowly deteriorate. It’s unknown what triggers the cell deterioration.
Retinal hemorrhage
A retinal hemorrhage happens when blood vessels in the retina start to bleed. Some diseases, such as diabetes and hypertension, can damage the blood vessels and cause the bleeding to start. Other causes of a retinal hemorrhage include eye trauma, head injury or a sudden change in air pressure.
Macular hole
Macular holes are a relatively rare occurrence that can happen as a result of aging. They occur when the macula gets pulled or stretched during vitreous detachment — an age-related vision change.
If pulled too suddenly, a hole can be torn in the macula. It’s possible for the hole to be small enough that immediate treatment isn’t needed. However, macular holes can get bigger over time and cause more damage to your vision.
SEE RELATED: Tunnel vision
Vitreomacular traction
Vitreomacular traction is similar to a macular hole in that it’s caused by vitreous detachment. However, with vitreomacular traction, the vitreous gets caught on the macula as it’s detaching. The vitreous then pulls on the macula, which can cause metamorphopsia to occur.
Vitreomacular traction may or may not result in a macular hole.
Retinal detachment
Another complication of vitreous detachment and potential cause of metamorphopsia is retinal detachment. During vitreous detachment, the gel that gives our eyes their shape (vitreous) pulls away from the surface of the retina.
Normally, this process happens with no problems. However, it’s possible for the vitreous to tug on the retina, create a rip or hole in it, and pull the retinal tissue from the back of the eye. When this happens, it can cause flashes of light, floaters and metamorphopsia, among other symptoms.
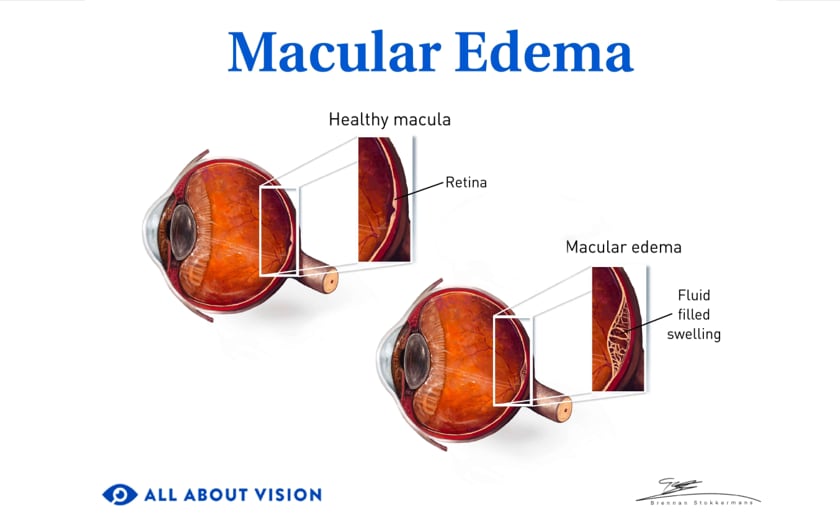
Macular edema
Macular edema is characterized by a buildup of fluid in the macula. Fluid comes from damaged blood vessels in the retina that begin to leak due to conditions like wet AMD and diabetic retinopathy. The leaked fluid that collects in the macula causes it to swell, which results in distorted vision.
Retinal vasculitis
Retinal vasculitis describes the inflammation of retinal vessels. It can occur on its own or as a result of another inflammatory disease. It is a sight-threatening condition that can cause metamorphopsia.
SEE RELATED: Eye floaters
Ocular histoplasmosis
Ocular histoplasmosis is when the fungal infection histoplasmosis spreads to the eyes. Histoplasmosis is a fungus found in bird and bat droppings, with spores that are typically inhaled and create infection in the lungs.
If the infection spreads to the eyes, causing ocular histoplasmosis, it can lead to vision complications. This includes abnormal blood vessel growth on the choroid, beneath the retina, which can cause metamorphopsia.
Epiretinal membrane (macular pucker)
An epiretinal membrane, also called a macular pucker, is a thin layer of tissue that grows over the macula. The membrane is opaque and resembles scar tissue, making it difficult to see through.
It’s possible for the membrane to shrink, which can pull on the macula and cause it to wrinkle or pucker. This disruption in the macula can cause vision distortion.
High myopia
High myopia, or severe nearsightedness, is categorized as having a vision prescription of -6.00 diopters or higher. The condition is caused by having eyes that are more elongated than average.
As the eyes elongate, the retina at the back of the eye can become stretched. Over time, this may cause cells in the macula to wither away and die, which can cause blind spots and distorted vision.
Central serous chorioretinopathy
Central serous chorioretinopathy occurs when fluid leaks from the choroid — the tissue layer below the retina. As this fluid builds up between the choroid and the retina, it can cause a small retinal detachment and vision distortion.
SEE RELATED: Blurry vision in one or both eyes
Migraine
Migraine is a neurological condition that is characterized by severe pain that’s focused on one side of the head. Before a migraine begins, many people experience a migraine aura.
A migraine aura is like a warning sign that a migraine is about to happen. It often involves visual symptoms, like flashes of light, zigzags or blind spots in vision, and metamorphopsia.
There have also been rare cases of migraine auras causing brief spells of visual hallucinations, where certain objects look larger or smaller than normal. This is known as Alice in Wonderland syndrome.
Drug use
Metamorphopsia, among other serious vision problems, has been linked to a drug known as “Poppers.” The drug is made up of various nitrite compounds and is usually inhaled.
When inhaled, the chemicals in Poppers can damage cells in the fovea, which is located in the macula. This is known as “Poppers maculopathy.” It can cause decreased visual acuity, blind spots in your central vision, metamorphopsia and phosphenes.
Peduncular hallucinosis
Peduncular hallucinosis is a rare cause of visual hallucination. Someone with this condition can have vibrant, colorful visions of various animals, objects or people. Metamorphopsia is described by some people experiencing peduncular hallucinosis.
Those with peduncular hallucinosis are aware that the hallucinations are not real, and, generally, the hallucinations are not felt to be threatening. They do not experience hallucinations in any other sensory modalities (such as hearing or smell). Experts are still trying to understand the exact cause of peduncular hallucinosis. It’s suspected that most cases are related to lesions in the midbrain.
Occipital lobe epilepsy
Occipital lobe epilepsy is a rare form of epilepsy in which abnormal electrical activity in the brain affects a person’s vision. Focal seizures in the occipital lobe can present with visual hallucinations and/or metamorphopsia as manifestations.
These types of seizures (or sensory seizure auras) may be mistaken for a migraine, as the symptoms are similar. One clue can be that focal sensory visual seizures usually last less than two minutes, whereas migraines can last hours or days.
SEE RELATED: Visual agnosia
Is metamorphopsia the same thing as macular degeneration?
No, metamorphopsia is not the same thing as macular degeneration. Macular degeneration is a disease that can cause the symptoms of metamorphopsia (distorted vision), but not all people experiencing metamorphopsia have macular degeneration. Many other issues can also cause distorted vision, not just macular degeneration.
What does metamorphopsia look like?
Metamorphopsia affects central vision. This means objects in your peripheral vision will likely appear normal, while things in front of you are distorted. While metamorphopsia is a symptom in itself, some signs to look out for include:
- Objects that are normally straight appear curved or warped. Example: A light pole looking bent or “melted.”
- Things that are normally flat appear rounded. Example: A frisbee looking like a bowl.
- Borders on objects appear smudged or distorted. Example: The face of a watch looks like someone smeared the edges of it.
- Objects change shape. Example: A rectangular door frame twists out of shape.
- Things look disproportionately larger than normal (macropsia).
- Things look disproportionately smaller than normal (micropsia).
If you experience any of the symptoms listed above without explanation, seek help from an eye doctor or medical professional.
How is metamorphopsia diagnosed?
Your eye doctor may run a series of tests to determine whether you have metamorphopsia and how severe it is. The tests usually involve having the patient look at some type of chart and answering questions about what they see. Some tests used to measure metamorphopsia include:
Amsler grid
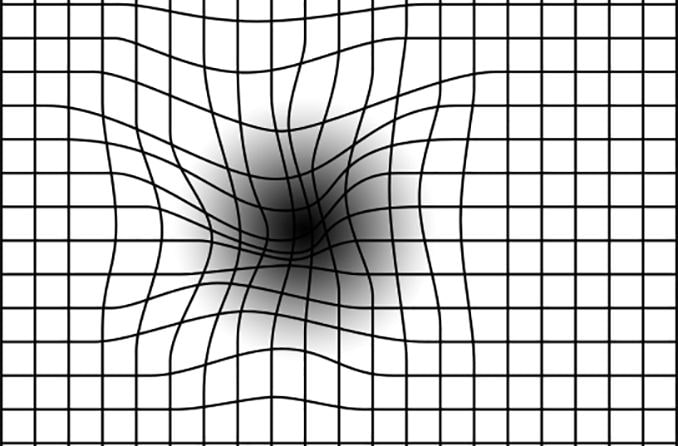
Amsler grid for metamorphopsia is the most well-known and the commonly used test that eye doctors use. It involves looking at a box with equally spaced horizontal and vertical lines that create a grid. In the middle of the grid is a small dot.
To take the test, the patient must be wearing corrective lenses, reading glasses or whatever is required for them to have their best corrected vision. Then, they focus on the dot in the middle of the grid while covering one eye at a time. This part is especially important, as looking at the grid with both eyes can cause the good eye to compensate for the bad eye.
While focusing on the dot in the middle, the patient should pay attention to how the lines around the dot appear. If they still appear straight, metamorphopsia isn’t the problem. If these lines appear curved or warped, metamorphopsia may be the problem.
M-chart
The M-chart is more specific than the Amsler grid, but it isn’t used as often. It was created to help pinpoint the degree of metamorphopsia and whether the distortion is more present in horizontal or vertical lines.
The test has 19 dotted lines, starting with a straight line (zero degrees). The size and space between the dots that create the line gradually go from very fine (0.2 degrees) to coarse (2.0 degrees). Each line has a dot in the middle of it that the patient is supposed to focus on.
Starting with the straight, solid line, the patient will focus on the dot and tell the eye doctor whether the line looks curved in places or not. They do this for every line, from fine to coarse, until the line no longer looks distorted to the patient.
Once this is recorded, the eye doctor will turn the M-chart 90 degrees (making vertical lines horizontal or vice versa). The patient will perform the test again.
The farther the patient goes before the line no longer looks curved, the more severe their metamorphopsia is. It’s also recorded whether vertical or horizontal lines are affected more than the other.
SEE RELATED: Commotio Retinae
Preferential hyperacuity perimeter (PHP)
This test is done on a computer screen. During the test, a dotted line will appear very quickly (less than a second). Somewhere along the line, a few dots will be misaligned to create a little bump or curve in the line.
The patient will use a stylus pen to tap the screen in the place they saw the most prominent distortion in the line. A preferential hyperacuity perimeter test usually takes about 3 to 5 minutes and uses the patient’s responses to measure 500 retinal data points.
These data points are then compared to a baseline. From this, eye doctors can pinpoint the relative location in the retina where the problem is.
SEE RELATED: Visual field testing for glaucoma and other eye problems
How is metamorphopsia treated?
Metamorphopsia is a symptom of an underlying problem, so its treatment depends on what’s causing it.
Many of the possible causes of metamorphopsia can be treated with surgery or medication. Once a eye doctor confirms a diagnosis, they can determine your treatment options.
When to see a doctor
It may take a few times experiencing metamorphopsia before you realize something is off. If distorted vision is something you experience regularly or constantly, seek medical attention.
Regardless of whether your metamorphopsia is caused by a problem with the eye or the brain, leaving it untreated can have serious health consequences. Discuss any changes or abnormalities in your vision with your eye doctor.
READ MORE: 9 causes of dizziness and blurred vision