Parinaud syndrome (dorsal midbrain syndrome)
Parinaud syndrome (also called Parinaud’s syndrome and dorsal midbrain syndrome) is a rare neurological disorder that causes upward gaze palsy (the inability to gaze upward). It can also include convergence-retraction nystagmus, bilateral eyelid retraction and light-near dissociation of the pupils.
The condition was named for a French ophthalmologist named Henri Parinaud, who discovered it in the late 1800s.
Signs of Parinaud syndrome

Left eye turned inward due to Parinaud syndrome. [Image credit: Parinaud oculoglandular syndrome. Permission granted by © 2022 American Academy of Ophthalmology]
There are three major ways that Parinaud syndrome presents itself in patients. This includes a “triad” of upward gaze palsy, convergence-retraction nystagmus and light-near dissociation of the pupils. Up to 65% of patients display all three.
Another primary sign of Parinaud syndrome is bilateral eyelid retraction. But it is much less common than the three conditions mentioned above.
Upward gaze palsy
The most prominent sign of Parinaud syndrome is an upward gaze palsy. This is when a person is unable to look upwards. Patients often develop a chin tip upward in order to get the eyes out of the restricted upward gaze. Between 87% and 100% of Parinaud syndrome patients experience upward gaze palsy.
Since they can’t look up, many patients default to gazing downward. (When someone has a primary downward gaze, it is referred to as the setting-sun sign or sunset eyes).
Convergence-retraction nystagmus
Nystagmus is a condition in which the eyes move or shake involuntarily. It is seen with many eye and neurological problems, including Parinaud syndrome.
Many patients with Parinaud syndrome experience a specific type of nystagmus called convergence-retraction nystagmus. With this variety, a person’s eyes converge and retract when they try to look upward.
Convergence-retraction nystagmus occurs due to damage in the fibers of the midbrain. Experts believe that 35%-88% of patients with Parinaud syndrome experience convergence-retraction nystagmus.
SEE RELATED: Types of nystagmus
Light-near dissociation of the pupils
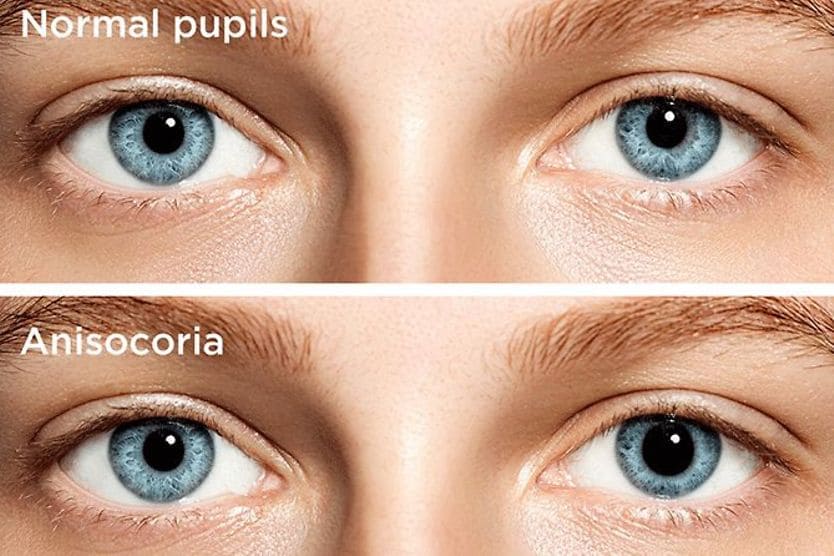
Light-near dissociation is a condition in which the pupils have a delayed response to light (the pupils do not constrict). But they have a normal response when viewing something up close (the pupils do constrict).
This can occur when lesions in the midbrain interfere with the pupillary light reflex. Between 65/% and 96% of patients with Parinaud syndrome have light-near dissociation of the pupils.
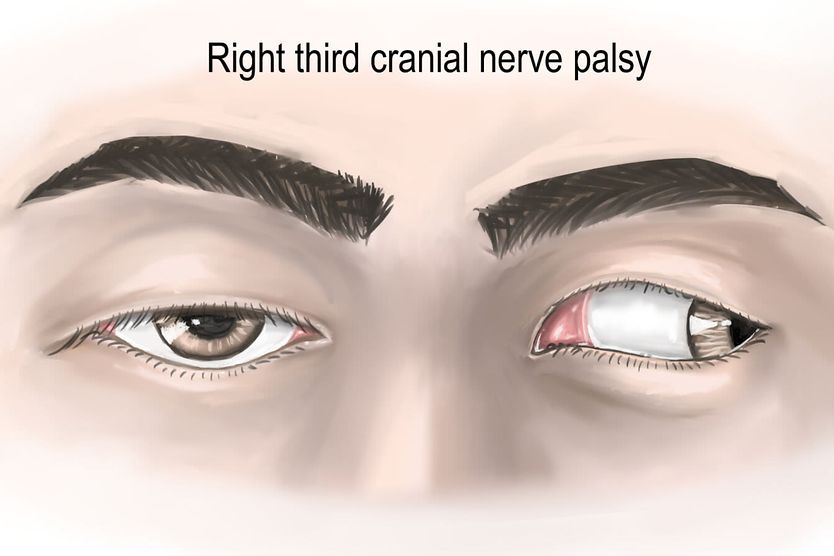
Bilateral eyelid retraction
Some patients also experience a bilateral eyelid retraction. This is when the upper and/or lower eyelids retract while the eyes are in a resting position. It’s also referred to as Collier’s sign, and it affects up to 40% of people with Parinaud syndrome.
Symptoms of Parinaud syndrome
In addition to these major signs, there are several symptoms of Parinaud syndrome that patients often experience. Many of these symptoms occur secondary to the nystagmus that is present.
These can include:
- Blurred vision
- Nausea and vomiting
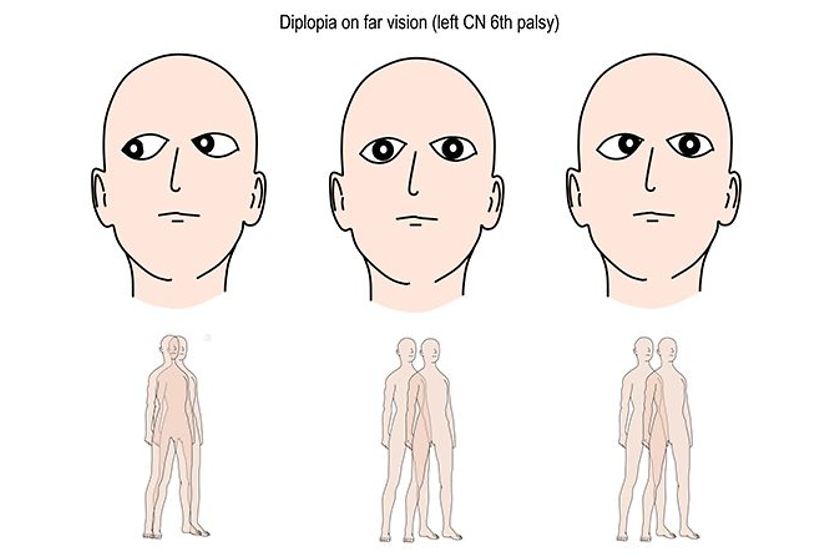
- Diplopia (double vision)
- Ataxia (feeling off-balance)
- Oscillopsia (feeling as though stationary objects are constantly moving)
Causes
When looking at the causes of Parinaud syndrome, it’s important to understand certain parts of the brain, including the midbrain and the pineal gland.
The midbrain is a part of the brainstem. The brainstem connects the cerebrum (the largest part of the brain) to the spinal cord and cerebellum. The midbrain also contains many structures that control things like vision, hearing, moving and coordination. Since problems in the midbrain can lead to Parinaud syndrome, the condition is sometimes referred to as dorsal midbrain syndrome.
The pineal gland is the part of the brain that responds to light and darkness. It also produces melatonin, which is the sleep hormone in the body. It is located deeper in the brain than the midbrain.
If there is an abnormality in either of these structures, it can contribute to Parinaud syndrome and other vision problems.
As for the direct causes and/or origins of Parinaud syndrome, they may include:
- Pineal gland tumors (said to be the most common cause)
- Lesions in the midbrain
- Hemorrhages occurring in the midbrain
- Multiple sclerosis
- Encephalitis (inflammation of the brain)
- Obstructive hydrocephalus (excessive fluid in the brain)
- Trauma
- Infection
- Arteriovenous (AV) malformations (a group of blood vessels that didn’t form correctly in the brain or spine)
Older patients’ conditions tend to be influenced by vascular (blood vessel) issues. Younger patients are more impacted by neurologic (tumors and abnormal growth) factors.
SEE MORE: Eye symptoms commonly seen in multiple sclerosis
Diagnosis
Parinaud syndrome is diagnosed through a series of tests by your eye doctor. A comprehensive eye exam is performed to identify any vision-related problems. This includes visual acuity testing, visual field tests, and retinal and pupillary exams.
MRIs and other neuroimaging tests are also recommended, since Parinaud syndrome is a neurological condition.
Your eye doctor may refer you to a neuro-ophthalmologist (focusing on complex vision problems related to the nervous system) or a neurologist.
Treatment and outlook
The treatment for Parinaud syndrome is targeted toward the underlying condition. Whether caused by trauma, infection, pineal gland tumor or otherwise, treatment should be prompt to prevent further damage.
Treatment begins with a proper refractive error correction. If necessary, prism can be added to the glasses to address the upward gaze palsy or diplopia (double vision). For patients whose vision and mobility are affected by the gaze palsy, an eye muscle surgery may be prescribed.
Annual eye exams are important for everyone in order to detect and treat any existing vision problems, both simple and complex. But, if you believe you may be experiencing Parinaud syndrome, it is recommended to seek urgent care to address the issue.
READ NEXT: What is a neuro-ophthalmologist?