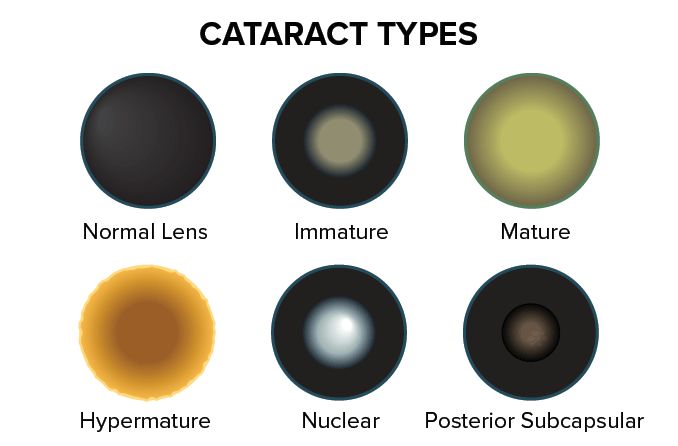
Nuclear
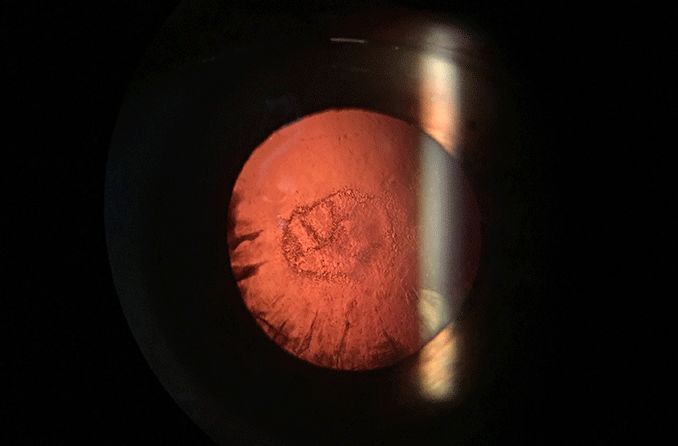
A nuclear cataract happens inside the center of the lens. Most are caused by aging.
It starts when the inside of the lens gets hazy and hardens. This is called nuclear sclerosis; it's a normal part of getting older. After a while, nuclear sclerosis can become a nuclear cataract.
Cortical
A cortical cataract develops along the edge of the lens.
At first, it looks like white wedges or spokes on a wheel. It slowly spreads farther into the center of the lens and blocks more light.
Posterior subcapsular
A posterior subcapsular cataract is on the back side of the lens, opposite your pupil.
It usually develops faster than nuclear and cortical cataracts. This type is often associated with diabetes.
Anterior subcapsular
An anterior subcapsular cataract develops on the front side of your lens, facing your pupil.
It's usually caused by eye injury, inflammation or irritation.
Traumatic
A traumatic cataract is usually caused by an eye injury. It can also happen after an electrical shock, exposure to certain chemicals or radiation, and other causes. But these are less common.
Some traumatic cataracts show up quickly after an injury or exposure. Others can take months to develop.
Snowflake
People with diabetes have a higher risk of developing eye problems, especially when their blood sugar isn't controlled very well. This includes different types of cataracts.
Diabetes can cause white spots shaped like a snowflake to form on the lens. Snowflake cataracts are rare, and they usually affect young people with Type 1 diabetes.
Christmas tree
A Christmas tree cataract is made of colorful specks shaped like a Christmas tree on the lens. They aren't white like most other cataracts.
This type is seen in many people who have a muscle disease called myotonic dystrophy. But it can affect other people, too.
Congenital
Some babies are born with congenital cataracts, but they're rare. They affect about 3 to 4 in every 10,000 newborns.
These cataracts can happen when a baby is born with one of several congenital disorders. They can also develop when the mother is exposed to certain infections, medicine or radiation while she's pregnant.
Secondary
Some people get a “secondary cataract” after cataract surgery. It isn’t a true cataract, but it has similar symptoms. It's common and can be treated with laser surgery.
READ MORE: A complete guide to different types of cataracts
How are cataracts diagnosed?
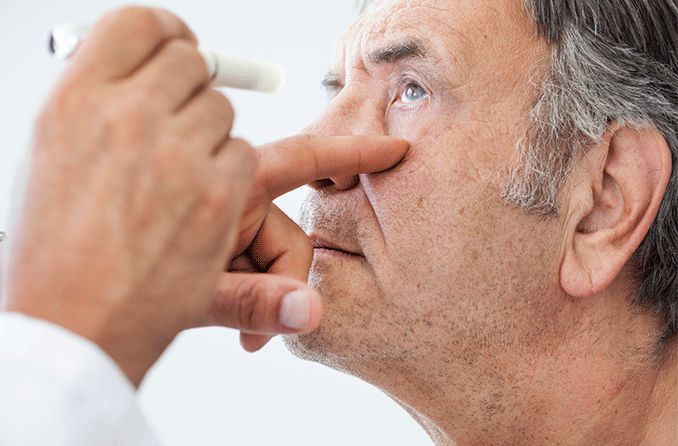
Eye doctors diagnose cataracts during an eye exam.
During the exam, your doctor will:
- Ask you to read letters on an eye chart to determine the sharpness of your eyesight.
- Shine a bright light into your eyes to look inside.
- Use eye drops to dilate your pupils to get a better view of your lens and inner eye.
Pupil dilation isn't painful, but it makes your vision blurry for a few hours. Your eyes will also feel sensitive to light, but the doctor will give you special sunglasses (if you don’t have them) so light doesn't hurt your eyes.
After the exam, your doctor will tell you if you have cataracts. If you had your eye exam with an optometrist, they might refer you to an ophthalmologist. Ophthalmologists are medical eye doctors licensed to perform eye surgery.
How to manage cataracts
You won't always need cataract surgery right away. If your doctor diagnoses a cataract early enough, you might be able to manage your symptoms for a while.
They might recommend that you:
- Update your vision prescription and use it to order new glasses or contact lenses.
- Wear eyeglasses or sunglasses with an anti-glare coating on the lenses.
- Use brighter lights around your home or workplace.
- Use a magnifying glass to read printed text.
- Increase the size of text on your phone or computer.
These temporary fixes may become less helpful as your cataract starts to block more light. This can make reading, driving and other everyday tasks feel more difficult. At this point, your doctor might ask you to consider surgery.
How can you treat cataracts?
Understanding cataract surgery
Surgery is the only proven way to treat cataracts and improve vision.
While the thought of any surgery can be scary, modern-day cataract surgery is generally safe and effective. It's the most common surgical procedure in the United States.
The goal of surgery is to remove the cloudy lens in your eye and replace it with a new one. The new lens, called an intraocular lens (IOL), is artificial, but it's designed to function like a healthy, natural lens. It's clear without any clouding.
Some optional advanced lens implants may help improve reading and computer vision with less need for glasses.
What to expect before, during and after the procedure
The procedure itself takes about 10 to 15 minutes. It is typically painless, and you'll go home the same day. You'll be awake during surgery, but the doctor will numb your eye. They can give you medicine to help you relax, too.
After the procedure, your vision will be blurry for a little while. You'll need to wear an eye shield and sunglasses to protect your eye while it heals.
Your eyesight will typically go back to normal within a few days to a few weeks.
Cataract prevention
There is no guaranteed way to prevent cataracts, but certain lifestyle changes could help lower your risk:
Protect your eyes from ultraviolet (UV) radiation from the sun
Make sure your sunglasses block 100% of UVA and UVB rays. This is sometimes labeled as "UV 400." Sunglasses should fit your face well and cover at least three-quarters of the light around your eyes (wraparound design).
Quit smoking
Quitting is never easy, but it can lower your risk of cataracts and improve your overall eye health.
Wear protective eyewear
Eye injuries can cause certain kinds of cataracts. Wear ANSI-standard safety glasses any time you're doing a high-risk activity.
Eat a healthy diet with lots of produce
Fruits and vegetables contain good chemicals called antioxidants. They help slow some of the "wear and tear" that happens to your body as it ages. It might be tempting to take over-the-counter supplements instead, but studies show they probably can't help your eyes like healthy foods can.
Consider your alcohol consumption
Researchers still have a lot to learn about how alcohol affects cataracts. One study found that even small amounts of alcohol increased the risk of age-related cataracts. Other studies found a smaller effect or none at all.
Maintain target blood sugar levels
Diabetes can hurt your eyes and overall health when it isn't controlled well. Talk to your doctor about new ways to help you keep your blood sugar in the target range.
Cataracts in children
Congenital vs. acquired cataracts
Cataracts are more common in adults, but they can happen at any age. Studies show that 3 to 4 in every 10,000 newborns have cataracts that impact their vision.
While some cataracts are present at birth (congenital), others develop later in childhood due to injury, illness or genetics (acquired). Even if a baby is born with cataracts, the signs may not be obvious right away. These cases are often diagnosed months or years later when a parent notices a vision problem or a health care provider finds them during an exam.
You might notice one or more of these symptoms:
- Little or no reaction to light
- Sensitivity to bright light
- Problems noticing people, toys and other objects in their field of view
- Quick, uncontrolled eye movements
- Delays in their development
Many congenital cataracts don't have a clear cause. In some cases, they're connected with:
- A congenital disorder, such as Down syndrome
- A whole-body disease, such as diabetes
- An infection the mother had during pregnancy, such as rubella or herpes simplex
Injuries and trauma can cause cataracts in children, too. These are called acquired cataracts.
How they’re treated
Childhood cataracts are usually treatable, but a child might not need treatment right away. Their doctor will take their cataract type, age and overall health into consideration.
When to see an eye doctor
Cataracts are very common and rarely serious, but they can affect your everyday life in many ways. Schedule a comprehensive eye exam with an eye doctor any time you notice the signs of cataracts or any other vision problems.
Your doctor may be able to help you manage your symptoms for a while. If you need treatment, cataract surgery can help you see more clearly.