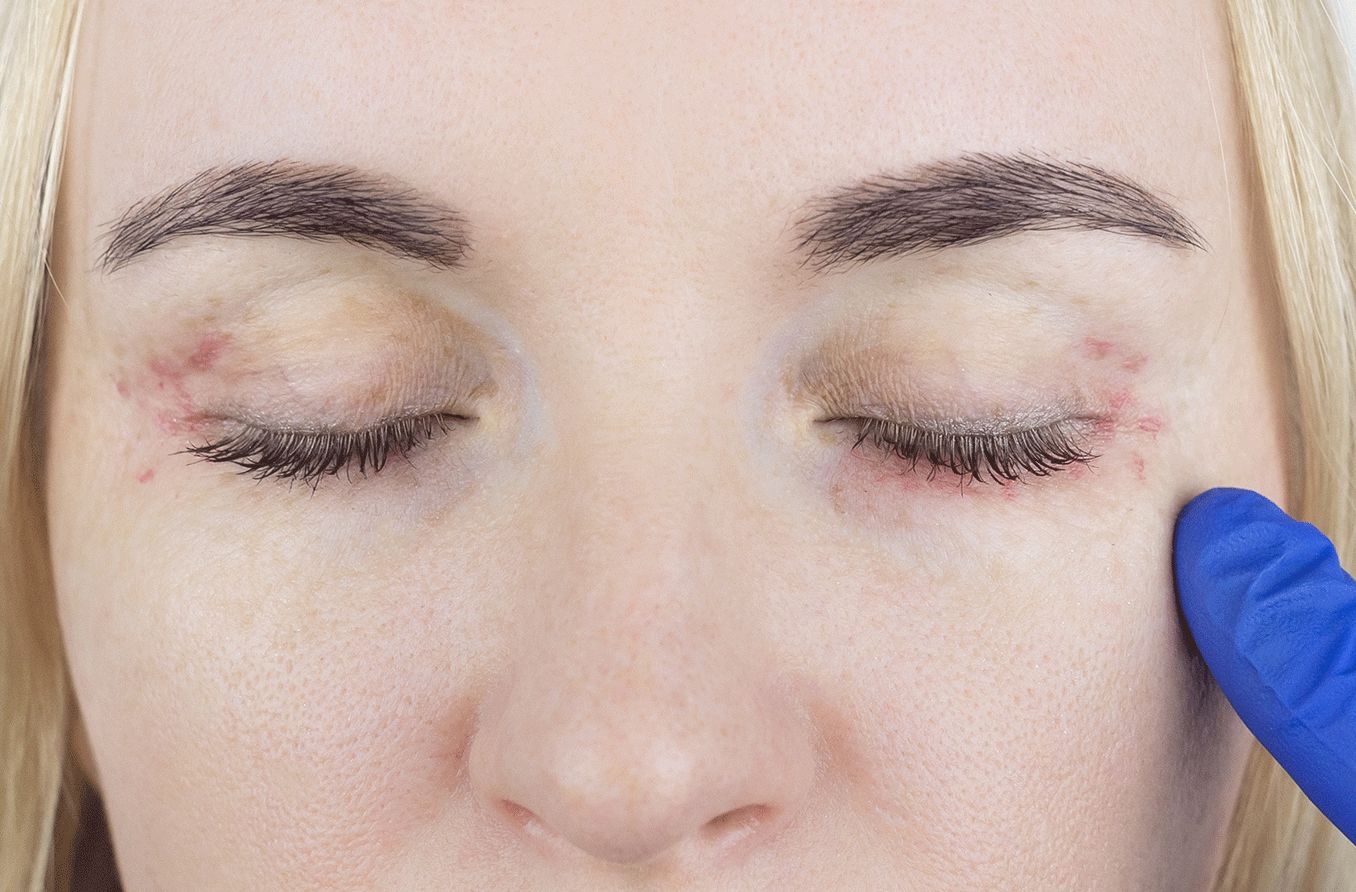
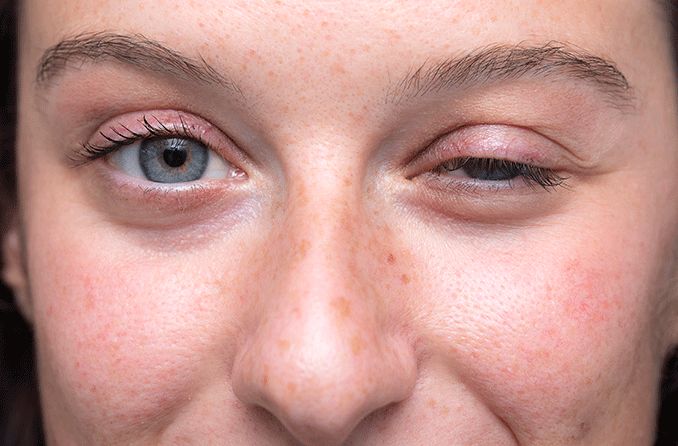
What is madarosis?
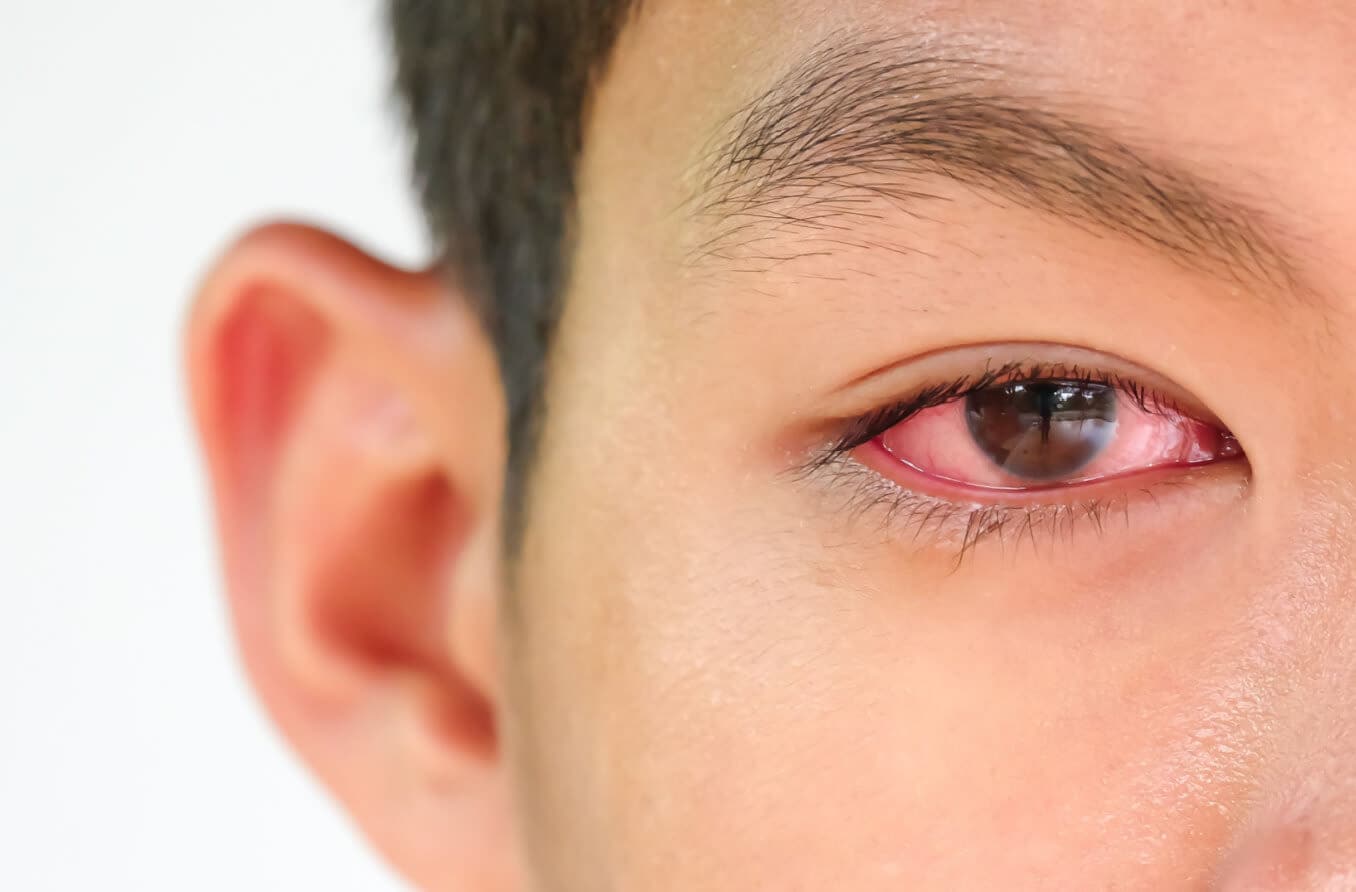
Madarosis is the medical term for the loss of eyebrow or eyelash hair. It is usually the result of another underlying eye, skin or health condition. Many cases of madarosis are often caused by eye conditions such as blepharitis or a local skin disorder.
Since madarosis can indicate the presence of another condition, it should be evaluated by a doctor when it is detected.
What is the difference between madarosis and superciliary madarosis?
Ciliary madarosis, also called milphosis, refers to the loss of eyelashes only. Superciliary madarosis indicates loss of eyebrows. The term “madarosis” is from the Greek word madao, meaning to fall off.
Eyebrows and eyelashes serve a protective function. Eyelashes protect our eyes from airborne particles. Eyebrows help to protect the bone above our eye socket and prevent sweat from trickling into our eyes.
Eyebrows are also important in conveying emotion and meaning in conversation. Both eyelashes and eyebrows visually enhance the features of our face. When there is a thinning or loss of eyebrows or eyelashes, not only are form and function affected, but so is an individual’s appearance.
Eyelashes grow very slowly, about 0.15 mm a day. They last for about half a year before they naturally fall out. If an eyelash is removed, it takes about 2 to 2 ½ months for a new lash to grow back. Eyebrows have a growth cycle of about 3 to 4 months.
What causes madarosis?
Since the underlying causes for madarosis are so varied, it is helpful to sort them into two categories — scarring and non-scarring.
This is a useful way to categorize madarosis because in scarring madarosis, there is no potential for hair regrowth. In non-scarring madarosis, there is potential for hair regrowth.
Non-scarring madarosis (hair regrowth possible)
The conditions that cause non-scarring madarosis do not destroy the hair follicle. This means that even though the hair has fallen out, it should grow back in a few months. Many of these conditions cause inflammation or hormonal disturbances that temporarily result in eyebrow or eyelash loss.
These conditions include:
- Blepharitis – This is a chronic inflammation of the eyelids.
- Seborrheic dermatitis – This is an inflammatory skin condition causing red, scaly skin.
- Psoriasis or atopic dermatitis – These are chronic skin conditions resulting in red, itchy skin.
- Alopecia areata – This is an autoimmune disease causing hair loss in patches.
- Rosacea – This is a chronic rash in the center part of the face.
- Herpes simplex – This is a viral infection causing cold sores.
- Thyroid hormonal disturbances – This includes hypothyroidism, hyperthyroidism or pituitary insufficiency.
- Drug induced – This is due to use of propranolol, miotics, anti-cholesterol, anticoagulants, chemotherapy drugs, retinoids, heparin and other medication.
- Radiation – This is due to a temporary disruption of certain phases of hair growth.
- Toxicity – This is due to thallium poisoning or excessive absorption of vitamin A.
- Nutritional deficiency – This is due to malnutrition, including lack of protein, zinc, iron or biotin.
- Secondary syphilis – This develops 2-8 weeks after primary syphilis.
- Trichotillomania – This is compulsive pulling out of one’s hair, including eyelash or eyebrow hair.
SEE RELATED: Do Eyelashes Grow Back?
Scarring madarosis (hair regrowth not possible)
The conditions that cause scarring madarosis destroy the hair follicle itself, rendering it unable to grow hair.
These conditions include:
- Trauma or burn – This can result in damage to the hair follicle.
- Discoid lupus erythematosus – This is a chronic skin disease causing scarring, hair loss and hyperpigmentation.
- Lepromatous leprosy – This is an infectious disease affecting the skin, nerves, respiratory tract and eyes.
- Lichen planopilaris – This is an inflammatory condition causing hair loss, pain and burning around scalp and hair.
- Folliculitis decalvans, tertiary syphilis and lupus vulgaris – These are inflammatory diseases that lead to follicle destruction.
- Malignant tumors – These are skin cancers such as squamous cell carcinoma or basal cell carcinoma that destroy the hair follicle.
- Congenital causes – This is an absence of eyelashes and eyebrows at birth.
How is madarosis diagnosed?
If a loss of eyelashes or eyebrows is noticed, it is important to be examined by a doctor as soon as possible.
History and lifestyle
The doctor will ask about your history and lifestyle. This is because factors such as family history, medication, allergy, poor nutrition or injury can all play a role in the progression of madarosis.
Medical conditions
Additionally, the doctor will ask if you are experiencing hair loss on other areas of the body. Hormone imbalance, skin disorders, medications and autoimmune diseases will cause hair loss throughout the body in addition to the eyebrow and eyelash area. If hair loss is present in other areas of the body, the doctor will order some diagnostic testing for underlying medical conditions.
Physical
The eyebrows, eyelashes and other areas of hair loss will be examined to determine:
- The degree of hair loss
- The location and pattern of hair loss
- Rate of hair loss and regrowth
- Presence of a local lesion or blepharitis
- Presence of skin irritation and inflammation
- Presence of trichotillomania
What is the treatment for madarosis?
The most effective madarosis treatment depends on the underlying cause for madarosis. If the disease causing the madarosis results in scarring of the hair follicle, regrowth of hair is not possible. Treatment options include a hair transplant or reconstruction in the area of hair loss. False lashes and tinting eyebrows are other options.
If the underlying cause for madarosis is non-scarring, the hair should generally grow back a few months after the condition is managed. (The exception is a form of leprosy that does not result in hair regrowth, although it is a non-scarring condition.)
Medications such as minoxidil solution can be used topically if the underlying cause is alopecia. Ocular drugs used to treat glaucoma, such as Latanoprost or Bimatoprost, have been reported to increase the length and thickness of eyelashes if the hair follicle is intact. Bimatoprost ( Latisse) has been approved by the FDA to grow, thicken and darken eyelashes in patients.
Since madarosis may be an indicator of a deeper medical problem, the first step is to treat and manage the disease that is causing madarosis. In addition to your internal medicine doctor, a team of doctors including an ophthalmologist, a dermatologist and an endocrinologist can work together to treat and manage the condition.