What is idiopathic juxtafoveal telangiectasia?
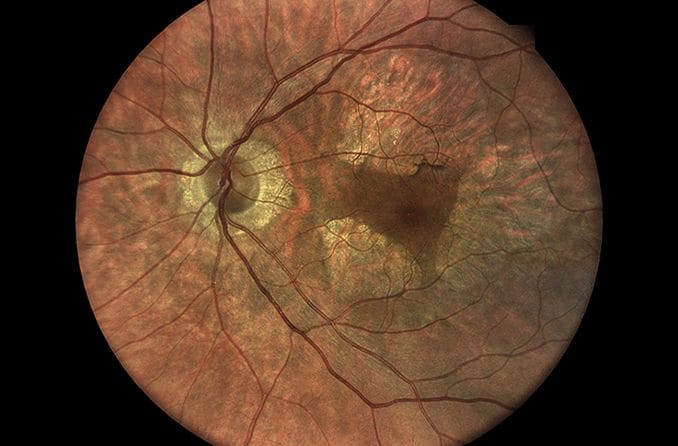
Idiopathic juxtafoveal telangiectasia, or macular telangiectasia (MacTel), is a rare condition that occurs due to abnormal, tiny blood vessels surrounding the fovea, the part of the retina that provides our most detailed vision. If left untreated, it can lead to distorted vision and vision loss.
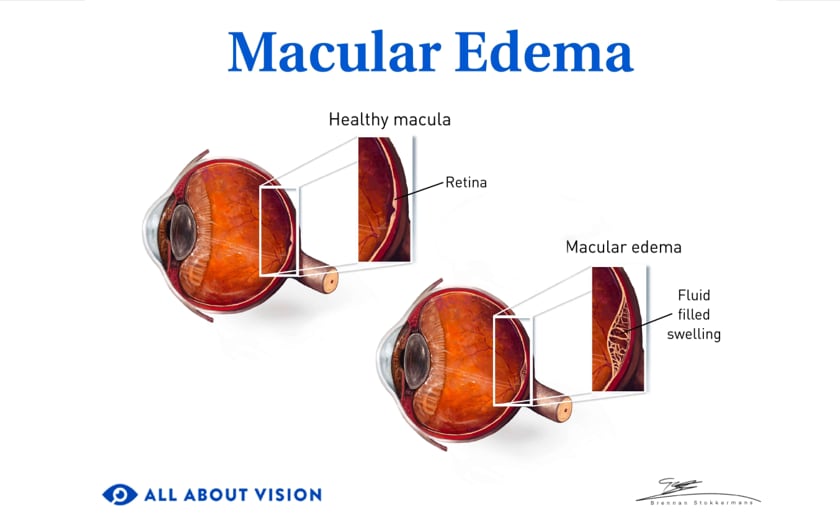
MacTel typically causes vision loss when blood vessels leak fluid or blood into the retina. This can damage the retina and cause swelling. It may also cause retinal cells to deteriorate or atrophy.

The condition occurs in three different forms. The most common, type 2, impacts middle-aged people and usually affects both eyes. Type 1, which impacts young people, usually only affects one eye.
MacTel usually progresses slowly, and most people maintain functional vision in at least one eye. During the early stages, some people may not experience symptoms and may only need to be monitored. Treatments address complications of the condition such as leaking blood vessels and macular edema.
Causes of macular telangiectasia
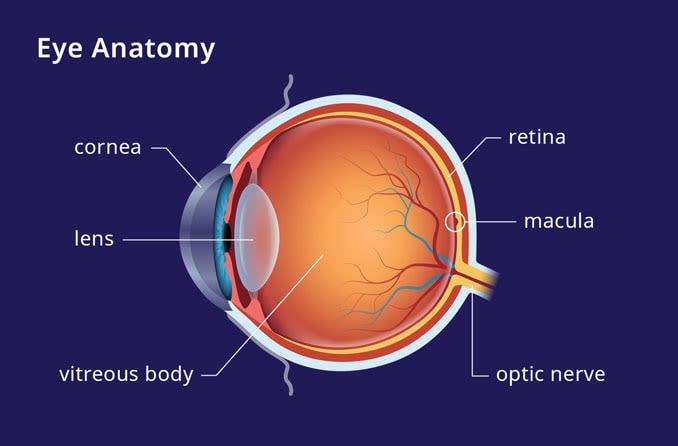
Idiopathic juxtafoveal telangiectasia is caused by abnormal, dilated blood vessels surrounding the fovea. The fovea provides our most precise vision and is located at the center of the macula, which lies on the retina, the light-sensitive tissue at the back of the eye.
Impact on the retina and vision
The fovea is surrounded by small blood vessels known as capillaries. This is why the condition is termed juxta foveal — the affected blood vessels are “near” the fovea. The center of the fovea has no blood vessels. Instead, it is nourished by an underlying network of blood vessels beneath it called the choroid. This allows light to pass without obstruction into specialized nerve cells in the center of the fovea — called cones.
These nerve cells, also known as photoreceptors, are responsible for color vision. They help provide detailed visual acuity, converting light into signals for the brain to process as images.
Peripheral vision is not usually affected in this condition because rods, the other type of photoreceptor cells, which are sensitive to low light levels, are concentrated in the retina’s outer edges.
Taking apart the term idiopathic juxtafoveal telangiectasia can help us to understand the condition further:
- Idiopathic – This means that there is no identifiable cause for the disease.
- Juxta – This means near or close to.
- Foveal – This is the center of the macula of the retina, which is responsible for detailed central vision.
- Telangiectasia – This refers to dilated and enlarged blood vessels that have abnormal branching and leak fluid or blood.
The dilated and swollen blood vessels form microaneurysms. These are small bulges in the blood vessels that can leak blood into the tissues of the retina. A buildup of blood and fluid can cause the macula to swell, known as macular edema.
The leaking fluids can damage the photoreceptors in the fovea and macula, impairing and distorting central vision.
Types of MacTel
Macular telangiectasia impacts the fovea and macula to varying degrees. Due to this, it is categorized into three different types. Type 2 is the most common, and types 1 and 3 are rare.
Type 1
Type 1 is less common and thought to be a variation of a condition called Coats disease. This is a rare disorder impacting young people and typically affects one eye. It causes abnormal development of retinal blood vessels. This is a congenital form of the condition, meaning it is present at birth. Signs include:
- Dilated blood vessels in the macula
- Development of microaneurysms
- Vision loss
Type 2
Type 2 is the most common. It usually impacts people in the fourth or fifth decade of life and typically affects both eyes. This form is associated with a higher occurrence of diabetes and high blood pressure. Signs and symptoms include:
- Dilated blood vessels in the macula begin to leak fluid, resulting in macular edema
- Development of microaneurysms
- New, abnormal blood vessel growth beneath the macula
- Distorted and impaired vision
LEARN MORE: Types of diabetic eye problems
Type 3
This is the most severe and uncommon type. It usually occurs in both eyes and results in progressive vision loss. It is associated with several systemic diseases, such as ulcerative colitis and some cancers.
What are the symptoms?
The severity and progression of symptoms vary depending on the type of MacTel. During the early stages, people with idiopathic juxtafoveal telangiectasia may not experience any symptoms. Peripheral vision is typically not affected because the disease damages the fovea and macula, which are responsible for central vision. Depending on how severe the condition is, symptoms can develop over 10 to 20 years. These include:
- Decreased visual acuity
- Distortion of vision
- Missing areas or blurry vision
How is the condition diagnosed?
A comprehensive eye exam is necessary to diagnose macular telangiectasia. This includes pupil dilation so that the retina can be seen clearly. The eye doctor looks for clinical signs such as abnormal blood vessel growth, bleeding and retinal scarring.
Additional procedures may be necessary to confirm and monitor the disease, including:
- Fluorescein angiography (FA) – In this procedure, fluorescein dye is injected into the arm. Within seconds, the dye moves through the body and into the eye’s retinal blood vessels, causing them to glow. A special camera takes pictures showing the location of leaking blood vessels.
- Optical coherence tomography (OCT) – This procedure provides 3D images of cross-sections of the macula and retina. It does not require an injection. It can be used to obtain a high-resolution retina scan to detect and monitor macular edema.
- Retinal photography – This allows doctors to analyze and document changes to the macula and retina.
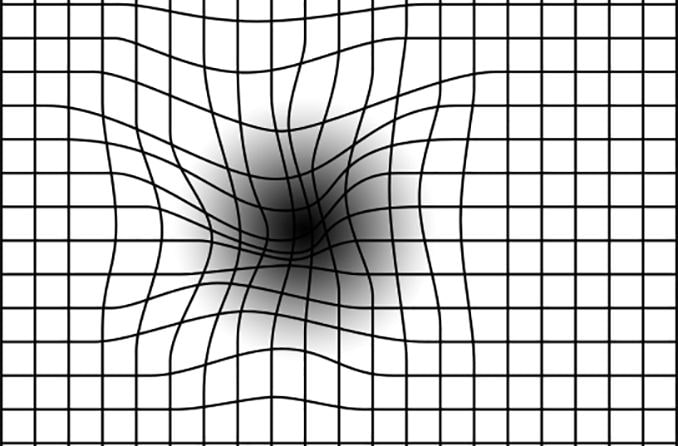
Your eye doctor will also check your central vision with an Amsler grid. This grid checks for distorted or blurred areas in your central vision. You may be asked to routinely check your vision with an Amsler grid at home. This allows you to contact your doctor and receive prompt treatment if you notice a sudden change in your vision.
READ MORE: How to choose an eye doctor
Treating and managing idiopathic juxtafoveal telangiectasia
At this time, there is no effective treatment for idiopathic juxtafoveal telangiectasia. Treatment is typically focused on decreasing vision loss from complications. Fortunately, some patients only need routine monitoring for changes to the retina.
If complications occur, such as the development of fluid and blood leakage into the retina or macular edema, the following medical or surgical treatments may be necessary:
Photodynamic therapy (PDT)
PDT treatment targets leaky blood vessels to reduce the amount of blood and fluid in the retina. A drug is injected into the arm and travels to the leaky blood vessels. It is activated by a low-power laser directed at these blood vessels, helping to seal them and reduce macular edema.
Anti-VEGF treatment
In some people with idiopathic juxtafoveal telangiectasia, excessive production of a chemical called VEGF — vascular endothelial growth factor — triggers the development of abnormal, leaky blood vessels. A series of anti-VEGF drugs directly injected into the eye treats leaky blood vessels and macular edema.
When to see a doctor
Someone who has been diagnosed with a type of idiopathic juxtafoveal telangiectasia should follow their eye doctor’s recommendations regarding follow-up visits to monitor their eyes. Early treatment is essential for reducing the risk of vision loss due to complications.
Routinely monitor your vision with an Amsler grid. Notify your doctor immediately if you notice a new onset of distorted or blurry vision or missing spots in your vision.
The MacTel Project
This international study and registry program was developed to enhance the understanding of macular telangiectasia (MacTel). It has over 30 centers around the globe. If you would like more information, please visit the MacTel Project website.
READ NEXT: Age-related macular degeneration (AMD): Causes, symptoms and treatments