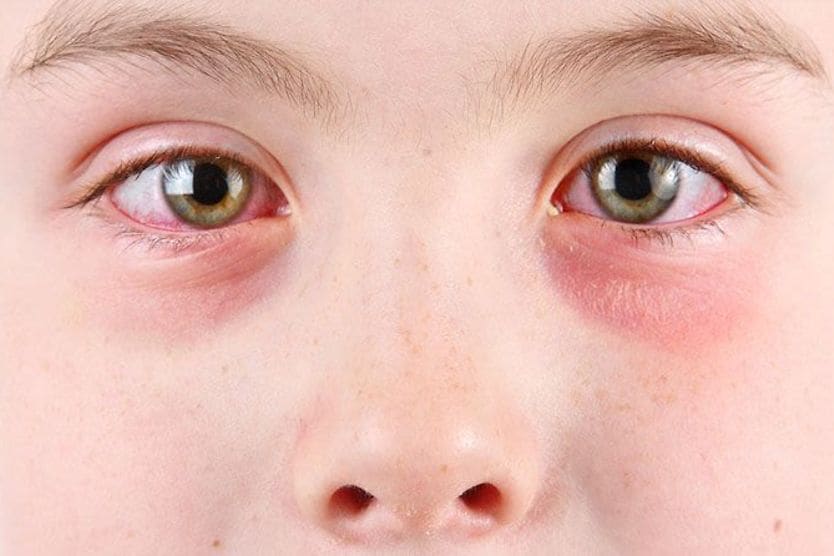
What is blepharoconjunctivitis?
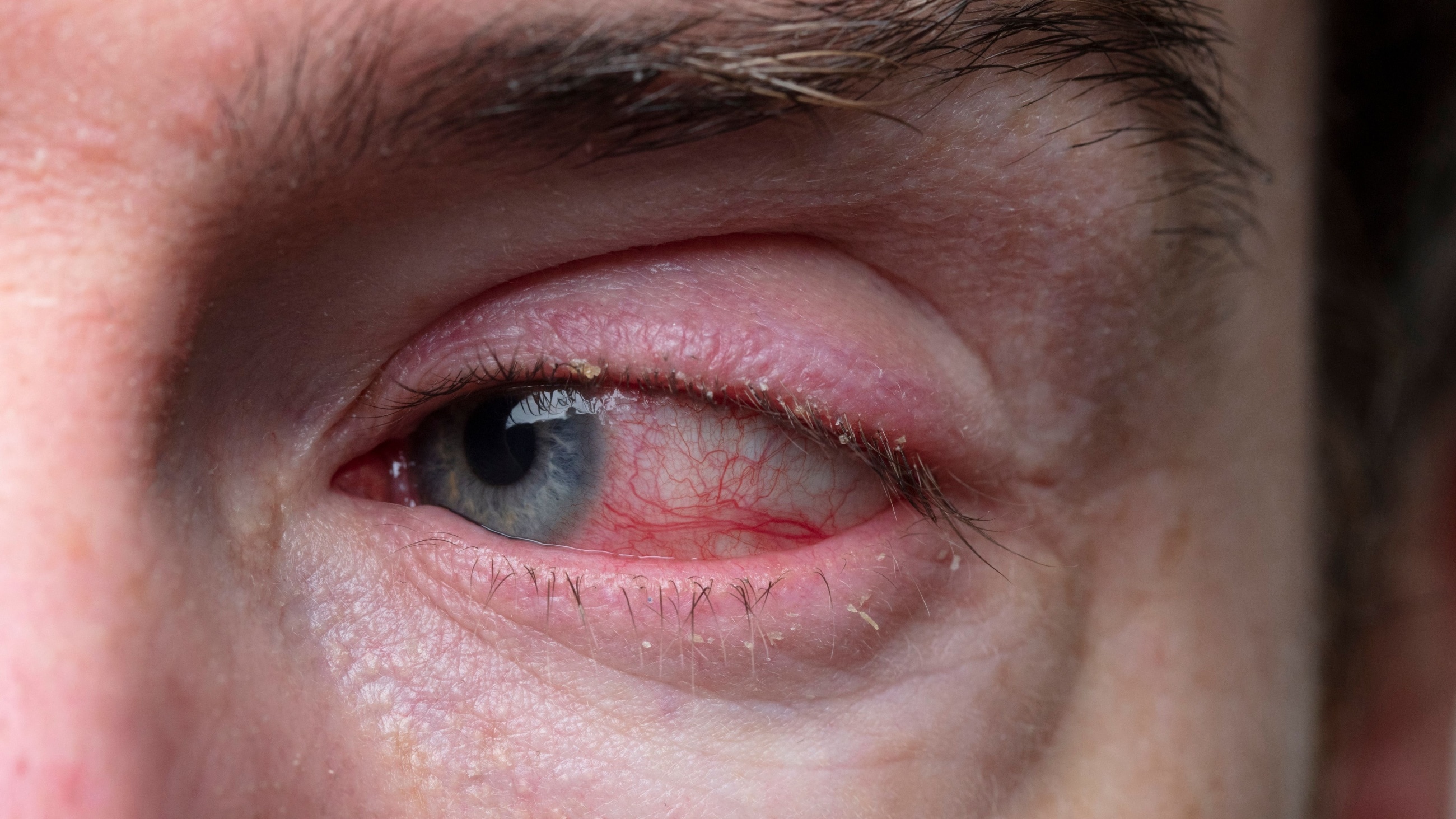
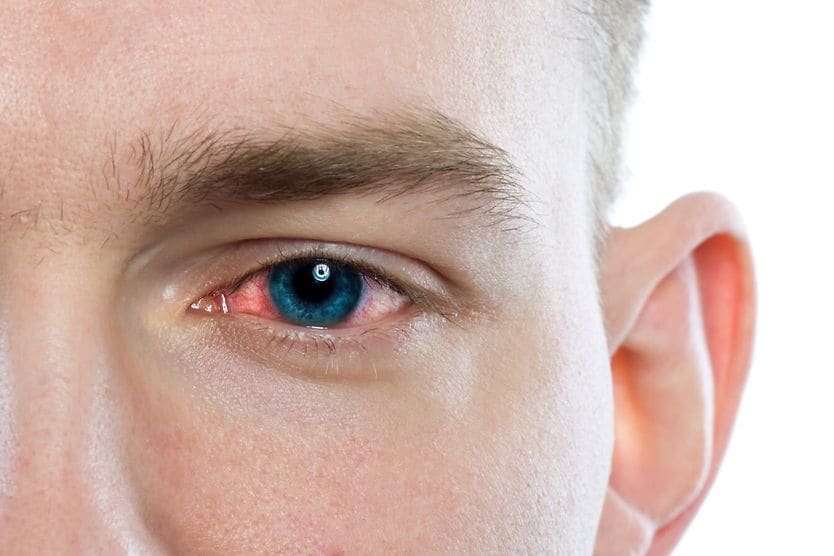
Blepharoconjunctivitis is a combination of blepharitis and conjunctivitis. Blepharitis causes crusty, red and swollen eyelids. Conjunctivitis causes inflammation of the clear lining which covers the white part of the eye (sclera) and the inside of the eyelids.
What causes blepharoconjunctivitis?
Blepharoconjunctivitis occurs due to inflammation and irritation. These can be caused by microorganisms, skin diseases, systemic health conditions, certain medications and underlying eyelid disorders. Some sources are more common than others.
Microorganisms
Staphylococcus aureus (the bacteria that causes staph infection). This is seen in acute (starting suddenly) infections of the eyelid and is caused by an overgrowth of bacteria. This bacterium can be resistant to penicillin and cephalosporin antibiotics — including methicillin. It is then called methicillin-resistant staphylococcus aureus or MRSA.
While MRSA blepharoconjunctivitis has become more common over the past two decades, it can still be treated with many other antibiotics.
Staphylococcus epidermidis, Corynebacterium and Propionibacterium acnes. These bacteria are normally present on the skin. Overgrowth of these bacteria will cause more chronic (long-lasting) infections.
Moraxella catarrhalis. These bacteria can cause sinus and ear infections in children. They also sometimes live in old makeup. This is considered an uncommon cause of blepharoconjunctivitis.
Demodex folliculorum. A skin mite that is normally present on the skin of the face. When present in larger numbers, it can cause acne rosacea — a condition that causes flushing and small pimples of the face and nose. It also causes Demodex blepharitis.
Molluscum contagiosum. This is a type of pox virus that causes small, smooth wart-like lesions on the skin and usually infects children. It can cause blepharoconjunctivitis when the lesions are close to the eye.
Monkeypox virus. This infection can also cause blepharoconjunctivitis when lesions are close to the eye or by touching a lesion and then touching the eye. While uncommon this can cause severe scarring of the cornea.
Phthiriasis palpebrarum. This occurs when lice infect the eyelid and attach to the base of the eyelashes.
Herpes simplex virus type 1 (and type 2). This is a common cause of cold sores around the mouth and on the lips. The virus usually occurs in the eye in patients who have already been exposed — usually as a child.
Skin and systemic health conditions
Allergies and atopic disease. Atopic disease is typified by eczema, asthma and allergies. It can cause thickening of the eyelids and cause wrinkling and darkening of the skin around the eyes.
Vitamin B6 deficiency. In rare cases, this deficiency may be associated with angular blepharoconjunctivitis. Other signs and symptoms of this deficiency are skin rash, a swollen tongue, confusion and irritability. Pinpricks and numbness of the hands and feet may also occur.
Down syndrome. Blepharoconjunctivitis, blepharitis, styes and excess tearing are all more common in people with Down syndrome.
Seborrheic dermatitis. This condition affects the skin in areas that are normally more oily. It can cause dandruff and a rash beside the nose, on the eyebrows and eyelids.
Medications
Dupilumab. This is a medication for eczema. Blepharoconjunctivitis may begin after the medication is started and typically goes away again once it is stopped.
Chemotherapy such as 5-fluorouracil. This is a treatment for cancer. It can cause blepharoconjunctivitis along with other diseases of the surface of the eye.
Isotretinoin. This is a treatment for acne. It can dry out the skin and block the formation of oils that are produced in the meibomian glands in the eyelid. Without these oils, the eye dries out, causing blepharoconjunctivitis.
Eyelid conditions
Ectropion and entropion. Aging, scarring, inflammation and allergies can cause the eyelid to tilt forward (ectropion) or fold inward (entropion). This allows bacteria to grow and may cause the eye to dry out and become inflamed as the folded eyelid rubs on the eye surface.
Floppy eyelid syndrome (FES). Aging, inflammation, excessive rubbing and being overweight can all cause the eyelids to become loose and more flexible. Floppy eyelid syndrome may cause drying of the eye at night and increase the risk that the open eye rubs on the pillow.
Meibomian gland dysfunction (MGD). MGD becomes more common with age, but can be present at any age. It is seen in chronic cases of blepharoconjunctivitis and is more common in patients that have had styes.
SEE RELATED: Eyelash lice: How do you get them and what are the treatments?
Signs and symptoms of blepharoconjunctivitis
Some of the most common symptoms of blepharoconjunctivitis include:
- Redness in or around the eyes
- Excess tearing
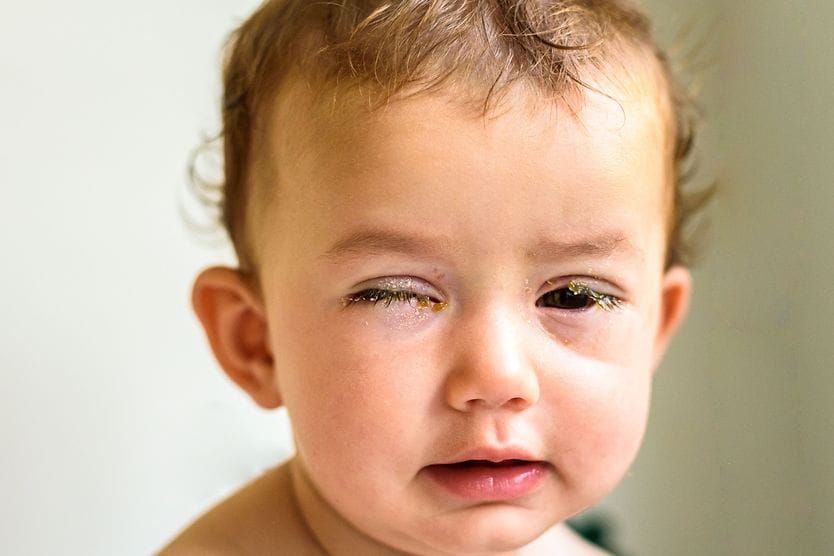
- Dry, scaly or crusty skin around the eye and eyelid
- Debris and deposits stuck to the eyelashes
- Feeling as though something is stuck in your eye (this is called a foreign body sensation)
- Eyelids sticking together
- Itching
- Burning
- Irritation
- Eyelash loss
- Greasy lids
- Red bumps including papules or pustules
- Eyelid inflammation
Symptoms often occur in both eyes and may feel better or worse at different times. Many find that symptoms are particularly unpleasant in the morning, just after waking up.
SEE RELATED: Eyelid dermatitis: Causes, symptoms and treatment
Types of blepharoconjunctivitis
Blepharoconjunctivitis can occur in one or both eyes, but it usually occurs in both. There are many types of blepharoconjunctivitis. Some are more severe than others.
The different types of blepharoconjunctivitis can be categorized based on the part of the eyelid that is affected or what is thought to be the cause:
Location
- Anterior disease – Affecting the area of the eyelid at the base of the eyelashes
- Posterior disease – Associated with meibomian gland disease and affects the edge of the eyelid that touches the eyeball
- Angular blepharoconjunctivitis – A rarer type of blepharoconjunctivitis caused by Moraxella or Staph bacteria
Cause
- Seborrheic blepharoconjunctivitis – There are often signs of seborrheic dermatitis elsewhere on the face and dandruff of the scalp and eyebrows. The edge of the eyelid has greasy yellow to gray scales.
- Atopic blepharoconjunctivitis – This condition is brought on by chronic allergies. It can involve the cornea in addition to the conjunctiva and eyelids. The eyelids will have dry scales that are not limited to the edge and may look like eczema.
- Molluscum contagiosum and monkeypox virus – Small round skin lesions are present elsewhere on the body, and at least one lesion is close enough to the eye to shed viral particles onto the conjunctiva.
- Phthiriasis palpebrarum – This is a sexually transmitted infection (STI) that causes small gray deposits – the eggs of the lice – at the base of the lashes. They cause redness and extreme itchiness.
- Herpes simplex virus-1 – May appear as a simple rash or look more like fluid-filled blisters that break open and then form a crust.
- Bacterial blepharoconjunctivitis – Can affect different parts of the eyelids. The conjunctivitis component is more likely to cause a thicker discharge.
- Ocular rosacea – Associated with rosacea of the face, this is a condition caused by Demodex mites. The edge of the eyelids have round scurf at the base of the eyelashes (called collarettes). And there are small blood vessels that appear at the surface of the skin (called telangiectasia).
A type of cancer called sebaceous cell carcinoma can look similar to blepharoconjunctivitis. Redness in both the conjunctiva and eyelids may appear, even without a cancerous mass. Lash loss can also occur. Patients that had a stye removed that grew back are more likely to have this condition. These symptoms should be examined to detect whether cancer may be present.
SEE RELATED: Eyelid cancer: Types, symptoms and treatments
Blepharoconjunctivitis treatment
The standard treatment method for blepharoconjunctivitis is hygiene-focused. Some recommended ways to achieve this include:
- Washing the eyelashes with a specially formulated shampoo to remove dandruff and cleanse the area. Some of these shampoos contain antimicrobial agents, such as hypochlorous acid or tea tree oil. For optimal results, these antimicrobial shampoos generally should be allowed to soak into the skin.
- Placing a warm compress over the eyes to soften the oil in the meibomian glands. Doing this for five to 10 minutes is often recommended, followed by gently massaging the eyelids to help release oil from the clogged glands.
Artificial tears may also be recommended — both for rinsing the eyes and relieving dryness.
If blepharoconjunctivitis is associated with an underlying condition, that condition is treated first. The methods listed above should generally be used with other prescribed treatments when needed.
It’s important to monitor healing, and seek help if your condition gets worse or does not respond to treatment. You may be given a topical antibiotic or steroid for one to two weeks if maintaining good hygiene isn’t enough. In some cases, antibiotic pills such as doxycycline and azithromycin are prescribed for longer periods of time.
Chronic blepharoconjunctivitis may lead to other eye conditions, such as:
- Severe dry eye
- Loss of the meibomian glands
- Styes
- Eyelid infection (called preseptal cellulitis)
- Misdirected eyelashes
- Growth of new eyelashes that rub on the cornea
- Formation of calcifications inside the eyelids (concretions)
When to see a doctor
If you find yourself asking, “Why won’t my eye infection go away?” additional treatment may be required. Contact your eye doctor if your condition worsens, persists or returns after initial treatment.
Be sure to discuss with your doctor any medications, eye cosmetics or skin products you use.
Additionally, be sure to stay up to date on annual comprehensive eye exams. Even if you haven’t noticed any changes in your visual clarity, it’s important to check for separate eye problems that need to be addressed.