What is corneal ectasia?
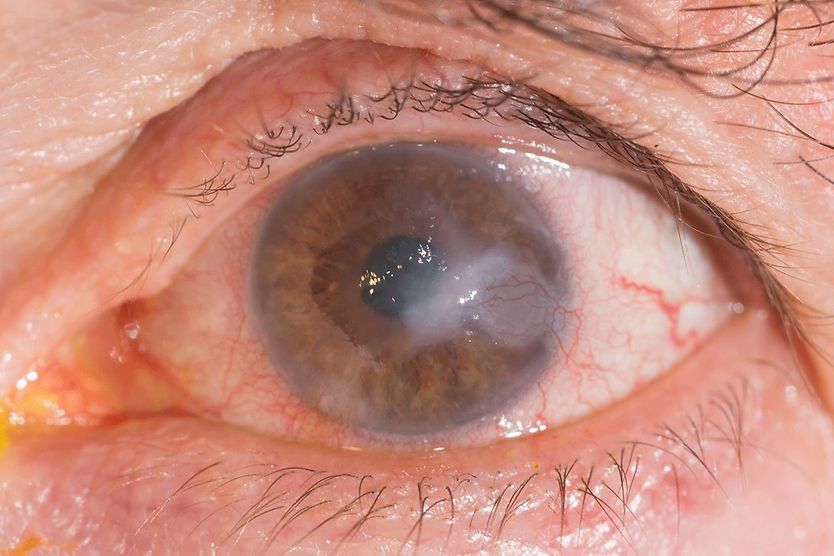
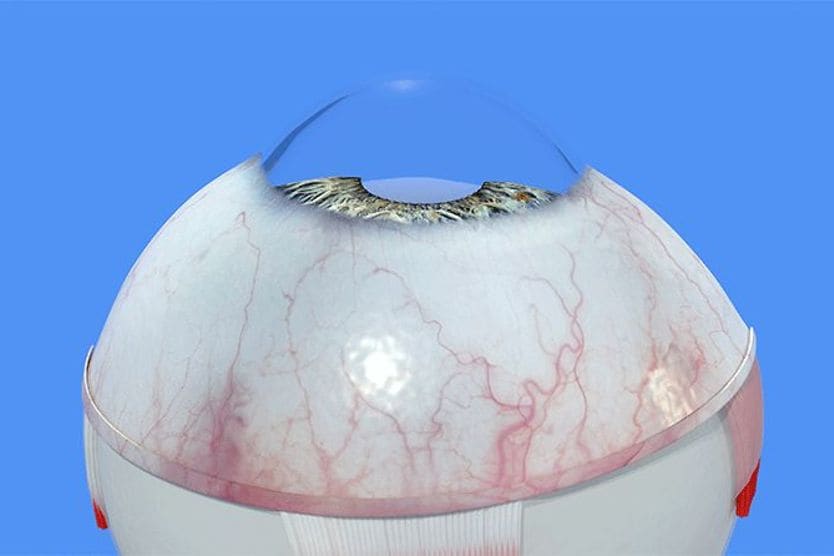
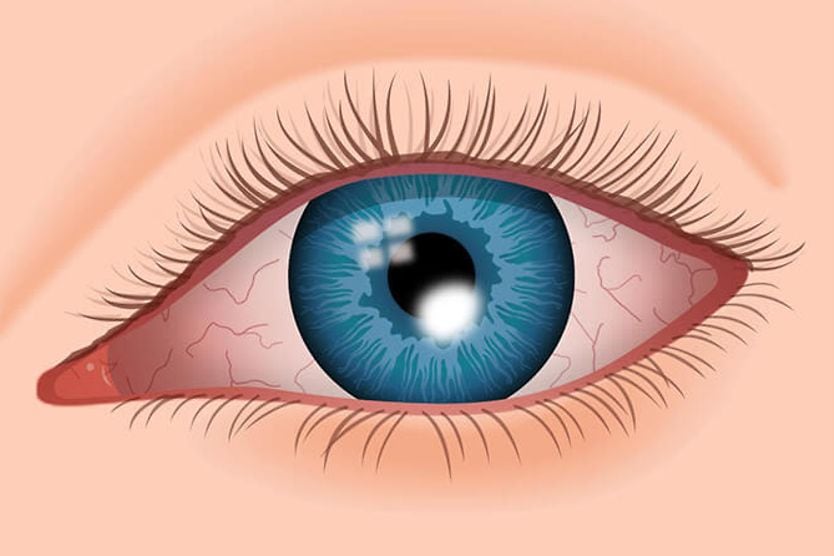
Corneal ectasia is when the cornea, the clear, dome-shaped outermost layer in the front of the eye, develops a bulge. This thinning can result from a condition called keratoconus, refractive surgery, or a corneal infection or injury.
Signs and symptoms of corneal ectasia
Ectasia can cause:
- The blurring of vision that cannot be corrected with glasses or soft contact lenses
- Halos around lights
- Double vision (diplopia) in one eye at a time
- Ghost images, when one eye sees a sharp image with a faded image right next to it
- High myopia (severe nearsightedness)
- High astigmatism
- A large difference between the prescription of each eye (anisometropia)
- Rapid and frequent changes in glasses prescriptions
- Squinting
- Headaches after using the eyes for reading or driving
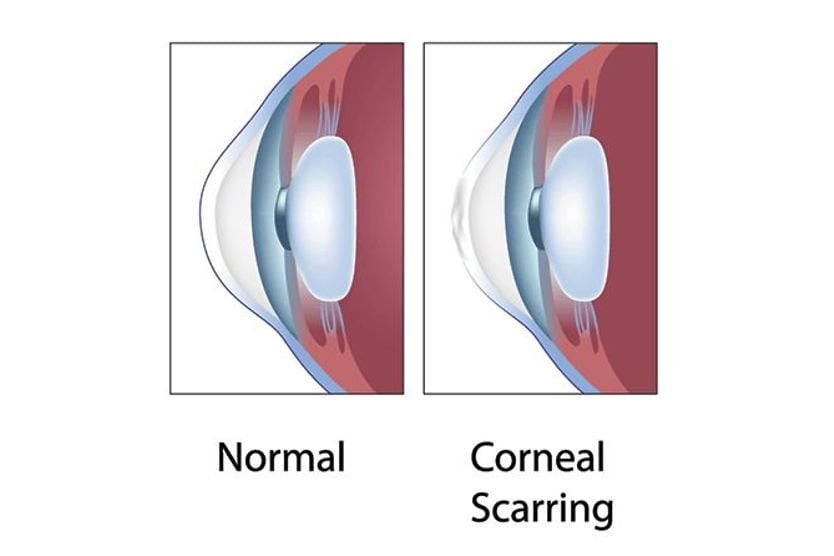
- Scarring of the cornea
What causes corneal ectasia?
The ciliary body pumps a constant flow of fluid, creating pressure on the inside structures of the eye. When one of these structures — such as the cornea — develops a thin spot, eye pressure will cause it to flex outwards. This is similar to a thin spot causing a bulge in a car tire.
The cornea is the strongest focusing lens of the eye, and a distortion will cause blurred vision, halos and glare.
There are multiple types and causes of corneal ectasia, including:
Keratoconus
Keratoconus is a type of corneal ectasia that affects about one in every 2,000 people in the United States. In some parts of the world, such as the Middle East, rates can be as high as one in 20 people. While the exact cause is unknown, a person’s family history, habits, contact lens usage and other health conditions can increase their risk of developing keratoconus.
For about one in 10 people with keratoconus, there is a clear genetic connection to the disorder, with someone else in their immediate family (a parent, sibling, child, aunt or uncle) also affected.
About half of the people with keratoconus have a habit of rubbing their eyes vigorously, and half also have eye allergies, asthma or eczema.
Keratoconus usually develops in both eyes — often more in one than the other. It begins during the teenage years and steadily becomes worse until it generally stops changing by age 40. Besides warping of the cornea and the development of irregular astigmatism, scars can develop on top of the bulging area of the cornea (the cone), leading to more severe vision loss.
In some cases, a breaking of the inside of the cornea — the endothelium — causes it to suddenly fill up with fluid, causing rapid vision loss. This complication, called corneal hydrops, occurs in about one in every 100 people with keratoconus.
The largest study ever done on keratoconus — the Collaborative Longitudinal Evaluation of Keratoconus (CLEK) observational study — showed that about two-thirds of patients with keratoconus wear some type of rigid contact lens.
This study and others also showed that between 15% and 20% of everyone with keratoconus eventually needs some type of corneal transplant surgery.
Other types of corneal ectasia that are similar to keratoconus in some ways include:
- Pellucid marginal degeneration – The ectasia is closer to the inferior (lower) edge of the cornea.
- Keratoglobus – The thinning of the cornea is all the way around and right at the edge.
- Posterior keratoconus – The thinning and ectasia are limited to the inside layer of the cornea (the endothelium) and do not affect the surface as much.
- Terrien’s marginal degeneration – This type affects the superior (upper) edge of the cornea.
Refractive surgery
Refractive surgery has been reported to cause ectasia in two to six out of every 1,000 surgeries. While this is a small number, it is still important to discuss ways to avoid this complication with your surgeon if you are thinking of having refractive surgery.
The cornea is normally around 540 to 550 microns thick, and refractive surgery involves changing the curvature of the cornea without making it too thin. Refractive surgeons agree that a minimum of 250 to 300 microns of the deeper corneal layers, called the “corneal bed,” need to remain untouched to avoid ectasia.
Refractive surgeries that are more likely to cause ectasia include:
Radial keratotomy
This refractive surgery was popular from the 1970s into the 1990s. Several deep incisions are made in the cornea with the goal of flattening the center of the cornea. These incisions weaken the cornea, causing ectasia just outside the center of the pupil.
In addition to ectasia, this surgery often led to complications such as daily changes in the focusing of the eye and gradual changes of the spectacle prescription over time. This has resulted in most surgeons abandoning radial keratotomy in favor of newer and better procedures.
LASIK (laser-assisted in situ keratomileusis)
With the LASIK procedure, an incision is made into the cornea, and the middle layer of the cornea (the stroma) is treated with a laser.
To ensure enough of the corneal bed can be left intact, LASIK surgeons will scan the contour and distribution of the cornea’s thickness. This test, called corneal topography, is designed to detect early signs of keratoconus. Other risk factors for post-surgical ectasia are high nearsightedness (over 8 diopters) and younger age.
If it’s determined that a patient is not a good candidate for traditional LASIK (e.g., the corneal bed is calculated to be too thin), possible safer options for refractive surgery include:
PRK (photorefractive keratectomy)
Since only the surface of the cornea is treated during PRK, less of the cornea’s deeper layer is removed with the laser.
Epi-LASIK
The “epi” in epi-LASIK stands for epithelial. This treatment uses a special knife blade to cut the surface layer (epithelium) only. There is more discomfort after this procedure, and the healing process is slightly different compared to LASIK, but it is safer.
LASEK (laser-assisted subepithelial keratectomy)
This treatment is similar to epi-LASIK, except the epithelium layer is loosened with alcohol. Since alcohol is toxic to the cornea, LASEK can cause a more vigorous healing process.
SMILE (small incision lenticule extraction)
In the SMILE procedure, a laser creates a “lenticule” of tissue that is then removed from underneath the epithelium through a tiny incision in the cornea. Because it does not require a larger incision to create a “flap” (like LASIK) and does not affect the epithelium (like PRK and epi-LASIK), SMILE has many advantages.
Refractive lens exchange
Also called clear lens extraction or lens replacement surgery, this procedure is similar to cataract surgery. It involves the removal of the crystalline lens and the placement of an intraocular lens (IOL) implant in the eye. Because this procedure is done inside the eye, it has a (very small) risk of infection, inflammation and retinal detachment.
For younger patients (under 40 years old), a focusing or presbyopia IOL is recommended. This is because regular IOLs allow you to focus either in the distance or up close, but not both.
Phakic IOL
This surgery involves inserting an implantable lens in front of the eye’s natural crystalline lens. This can be a good option for people with high nearsightedness. The advantages of phakic IOLs are that there’s no loss of up-close vision and no increase in the risk of retinal detachment. This procedure is also available for people who have developed ectasia due to keratoconus and other reasons.
Since refractive lens exchange and phakic IOL implantation do not alter the cornea, there is a near-zero risk for ectasia. In one study, per 100,000 surgeries, LASIK had the highest risk of ectasia (90), while both PRK (20) and SMILE (11) had much lower rates.
Infection and inflammation
Certain infections and inflammations can cause thinning of the corneal tissues, which can then cause ectasia. Some of these causes include:
- Microbial keratitis (MK) – Bacteria or other microbes — such as fungi and amoeba — can infect the cornea and cause thinning and even perforation. Sleeping while wearing contact lenses is a risk for this.
- Neurotrophic keratitis ( NK) – This type of thinning is caused by a lack of nerve signal (innervation) to the cornea. This occurs when the nerve that connects to the cornea and sends pain signals back to the brain — the trigeminal nerve — becomes damaged.
- Atopic keratoconjunctivitis (AKC) – Severe allergies can cause a shield ulcer. This is a type of thinning that is situated on the part of the cornea that is normally covered by the upper eyelid. People at risk for this type of thinning have small bumps on the inside of their eyelids called giant papillae.
- Mooren’s ulcer – A painful area of thinning in the mid-periphery of the cornea.
- Peripheral ulcerative keratitis (PUK) – A condition that can cause severe thinning at the edge of the cornea. It is more common in people with rheumatoid arthritis.
Other infections and inflammations that are less common may result from collagen vascular diseases such as lupus erythematosus.
They may also be caused by microorganisms that infect the cornea and cause inflammation and damage. These can include:
- Herpes simplex virus (HSV)
- Acanthamoeba (a microscopic amoeba)
- Staphylococcus bacteria
Non-refractive eye surgery
When eye surgery results in the removal of corneal tissue, especially in the middle of the cornea, it can result in ectasia.
One type of surgery that can cause ectasia is pterygium surgery. A pterygium is a white growth that starts at the edge of the cornea and slowly grows into the center. A pterygium is only removed when it gets too large and starts to affect a person’s vision.
Surgeons may add a special chemical (mitomycin-C) as part of the surgery to reduce the risk of the pterygium growing back again. Unfortunately, this chemical can cause thinning of the sclera and cornea and result in ectasia.
Eye injury
Blunt trauma and injury with sharp objects can damage the cornea and ultimately lead to ectasia.
This type of trauma can result from:
- Motor vehicle accidents (including airbag deployment)
- Physical altercations
- Workplace injuries and other incidents
It’s important to treat any eye injury as a potential emergency. Contact your eye doctor immediately if you ever injure one of your eyes. It could save your sight!
Testing for ectasia
There are several ways that thinning and warpage of the cornea can be detected:
Slit lamp exam
Using a magnifier called a slit lamp or biomicroscope, an eye doctor is able to detect subtle signs of ectasia on the cornea. These signs may include:
- Fleischer ring – A ring of iron deposits at the base of the bulge in the cornea.
- Munson sign – When the patient looks down, the cone-shaped cornea causes a triangular (or V-shaped) distortion of the lower eyelid.
- Vogt striae – Small vertical lines (folds) on the inside of the cornea.
- Apical scarring – Scars at the apex (top) of the cone (the bulging area of the cornea).
- Corneal thinning – An average human cornea should be around 540 to 550 microns thick at its center. If the central thickness is less than 500 microns, it’s considered a thin cornea. A special light beam can trace the thickness of the central cornea in different places and detect thinning.
Keratometry
A keratometer is a machine that eye doctors use to measure the curvature of the cornea. This measurement is called keratometry. Also called an ophthalmometer, this machine records the abnormal reflection from the ectatic cornea.
Corneal topography and pachymetry
These tests are the gold standard for detecting ectasia. Corneal topography maps the cornea’s surface contour while pachymetry measures the cornea’s thickness. Some machines allow for early detection of ectasia by combining these features to create a map of the cornea’s surface, thickness and inside contour.
Rigid lens over-refraction
There may be times when all the above tests are inconclusive, but the eye doctor still has a suspicion that the warping of the cornea is the cause of their patient’s vision loss. In these cases, they may create a new focusing surface on top of the front of the eye by placing a rigid lens on the eye and measuring vision. This can be the key to figuring out what is going on.
Nonsurgical treatments for ectasia
Glasses
Many cases of corneal ectasia are correctable with glasses, allowing people to see 20/20 in at least one eye (chiefly in the earlier stages of the disease). But correction to 20/20 vision does not always mean that a person’s vision is completely normal. Glare and ghosting may be present, especially at night.
Since corneal ectasia is often worse in one eye, a person’s glasses prescription can be very different between the two eyes. Called anisometropia, this difference in prescriptions can sometimes cause an intolerance to glasses.
Contact lenses
Similarly to glasses, regular soft contact lenses can often be used in the early stages of corneal ectasia. In these cases, when anisometropia precludes wearing glasses, these types of contact lenses can often still be used.
Corneal ectasia causes astigmatism, higher amounts of nearsightedness and an irregular corneal shape. This can mean the doctor may have a tough time finding a lens that is completely satisfactory.
There are two special soft contact lens options that may work for someone with ectasia. Both are stiff enough to create a less irregular surface and allow for better focusing of light into the eye.
These lenses can be modified in different ways to provide a custom-made fit of the ectatic cornea.
Rigid gas permeable (RGP) contact lenses are used for the majority of people with ectasia. Unlike soft contact lenses, rigid lenses will retain their round shape and create a sharp focusing image on the retina.
There are several categories of RGPs:
- Corneal RGPs – These lenses have a significantly smaller diameter than the cornea (12 mm), are easy to put in and take out of the eye, and allow enough oxygen to reach the cornea.
- Intralimbal RGPs – When a patient requires a lens that is more stable and less likely to jump out of their eye, or when the irregular area is at the edge of the cornea, intralimbal lenses are a good option. These lenses are slightly smaller than the diameter of the cornea.
- Scleral lenses – These come in two sizes: “mini-scleral” (13 to 16 mm) and “scleral” (over 16 mm). These lenses are extremely stable and will not rub on the corneal cone area, reducing the risk of scarring. However, they are hard to insert and remove from the eye, and they require a lot of care.
- Hybrid lenses – This type of lens combines a rigid center with a soft edge (called the “skirt”). The advantages are that these lenses are stable and provide the visual clarity of RGPs with the comfort of a soft contact lens. Disadvantages are that they require a lot of care, are harder to insert and remove, and can sometimes lead to inflammation if they fit too tight (tight lens syndrome).
- Piggyback contact lenses – Placing an RGP on top of a soft contact lens is called a “piggyback” combination. Using both lenses at the same time can improve a patient’s comfort when using an RGP by itself causes discomfort or damage to the cornea. In these cases, the soft lens is also called a bandage lens.
Surgical treatments for ectasia
Corneal cross-linking (CXL)
The cornea is made up of collagen fibers (called fibrils) that are arranged in special patterns that allow it to transmit light. These fibrils contain proteoglycan molecules that keep the cornea strong.
Researchers discovered that as people age, and when they develop diabetes, the cornea becomes even stronger because more bonds are made between and inside the fibrils. Corneal ectasia, on the other hand, weakens these bonds and the cornea’s ability to accurately focus light.
Corneal collagen cross-linking (CXL) is a process that was developed in the late 1990s and approved in 2016 by the Food and Drug Administration (FDA) to treat corneal ectasia. During this treatment, riboflavin (vitamin B2) is allowed to soak into the cornea before the eye is given limited exposure to ultraviolet light. This activates the formation of new bonds between and inside the fibrils to strengthen the cornea.
This treatment can only be done if the cornea is more than 400 microns thick and has no scarring. Therefore, it’s essential to get a timely diagnosis by an eye doctor and an early referral for the procedure.
The number of corneal transplants to treat ectasia went down by 25% in the three years following the FDA’s approval of corneal cross-linking. This indicates a major benefit of CXL in that it lowers the risk of needing a corneal transplant.
Corneal transplantation
About 15% to 20% of people with corneal ectasia will eventually require a cornea transplant.
Types of corneal transplant surgery include:
- Full-thickness corneal transplant, also called penetrating keratoplasty (PKP)
- Deep anterior lamellar keratoplasty (DALK)
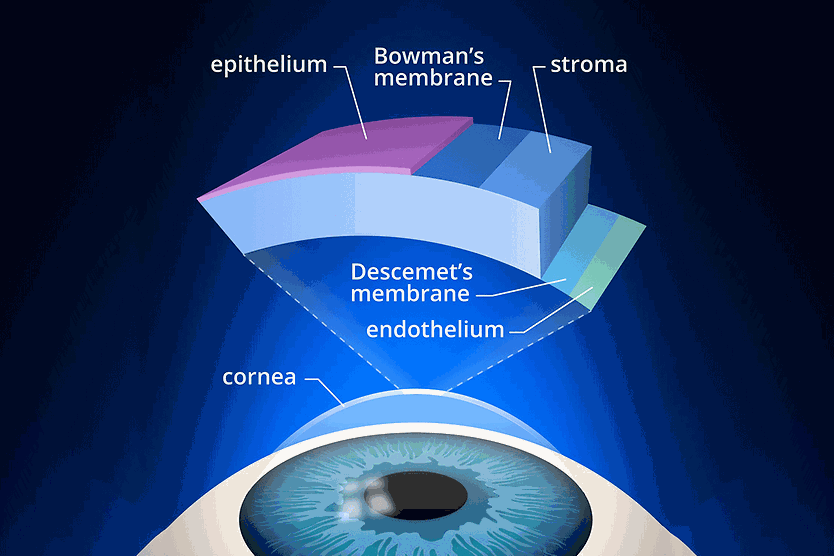
With PKP, the eye surgeon removes all the layers of the cornea (the epithelium, stroma and endothelium) and replaces them with a donated non-diseased cornea. In DALK, only the epithelium and stroma layers are removed.
Both PKP and DALK have very good results, along with their own set of advantages and disadvantages.
While PKP generally results in better visual acuity, it also comes with a higher risk of:
- Infection
- Inflammation
- Formation of cataracts
- Graft rejection (where the body rejects the transplanted cornea)
- Failure of the graft (where the graft fills up with fluid)
- Other complications
In some cases, corneal transplantation results in vision that can be corrected with glasses, but in the majority of cases, RGPs are required for optimal vision.
Intracorneal ring segments (ICRSs)
ICRSs are, in essence, expander rings inserted into the middle of the cornea to help flatten and smooth it out. This creates a more regular corneal surface that focuses light better and reduces the amount of nearsightedness and astigmatism.
The expander rings form a circle around the pupil. Two main types are available: One type leaves an open space of 7 mm, and the other leaves 5 mm open.
Advantages of ICRSs include:
- Insertion of the rings is not as large a surgery as a corneal transplant.
- The procedure is reversible, meaning the rings can be removed.
- It can be combined with corneal cross-linking and phakic IOLs.
- Vision improves significantly for many recipients of ICRSs.
- Having an ICRS can make it easier to fit both soft contact lenses and RGPs (for piggyback contacts).
ICRS disadvantages include:
- The results can be variable.
- This treatment is still a surgical procedure with potential risks.
- It is not an ideal treatment for advanced ectasia, and it cannot treat scarring caused by ectasia.
When to see an eye doctor
If you’ve had refractive surgery and are experiencing blurry vision — especially if your vision is more blurry in the distance than up close — it’s important to see your eye surgeon or eye doctor to rule out ectasia.
If you rapidly develop nearsightedness and/or astigmatism in your teenage years or your 20s — particularly if it’s more in one eye than the other — it is recommended to see an eye doctor and ask to be checked for corneal ectasia.
It’s also important to have regular comprehensive eye exams. This is especially true if you have a family history of keratoconus, which puts you at increased risk of developing corneal ectasia. If you haven’t had your eyes examined recently, schedule an appointment with your eye doctor today.