What is a corneal descemetocele?
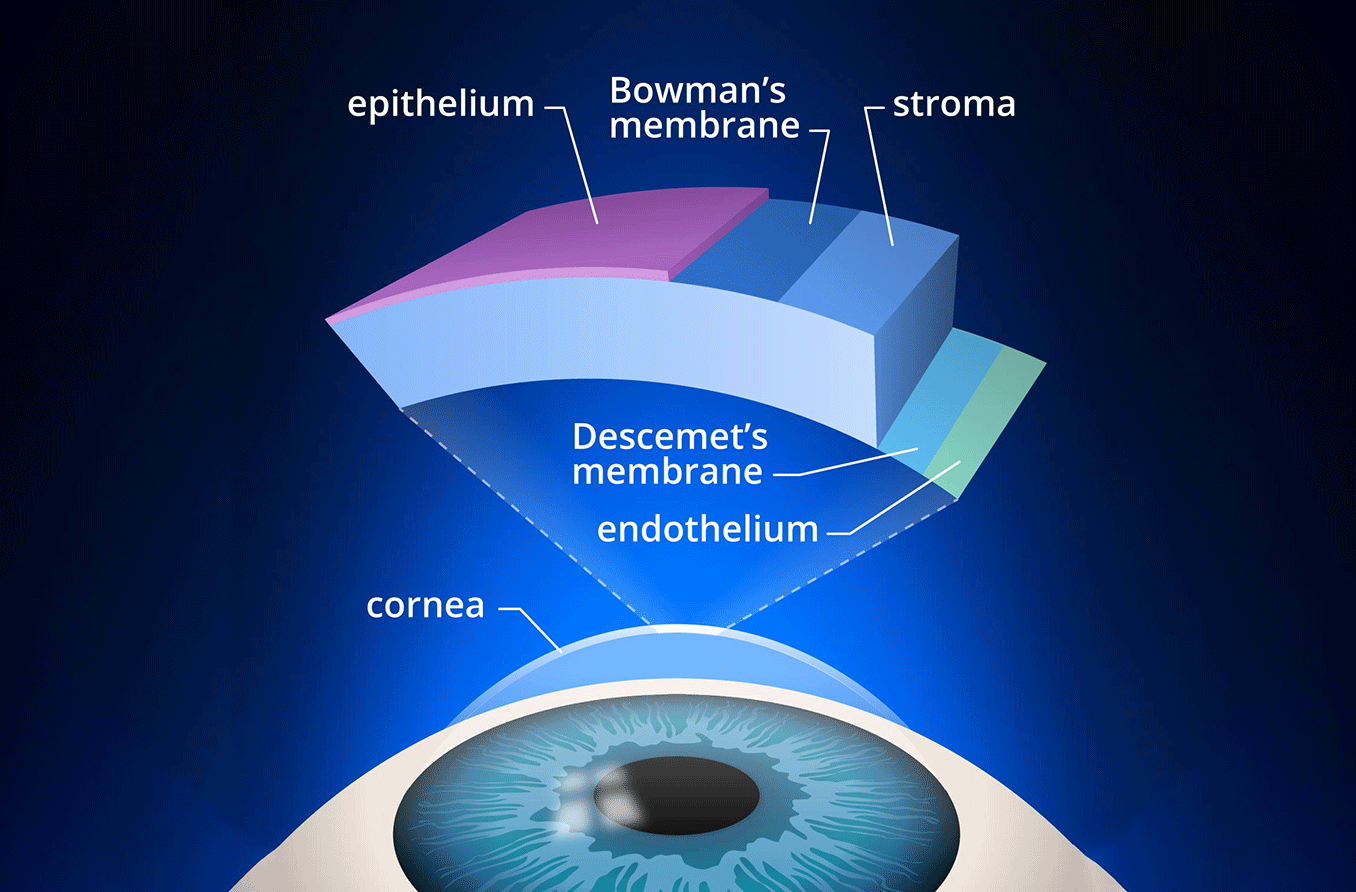
A corneal descemetocele is a condition in which the Descemet membrane, a layer of the cornea, protrudes through a thin area in the corneal layers above it. The cornea is made up of three main layers:
- The epithelium on the surface of the eye
- The stroma in the middle
- The endothelium on the inside
The Descemet membrane anchors the endothelium to the stroma. The endothelium is also adjacent to the fluid that circulates inside the eye (the aqueous humor). Since this fluid is under pressure, it can press the endothelium and the Descemet membrane forward through a damaged cornea, just like an inner tube can bulge through a thin spot in a tire.
Corneal descemetoceles are rare but may be dangerous. They are often caused by a corneal ulcer. If left untreated, they can cause the cornea to leak and the eye to lose pressure.
Corneal ulcers are considered a medical emergency. It is important to seek immediate emergency eye care with your eye doctor if you have any of the associated symptoms.
What causes a corneal descemetocele?
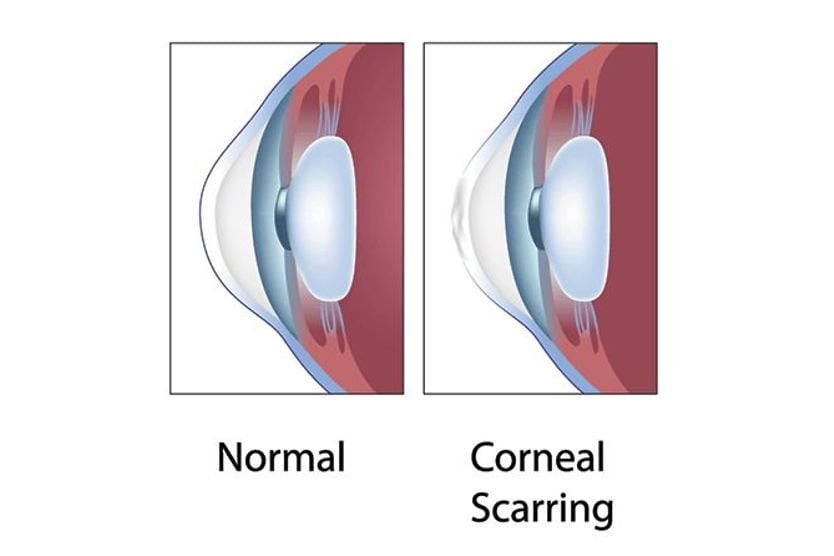
A descemetocele can develop from corneal ulcers that have been left untreated. Corneal ulcers are open sores that form on the cornea — the clear layer of tissue on the outside of the eye. These sores can cause the structure of the cornea to weaken.
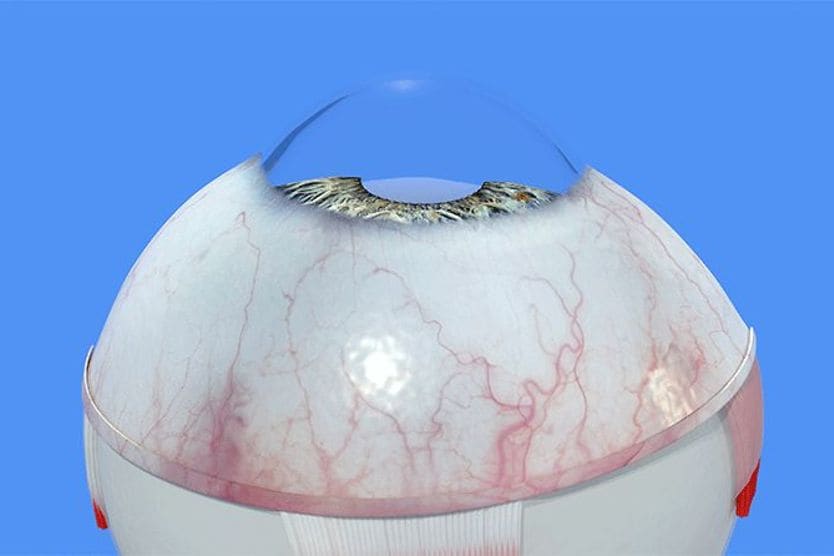
When the Descemet membrane is the only layer of the cornea to remain intact, pressure from inside the eye may cause it to bulge out. This results in a corneal descemetocele.
Corneal ulcers can be caused by:
- Infections of bacteria, viruses, fungi or parasites
- Autoimmune diseases
- Severe dry eye
- Severe eye allergies
- Exposure of the eye
- Inflammation
- Trauma to the cornea, such as a corneal abrasion
People at risk for corneal ulcers may include those who:
- Sleep in their contact lenses
- Have had cold sores, shingles or chickenpox
- Have eyelids that do not close completely or are damaged
- Have severe rheumatoid arthritis (RA) or systemic lupus erythematosus (SLE)
- Use steroid eye drops
- Have had an injury or chemical burn to their cornea
- Have a type of allergy called atopic disease
What are the symptoms of a corneal descemetocele?
Corneal descemetocele can lead to a sudden loss of visual clarity, depending on where the protrusion is located. It also may cause eye pain and watering. These may develop after symptoms associated with corneal ulcers.
Symptoms of a corneal descemetocele may include:
- Blurred vision
- Red or bloodshot eyes
- Itchy eyes
- Eye discharge
- Photophobia (light sensitivity)
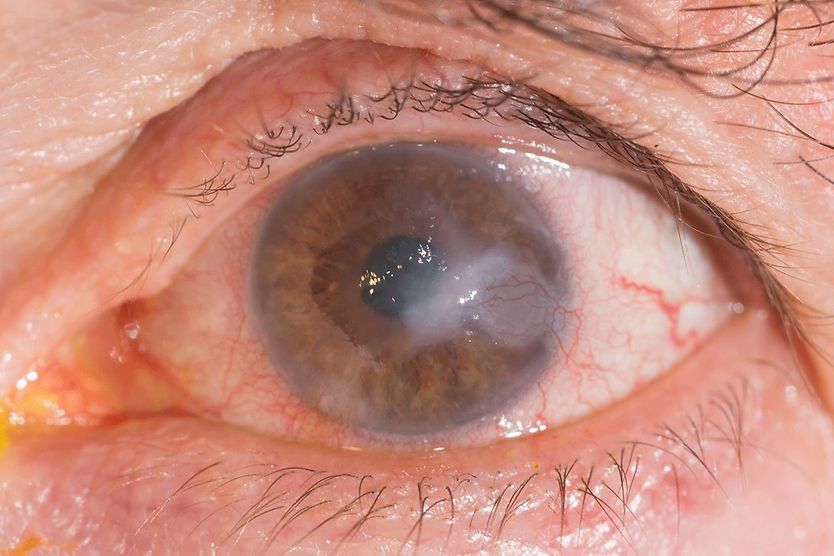
- A white patch on the cornea
One common sign of a descemetocele is a white, cloudy ring circling the protrusion.
Because of the similarities in their appearance, corneal ulcers may be mistaken for conjunctivitis (pink eye).
How is a corneal descemetocele diagnosed?
To help diagnose a corneal ulcer and potential descemetocele, your eye doctor may perform a slit lamp examination. This exam involves the use of a microscope with a bright light, called a slit lamp. The microscope allows the doctor to examine the structure of the eye.
Your doctor may take a sample of the infected tissue for further examination. This may help them to determine what kind of infection is present.
They may also perform a Seidel test, which may help them determine whether the cornea is perforated and actively leaking fluid. The Seidel test uses a dye called fluorescein, which highlights any fluid leaking out of the cornea.
How is a corneal descemetocele treated?
Your eye doctor may focus on two main things when treating descemetoceles: ocular integrity and the root cause of the corneal ulcer. Reinforcing the corneal structure may help prevent new holes (corneal perforations)from forming in the cornea.
Depending on the size of the descemetocele and the eye doctor’s recommendation, any of the following treatment options may be used:
- Tissue adhesive – This glue-like substance helps hold tissue together as an alternative to stitches.
- Amniotic membrane transplantation – The inner layer of placenta can be used as a graft to help heal the surface of the eye.
- Conjunctival flaps – This is a procedure in which a thin flap of conjunctiva is pulled over the area of the cornea that’s been impacted. The flap is then secured with sutures. The conjunctiva is a thin membrane that covers the white of the eye (the sclera).
- Corneal transplantation – Also called keratoplasty, this is the use of a donor’s cornea to replace the patient’s affected cornea.
- Conjunctival resectioning – This is the surgical removal of about 3 millimeters of conjunctiva near the ulcer.
The variety of conditions that lead to descemetoceles means that there are multiple treatment options, some of which may address underlying causes. Other treatment options can include:
- Antibiotics to treat infection
- Lubricating eye drops to treat dry eye
- Drops to reduce eye pressure
- Bandage contact lens, a special type of contact used to help heal the cornea rather than improve visual acuity
- Anti-collagenase medications and/or vitamin C to help treat corneal ulcers
- Anti-inflammatory medications and/or immunosuppressants to help reduce inflammation
What risks are associated with a corneal descemetocele?
If a corneal descemetocele goes untreated, the protrusion (or hernia)may rupture or burst, leading to a corneal perforation. This means that a hole has formed through all layers of the cornea.
Other possible complications of a corneal descemetocele may include:
- A weakened anterior chamber – When the space containing clear fluid between the cornea and the iris is weakened
- Endophthalmitis – An infection in the tissue or fluid of the eye
- Glaucoma – An eye disease that causes damage to the optic nerve
- Cataracts – Cloudiness of the eye’s natural lens
- Significant loss of vision
- Loss of the affected eye
When to see an eye doctor
Remember: Corneal ulcers are considered a medical emergency. If you notice any of the signs or symptoms of a corneal ulcer or descemetocele, you should seek immediate medical attention with your eye doctor.