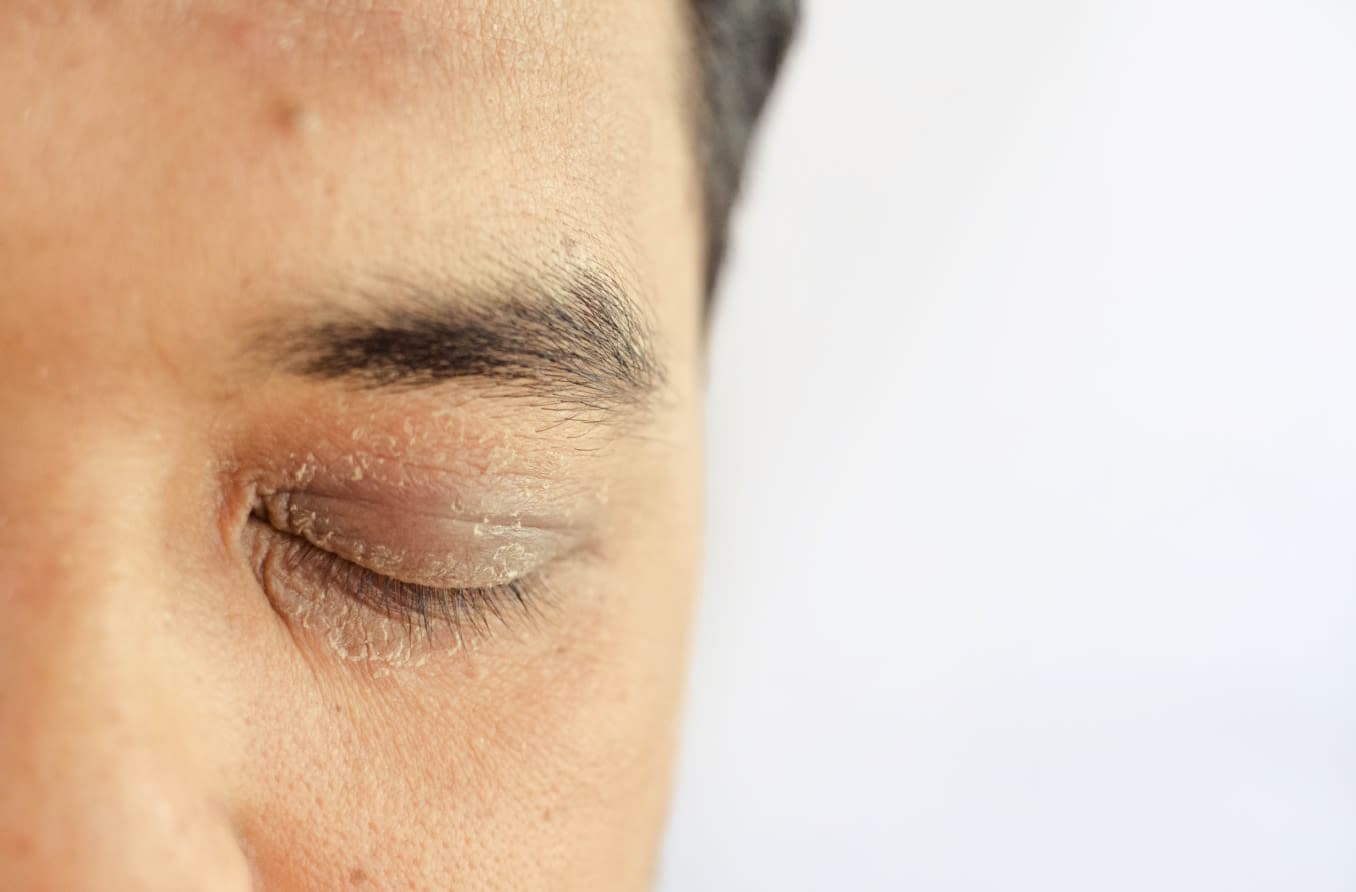
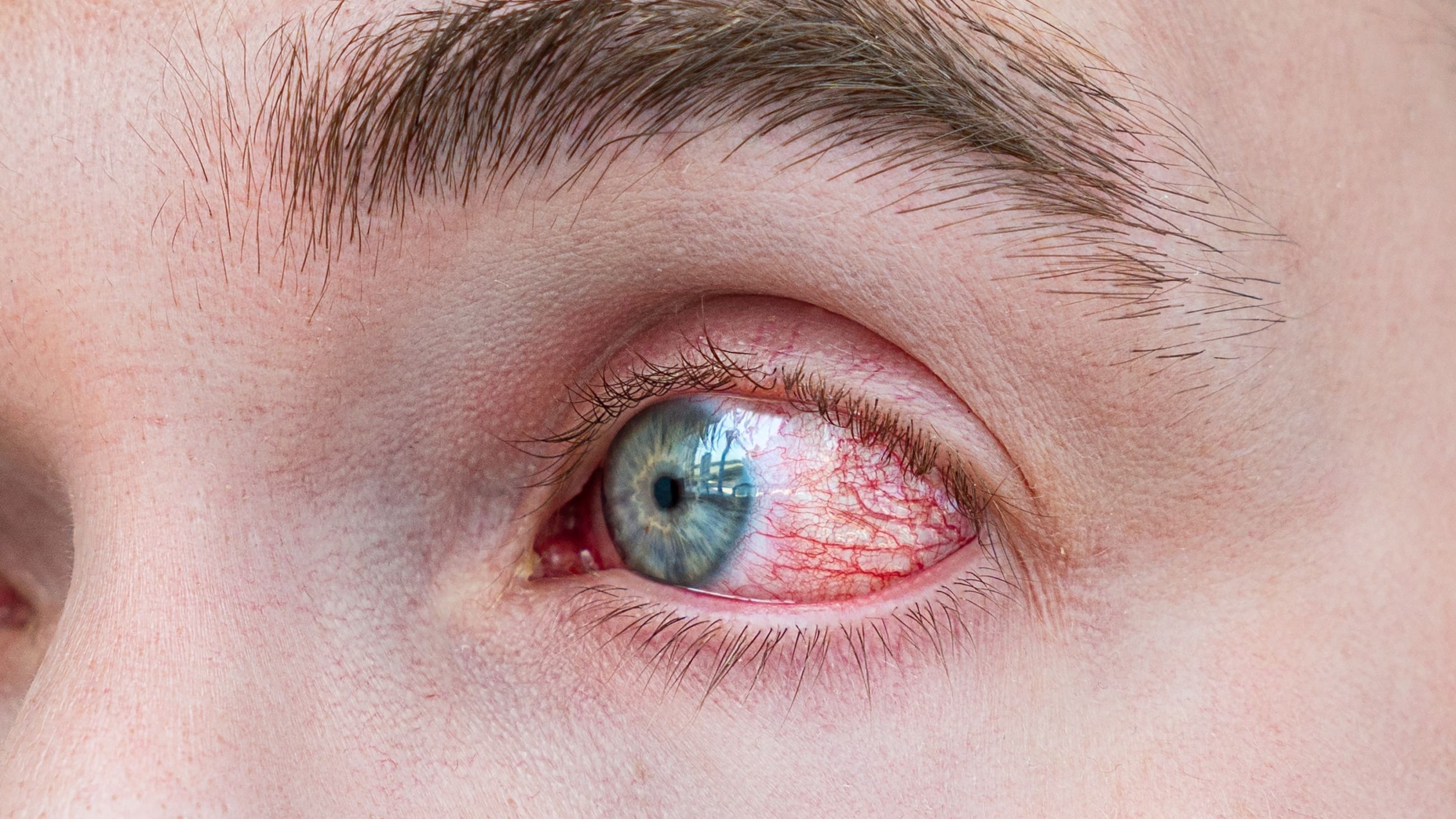
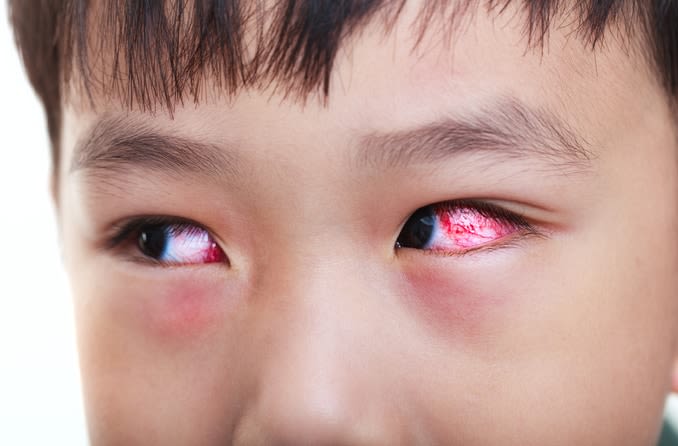
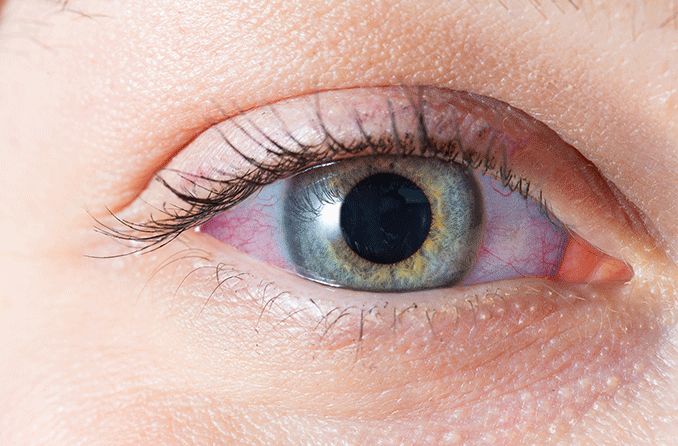
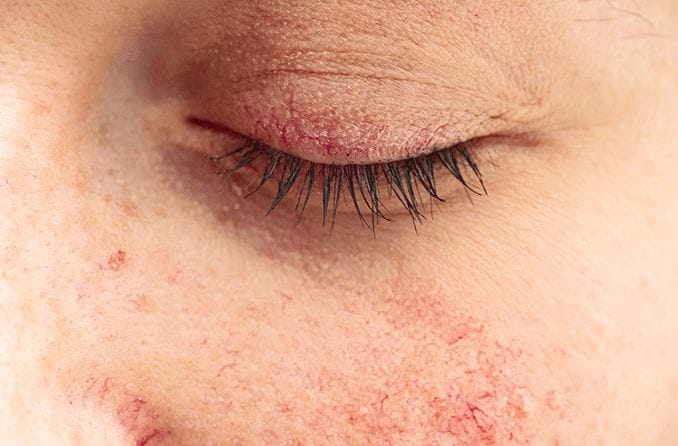
Why are my eyelids so dry?
The eyelids naturally stay hydrated thanks to a significant amount of blood flow, as well as to oils that provide a moisture barrier. But because eyelid skin is so thin, it can easily become dry. Factors like a decrease in natural oil production, irritant exposure and underlying conditions can cause dry eyelids.
Affected areas may also be red, itchy, flaky and, in some cases, painful. Fortunately, there are many ways to treat and prevent dry skin around the eyes.
Causes of dry eyelids
Dry eyelids can happen to anyone at any time during their life. However, aging is a heavy contributor to dry skin, including around the eyes. By age 40 and after, the level of natural oils produced by your skin significantly decreases. These oils help keep moisture in, so a decline in oil production can result in eyelid dryness.
Scaly eyelids can also be caused by an underlying condition, irritant exposure or certain lifestyle choices.
Underlying conditions
Underlying problems can show themselves through skin irritation and flakiness. Dermatological conditions are usually the first thing eye doctors and dermatologists check for.
Atopic dermatitis, also known as eczema, is a lifelong disease that causes dry, irritated, inflamed skin. It often begins in childhood and may or may not improve as the child gets older.
The red, scaly rash associated with atopic dermatitis is usually seen on the neck and face, around the eyes, on the eyelids and in areas where joints bend, like the knees and elbows. An exact cause of the disease is unknown, but experts believe genetics, immune system health and environmental factors play a role.
LEARN MORE: Eyelid eczema: Causes, symptoms and treatment
Seborrheic dermatitis is another form of eczema. It appears as an inflammatory response to an overgrowth of a certain type of yeast on the epidermis. In facial seborrheic dermatitis, areas of the scalp and around the eyes are affected.
Blepharitis is a common problem that is characterized by inflamed eyelids. It usually occurs in response to natural bacteria and other microbes that live on the eyelids. Blepharitis can be associated with seborrheic dermatitis, psoriasis and acne rosacea. However, it can also affect people who do not have those conditions.
Psoriasis is a chronic immune-related inflammatory disease. It causes thick, red, crusty patches called “plaques” to appear on various areas of the skin — including near the eyes.
Eyelid psoriasis can cause dry patches on eyelids and may raise a person’s risk for blepharitis. While the connection isn’t totally understood, experts believe the increased cell turnover and shedding rate can cause a blockage in the meibomian ducts along the eyelash line.
Acne rosacea is a skin condition that is thought to be caused by exposure to ultraviolet light and an overgrowth of Demodex face mites. These microbes colonize the oil glands of the face, causing a rash and red coloration of the cheeks, nose, chin, forehead and eyelids. Ocular rosacea is when the oil glands at the base of the eyelashes are primarily affected. It causes small flakes around the base of the eyelashes called collarettes.
Other underlying conditions that can cause scaly eyelids include diabetes, kidney disease, thyroid disease, vitamin deficiency, anorexia and HIV. Flaky skin can also be a result of current or past cancer treatment.
Exposure
Being exposed to certain irritants and climates can cause the skin to become dehydrated, red and scaly. This irritation is also known as contact dermatitis.
Contact dermatitis occurs when the skin becomes inflamed in response to an outside source. The cause of eyelid dermatitis may be an allergen (allergic dermatitis) or an irritant (irritant dermatitis).
Allergic dermatitis usually appears a day or two after exposure to the allergen. Allergens responsible for contact dermatitis often include poison oak or ivy, nickel and certain fragrances or preservatives. Contact lens systems may use preservatives that can cause symptoms.
Irritant contact dermatitis appears immediately after exposure. It accounts for 80% of contact dermatitis cases and happens when skin cells are damaged by an irritating substance. Common substances include certain detergents, soaps and bleach, as well as specific eye makeups or dyes (like dye used in eyelash or eyebrow tinting).
A person’s environment can also cause their eyelids to become scaly. Living in conditions of low air humidity, such as what occurs in dry climates like the desert or in cold climates when the heat is on inside the house, can leave eyelids dry.
Prolonged sun exposure and windy conditions can also cause dehydration. Wearing SPF and a pair of UV400 sunglasses when outdoors can guard your skin and eyes from harmful ultraviolet rays.
Lifestyle choices
Eyelid moisture is also affected by the choices people make. Dehydration, certain diets, and tobacco and alcohol use can all contribute to dry skin around the eyes.
Other habits that can cause dry eyelids are frequently swimming in chlorine water, taking long showers in too-hot water and using harsh soaps. These actions strip the skin of its natural oils, causing it to become dry.
A person’s age, where they choose to live and their profession can also lead to facial dryness. As mentioned, certain climates are harsher than others. Similarly, specific careers may require employees to be exposed to chemical fumes, which can irritate and dehydrate facial skin.
Certain causes of dry eyelids typically cannot be helped. Being aware of those causes and combating them with proper hydration — both outside and inside the body — can provide relief for itchy eyelids.
SEE RELATED: Can I use face oil around my eyes?
Signs and symptoms
Dry eyelids can look different from person to person. They may even appear differently each time you experience them. Dry skin under the eyes, on the eyelids or near the eyebrows may look red, rough or flaky.
Other symptoms that may also be experienced include:
- Itchiness
- Tightness in the affected area
- Fine lines that are more noticeable
- Texture that appears rough, thickened or hardened
- Cracks in the skin
- Stinging or burning
- Skin that appears looser than normal
- Peeling, crusting or flaking
- Skin that feels raw and/or irritated
These symptoms may appear and disappear quickly as a one-time occurrence. They may also flare up frequently and for longer periods of time.
Home remedies and medical treatment options
Treatment for dry eyelids depends on what’s causing the symptoms. For example, conditions like psoriasis are often treated with topical steroid creams to help with inflammation.
Other treatments that may be prescribed by your eye doctor or dermatologist include oral medication, IPL (a type of phototherapy that uses a range of wavelengths) and wet wrap therapy. Wet wrap therapy is a new method for treating severe eczema that helps increase and maintain moisture.
It is important to not get wet wrap therapy confused with hot compresses. Hot compresses can aggravate eczema and make dry eyelids worse. Wet wrap therapy involves applying body-temperature compresses to the eyes for several hours. Hot compresses are applied for five to 10 minutes and are above body temperature.
Discuss your symptoms with your primary care or eye doctor to find out what the preferred treatment method is for you.
For minor cases, there are several things you can do at home to relieve your symptoms. To reduce instances of dry skin around the eyes, it may help to:
- Use fragrance-free moisturizer often — especially after you shower or bathe. Choose a moisturizer with active ingredients like ceramides, glycerol, lactic acid and urea to help heal the skin. Be sure the moisturizer is gentle enough to use around the eyes.
- Take no more than one bath or shower per day, try to keep the shower within five minutes and use lukewarm water instead of hot water, especially when washing your face.
- Pat the skin dry after washing rather than rubbing. Be sure to thoroughly dry areas where skin touches skin, like under the arms and between the legs.
- Use mild, fragrance-free soaps and detergents.
- Protect your eyes from the sun and harsh weather, like extremely cold, dry or windy conditions.
- Use a humidifier to add extra moisture to the air. This is particularly useful if you live in an area with a harsh climate.
- Drink more water and increase your overall hydration.
When trying to heal dry skin around the eyes, there are just as many things to avoid as there are things to include. To help the healing process, you should avoid:
- Using substances that may worsen symptoms, including hot water, fragrant soaps, perfumes and makeup
- Touching, scratching or rubbing your eyes
- Spending time in the sun or in tanning beds
- Sweating (keep your environment cool — not cold — and minimize stress)
- Scrubbing the skin to exfoliate
SEE RELATED: Eyelid wipes and cleaning
Risk factors and prevention
While facial dryness is something everyone experiences at one point or another, there are certain factors that put someone at a higher risk. Risk factors may include:
- Being age 40 or older
- Having an underlying condition, such as psoriasis or eczema
- Living in a harsh climate
- Having a family history of dry skin
- Eating a poor diet that’s low in fats
- Having a medical condition that may cause dryness, such as diabetes, thyroid or kidney disease, or vitamin A deficiency
Some risk factors listed above are out of your control — you cannot prevent aging or inherited conditions. However, there are a few things you can do to lower your risk of developing dry patches on your eyelids. Incorporate these practices into your daily routine to avoid a flare up:
- Moisturize regularly.
- Bathe using warm water, not hot water.
- Avoid washing and drying your face using washcloths made from harsh or synthetic fabrics.
- Drink plenty of water each day to help hydrate from within.
- Use a humidifier in dry environments.
- Avoid triggers for a pre-existing dermal condition, like stress, allergens, irritants, fragrances, etc.
When to see an eye doctor
If you experience dry eyelids, an eye doctor can help identify the source of the problem and provide any necessary medical treatment.
You should schedule an eye exam if your symptoms worsen, for example, if flaky patches start to blister or eyelid swelling occurs.
An eye doctor may also be helpful if the steps you’ve taken at home haven’t helped your symptoms. Finally, seek medical attention if you notice vision changes or your eyes become affected. This may present as overly watery eyes, blurred vision or light sensitivity.
Eye health is important to your general well-being, so it’s typically a good idea to consult with an eye doctor if you notice any changes to your sight or eyes.
READ MORE about other causes of eyelid inflammation