What is Graves’ disease?
Graves’ disease is an immune system disorder that affects the body’s thyroid gland. The disease causes the body to produce too much thyroid hormone (hyperthyroidism). Some patients also develop thyroid eye disease (TED), which can cause eye-bulging, double vision and other eye problems.
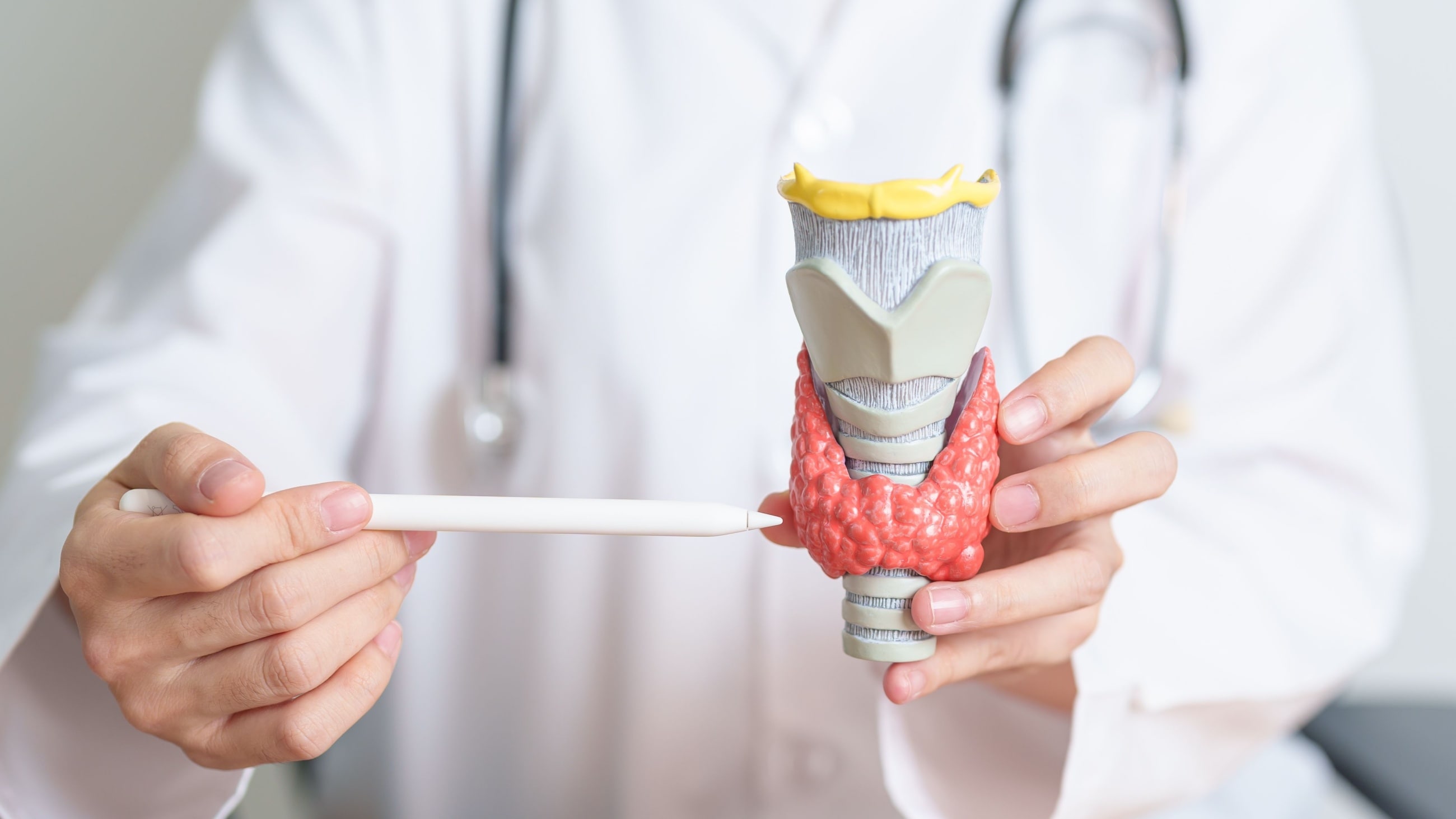
Graves’ disease and hyperthyroidism
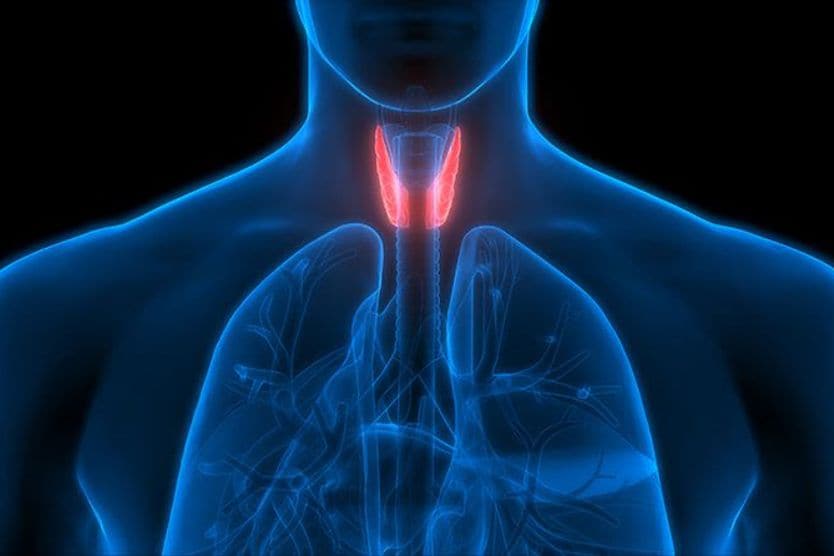
The thyroid is a small organ, shaped like a butterfly, that sits at the base of your neck. This gland makes thyroid hormones, which can affect your:
- Breathing
- Digestion
- Heart rate
- Mental health
- Metabolism
Different conditions can cause the thyroid to make too much thyroid hormone (hyperthyroidism) or too little thyroid hormone (hypothyroidism.) In Graves’ disease, the thyroid makes too much thyroid hormone.
Graves’ disease is the most common cause of an overactive thyroid. About one in 200 Americans has Graves’ disease.
Other causes of hyperthyroidism include thyroid inflammation, thyroid growths (nodules) that are usually benign, and too much iodine in the diet. If you have symptoms of an overactive thyroid, your doctor can do an exam and run tests to find out whether you have Graves’ disease.
Graves’ disease symptoms
Graves’ disease may cause symptoms related to the thyroid, skin and eyes. Having too much thyroid hormone can affect your body temperature, blood pressure, heart rate and even your mood.
Different people may have very different symptoms, and many won’t have all of the symptoms. Symptoms may include:
- Anxiety
- Brittle fingernails
- Bulging and/or swollen eyes (Graves’ eye disease)
- Diarrhea or frequent bowel movements
- Enlarged thyroid (goiter) that may make your neck look swollen and/or cause problems with swallowing
- Hair loss
- Hand tremors
- Heart palpitations
- Increased appetite
- Irritability
- Muscle weakness
- Racing or irregular heartbeat
- Thick, reddish skin on the shins or feet (Graves’ dermopathy)
- Trouble tolerating heat
- Tiredness and sleep issues
- Weight loss
Not everyone with Graves’ disease will have eye symptoms or skin symptoms. In fact, it’s pretty rare for Graves’ disease patients to have Graves’ dermopathy.
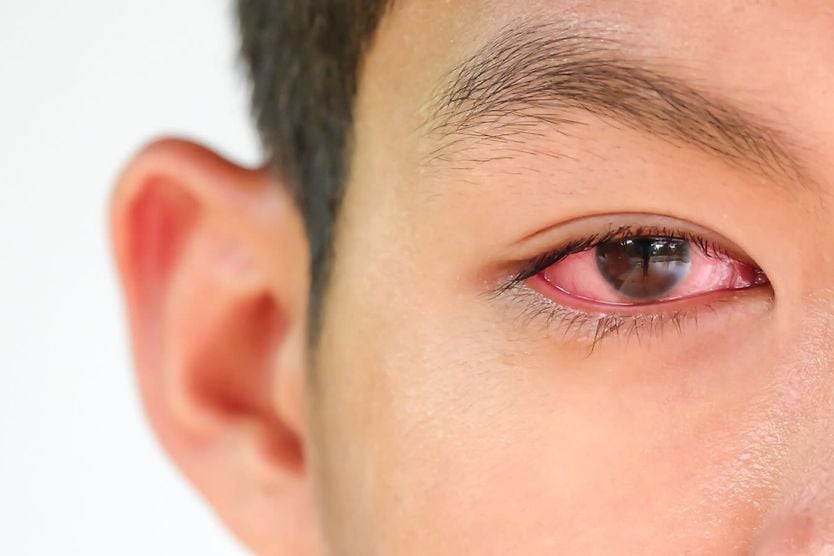
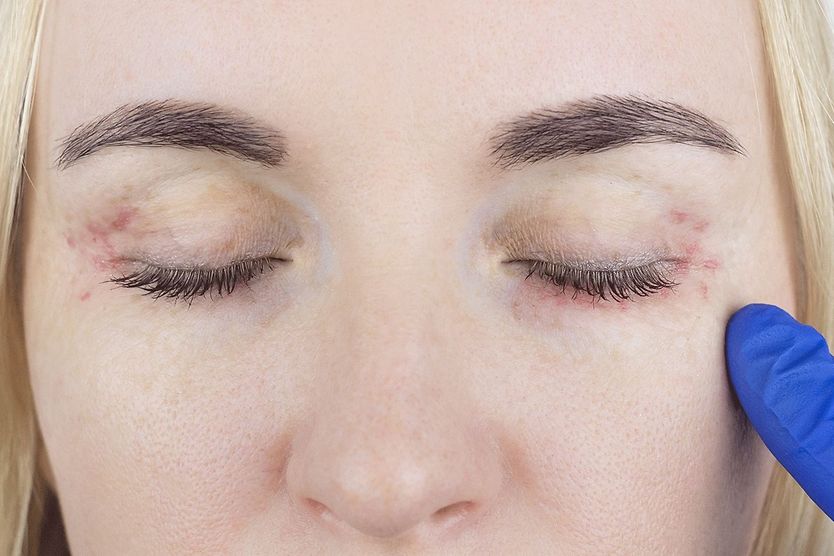
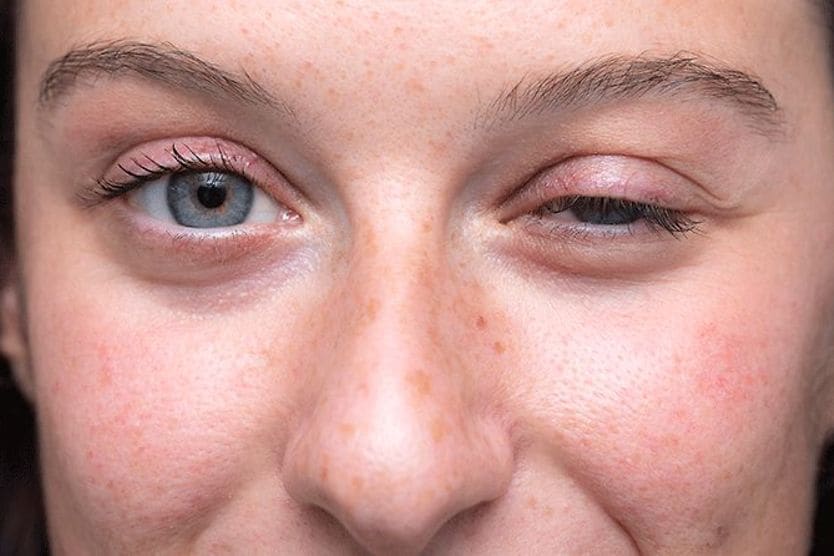
Graves’ disease and the eyes
TED occurs in 25-50% of people who have Grave’s disease. It also is known as Graves’ eye disease (GED) and Graves’ ophthalmopathy (GO).
Graves’ eye disease causes inflammation and swelling in and around the eyes that can make the eyes bulge. It may cause permanent damage to the eyes. GED also can cause other symptoms, including:
- Blurry vision
- Double vision
- Eye pain
- Irritation and a feeling of grittiness
- Eye misalignment (strabismus)
- Redness
- Sensitivity to light
- Vision loss
An eye doctor may use blood tests, eye measurements and imaging to diagnose thyroid eye disease. Many patients with thyroid eye disease have an overactive thyroid (hyperthyroid), which is most commonly caused by Graves’ disease. But not all patients with TED have Graves’ disease or even hyperthyroidism.

What causes Graves’ disease?
Your immune system keeps you healthy by fighting off bacteria, viruses and other pathogens that can make you sick. But your immune system also can cause disease if it attacks your body by mistake.
Graves’ disease develops when the immune system makes an antibody that stimulates the thyroid gland to grow and to make more thyroid hormones than the body needs, causing a variety of symptoms and health problems.
Some people have genes that make them more likely to get Graves’ disease. These genes may get “switched on” by a variety of factors such as illness, extreme stress or pregnancy. Smoking also increases the risk.
Who gets Graves’ disease?
Anyone can get Graves’ disease, but some people are more likely to get it than others. Factors that may increase risk include:
- Sex – It occurs about seven to eight times more often in women than men.
- Age – Graves’ disease is most common in patients ages 30 to 50.
- Other conditions – Patients with other autoimmune conditions like celiac disease, lupus, rheumatoid arthritis, type 1 diabetes and other conditions are more likely to get Graves’ disease.
A family history of Graves’ disease or other thyroid or autoimmune diseases may make you more likely to get Graves’ disease. If you have Graves’ disease symptoms, your doctor will ask questions about your medical history and your family medical history when making a diagnosis.
How is Graves’ disease diagnosed?
If you have any symptoms of hyperthyroidism, it’s important to see your doctor right away. Your doctor will do a physical exam, take a family history and use one or more tests to make a diagnosis.
Tests for Graves’ disease may include:
- Antibody test – A blood test can find antibodies (TRAb or TSI) that will only exist in your body if you have Graves’ disease.
- Blood test for thyroid hormones – Lab tests can measure thyroid hormones (T3, T4 and TSH) in your blood to see if your thyroid hormone levels are higher than normal.
- Radioactive iodine test – The thyroid uses iodine to make thyroid hormones. A radioactive iodine uptake test can check the amount of iodine your thyroid takes up.
- Ultrasound – An ultrasound can allow your doctor to see if the thyroid is enlarged. An ultrasound may be used for pregnant patients who can’t safely undergo a radioactive iodine test because it can cause damage to the fetus.
- CT scan or MRI – In some cases, a doctor may order further imaging to confirm a diagnosis.
A diagnosis of hyperthyroidism does not necessarily mean the patient has Graves’ disease. However, symptoms of thyroid eye disease or thyroid skin disease combined with hyperthyroidism may help a doctor confirm the diagnosis.
Graves’ disease treatments
It’s important to get prompt treatment for Graves’ disease. Without treatment, hyperthyroidism can lead to blood clots, heart problems, stroke, osteoporosis and pregnancy complications like miscarriage or low birth weight.
Untreated or improperly treated Graves’ disease also can cause a health emergency known as a thyroid storm. A thyroid storm is a sudden surge of thyroid hormone that can cause symptoms such as:
- Fever
- Seizures
- Weakness
- Yellowing of the skin and the whites of the eyes (jaundice)
- Vomiting
- Coma
The main goal of treatment is to stop the thyroid from making too much thyroid hormone and to reduce symptoms. Treatments include medication, surgery and radioiodine therapy.
Medication
Antithyroid medicines. The least invasive treatment for Graves’ disease, antithyroid medications, lessen the amount of hormone the thyroid makes. Common antithyroid medications include methimazole and propylthiouracil. A doctor may choose propylthiouracil for patients in the first trimester of pregnancy due to a lower risk of birth defects.
Both drugs gradually make the thyroid less active and lower the amount of hormones the thyroid makes. It can take weeks or months to get thyroid hormone levels into a normal range. You may have to take antithyroid medicine for one to two years or longer if you decide not to have surgery or radioiodine therapy.
You should tell your doctor if you have any side effects after you start taking antithyroid medications. Side effects may include:
- Bruising
- Fever
- Itchy skin or rashes
- Lack of appetite
- Sore throat
- Stomach pain
- Tiredness
- Weakness
- Yellowing of skin or whites of eyes (jaundice)
It’s very uncommon, but antithyroid medications can cause serious problems such as liver failure. These medicines can also reduce the number of white blood cells, which may lead to an infection.
Beta-blockers. Doctors sometimes prescribe beta-blockers to ease symptoms while antithyroid medicines are starting to work. Beta-blockers are drugs that are usually used to lower blood pressure and prevent heart attacks. These drugs block the effects of thyroid hormone and can reduce some symptoms right away.
Radioiodine therapy
Another treatment option is radioiodine therapy. This treatment cannot be used for pregnant patients because it can harm the fetus. In radioactive iodine therapy, you take radioactive iodine by mouth. This therapy destroys the thyroid slowly without surgery. Most patients who get radioiodine therapy will develop an underactive thyroid and will need to take thyroid hormones daily.
Surgery
Some patients have a very enlarged thyroid (goiter) or have serious side effects from antithyroid medications. In these cases, a doctor may recommend surgery to take out the thyroid.
Thyroid surgery for may involve removing all of the thyroid (thyroidectomy) or part of the thyroid (subtotal thyroidectomy). It’s important to choose a doctor who has experience with thyroid surgery.
Risks of thyroid surgery may include:
- Nerve damage that can affect your vocal cords.
- Injury to the parathyroid glands that regulate your blood calcium levels.
Patients who have had all or part of their thyroid removed will need to take thyroid hormones every day for life and get their thyroid hormone levels checked regularly.
Graves’ eye disease treatment
Thyroid eye disease can occur before, during or after diagnosis with Graves’ disease. It can also happen in patients who don’t have Graves’ disease or even hyperthyroidism.
TED typically has two phases: an active phase and an inactive phase. During the active phase, symptoms may continually get worse and tissue damage may occur around the eyes. In the inactive phase, a patient still may experience some symptoms or have lasting eye changes.
Patients who have thyroid eye disease also will need to see an eye doctor with experience treating this condition. Treatment will depend on your symptoms.
Treatment for TED may include:
- Corticosteroids – Prednisone can reduce swelling behind the eyes, but side effects may include high blood pressure, weight gain and mood issues.
- Eye patch – An eye patch can help to treat double vision caused by Graves’ eye disease.
- Glasses with prisms – Special glasses that contain prisms may correct double vision caused by Graves’ eye disease.
- Head elevation – Propping your head higher than the rest of your body while you sleep can lessen eye swelling.
- Lubricating eye drops – Artificial tears and lubricating drops or gels can help keep eyes moist and reduce eye pain and irritation caused by thyroid eye disease.
- Medication – A newer drug for thyroid eye disease, teprotumumab-trbw, was approved by the U.S. Food and Drug Administration. The drug may reduce TED symptoms and signs like double vision and eye-bulging. Your eye doctor might work with an endocrinologist, a specialist who treats disorders of the endocrine system, which includes the glands and organs that produce hormones.
- Sunglasses – Protecting the eyes from UV rays can both help with light sensitivity and hide cosmetic issues caused by Graves’ eye disease.
- Surgery – There are different types of surgery for thyroid eye disease that can be used to treat cosmetic issues or vision problems. For example, strabismus surgery may be used for misaligned eyes. Orbital decompression surgery, which involves removing bone or fat around the eye (orbital fat), may be used to lessen eye-bulging. This surgery is usually used to prevent vision loss that may be caused by pressure on the optic nerve.
See your eye doctor for an exam
Regular eye exams are important for your eye health and because eye exams can reveal health problems like Graves’ eye disease. In some cases, your eye doctor may be the first health care provider to spot signs of Graves’ disease.
If you’re due for a comprehensive eye exam, make sure to get one on the calendar soon.