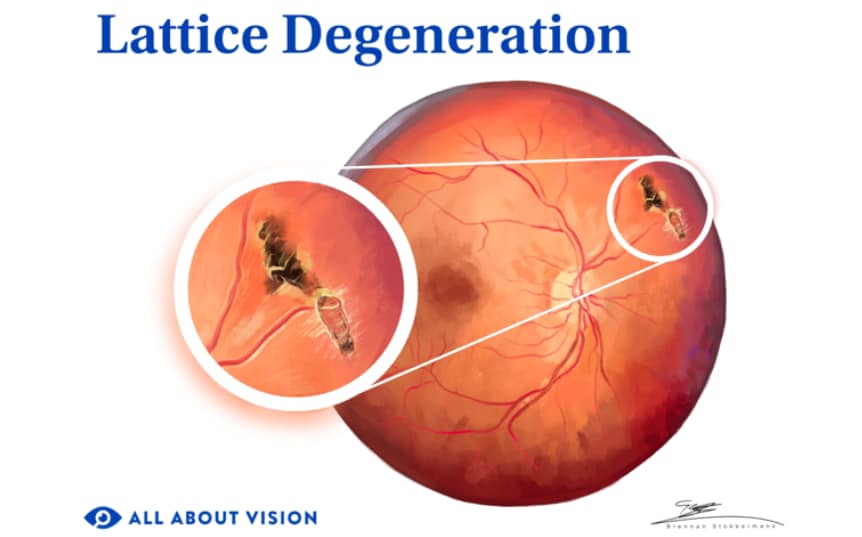
What is lattice degeneration?
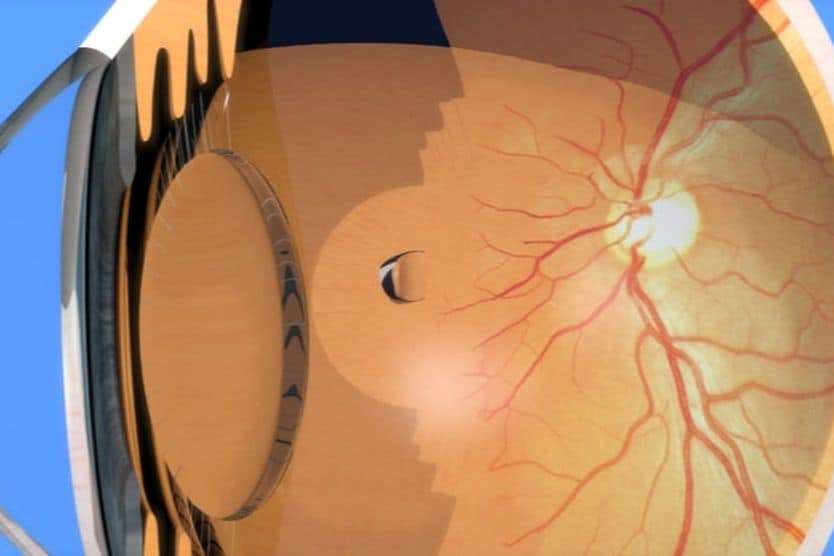
Lattice degeneration is a condition in which there are thinning areas in the periphery (outer portion) of the retina. It usually does not progress or cause symptoms, but it can increase the risk of developing retinal tears, holes or breaks. These can lead to retinal detachment.
The retina — the eye's light-sensitive tissue — is a curved, circular area at the very back of the eye. Retinal detachment, left untreated, can result in blindness. Fortunately, it only occurs in a small number of people with lattice degeneration. But this type of peripheral retinal thinning is present in about a quarter of the eyes that do develop a detachment.
Lattice degeneration often occurs in both eyes and is found in about 10% of the population. It is seen more often in people with myopia and tends to run in families.
Causes of retinal thinning
The precise cause of lattice degeneration is not well understood, though it is a common condition. It is not passed down from parents, but some hereditary factors are associated with it.
Myopia
People with myopia (nearsightedness) are more likely to have lattice degeneration. One study found that 1 in 3 myopic eyes had lattice degeneration compared to about 1 in 10 in the general population.
Myopes have a higher risk of retinal detachment, and it is thought that lattice degeneration may be a risk factor contributing to this. The most common type of myopia results from the eyeball growing longer. As the eyeball grows longer, lattice degeneration is seen more commonly.
READ MORE: Types of myopia and the increased risk of eye complications
Family history
Lattice degeneration can run in families, though it is not inherited directly from parents. People with a family history are more likely to have the condition.
Certain genetic conditions are also associated with lattice degeneration. They sometimes cause degeneration of the retina and vitreous — the fluid in the middle of the eye. These include:
- Stickler syndrome – A condition that affects the connective tissue of the body. Complications can impact many body systems, including the eyes, ears, joints and skeleton.
- Marfan syndrome – A condition that causes improper protein production in connective tissue. It can impact many body parts, including the eyes, skin, heart, blood vessels and bones.
- Ehlers-Danlos syndrome – A group of conditions caused by abnormal collagen protein in the connective tissue. It can affect the eyes, heart, spine, gums and teeth.
Lattice degeneration symptoms
Lattice degeneration does not cause vision symptoms. This is because the retinal thinning is in the periphery, not the center. The central retina provides our straight-ahead vision. Since there are no lattice degeneration symptoms, it is possible to be unaware of it. It is typically found during routine comprehensive eye exams.
Because there is retinal thinning in some areas, there is a higher risk that the tissue could break or detach. A detachment, if not treated promptly, can lead to blindness. Due to this, it is critical to know the symptoms.
Symptoms of a retinal tear or detachment include:
- Floaters
- Flashes of light
- Blurry vision
- A “curtain” blocking some of your peripheral (side) vision
Contact a doctor immediately if you notice these symptoms.
In patients with lattice degeneration, the long-term risk of retinal detachment ranges from 0.5% to 0.7%. This means about 5 to 7 of 1,000 people with lattice degeneration will develop a detachment.
The most common type is a rhegmatogenous detachment (RRD). This occurs when the retina is torn, and fluid enters behind it. This forces the retina away from the layer underneath and leads to a detachment. About 20% to 30% of people who develop an RRD are found to have lattice degeneration.
LEARN MORE: Common questions about retinal detachment
How is lattice degeneration diagnosed?
Lattice degeneration is diagnosed in the clinic during a dilated eye exam. The absence of lattice degeneration symptoms means it can only be found by viewing the retina.
An eye doctor must dilate the eyes with eye drops to see lattice degeneration. This is because the condition occurs in the outer edges of the retina, and small pupils will not allow a view of the retina’s outer boundaries.
An instrument called a binocular indirect ophthalmoscope (BIO) is used to see lattice degeneration in the peripheral retina. A BIO looks like a headband with a light and viewing lens attached. The exam is often done in a reclined position, and the patient is asked to look in different directions. An additional lens the doctor holds allows them to focus on the retina, providing a high-resolution view.
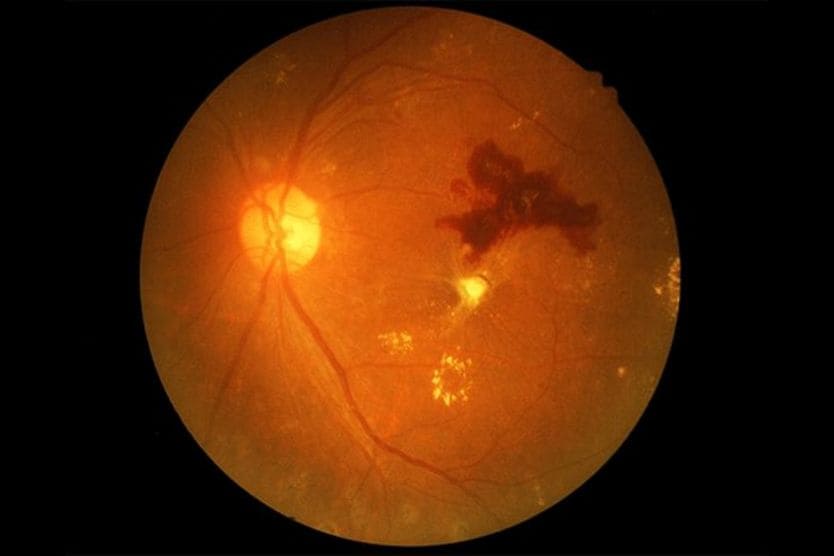
If the doctor sees pigmented areas in the shape of ovals or lines, they may suspect that retinal thinning has occurred. White patches, pockets of red and spots with white-yellow coloration may also be seen in lattice degeneration.
Treatment for lattice degeneration retinal thinning
Lattice degeneration cannot be medically treated or prevented. However, treatment is usually not needed. This type of retinal thinning doesn't cause symptoms and is usually not progressive.
While the risk of a retinal tear, hole or detachment is higher in people with lattice degeneration, most people will not experience these complications. More than likely, an eye doctor will monitor the condition during routine follow-up appointments.
If they detect one of these complications, they will recommend appropriate treatment.
Treatments for complications
There are no treatments for lattice degeneration. Laser treatments or other surgical procedures, however, may be necessary to treat its complications. A break or hole in the retina can cause it to become detached, leading to blindness.
Retinal laser photocoagulation
If a break or detachment develops due to lattice degeneration, laser photocoagulation may be used to repair it. This special type of laser produces a small burn area, promoting scar tissue growth. Small detachments or holes in the retina can be "welded" down with the scar tissue to avoid further vision loss.
Additional treatments for complications:
- Cryopexy – This procedure involves using a probe to freeze the tissue surrounding a retinal tear or detachment. It leaves behind a scar that will aid in reattaching the retina.
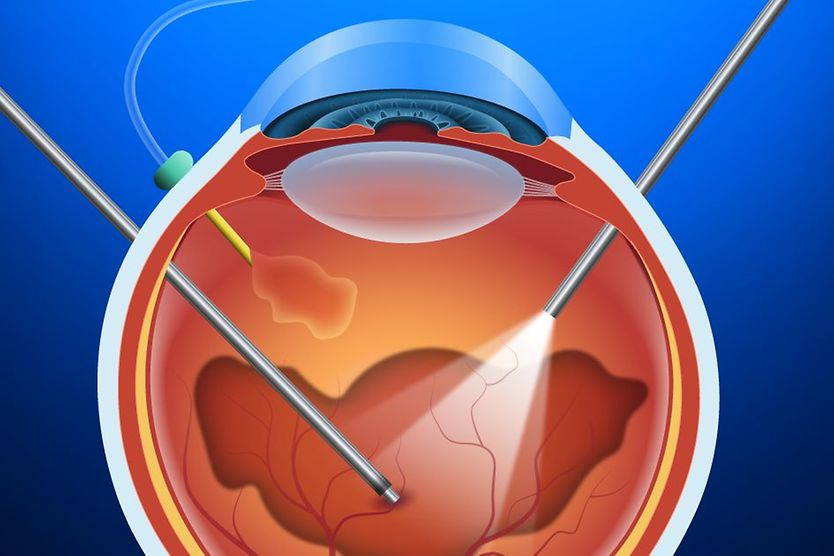
- Vitrectomy – A vitrectomy removes the gel-like substance inside the eye to lessen the traction on the retina.
- External needle drainage – This procedure drains the fluid under the retina, aiding reattachment.
- Pneumatic retinopexy – This procedure involves injecting a gas bubble into the eyeball. The bubble provides light pressure against the retina, aiding reattachment.
- Scleral buckle – This procedure places a silicone band on the outside of the eyeball to help prevent the retina from detaching again.
READ MORE: Laser photocoagulation eye surgery: Uses, benefits and what to expect
Eye vitamins for lattice degeneration
A healthy diet and lifestyle do benefit the overall health of the eyes. But there are no studies that show that vitamins can directly prevent or treat lattice degeneration. Follow your doctor’s guidelines on any vitamin supplements they recommend.
When to see a doctor
There are no lattice degeneration symptoms, so many people do not know they have it. An important step you can take to safeguard the health of your eyes is to have routine eye exams.
If you have been diagnosed with lattice degeneration, it is important to attend all of your follow-up exams. Follow your eye doctor’s recommendations for how closely you should be monitored.
Overall, the risk of retinal detachment is low in eyes with lattice degeneration. Most people with the condition will not develop this complication. However, it is important to know the symptoms of retinal detachment. These include the sudden onset of floaters, flashes of light, blurry vision or a dark curtain coming over your side vision.
Be aware of the signs of a retinal tear or detachment so you can seek treatment right away if necessary.