What is vernal conjunctivitis?
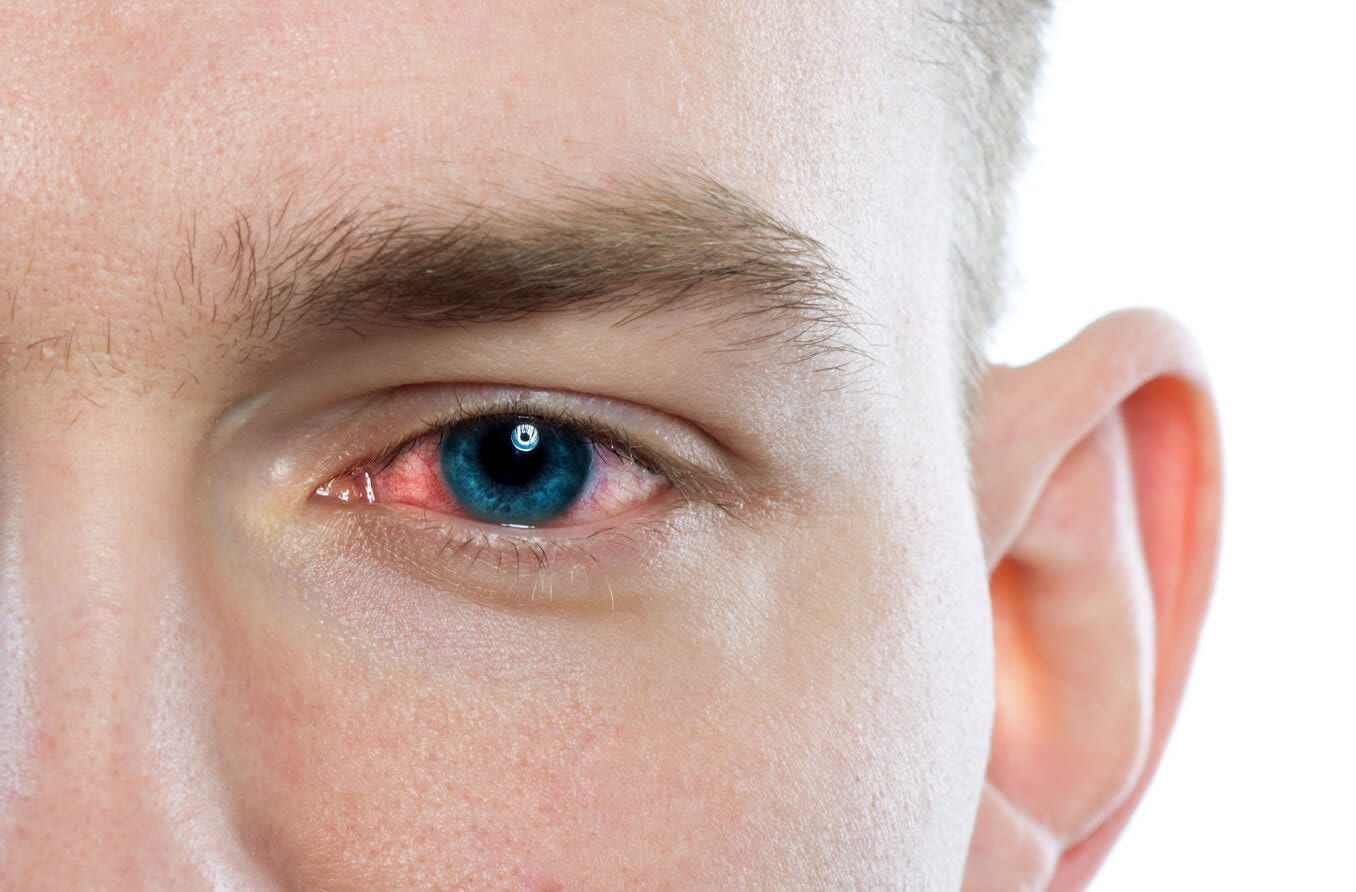
Vernal conjunctivitis is a severe form of allergic conjunctivitis. It can cause symptoms like itching and burning eyes, as well as tearing and light sensitivity. It most commonly affects young men and boys between the ages of 3 and 25 during the warmer, drier months of the year.
Vernal conjunctivitis vs. allergic conjunctivitis
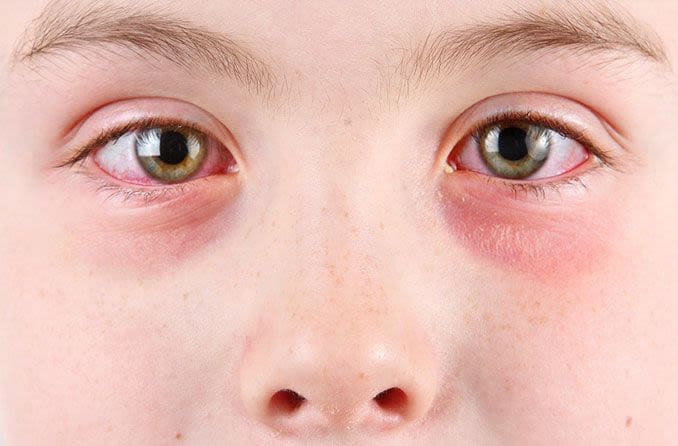
Allergic conjunctivitis (also called eye allergies) develops when allergies affect the eyes. The most telltale symptoms of eye allergies are redness, inflammation and eye watering. Many people experience mild to moderate discomfort from allergic conjunctivitis.
Eye allergies are usually caused by airborne allergens. They can be seasonal, but some people have eye allergies year round.
Seasonal allergies often reach their peak during the spring and summer and go away during the winter. This correlates to the life cycles of most plants. Perennial allergies often last all year. This is because their sources aren’t influenced by the seasons.
Seasonal allergies come from:
- Pollen
- Grass
- Weeds
- Mold spores
Perennial allergies are most often caused by animal dander and dust mites.
Vernal conjunctivitis is a type of allergic conjunctivitis usually caused by seasonal allergens. But it’s important to note that this condition can often be more rare and severe than typical eye allergies.
Like other types of allergic conjunctivitis, vernal conjunctivitis affects the conjunctiva. The conjunctiva is the mucous membrane that covers the sclera (the white of the eye) and the inner surface of both eyelids. It provides protection and lubrication and helps produce tears and mucus.
Vernal keratoconjunctivitis
Vernal keratoconjunctivitis (VKC) is a subtype of vernal conjunctivitis. It develops when the condition spreads to the cornea.
Keratoconjunctivitis is a combination of keratitis and conjunctivitis, which impact the eyes differently. In the case of vernal conjunctivitis, the conjunctiva is always affected, but the cornea may not be. If the cornea is involved, the term vernal keratoconjunctivitis may be used instead.
It’s been shown that most cases of vernal conjunctivitis are severe enough to be considered VKC.
What are the symptoms of vernal conjunctivitis?
Some of the most common symptoms experienced with vernal conjunctivitis include:
Along with these symptoms, vernal conjunctivitis can also cause visible signs, such as:
- Giant papillae, which take the form of bumps on the inner lining of the eyelid.
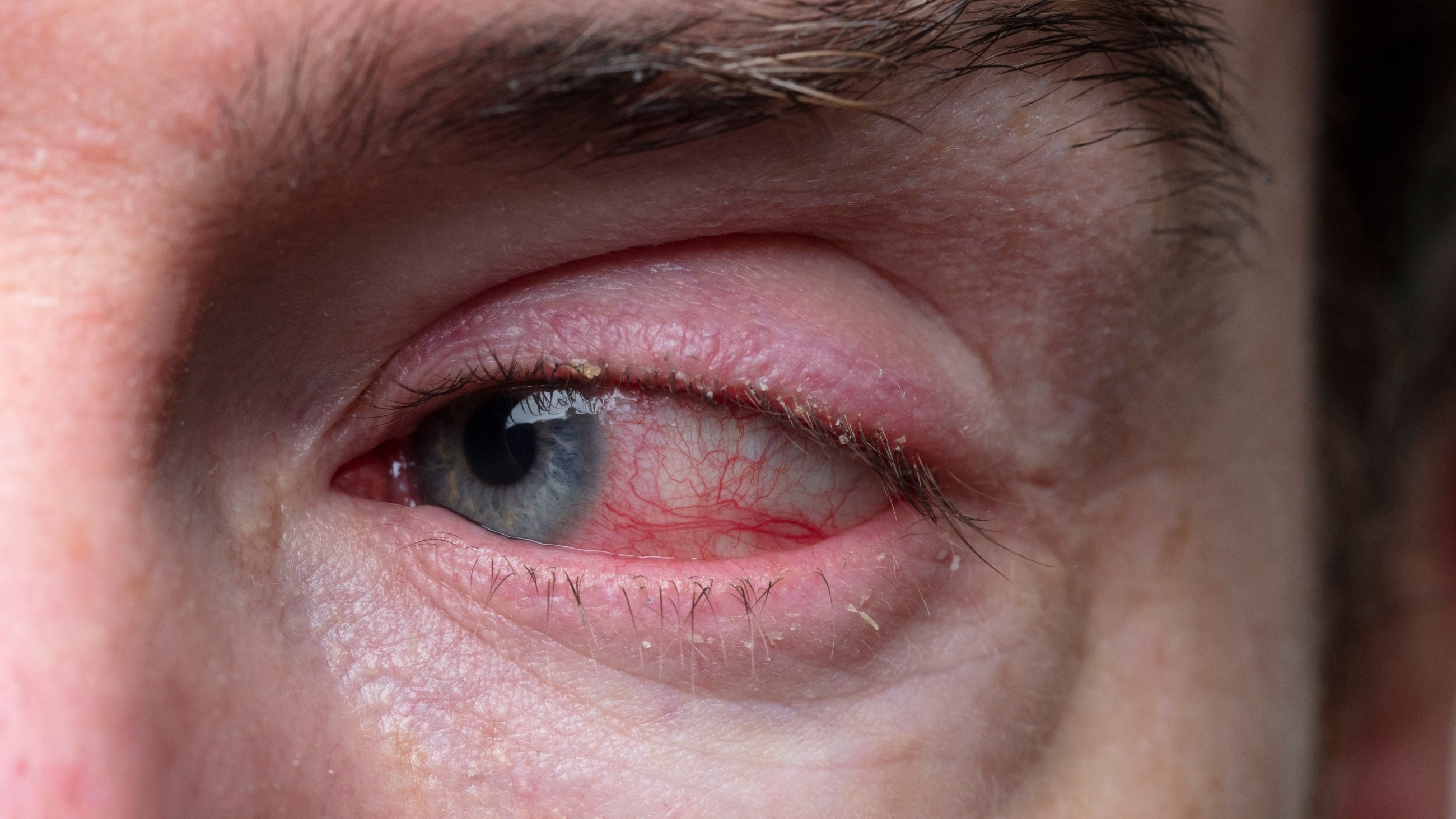
- Superficial keratitis, which makes the cornea appear bloodshot and may cause light sensitivity.
- Conjunctival hyperemia, which makes the outer eye membrane look red due to dilated blood vessels.
In more extreme instances, the cornea can develop a shield ulcer (scar), or the lens of the eye may become clouded. This can lead to vision impairment. Shield ulcers are a symptom of severe vernal conjunctivitis, developing in 3% to 11% of cases.
LEARN MORE: Types and causes of corneal ulcers
What are the risk factors?
Knowing the risk factors for vernal conjunctivitis can help prepare someone if they start to notice the symptoms. This condition is often more prevalent in people with a long family history of allergies.
It is also found in patients who have a history of the following:
- Allergic rhinitis
- Asthma
- Eczema
Vernal conjunctivitis tends to be more common in men and boys than in women and girls.
Male patients between the ages of 3 and 25 who have a history of allergies are the most at-risk for VC. This condition is also more likely to develop in people who live in warm, dry climates.
Like other seasonal allergies, vernal conjunctivitis will typically resolve during the colder months.
How is vernal conjunctivitis treated?
There are a few options available to treat vernal conjunctivitis. These include mast cell stabilizers and antihistamines, or a combination of the two.
Mast cell stabilizers are shown to be effective at reducing symptoms like:
- Itching
- Mucous discharge
- Hyperemia (eye redness)
Antihistamines are also useful at reducing itchiness, which can provide some relief.
Both of these medications are eye drops and should be applied as directed by your eye doctor. They are prescribed for prevention and management. Treatment can start about a month before the allergy season begins.
If vernal conjunctivitis causes inflammation or shield ulcers, treatment may include:
- A topical steroid paired with an antibiotic.
- A cycloplegic agent.
Cool compresses may also be applied to reduce swelling.
If the condition doesn’t respond to these treatments, other options (like cyclosporine) might be useful.
Is vernal conjunctivitis contagious?
Vernal conjunctivitis is not a contagious condition. Since it’s caused by seasonal allergens, patients cannot pass this illness on to others. However, it’s important to learn about the risk factors. This way, you'll know what steps to take if any symptoms start to develop.
SEE RELATED: Is pink eye contagious?
Should I see a doctor?
Vernal conjunctivitis is a rare and serious type of allergic conjunctivitis. It can only be diagnosed in a clinical setting, based on the patient’s medical history and an eye exam.
You should always see an eye doctor if you suspect that you have vernal conjunctivitis. They will be able to diagnose the condition and recommend the appropriate treatments.