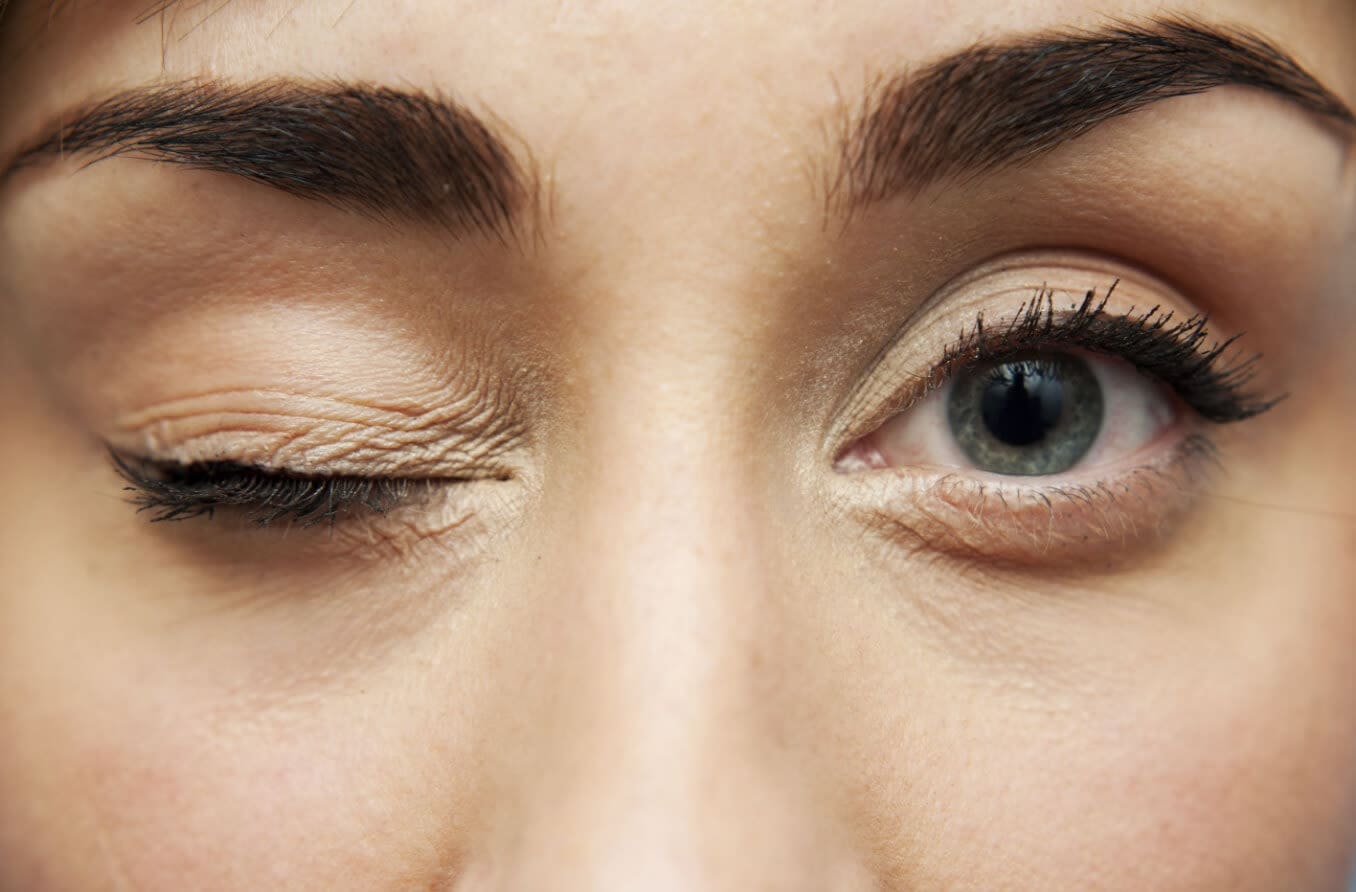
What is apraxia of eyelid opening?
Apraxia of eyelid opening, also known as ALO, is a condition in which a person is unable to intentionally open their eyes after closing them. ALO can be caused by certain diseases, a side effect from some medications or other factors. It typically occurs in older people.
Causes of eyelid apraxia
Apraxia of eyelid opening can develop on its own, but it is rare. It is most often seen along with blepharospasm — involuntary spasms of the eyelids.
Note: Blepharospasm is different from ALO. In blepharospasm, blinking is affected, and the eyes will close involuntarily. In ALO, blinking is not affected, and the eyes do not close involuntarily; it is just hard to open the eyes again after they have been closed.
Disorders and diseases that can cause ALO include:
- Motor neuron disease – A class of progressive diseases that damage motor neurons. These neurons control muscle movements.
- Progressive supranuclear palsy – A neurological disorder that affects body movements, such as walking, speech and eye movements.
- Parkinson’s disease – A degenerative brain disease that affects muscle control and movement.
- Shy-Drager syndrome – A progressive neurological disorder that affects the nervous system. It is also called multiple system atrophy with orthostatic hypotension.
- Hydrocephalus – A neurological disorder caused by a build up of fluid in the brain.
- Choreoathetosis – A neurological disorder that causes uncontrollable muscle movements, often beginning in childhood.
- Huntington’s disease – A disorder that affects parts of the brain that control movement. It is an inherited disease that is usually seen in middle-aged people.
- Myasthenia gravis – An autoimmune disease that causes muscle weakness.
- Multiple sclerosis – An autoimmune neurological disease that causes muscle spasms and muscle weakness.
- Idiopathic focal dystonia – Involuntary muscle contractions in a part of the body with no particular cause.
- Brain lesions – Central nervous system lesions on certain parts of the brain, including the non-dominant hemisphere, the medial frontal lobe, the basal ganglia and rostral brain stem.
Inflammations of the eye can also cause ALO. They include:
- Blepharitis – Inflammation of the eyelid
- Keratitis – Inflammation of the cornea
- Conjunctivitis – Inflammation of the conjunctiva
Other causes of apraxia of eyelid opening include:
- Dermatochalasis – Skin on the upper and lower eyelids that is loose, usually seen in middle-aged and older people
- Abnormal development of the levator palpebrae superioris muscle, which is the muscle used to raise the upper eyelid
- Side effect from eye surgery
- Being outdoors in the sunlight for long periods
- Side effect from medications, including lithium, sulpiride and MPTP
- Trauma
- Sleep
Symptoms
Symptoms of ocular apraxia include:
- One or both eyes opening slowly.
- The inability to open one or both eyes voluntarily from the closed position.
- Eyelid muscle contractions.
In order to open their eyes, patients may:
- Toss their head back, using the movement to try and open their eyes.
- Use their fingers to open their eyes.
- Rub the eyebrows or eyelids.
Symptoms do not appear when blinking. They also do not appear when the eyes are open. Symptoms usually only appear when the eyes are closed, and then the patient cannot open their eyes without assistance.
Diagnosis
If you are experiencing any symptoms of ALO, your doctor will go over your medical history, including eye health history. A variety of exams and tests are used to diagnose ALO.
These may include:
- Physical exam
- Visual exam
- CT scan or MRI if the cause is believed to be related to the nervous system or to locate a possible lesion
- Electromyography (EMG) – A test used to check the health of the muscles and nerves in your body
Differential diagnosis
Like blepharospasm, other diseases exhibit similar symptoms to ALO and should be ruled out.
These include but are not limited to:
- Meige syndrome – A nervous system disorder that involves spasms of the eye muscles and other facial muscles. It also includes blepharospasm.
- Bell’s palsy – A condition that causes numbness or weakness on one side of the face, and can lead to a drooping eyebrow.
- Hemifacial spasm – A neuromuscular disorder that causes muscle spasms on one side of the face.
- Ocular myasthenia gravis – An autoimmune disease that weakens the muscles around the eye, causing fatigue, among other symptoms.
- Parkinson’s disease.
Side effects from certain mood stabilizers, antimicrobials and antiarrhythmics can also present symptoms of ALO. A brain injury should also be ruled out in order to properly treat symptoms.
Treatment options
A common treatment for some types of ALO is botulinum toxin. The doctor injects the medication upper and lower eyelids that allows the eyelids to close. More injections may be needed over time. While botulinum toxin can help with ALO, drooping eyelids are a possible side effect of the injections.
Certain anti-Parkinson’s medications, including levodopa and trihexyphenidyl, have been prescribed. Valproic acid, an anticonvulsant, has also shown to improve symptoms in some individuals.
Depending on the cause, certain surgical procedures are also available, including:
- Removal of excess eyelid skin, if dermatochalasis is the cause.
- Tightening the tendon that raises the eyelid, for drooping of the upper eyelid.
- Orbicularis myectomy – a procedure in which the surgeon removes the orbicularis muscle fibers in the eyelid. This can help the patient have more muscle control of the eyelid.
- Frontalis suspension – a procedure in which the forehead muscle is attached to the eyelids. This allows the lid to open.
If apraxia of eye occurs due to other underlying diseases, then treatment for those diseases is important in order to improve symptoms.
Prognosis and living with eyelid apraxia
If the patient responds well to treatment, then the prognosis for ALO is positive. However, if symptoms return after treatment, the patient’s independence may become compromised. Job tasks and daily habits may be more difficult.
In addition to both your primary care doctor and eye doctor, a neurologist, movement disorder specialist and/or occupational therapist may be needed. A case manager and social worker might also be helpful with disabilities that occur from apraxia of eyelid opening.
A comprehensive medical team is important and can assist those living with ALO.