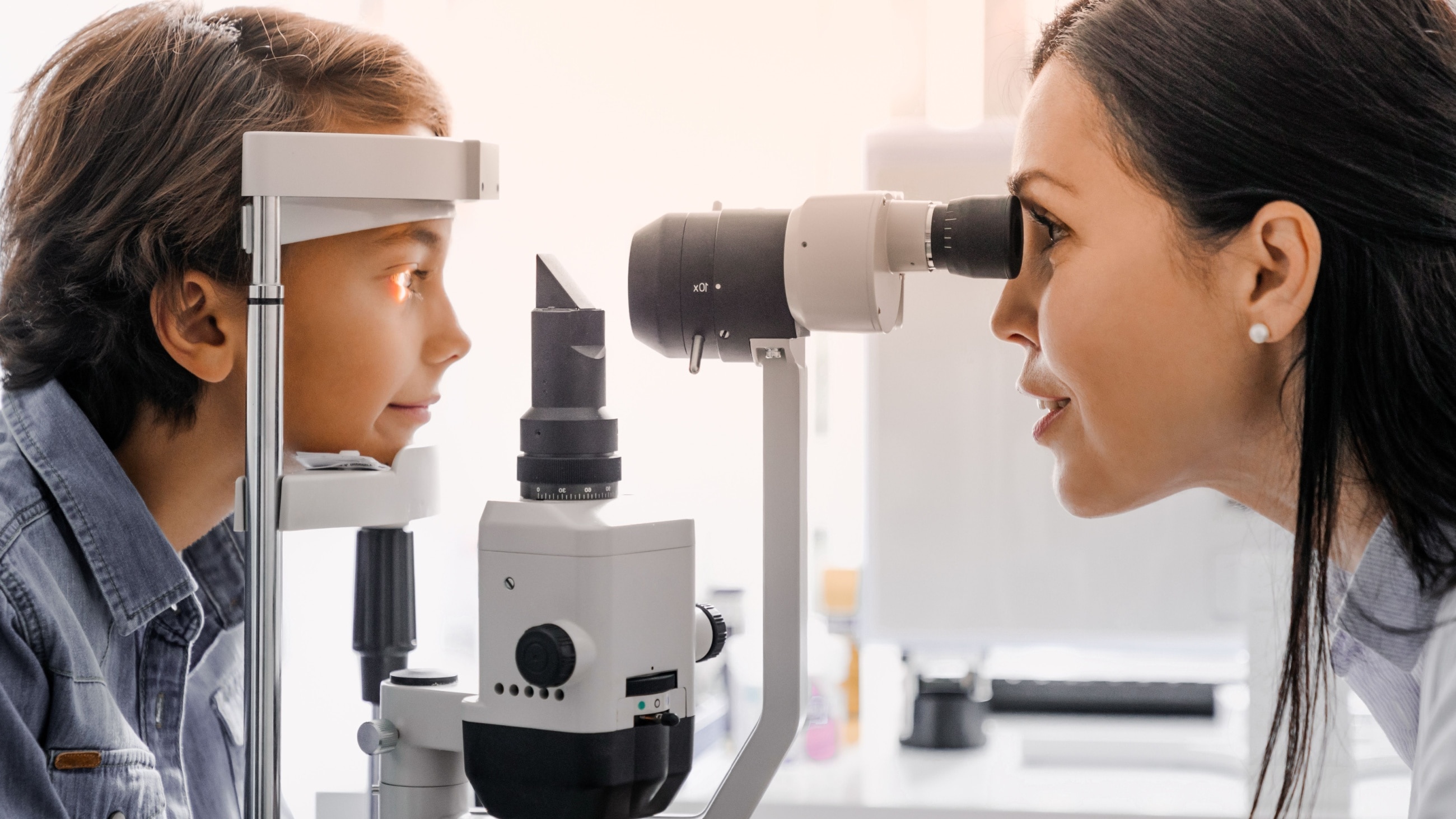
An introduction to buphthalmos
Buphthalmos is the medical term for an enlarged eyeball. This condition can be congenital (present at birth) or develop in the early childhood years. It typically results from increased pressure in the developing eye, which causes the eyeball to stretch. Buphthalmos is often treatable if addressed early.

High intraocular pressure (IOP), or pressure inside the eye, leads to stretching of the cornea (the dome-shaped barrier at the front of the eye) and the sclera (the white of the eye, which helps form the eyeball’s shape). This leads to the large appearance of the eyes characteristic of buphthalmos. The term buphthalmos is derived from the words for “ox” and “eye” in Greek.
An infant’s eyes are very soft and elastic, meaning they stretch easily. This makes them more susceptible to stretching from elevated IOP.
When the eyeball is stretched, it can cause a condition called axial myopia. This is when the eyeball becomes too long, which changes the way the eye is able to process light. (“Myopia” refers to near-sightedness, or difficulty seeing distant objects clearly.)
Studies have found that buphthalmos is rare, occurring in an estimated 1 out of every 30,000 births. It can affect one or both eyes.
The most important aspect of managing buphthalmos is to control IOP. With early treatment and intervention, the most serious effects can often be prevented.
What causes buphthalmos?
Congenital glaucoma and infantile glaucoma (which develops within the first three years of life) are the most common causes of buphthalmos.
Glaucoma refers to a group of diseases that affect the optic nerve, which is a nerve in the back of your eye that sends visual information to your brain. Babies with congenital glaucoma are born with eyes that can’t drain fluid like normal. The fluid builds up, which increases the IOP. This can stretch the eyeball, leading to buphthalmos as well as damaging the optic nerve.
Buphthalmos is a genetic condition, which means it can occur in babies who inherit certain genes from their parents. Because of this, it can’t be prevented. Many parents may not even be aware they are carrying these genes. Congenital glaucoma may also sometimes be inherited.
Additionally, conditions such as the following can cause or be related to buphthalmos:
- Neurofibromatosis Type 1 – A condition that causes tumors to develop on the nerves in the spinal cord, brain or skin. Symptoms sometimes involve growths in the eye, leading to vision problems.
- Aniridia – The partial or complete absence of the iris (the colored part of the eye positioned behind the cornea).
- Sturge-Weber syndrome – A rare neurological condition that affects the development of capillaries (small blood vessels) in the brain, eyes and skin. A key feature of Sturge-Weber syndrome is a large port-wine birthmark located near the eye.
READ MORE: Ocular hypertension: 5 causes of high eye pressure
Buphthalmos vs. exophthalmos
The eye is enlarged in buphthalmos, but the eyeball is actually a normal size in exophthalmos. Exophthalmos happens when the eyeball is pushed forward, displaced by other contents of the orbit (the eye socket). It is often due to problems with the thyroid gland, but it can also be caused by infection or injury in the eye area and other factors.
Signs of buphthalmos in babies

Certain features are commonly found in cases of buphthalmos, including:
Enlarged eyes
The most obvious sign of buphthalmos in babies is a larger-than-normal eyeball, including the iris. One or both eyeballs may appear enlarged.
Watery or light-sensitive eyes
If a baby has buphthalmos, their eyes may water or tear up easily (epiphora). They may be very sensitive to light (photophobia), and their eyes might look cloudy. These are also common signs and symptoms of congenital glaucoma.
Blinking or twitching
Buphthalmos may also cause your baby’s eyes to blink or twitch frequently. This is known as blepharospasm, which refers to involuntary eyelid movements.
How doctors find buphthalmos
Some features of buphthalmos, such as high IOP and specific eye measurements, need to be evaluated by an eye doctor. A comprehensive eye exam can be done to check the cornea for damage and rule out other diseases or conditions.
Some tests may be performed under general anesthesia to avoid involuntary reactions like crying or squeezing the eyes closed. The parameters measured by these tests can include:
- High eye pressure (IOP) – IOP is measured by using an instrument called a tonometer. This determines IOP by measuring the force necessary to flatten the cornea.
- Drainage inside the eye – A gonioscopy involves placing a special lens on the cornea that helps the examiner see the eye’s anterior chamber. This is the area right behind the cornea that contains aqueous humor (a fluid that helps maintain IOP). Ultrasound biomicroscopy, which is noninvasive, may also be performed.
- Increased diameter of the cornea – An instrument called a caliper is used to measure the diameter of the cornea. (A diameter greater than 12 mm before the age of 1 is usually considered abnormal.)
- Refractive errors – Refractive errors occur when the eye cannot properly focus light on the retina (as in axial myopia). Streak retinoscopy, which produces a line of light to assess reflected light, is typically used to measure refractive errors.
Treating buphthalmos
The most important aspect of treating buphthalmos is managing high IOP. There are several surgical and medical options that might be used to keep the pressure from getting too high.
Surgery
Glaucoma surgeries typically aim to reduce IOP by helping fluid drain from the eye. These surgeries can include:
- Goniotomy – A procedure in which openings are made within the trabecular meshwork to increase fluid outflow. The trabecular meshwork is the part of the eye that controls the rate at which aqueous humor drains.
- Trabeculotomy or trabeculectomy – Additional procedures that also involve the trabecular meshwork, either by making specific incisions or removing parts of it. One or both of these surgeries may be performed, depending on the circumstances.
- Glaucoma drainage implants – Special devices implanted in the eye to increase fluid drainage.
- Cyclodestructive procedures – Used to target the ciliary body (the part of the eye that creates aqueous humor) to reduce fluid production.
Surgery is the most common treatment to help manage high IOP in buphthalmos. However, early treatment is crucial to preserve sight. Generally, the earlier the treatment, the better the prognosis.
Eye drops
Topical medications are typically used to control eye pressure and swelling before surgery. They can also be used after surgery if needed.
Eye drops can contain medications that slow or reduce the production of fluid, like beta blockers or carbonic anhydrase inhibitors. Prostaglandin analogs (synthetic versions of a hormone-like substance in the body) increase the outflow of fluid.
Although studies have shown that many of these substances are safe and effective in children, some may not be appropriate for those of certain ages. For instance, alpha 2 agonists (which also decrease fluid) can cause apnea in children under age 2. It is important to discuss these options with a doctor, especially when it involves a child.
READ MORE: What do the different cap colors mean on medicated eye drops?
Glasses
While glasses will not change the size of the eyeball, prescription glasses may be prescribed in cases where vision is affected.
What happens if it’s not treated?
Buphthalmos is a serious condition, especially when it’s caused by congenital glaucoma. It should be treated immediately to prevent irreversible damage to the optic nerve, which can lead to visual impairment or even blindness. If left untreated, buphthalmos can cause complications that pose a threat to eye health and vision.
Some of these complications are:
- Damage to the cornea (causing the corneal haziness that is sometimes a symptom)
- Amblyopia (lazy eye)
- Refractive errors
- Glaucoma
- Retinal detachment and other retinal complications
- Dislocation of the eye’s natural crystalline lens
- Vision loss
In more severe cases, some of these problems may require surgery. But treating buphthalmos early greatly reduces the risks and severity of these complications.
Living with buphthalmos
If you or your child has a congenital eye condition, it’s important to see an eye doctor regularly. With buphthalmos, IOP needs to be monitored to prevent complications. Getting regular eye exams is key to tracking damage so you can start treatment when you need it.
Surgical intervention may be needed at some point to lower IOP, but eye drops may also be used to help manage it in the meantime. Vision problems caused by refractive errors can typically be corrected with prescription eyeglasses.
Staying in good health and taking care of your eyes in general is also important to prevent serious complications. Other steps you can take include:
- Protecting your eyes in the workplace and when playing sports
- Wearing sunglasses that provide 100% UVA and UVB protection
- Keeping contact lenses clean and washing your hands before removing and inserting them
Worried about buphthalmos? See a doctor
Buphthalmos is the enlargement of one or both eyes due to high IOP, usually caused by fluid buildup in the eye. This condition is normally observed at birth or shortly after. It is often a sign of congenital glaucoma.
High pressure in the developing eye can cause irreversible changes over time, possibly even leading to vision loss. It is important to treat this condition early. If your baby’s eyes are larger than normal or show other signs of the condition, consult a doctor as soon as possible. With early diagnosis and treatment, it’s often possible to avoid the most serious complications, such as visual impairment.